Abstract
Abstract 939
Although IFNα has shown some efficacy in the treatment of multiple myeloma (MM), this efficacy has been limited in large part because systemic toxicity makes it difficult if not impossible to reach therapeutically effective doses at the site of the tumor. The short half-life of IFN also makes it difficult to sustain high levels during treatment, and because of the side effects, the patients often discontinue therapy. To address these issues, we have genetically fused IFNα2 to a chimeric IgG1 antibody specific for the antigen CD138 expressed on the surface of MM cells, yielding anti-CD138-IFNα. We have also produced a fusion protein (anti-CD138-mutIFNα) using a mutant IFNα that binds the IFN receptor (IFNAR) more tightly. The fusion proteins continued to bind CD138 and retained IFN activity and showed anti-proliferative activity against a broad panel of myeloma cell lines (HMCL) representing MM with different characteristic.
To investigate the events responsible for the inhibition of proliferation, 8226/S, ANBL-6, MM1-144, H929, OCI-My5 and U266 cells were incubated with 500 pM anti-CD138-IFNα for 72 h and their DNA content analyzed by FLOW cytometry following permeabilization and staining with PI. The different cell lines exhibited different responses. All of the cell lines except OCI-My5 underwent apoptosis. For 8226/S, OCI-My5 and U266 there was little change in DNA content following treatment. ANBL-6 showed a slight increase in the number of cells in S. However, MM1-144 and H929 showed a marked accumulation in G2 with H929 also showing accumulation of cells with sub-G0content of DNA. Therefore, there is heterogeneity in the response of different HMCL to treatment with targeted IFNα2. For many but not all of the cell lines, anti-CD138-mutIFNα was more effective than anti-CD138-IFNα in inhibiting proliferation and causing DNA fragmentation. Anti-CD138-mutIFNα was more effective than anti-CD138-IFNα in inducing senescence-associated β-galactosidase and STAT1 activation in OCI-My5 cells. Treatment with anti-CD138-IFNα or anti-CD138-mutIFNα resulted in a decrease in the amount of IRF4 present in U266, suggesting that this may be responsible for the efficacy of the fusion proteins in this cell line. Treatment of the other cell lines did not alter the level of IRF4 present, but anti-CD138-IFNα and anti-CD138-mutIFNα treatment caused a decrease in the amount of ppRB present in 8226/S, OCI-My5 and MM1-144, and to a lesser extent in H929.
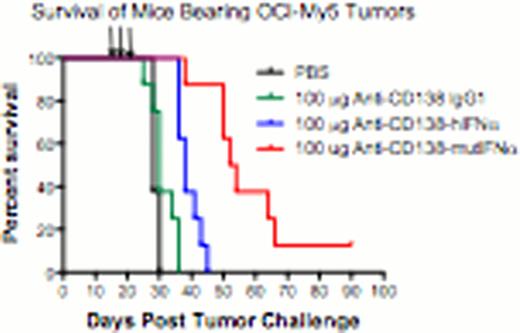
To determine the in vivo efficacy of fusion protein treatment, SCID mice were injected subcutaneously with OCI-My5 cells and treated intravenously on days 14, 16 and 18 with 100 μg of the indicated proteins and monitored for tumor growth (Figure 1). Mice were sacrificed when tumors exceeded 1.5 cm in diameter. Treatment with anti-CD138-IFNα provided some protection (p ≤ 0.0001 compared to PBS). However, treatment with anti-CD138-mutIFNα was even more effective (p = 0.0004 compared to anti-CD138-IFNα).
Anti-CD138-mutIFNα was also found to be more effective than anti-CD138-IFNα against primary MM cells. Patients with active myeloma were biopsied while off therapy and the marrow cells isolated by a negative antibody selection to >95% purity. After 72 h incubation with 25 nM of protein, anti-CD138 was found to have little effect. In contrast treatment with anti-CD138-IFNα caused a decrease in viability with anti-CD138-mutIFNα treatment leading to an even greater decrease in cell viability. Following 72 h of treatment, 25 nM of anti-CD138-mutIFNα was found to have more potent cytoreductive effects than 100 nM of anti-CD138-IFNα.
No relevant conflicts of interest to declare.
Author notes
Asterisk with author names denotes non-ASH members.