Abstract
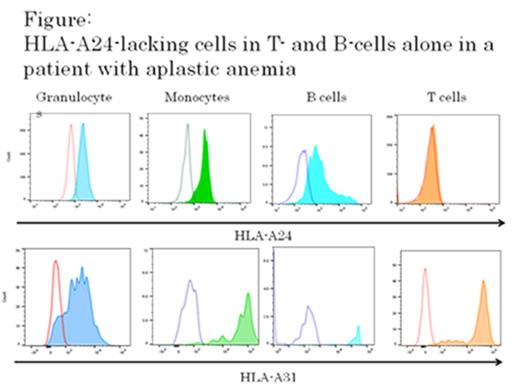
A T-cell attack against hematopoietic stem cells (HSCs) is believed to be the principal mechanism underlying the development of acquired aplastic anemia (AA). The presence of leukocytes that lack HLA class I alleles as a result of the copy number-neutral loss of heterozygosity of the HLA haplotype due to uniparental disomy in the short arm of chromosome 6 (6pLOH) is compelling evidence for the involvement of cytotoxic T lymphocytes (CTLs) in the HSC destruction; this is based on the high response rate to immunosuppressive therapy (IST) in 6pLOH(+) patients (Katagiri, et al. Blood, 2011). However, target cells of the putative CTLs have not yet been characterized because of the small number of patients analyzed via flow cytometry (FCM) in our previous study. FCM can be substituted for SNP arrays by detecting HLA-A allele-lacking leukocytes (HLA-LLs) caused by 6pLOH. To gain insight into the CTL target responsible for the development of AA, we examined a total of 223 patients (213 idiopathic and 10 hepatitis-associated AA; 93 severe and 130 non-severe AA) for the presence of HLA-LLs and determined the lineage combinations of the aberrant leukocyte population. Of the 223 patients, 145 (65.0%) were heterozygous for the HLA-A allele and could be assessed for the presence of HLA-LLs by FCM. Eighteen (25.4%; 10 with severe AA and 8 with non-severe AA) of the 71 pre-treatment patients, and 26 (35.1%; 13 with severe AA and 13 with non-severe AA) of the 74 post-treatment patients were found to be positive for HLA-LLs. The lineage combinations of HLA-LLs in the 44 HLA-LL(+) patients were granulocytes (Gs), monocytes (Ms), B cells (Bs), and T cells (Ts, GMBT) in 13, GMB in 16 and GM in 11 patients. Surprisingly, HLA-LLs were found in Bs alone in three patients, and in one patient, the lineage combination pattern was TB (Figure). The presence of 6pLOH was confirmed via deep sequencing of isolated Bs from one of the three Bs alone patients. These lineage combination patterns were not observed to change for 1-40 months in 22 of 23 patients whose blood samples were available for follow-up analyses. In one patient with the GMB pattern, HLA-LLs decreased from 11.7% before treatment to 0% after 12 months of ATG therapy. The response rate to IST in GMBT patients (3/4, 75%) and in patients with GMB or GM (9/10, 90%) were similarly higher than in patients without HLA-LLs (22/39, 56%) or in patients who were homozygous for the HLA-A allele (23/36, 64%). Two of the three Bs alone patients showed complete responses at the time of sampling three years after ATG therapy and 20 years after CsA therapy, and another patient had a secondary myelodysplastic syndrome two years after response to ATG. The TB alone patient developed AA 20 years earlier, but had not been treated until recently because there was no need for blood transfusions, and is now improving in response to eltrombapag. This study revealed that the targets of putative CTLs in more than half of AA patients are hematopoietic progenitor cells with limited differentiation but long-lasting capacity, and in some patients, they are lymphoid progenitor cells that do not contribute to hematopoiesis. This suggests that CTL attack against non-HSCs including lymphoid precursors could trigger BM failure. Consistent with our previous report, the bystander effects caused by the immune response to non-HSCs such as myelosuppressive cytokines may play a major role in the development of AA.
No relevant conflicts of interest to declare.
Author notes
Asterisk with author names denotes non-ASH members.