Abstract
Objectives and background: The level of early MR is important for the optimization of therapy and making a decision to a switch to 2nd line therapy in patients (pts) who have not achieved an optimal response (OR). According to the recent recommendations at definition of OR on CML therapy, pts must have the level of BCR-ABL transcript gene at 10% or less and Ph-positive cells 35% or less at 3 months. But, in half of all cases of pts with BCR-ABL >10% at 3 months progression events happen between 3 and 6 months. The goal of our research was to investigate the prognostic impact of a large BCR-ABL transcript amount at 3 months on the subsequent response and the long-term outcome of CML pts treated frontline with IM.
Methods: We have examined 185 pts, who have got IM from January 2010 up to the present. Molecular monitoring has been done regularly in all patients according to ELN recommendations. Median age was 49 years. All pts were in CP. BCR-ABL transcript levels were assessed by real-time quantitative PCR.
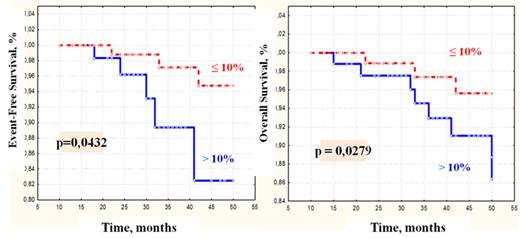
Results: In our study 54% (100/185 cases) of pts achieved the optimal response with BCR-ABL transcript levels ≤10% at 3 months, 50,3% (93/185 cases) did it - with BCR-ABL transcript levels ≤1% at 6 months, and only 18% achieved the optimal response at 12 months. The comparative analysis has shown statistical differences in all characteristics in 2 groups of pts, who either achieved or not the optimal response at 3 months. Pts with BCR-ABL transcript levels ≤10% more often achieved CCgR at 6 months (g=0,0000), CCgR during all period (g=0,0004), MMR at 12 months (g=0,0000), MMR during all period (g=0,0012) and MR4 during all period (g=0,0000), pts had londer event-free (g=0,0432) and overall (g=0,0279) 4-year survival.
In our center we have switched 6 patients to the 2nd TKI - those who didn't achieve the optimal response at 3 months. The switching showed the positive influence on loss level expression of BCR-ABL gene in 5 out of 6 patients. After that all patients achieved the optimal response in the future. For example, we had one patient with failure of IM at 3 months. We switched him the therapy to NI in 5 months after the diagnosis. As a result the patient achieved CCgR at 1,5 months, and the deep molecular response 4,5 log at 3 months.
Conclusions: Early and deep responses to TKIs are predictive of long-term response and favorable survival outcomes. 3-month reduction in BCR-ABL transcript levels to >10% is a factor of bad effectiveness of TKI therapy and requires switching to the 2nd TKI. Timely switching to the 2nd TKIs allows us to achieve an optimal response in CML patients with level BCR-ABL >10% at 3 months.
References: Timothy P. Hughes, Giuseppe Saglio, Hagop M. Kantarjian et al. Early molecular response predicts outcomes in patients with chronic myeloid leukemia in chronic phase treated with frontline nilotinib or imatinib. Blood, 27 February 2014 x Volume 123, Number 9.
No relevant conflicts of interest to declare.
Author notes
Asterisk with author names denotes non-ASH members.