Introduction: Detection of measurable residual disease (MRD) in AML patients during remission is associated with adverse clinical outcomes after allogeneic hematopoietic cell transplant (alloHCT), including recent strong evidence from our group regarding residual NPM1 and/or FLT3-ITD variants (PMID: 36881031). Large studies examining the significance of other potential MRD targets, including isocitrate dehydrogenase isoform 2 ( IDH2), are needed. IDH2, which is mutated in approximately 12% of AML patients, is of particular interest due to the possibility of targeted clinical intervention.
Methods: Patients over the age of 18 in first complete remission (CR1) with IDH2 mutated AML undergoing alloHCT transplant at a CIBMTR site between 2013-2019 with remission blood samples within 100 days of alloHCT and available clinical data were included in this study. Residual variants in IDH2, NPM1, and FLT3genes were detected by ultrasensitive error-corrected next-generation sequencing (NGS-MRD) on genomic DNA from pre-conditioning blood and validated by digital droplet PCR (ddPCR). The primary outcomes were overall survival (OS) and cumulative incidence of relapse with non-relapse mortality as a competing risk. The day of transplant was considered as time 0, and the median follow-up time was calculated for censored patients. Kaplan-Meier estimation (log-rank tests), Cox proportional hazards models, and Fine-Gray regression models were fitted to examine the clinical outcomes.
Results: Among the 257 IDH2-mutated AML patients in this study, 57 (23%) experienced relapse, with 41 events occurring within 12 months after alloHCT. The median follow-up time was 25 months. Among 247 patients with pre-transplant remission flow cytometry results reported, 25% were positive, but no difference in rates of relapse or OS was observed between positive and negative patients.
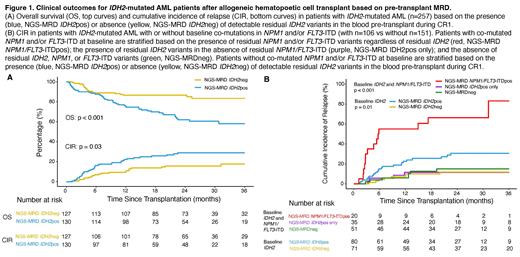
NGS MRD analysis detected residual IDH2 variants in remission samples of 130 patients (51%) with variant allele fraction (VAF) ranging from 0.05-56% (median: 3%), and 100% validation by ddPCR. NGS MRD IDH2 positive patients had increased rates of relapse (p = 0.03; 3yr: +11%, 95% CI: 0.2% to 22%) and decreased OS (p < 0.001; 3yr: -25%, 95% CI: -13% to -38%) compared to those who tested negative (Figure 1A). These OS differences were still observed between NGS MRD IDH2 positive and negative patients, regardless of age stratification (under 60yr p < 0.001, 3yr: -28%, 95% CI: -12% to -43%; over 60yr p = 0.04, 3yr: -19%, 95% CI: -1% to -40%); however, only patients over 60yrs had increased rates of relapse (p = 0.007; 3yr: +21, 95% CI: 6% to 36%).
The impact of co-mutation status was examined by subdividing the cohort based on the presence of NPM1 or FLT3-ITD mutations at baseline. Residual IDH2 variants in patients without baseline NPM1 or FLT3-ITD co-mutations (n = 151) were associated with decreased OS and increased relapse ( IDH2+ vs IDH2-; OS p = 0.005, 3yr: -23%, 95% CI: -6% to -40%; Relapse p = 0.01, 3yr: +19, 95% CI: 6% to 32%; Figure 1B). In contrast, residual IDH2 variants were not predictive of relapse in co-mutated patients (n=106, p = 0.5). In these patients, the only prognostic marker for relapse was NPM1 and/or FLT3-ITD MRD, with similar relapse risk between IDH2 only positive and MRD negative groups (p < 0.001; 3yr: 83% vs. 11% vs. 15%; Figure 1B).
In multivariable analysis, IDH2 MRD positivity was associated with decreased OS (HR 2.5, 95% CI: 1.5-4.2, p < 0.001) and increased rates of relapse (HR 2.1, 95% CI: 1.4-5.7, p = 0.003) after adjusting for other characteristics.
Conclusion: In this study, we demonstrate that adult patients with IDH2-mutated AML who have IDH2 variants detected in CR1 prior to first alloHCT experienced increased relapse rates and decreased overall survival. However, this association is significant only in patients without baseline NPM1 and FLT3-ITD mutations. In co-mutated patients, NPM1 and/or FLT3-ITD MRD serve as superior prognostic markers. Subgroup analyses show the potential influence of factors such as conditioning intensity and age on clinical outcomes. Nevertheless, larger studies with balanced subgroups and more comprehensive baseline mutational information, including IDH2 mutation subtype, are needed to better define the clinical relevance of IDH2 MRD in this context.
Disclosures
Andrew:Astra Zeneca: Current Employment. Auletta:Takeda: Membership on an entity's Board of Directors or advisory committees; National Marrow Donor Program: Current Employment; AscellaHealth: Membership on an entity's Board of Directors or advisory committees. El Chaer:Arog Pharmaceuticals: Research Funding; Novartis: Research Funding; MEI Pharma: Research Funding; BioSight: Research Funding; PharmaEssentia: Research Funding; Sanofi: Research Funding; Sumitomo Pharma Oncology: Consultancy, Research Funding; Fibrogen: Research Funding; Amgen: Consultancy, Research Funding; Bristol Myers Squib: Research Funding; Celgene: Research Funding; DAVA Oncology: Other: Travel grant; Association of Community Cancer Centers: Consultancy. Chen:Rigel: Consultancy; Abbvie: Consultancy. Corner:Bio-Rad Laboratories: Current Employment, Current holder of stock options in a privately-held company. Jimenez Jimenez:Abbvie: Research Funding. de Lima:Novartis: Other: Data Safety Monitoring Board; Bristol Myers Scribb: Membership on an entity's Board of Directors or advisory committees; Pfizer: Membership on an entity's Board of Directors or advisory committees; AbbVie: Other: Data Safety Monitoring Board; Miltenyi Biotec: Research Funding. Kebriaei:Jazz: Consultancy, Honoraria; Pfizer: Consultancy, Honoraria. Hourigan:Foundation of the NIH AML MRD Biomarkers Consortium: Research Funding.