Abstract
Abstract 3001
Vasoactive intestinal peptide (VIP) has potent immune-suppressive activity and can generate tolerogenic dendritic cells (DC) in vitro that block graft versus host disease (GvHD) in mouse model of BMT. We have previously published that absence of VIP signaling dramatically decreases PD-1 expression on activated CD8 T-cells and increases cellular antiviral immunity (JI 2011, 187:1057). To determine whether blockade of VIP-signaling enhances the graft-versus-leukemia (GvL) activity of donor T-cells in an allogeneic BMT model, we treated tumor bearing B6B̂10BR allogeneic transplant recipients with a short course of daily s.c. injections of a small molecule VIP antagonist - VIPhyb or used VIP-knockout (VIP-KO) mice as BM donors.
Recipient mice were inoculated with luciferase+ murine acute T-cell lymphoma cells (Luc+ LBRM) by i.v. injection one day after lethal total body irradiation, then transplanted with the combination of 5 × 106 T cell-depleted BM (TCD-BM) plus splenocytes from either VIP-KO mice or wild-type (WT) littermates two days after irradiation. One group transplanted with WT BM and splenocytes received daily injections of 10 μg VIPhyb for one week; another group received saline injections. Survival, GvHD clinical sores (body weight, activity, posture, fur texture and skin), and bioluminescence imaging (BLI) were collected daily, twice a week, and weekly, respectively.
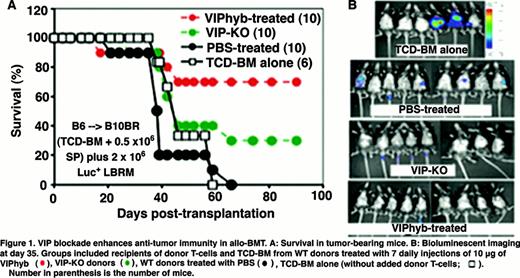
Transplantation of low dose (0.5 × 106) splenocytes from VIP-KO donors or low dose WT splenocytes in conjunction with VIPhyb-treatment dramatically improved tumor-free survival in the B6B̂10BR allogeneic BMT model compared with PBS-treated recipients of WT grafts (Figure 1). The best overall survival (70%) and lowest number of mice with detectable tumor (10%) were seen in the VIPhyb-treated group. VIPhyb-treated mice did not have increased GvHD as assessed by clinical scoring. Recipients of VIP-KO grafts had 40% survival with no detectable tumors by BLI, and were without significant GvHD by clinical scoring. In contrast, the recipients transplanted with TCD-BM alone (without added splenocytes) and recipients that received 0.5 × 106 splenocytes and TCD-BM from WT donors and treated with PBS had increased tumor growth detected by BLI following BMT, and all of the mice died by 2 months post-BMT.
Moreover, in non-tumor bearing mice transplanted with an intermediate dose (1 × 106) of splenocytes, survival was not different among recipients engrafted with VIP-KO BM and T-cells (84 ± 6 %), WT BM and T-cells treated with VIPhyb (89 ± 8 %) and WT BM and T-cells treated with PBS (94 ± 5 %). A similar enhancement of the GvL effect and a corresponding survival advantage for VIP-signaling blockade was seen in tumor-bearing transplant recipients of TCD-BM plus 1 × 106 splenocytes, with significantly better survival among recipients of VIP-KO donor cells (50%), recipients of WT cells treated with VIPhyb (60%) compared with recipients of WT cells treated with PBS (20%; p=0.04). Furthermore, in non-tumor bearing mice that received a higher dose (3 × 106) of splenocytes, recipients of VIP-KO BM and recipients of WT BM treated with VIPhyb had no significant increase in GvHD compared with recipients of WT BM treated with PBS (66 ± 9 %, 71 ± 8 % and 71 ± 8 % survival at 80 days, respectively). The mechanism by which administration of a VIP antagonist enhanced anti-tumor immunity includes the effect of blocking VIP-signaling induction of cAMP, leading to fewer Treg and fewer tolerogenic DC. Of note, blocking VIP-signaling led to significant decreases in expression of PD-1 and PD-L1 on CD8+ T-cells and DCs, respectively.
Treatment with a small molecule antagonist of VIP-signaling, VIPhyb, dramatically increased anti-leukemic activity of donor T-cells without significantly increased GvHD.
No relevant conflicts of interest to declare.
Author notes
Asterisk with author names denotes non-ASH members.