Abstract
Background: Prior studies have demonstrated the utility of involved field radiation therapy to reduce relapse rates and improve local control in Hodgkin Lymphoma (HL). The standard treatment for early stage unfavorable HL is combined modality approach with chemotherapy and radiation therapy (XRT). Despite reduction in the fields of XRT, long term adverse outcomes are associated with the combined modality approach. Recent clinical trials have focused on adapting therapy based on interim PET scans. There is, however, limited data evaluating patient outcomes with chemotherapy alone in unfavorable, bulky HL patients.
Methods: Two hundred and fifteen patients diagnosed with HL at our institution were included in our retrospective analysis after obtaining IRB approval. Statistical analysis was performed by chi-square analysis, Wilcoxon signed rank sum test and Kaplan-Meier plots using SPSS.19 software.
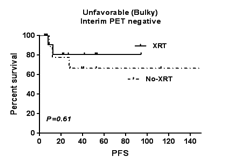
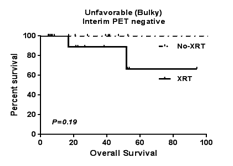
Results: Of the 215 patients, 48 had early stage unfavorable HL and were included in this analysis. Unfavorable HL was defined as bulky disease (>10cm or >1/3 thoracic diameter), ESR >50 or >3 extra nodal sites involvement at presentation. The median age at diagnosis was 31 years (range 17-58). Twenty-two patients (46%) were male. All patients had an Eastern Cooperative Oncology Group performance status of either 0 or 1. Nineteen patients (40%) presented with B symptoms. The majority (83%) of patients were treated with 4-6 cycles of ABVD as first line therapy, while the remainder were treated with COPP/ABV, Stanford V, ABV or MOPP/ABV. Approximately half of the patients received XRT (54%), which was determined by physician choice. Forty-six patients (96%) were alive at the time of analysis. Seven patients (15%) underwent autologous stem cell transplantation for either disease relapse or for an incomplete response. Interim PET data was missing in 8 patients, who were excluded from subsequent analysis. Interim PET was positive in 13 of the remaining 40 patients, 9 of whom received consolidative radiation therapy and 4 of whom received high dose therapy followed by autologous stem cell transplantation. Among the 27 patients with negative interim PET, 12 received XRT. The median overall survival (OS) of all patients was 38.8 months. In patients with negative interim PET scan, the PFS was 83% and 80% in patients who received chemotherapy with and without XRT, respectively. The OS was 83% and 100% in patients who received chemotherapy with and without XRT, respectively. The differences in PFS and OS were not statistically significant between the two groups. Two patients died in the group that received combined modality treatment after negative interim PET, one from pre-existing cardiomyopathy and one from progression of disease. No death was related to XRT. In a subgroup analysis, eleven of the 27 patients with negative interim PET had bulky disease, 8 of whom received XRT. The PFS in this subgroup was 75% and 100% in patients who received chemotherapy with and without XRT, respectively. The OS in this subgroup was 88% and 100% in patients who received chemotherapy with and without XRT, respectively.
Conclusion: Our data suggests that radiation therapy can be avoided based on interim PET scan in early stage unfavorable HL without compromising OS. The high overall survival of these patients may be accounted for by the fact that many who fail initial treatment can be salvaged with high dose chemotherapy and autologous stem cell transplantation. Given the potential for reduction in radiation related adverse outcomes, we encourage participation in ongoing prospective, PET-adapted, clinical trials investigating the need for consolidative XRT following chemotherapy in patients with unfavorable, bulky disease.
No relevant conflicts of interest to declare.
Author notes
Asterisk with author names denotes non-ASH members.