Abstract
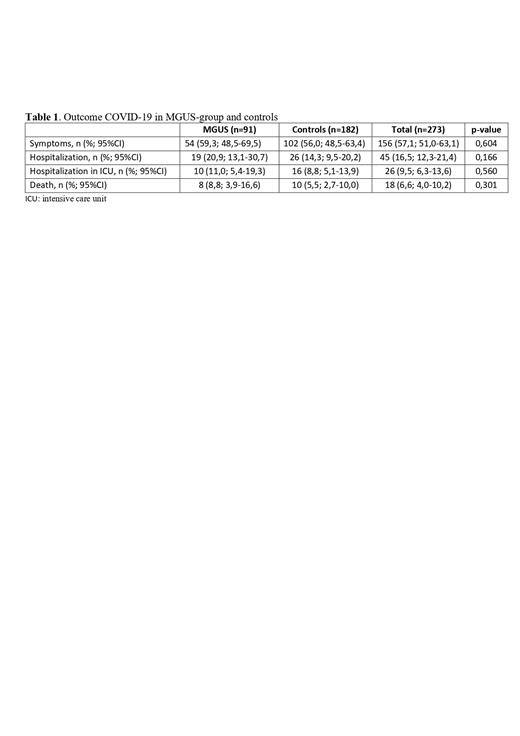
Introduction. Monoclonal Gammopathy of Undetermined Significance (MGUS) is a pre-malignant plasma cell disorder reported in approximately 3% of individuals aged > 50 years, characterized by a low risk (about 1% per year) of evolution into "overt" myeloma or other lymphoproliferative diseases. It is classified as IgM-MGUS (15%) and non-IgM-MGUS (80-85%). MGUS is usually asymptomatic, but a higher risk of deep venous thrombosis and infection has been reported. In March 2020, "Coronavirus Disease 2019" (COVID-19) outbreak has been declared a pandemic by the World Health Organization. Regarding outcome of COVID-19 in patients with plasma cell dyscrasia, many papers have been published about multiple myeloma (MM), reporting a higher fatality rate respect to general population, while few data are available about the outcome of SARS-CoV-2 infection in patients with MGUS. Methods. We collected clinical data on MGUS Apulian patients with SARS- CoV-2 infection, tested by RT-PCR on nasopharyngeal swabs between March 1st, 2020 and April 30st, 2021. Among 1454 MGUS patients followed at our center, 91 were found SARS-CoV-2 positive, enrolled in this observational, retrospective study and compared with 182 age and sex-matched normal controls. Clinical data collected regarded: symptoms, hospitalization, hospitalization in intensive care unit, death. Calculations were carried out using Stata MP17. Results. Mean age of whole group (n. 273) was 65,3+/-13,3 years (range: 29-89), with no statistically-significant differences (p=0,734) observed between MGUS-group (65,6+/-13,3; range: 29-89 years) and controls-group (65,2+/- 13,4; range: 29-89 years). Mean number of comorbidities in the whole group was 1,2+/-1,2 (range: 0-5) and no statistically-significant differences (p=0,844) were found between MGUS-group (1,3+/-1,3; range: 0-5) and control group (1,2+/- 0,9; range: 0-3). About MGUS-subtypes, the most frequent was IgG-kappa (n=36; 39,6%), followed by IgG-lambda (n=27; 29,7%) and IgM-kappa (n=6; 6,6%). Regarding MGUS risk-stratification, application of Mayo Clinic model identified 22 patients (24,2%) with low risk, 22 (24,2%) with low-intermediate risk, and 3 (3,3%) with high-intermediate risk; in 44 patients (48,3%) this data was missing. Immunoparesis was present in 13 cases (14,3%) and absent in 55 (60,4%), missing in 23 (25,3%). No patient developed MM or a lymphoproliferative disease progression during and immediately after COVID-19. Rates of symptoms (59,3% vs 56%), hospitalization (20,9% vs 14,3%), hospitalization in intensive care unit (11% vs 8,8%) and death (8,8% vs 5,5%) were slightly higher in MGUS group than controls (Table 1), but these differences were not statistically significant. A statistically significant association (p<0,05), was observed between higher age and death in both groups. Lastly, incidence of SARS-CoV-2 infection in MGUS patients (6,2%) was not statistically significant different from that observed in the population of the Puglia region (5,8%) in the same period. Conclusions. To our knowledge, this report is the largest study of patients with MGUS and SARS-CoV-2 infection to date. In our study patients with MGUS did not show an increased incidence of this infection compared to the general population and did not appear to represent a risk factor for poor outcome in COVID-19.
No relevant conflicts of interest to declare.