Abstract
Vasoactive intestinal peptide (VIP) is a neuropeptide hormone that suppresses Th1 immunity and inhibits antiviral immunity. Decreased Th1 immunity is problematic for allogeneic bone marrow transplant (allo-BMT) patients requiring T-cell immunity against blood cancers (Graft-versus-Tumor) and against secondary infections such as CMV. VIPhyb, a modified VIP peptide, is a VIP receptor antagonist that decreases VIP signaling. VIP-knockout mice and mice treated with VIPhyb after allo-BMT are known to have better antiviral immunity and survival after CMV infection without increasing GvHD (Li et al. PLoS One. 2013 May 27;8(5):e63381) (Li et al. Blood. 2013 Mar 21;121(12):2347-51.), thus making VIPhyb of interest for pharmacological use in humans to improve the efficacy of allo-BMT
The effects of VIPhyb on T-cell immunity are not yet fully profiled. This study aimed to analyze the effects of VIPhyb on CD4+ and CD8+ T-cell proliferation and activation in order to better understand the mechanistic implications of VIP inhibition on T-cell adaptive immunity. This study also aimed to show that mixed lymphocyte reactions (MLRs), an in vitro allo-BMT model, could be used to provide rapid and reliable results that are consistent with in vivo data. It was hypothesized that VIPhyb would increase T-cell immunity as profiled by: increased T-cell proliferation, CD69 and PD1 co-upregulation in early T-cell activation, and PD1 downregulation in T-cells after initial activation.
Splenocytes from two histoincompatible mice were cultured together at 37°C in a 1:1 ratio in a one-way MLR. BALB/c splenocytes (stimulators) were irradiated at 20Gy, and Pepboy splenocytes (responders) were labeled with CFSE to trace proliferation. VIPhyb was added daily to the cell cultures in doses of 0.1μM, 0.3μM, 1μM, or 3μM. Treatment groups were compared to a PBS control. Proliferation, CD69, and PD1 were assessed by flow cytometry on the BD FACSAria. All results are shown as mean ± SEM (n=3). One-way ANOVA tests with Dunnett post-tests were calculated using Prism software. *p < 0.05; **p < 0.01; ***p < 0.001
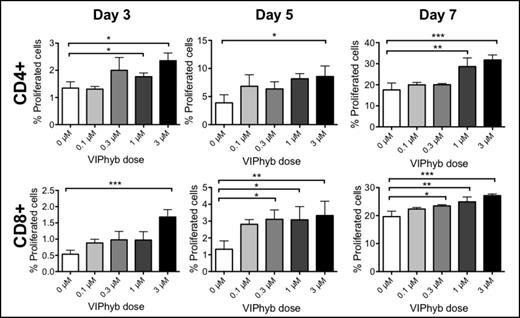
VIPhyb increased CD4+ and CD8+ T-cell proliferation: 3, 5, and 7 days after initiating a one-way MLR, CFSE expression of Pepboy responder T-cells was assessed using flow cytometry (Figure 1). As the VIPhyb dose increased, the percentage of initial splenocytes that underwent proliferation increased in both CD4+ and CD8+ T-cells.
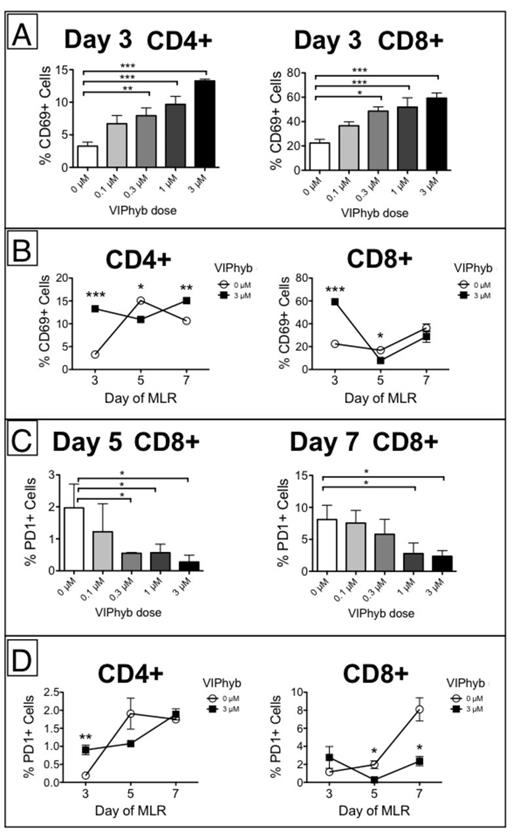
VIPhyb increased early T-cell CD69 expression and abrogated later PD1 upregulation in CD8+ T-cells: 3, 5, and 7 days after initiating a one-way MLR, expression levels of CD69 and PD1 on Pepboy responder T-cells were assessed by flow cytometry. Significant upregulation of CD69 on CD4+ and CD8+ T-cells on day 3 occurred with increasing VIPhyb doses (Figures 2A and 2B). PD1 was co-upregulated with CD69 during early activation, and VIPhyb significantly decreased PD1 expression on CD8+ T-cells on days 5 and 7 (Figures 2C and 2D).
VIPhyb increased early CD69 expression and abrogated PD1 upregulation in CD8+ T-cells
VIPhyb increased early CD69 expression and abrogated PD1 upregulation in CD8+ T-cells
VIPhyb increased T-cell proliferation; CD8+ T-cells were affected more significantly. VIPhyb increased early co-upregulation of CD69 and PD1 in all T-cells and significantly decreased later CD8+ T-cell PD1 expression, indicating that VIPhyb increases T-cell activation. We hypothesize that the decreased PD1 expression will be critical for understanding the pathways involved in VIP inhibition. Importantly, since it has been shown in vivo that VIPhyb does not increase GvHD, then it can be assumed that the VIPhyb-induced T-cell proliferation and activation will increase GvL and adaptive immunity without increasing alloreactivity. Notably, these results are consistent with published in vivo data, which demonstrates that the MLR can be used as a faster method of analyzing pharmacological compounds than in vivo experiments. Given these results, VIPhyb is still of interest as a potential therapy for allo-BMT patients.
No relevant conflicts of interest to declare.
Author notes
Asterisk with author names denotes non-ASH members.