Abstract
Abstract 4253
Hypoalbuminemia (HA) is a strong predictor of poor clinical outcomes in many medical conditions. Low serum albumin is recognized as an adverse prognostic factor in patients with neoplastic diseases such as multiple myeloma, melanoma, and colon cancer. Severe hypoalbuminemia (<3.0 g/dl) at day +90 post allogeneic hematopoietic cell transplant (AHCT) was reported as an independent predictive variable for non-relapse mortality and overall survival (Kharfan-Dabaja, et al Biol Blood Marrow Transplant 2009; 15). A separate study conducted by our group showed that in patients with relapsed and refractory AML, serum albumin < 3.5 g/dl prior to salvage chemotherapy, correlated with lower complete remission (CR) rate and inferior overall survival (OS) (Komrokji, et al ASH 2009). We examined the prognostic value of serum albumin level prior to induction chemotherapy in patients with newly diagnosed AML.
Data were collected retrospectively in a cohort of newly diagnosed AML patients who received induction chemotherapy (3+ 7 regimen). The primary objective of this study is to examine the relationship between serum albumin at baseline and probability for achieving complete remission (CR) or incomplete remission (CRi) and overall survival (OS). All analyses were conducted using SPSS version 19.0. The Kaplan–Meier method was used to estimate median overall survival; chi-square test was used for comparison of categorical variables and t-test for continuous variables. Log rank test was used to compare Kaplan–Meier survival estimates between two groups and Cox regression for multivariable analysis.
Between November 2004 and July 2007, 135 patients who received 3+7 induction chemotherapy at Moffitt Cancer Center were included in this analysis. Patient baseline characteristics were similar between patients with baseline serum albumin < 3.5 g/dl (HA) and those with serum albumin ≥ 3.5 g/dl (no HA) with respect to age, sex, FAB subtype, history of antecedent MDS, karyotype, and chemotherapy. Patients with HA, mean age was 60 years compared to 56.5 years in non HA group.
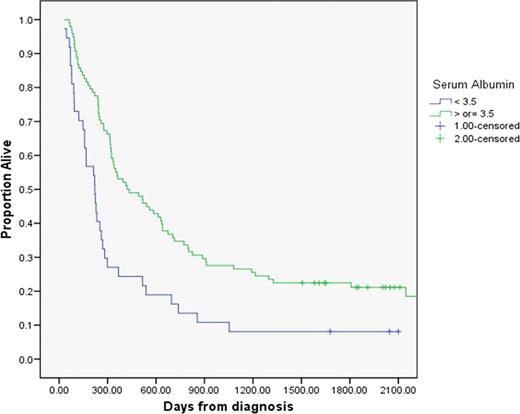
The median OS for patients with HA was 221 days (95%CI 149.5–292.5) compared to 421 days (95%CI 236.7–605) with normal serum albumin (p<0.005). (Figure-1) The CR/CRi rate was 64%% for HA and 77.6% for those with normal albumin (p=0.09).
Kaplan-Meier Survival curves for patients with normal serum albumin and HA
In a multivariable Cox regression analysis including age ≥ 60 years, history of MDS, karyotype, and serum albumin level at baseline; only age, karyotype and serum albumin were independent predictors of OS [Hazard ratio 0.47 (95%CI 0.31–0.71) (p<0.005) for normal serum albumin group].
In this cohort of patients with newly diagnosed AML, we demonstrate that hypoalbuminemia < 3.5 g/dl is an independent covariate for overall survival with conventional chemotherapy management. Serum albumin is a surrogate marker of general health, comorbidities, and performance status. The prognostic value of low serum albumin should be validated in a prospective study.
No relevant conflicts of interest to declare.
Author notes
Asterisk with author names denotes non-ASH members.