Introduction: Splenectomy has been a historically important diagnostic and therapeutic modality for splenic lymphomas, but with the advent of sensitive diagnostic tools and efficacious immunochemotherapy, its role has diminished. Our objective was to describe trends in the use of splenectomy for management of splenic lymphomas, and to determine the association of practice setting with choice of surgical treatment.
Methods: Using the National Cancer Data Base (NCDB), a nationwide registry capturing >80% of lymphomas in the United States, we selected non-Hodgkin lymphoma cases diagnosed in 2004-2013, with spleen recorded as the primary site. We identified the use of splenectomy and chemotherapy as part of the initial treatment. Splenectomy was assumed to be diagnostic when it was coincident with lymphoma diagnosis (0 days from diagnosis to surgery). Treatment facilities were designated by the NCDB as community, comprehensive community, academic/research, or integrated network cancer programs, depending on case volume and available services. We studied factors associated with the use of splenectomy in a multilevel mixed-effects logistic model (with random intercepts for each geographic region and each facility within it), reporting odds ratios (OR) and intraclass correlation (ICC) with 95% confidence intervals (CI). Linearized trends from log-binomial regression were expressed as average annual percent change (APC) in the proportion of patients (pts) undergoing splenectomy.
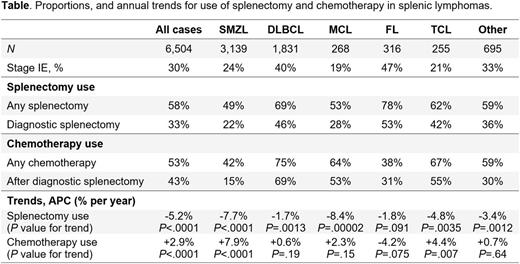
Results: Among 6,504 of pts with splenic lymphomas, 48% were classified as splenic marginal zone (SMZL), 28% as diffuse large B-cell (DLBCL), 4% as mantle cell (MCL), 5% as follicular (FL), 4% as T-cell lymphoma (TCL, 52% being hepatosplenic γd-TCL), and 11% were other or unspecified histologies. Overall, 58% of pts underwent any splenectomy, and 33% a diagnostic splenectomy, but these proportions significantly varied by histology (χ2P<.0001, Table). After a diagnostic splenectomy, 31% of DLBCL and 47% of MCL pts did not receive chemotherapy.
Between 2004 and 2013, the proportion undergoing splenectomy significantly decreased for most histologies (Figure). This trend was most pronounced in SMZL (APC, -7.7%; Table), and MCL (APC, -8.4%), and it was paralleled by a significant increase in the use of chemotherapy for management of SMZL and TCL. Mortality at 30 days after splenectomy was 4% overall, varying from <2% in SMZL/MCL/FL, 6% in DLBCL, to 10% in TCL (χ2P<.0001).
The proportion of pts undergoing splenectomy differed significantly according to type of treating hospital only in SMZL, where it was 39% for pts treated in "community", 52% in "comprehensive community", 50% in "academic/research", and 44% in "integrated network" centers (χ2P=.0004). In contrast, facility type was not associated with splenectomy use in DLBCL (P=.47), MCL (P=.55), FL (P=.75), or TCL (P=.15). The proportion of splenectomies performed for diagnosis was significantly lower in academic (51%) than in community (62%), comprehensive community (59%), or integrated network centers (60%, χ2P<.0001)
In a multivariable model in treated SMZL pts, those who had advanced-stage lymphoma or B symptoms, and those who were older, male, without comorbidities, with Medicaid, or with no insurance were significantly less likely to undergo splenectomy. There was evidence of significant clustering of treatment selection in each hospital (ICC, 24%; CI, 17-32%), but not in geographical regions (ICC, 2%; CI, 0.2-9.5%). Compared with academic/research centers, splenectomy was performed less frequently in smaller community centers (adjusted OR, 0.59; CI, 0.38-0.93, P=.022), but not in larger comprehensive community centers (OR, 0.97; CI, 0.72-1.32, P=.86).
Conclusions: Although the use of splenectomy for management of splenic lymphomas has declined, nearly half of pts with splenic DLBCL, FL, or TCL still undergo surgery for diagnosis, highlighting the ongoing need for reliable, non-invasive diagnostic modalities. A substantial proportion of pts with DLBCL and MCL do not receive chemotherapy after surgery. Further research should elucidate the reasons for it, and associated outcomes in those groups. In SMZL, the use of splenectomy is facility-dependent after adjusting for patient- and lymphoma-related characteristics, with lower rate of splenectomy in smaller community centers, possibly reflecting availability of surgical expertise.
Olszewski:TG Therapeutics: Research Funding; Genentech: Research Funding; Bristol-Myers Squibb: Consultancy.
Author notes
Asterisk with author names denotes non-ASH members.