Abstract
The majority of children and adults who experience relapse of acute lymphoblastic leukemia (ALL) will die from the disease. The presence of leukemic blasts within the cerebrospinal fluid (CSF) is an important predictor of disease recurrence in both the bone marrow (BM) and central nervous system (CNS), a frequent site of disease involvement. In the absence of intrathecal chemotherapy or craniospinal irradiation, 30%‒50% of patients will in fact develop CNS disease. All patients therefore receive CNS prophylaxis. High-risk patients require intensive CNS-directed treatment that causes toxic side effects and can impact cognitive development in children. Patients who develop recurrence in the CNS have limited treatment options and an extremely poor prognosis.
The enzyme PI3K plays an important role in many biological effects including cell proliferation, migration, and apoptosis. The d isoform of PI3K is specifically expressed in immune cells. The PI3Kd inhibitor idelalisib is approved for use in combination with rituximab for the treatment of chronic lymphocytic leukemia (CLL). However, little is known about the efficacy of PI3Kd inhibition in ALL. Here, the PI3Kd inhibitor GS-649443, a potent and specific in vivo tool compound, was evaluated in a xenograft mouse model.
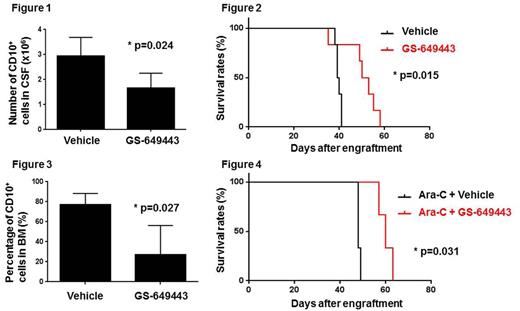
The in vivo effects of GS-649443 were investigated in a Nalm-6 pre-B ALL SCID model. At approximately 40 days postengraftment, untreated mice all developed symptoms of CNS involvement and displayed hind limb paralysis. Hind limb paralysis is the clinical endpoint for sacrifice, occurring prior to death from progressive BM disease. Mice were treated with GS-649443 by oral gavage beginning on postengraftment day 1 and continuing until the development of clinical symptoms requiring sacrifice (hind limb paralysis, weight loss >20%, respiratory or other distress). Only 17% of GS-649443‒treated mice developed hind limb paralysis at their clinical endpoint, while 100% of vehicle-treated mice showed hind limb paralysis. In addition, mice treated with GS-649443 or vehicle control were paired. When either mouse in a treatment pair reached a clinical endpoint, both were sacrificed so disease burden in individual organs could be compared at matched time points. There was no difference in tumor burden or leukemic cell apoptotic rate in the BM of treated vs vehicle control groups. In contrast, there was a significant decrease in the number of leukemic blasts harvested from the CSF of treated mice (Fig. 1). Consistent with the inhibition of CNS disease progression, GS-649443 significantly prolonged the survival of treated mice (Fig. 2).
While compromised blood-brain barrier in leukemic mice may allow therapeutic targeting of CNS disease, it is unknown whether GS-649443 enters the CNS in healthy rodents. Given the well-described effects of idelalisib on CLL cell migration, we hypothesized that PI3Kd blockade impacts disease in this ALL model by impairing leukemia migration into the CNS. To investigate the in vitro effect of GS-649443 on ALL cell migration, transwell migration assays with SDF-1 as chemoattractant were performed. Both GS-649443 and idelalisib suppressed migration of Nalm-6 and primary human ALL cells toward SDF-1.
Lastly, the effects of GS-649443 in combination with conventional chemotherapy were examined. GS-649443 alone did not cause significant cytotoxicity of Nalm-6 in vitro, however, treatment with GS-649443 after cytarabine significantly increased apoptosis. Leukemic mice (20 days post-engraftment) were then treated with cytarabine (days 1‒5) in combination with GS-649443 or cytarabine alone (days 1‒7) for 1 cycle. In contrast to the single-agent study, significant decreases in the number of leukemic blasts harvested from both the BM and CSF of treated mice were observed, suggesting that PI3Kd inhibition sensitized ALL cells to cytarabine chemotherapy (Fig. 3). This decrease in residual disease after combination therapy led to significantly prolonged survival in GS-649443‒treated mice (Fig. 4).
Taken together, this study provides evidence that PI3Kd inhibition prevents ALL progression in the CNS. In addition, GS-649443 and conventional chemotherapy appear to synergize to decrease residual BM disease. The potential for PI3Kd inhibition to improve chemotherapy response and impede development of CNS disease in ALL warrants further investigation in a translational clinical study.
Yao:Gilead Sciences, Inc.: Research Funding. Price:Gilead Sciences, Inc.: Research Funding. Olivere:Gilead Sciences, Inc.: Research Funding. Warner:Gilead Sciences, Inc.: Research Funding. Tannheimer:Gilead Sciences: Employment. Sipkins:Gilead Sciences, Inc.: Research Funding.
Author notes
Asterisk with author names denotes non-ASH members.