Abstract
INTRODUCTION: Lymphoma is associated with a high risk of venous-thromboembolism (VTE); we have previously shown that elderly patients with diffuse large B cell lymphoma (DLBCL) have a 6.7-fold higher risk of VTE compared to control population without a history of cancer. Given this high risk, we sought to examine the impact of VTE on healthcare utilization using Surveillance, Epidemiology, and End Results Registry (SEER) data linked with Medicare.
METHODS: We identified 5,537 Medicare beneficiaries diagnosed with DLBCL at age ≥66 years between 2011 and 2015, with at least 1 year of coverage prior to diagnosis, and initiation of chemotherapy within 1 year post-diagnosis. We ascertained pre-existing comorbidities for the 1 year prior to DLBCL diagnosis. Patients were followed from DLBCL diagnosis until 1 year after cancer diagnosis, or until death, loss of continuous Part A or Part B coverage, blood or marrow transplantation, or end of study (12/31/2016), whichever came first. VTE diagnosis was based on ICD 9 and ICD 10 codes for events including deep vein thrombosis (DVT) and pulmonary embolism (PE).
Hospitalizations and Outpatient Visits: Total number of hospitalizations and outpatient visits were compared in DLBCL patients with and without VTE for 1 year after cancer diagnosis, using multivariable negative binomial regression, offset for person-months and adjusting for age at diagnosis, race/ethnicity, stage at diagnosis and number of pre-DLBCL comorbidities (0, 1, 2+). Predicted counts for hospitalizations and outpatient visits were estimated from the multivariable models.
Healthcare Spending: Total inpatient and outpatient Medicare spending and spending per visit was estimated from multivariable quantile regression, offset for person-months contributed and adjusting for age at diagnosis, race/ethnicity, stage at diagnosis, and pre-DLBCL comorbidities (0, 1, 2+).
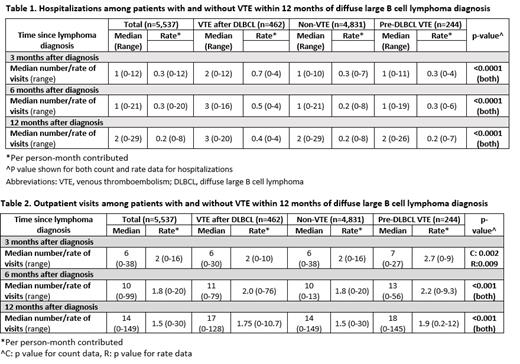
RESULTS: Overall, 462 (8.3%) patients developed VTE within 1 year of diagnosis of DLBCL and 244 patients had a VTE history before lymphoma diagnosis. Patients with VTE after DLBCL diagnosis had increased number of hospitalizations compared to those without VTE at the 3, 6 and 12 month time points in the first year after cancer diagnosis (Table 1). The median number of hospitalizations in patients with VTE was 2 compared to 1 in those without VTE at 3 months (p<0.0001). Increased hospitalizations continued until 1 year after lymphoma diagnosis; median number of hospitalizations was 3 in those with VTE compared to 2 in those without VTE at 1 year (p<0.0001). This lead to $51,285 in Medicare spending for hospitalizations in those with VTE compared to $37,065 in those without VTE (excess Medicare spending of $14,220 in those with VTE) in the first year after DLBCL diagnosis (p<0.001). We found no difference in the cost per visit; the excess costs were due to increased number of hospitalizations. The excess hospitalizations in those with VTE compared to those without VTE were primarily related to admissions for cardiovascular problems that included PE and/or DVT (14% vs 5%, respectively; p<0.001).
Patients with VTE also had increased outpatient visits in the first year (Table 2). Median number of outpatient visits was 17 in those with VTE compared to 14 in those without VTE at 1 year (p<0.001). Medicare spending for outpatient visits in patients with a VTE diagnosis after DLBCL was $13,851 in the first year compared to $5,863 in those without VTE ($7,988 excess in those with VTE, p<0.001). Similar to hospitalizations, there was no difference in the cost per outpatient visit and the excess costs were due to increased number of visits. Increased outpatient healthcare utilization was also noted in patients who had a history of VTE prior to DLBCL diagnosis compared to those without VTE (median number of outpatient visits: 18 vs 14, p<0.001).
CONCLUSION: In conclusion, elderly patients with DLBCL and VTE (diagnosed both before and after DLBCL diagnosis) have substantially higher healthcare utilization compared to those without VTE, resulting from both increased hospitalizations and outpatient visits in the first year after cancer diagnosis; these translate into higher Medicare spending. These findings identify a need for thromboprophylaxis in high risk patients after DLBCL diagnosis and future studies should assess cost-benefit analysis with thromboprophylaxis.
Gangaraju: Alexion: Consultancy; Sanofi Genzyme: Consultancy.