Background: Crizanlizumab, a selective, humanized immunoglobulin G2 kappa anti-P-selectin monoclonal antibody, demonstrated positive clinical activity and general tolerability in patients (pts) aged ≥16 years (yrs) with sickle cell disease (SCD) in a phase II SUSTAIN trial at a dose of 5 mg/kg when compared to placebo (PBO). This primary analysis (cutoff: August 31, 2022) from the ongoing multicenter (at 65 sites in 21 countries), Phase III STAND study (NCT03814746) included the comparison of the efficacy, safety, and expression levels of biomarkers, of crizanlizumab (5 & 7.5 mg/kg) vs PBO, over 1-year post randomization, in adolescent and adult pts with SCD.
Method: Pts aged ≥12 yrs, with a history of ≥2 vaso-occlusive crises (VOCs), with/without concomitant treatment with hydroxyurea/hydroxycarbamide were randomized (1:1:1) to receive intravenous crizanlizumab 5 mg/kg, 7.5 mg/kg, or PBO, on Day 1 of weeks (wks) 1 and 3, followed by every 4 wks in addition to standard of care therapy. Adverse events (AEs) were evaluated based on MedDRA version 25.1 and severity on CTCAE v5.0. Levels of biomarkers such as soluble P-selectin (sPsel), were evaluated.
Results: Overall, 252 SCD pts were enrolled: 85, 84 & 83 pts received PBO, crizanlizumab 5 & 7.5 mg/kg respectively. Mean (SD) age of pts was 27.8 (12) yrs, 54 (21.4%) were adolescents, and 139 (55.2%) were females. Treatment was discontinued in 27 (31.8%), 18 (21.4%), and 15 (18.1%) pts in PBO, crizanlizumab 5 & 7.5 mg/kg arms, respectively, primarily due to pts' (n=30) and physicians' decisions (n=8). Protocol deviations (n=97) were comparable across all arms; deviations due to COVID-19 (n=80) were mostly attributed to missed visits and assessment/procedure changes during lockdown/quarantine of pts.
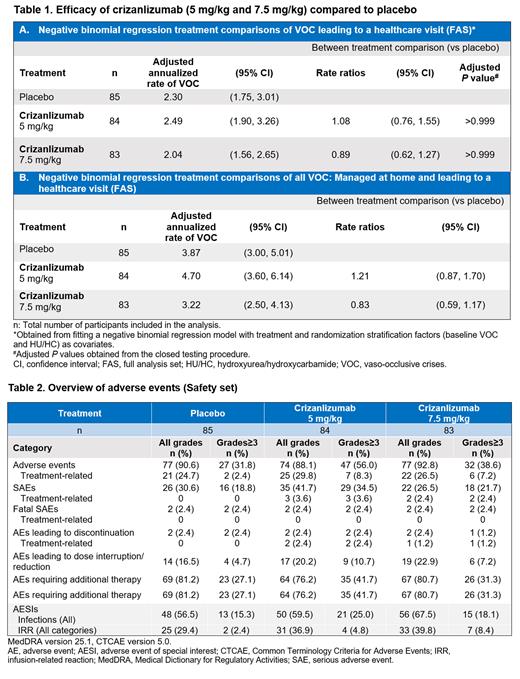
Rate ratios of adjusted annualized rates of VOCs leading to healthcare visits, with crizanlizumab 5 & 7.5 mg/kg vs PBO, were 1.08 (95%CI: 0.76, 1.55; P>0.999) and 0.89 (95%CI: 0.62, 1.27; P>0.999), respectively, indicating no statistically significant difference (Table 1A). Mean (SD) annualized rates of VOCs leading to healthcare visits were similar across PBO (2.1 [2.8]), 5 mg/kg (2.5 [3.0]), and 7.5 mg/kg (1.9 [2.3]) arms. Rate ratios of the adjusted annualized rates of VOCs managed at home and/or leading to a healthcare visit, with crizanlizumab 5 & 7.5 mg/kg vs PBO, were 1.21 (95%CI: 0.87, 1.70) and 0.83 (95%CI: 0.59, 1.17), respectively, suggesting no statistically significant difference (Table 1B).
Overall, AEs were reported in 77 (90.6%), 74 (88.1%), & 77 (92.8%) pts with PBO, crizanlizumab 5 & 7.5 mg/kg, respectively (Table 2), the most common being, pyrexia (22 [25.9%], 22 [26.2%], 19 [22.9%]), COVID-19 (17 [20.0%], 18 [21.4%], 27 [32.5%]), and headache (16 [18.8%], 21 [25.0%], 13 [15.7%]). Serious AEs (SAEs) and grade ≥3 AEs were less frequent with PBO (30.6%, 31.8%) and crizanlizumab 7.5 mg/kg (26.5%, 38.6%) than with 5 mg/kg (41.7%, 56.0%). Among AEs of special interest, infections, and infusion-related reactions (all categories) were the most frequent (Table 2). Treatment-related SAEs and AEs leading to discontinuation were rare (<4% pts, all arms). None of the 6 fatal SAEs were related to treatment.
Levels of free and total sPsel were measured across time: At Wk 3 Day 1, free sPsel showed a relative change from baseline in geometric mean (CV%, range) of 1.01 (56.2, 0.201-7.37) with PBO vs 0.05 (88.9, 0.00507-0.225) and 0.06 (68.4, 0.0146-0.208) with 5 & 7.5 mg/kg doses, respectively. Relative change from baseline in total sPsel remained close to 0% in the PBO arm at different study visits, while it increased in treatment arms from Wk 3 Day 1 onward, plateauing at Wk 15 Day 1.
Conclusion: Unlike the previous phase II PBO-controlled SUSTAIN study, the STAND study did not demonstrate superiority of crizanlizumab (5 or 7.5 mg/kg) over PBO on its primary and key secondary efficacy endpoints, in pts aged ≥12 yrs. These results differ from the previous study results and may be due to various factors, such as geographic differences in healthcare utilization as well as the low VOC rates in all arms, possibly either due to selection of pts with less severe disease, or, more likely due to the lower reporting of VOCs during the pandemic. The safety results were consistent with the known safety profile of crizanlizumab in SCD pts with no new safety concerns. Both treatment arms showed reductions in free sPsel vs PBO, demonstrating crizanlizumab activity on this biological parameter.
OffLabel Disclosure:
Abboud:Agios: Membership on an entity's Board of Directors or advisory committees; GBT: Research Funding; Novartis: Membership on an entity's Board of Directors or advisory committees, Research Funding; Forma: Research Funding. De Montalembert:Addmedica: Consultancy, Membership on an entity's Board of Directors or advisory committees; Novartis: Consultancy; Vertex: Other: Steering committee. Smith:Agios: Consultancy, Research Funding. Keefe:Novartis Pharmaceuticals Corporation, East Hanover, New Jersey, USA: Current Employment, Other: Eligible to receive stocks. Grosch:Novartis Pharma AG: Current Employment. Nassin:Novartis Pharmaceuticals Corporation, East Hanover, New Jersey, USA: Current Employment, Other: Eligible to receive stocks. Watson:Novartis: Current Employment. Yssel:Novartis Ireland Limited: Current Employment. Reshetnyak:Novartis: Current Employment.
Crizanlizumab is approved to reduce the frequency of or prevent recurrent vaso-occlusive crises in 16 years and older patients with sickle cell disease (SCD). In the STAND study, 12 years and older patients with SCD were treated with crizanlizumab. So, this abstract includes information or discussion of off-label use of crizanlizumab.