Abstract
During cell death of human cultured leukocytes (Jurkat, HL-60, THP-1, U937) and freshly prepared leukocytes, we observed a greater than 100-fold increase in the affinity of apoptotic and necrotic cells for fluorescein isothiocyanate (FITC)–heparin in comparison with live cells. Binding of FITC-heparin was reversed in the presence of high ionic strength, unlabeled heparan sulfate, and heparin and pentosan polysulfate, but not in the presence of chondroitin and dermatan sulfates. During the course of cell death, the increase in the percentage of cells positive for annexin V binding correlated with the increase in the population positive for binding FITC-heparin. Confocal microscopy demonstrated that heparin binding to dead cells was restricted to 1 or 2 small domains on the surfaces of apoptotic cells and to larger, but still discrete, areas that did not localize with chromatin on ruptured necrotic cells. The heparin-binding domains originated from the nucleus and may correspond to the ribonucleoprotein-containing structures that have recently been shown to segregate within the nucleus of cells and to move onto the cell membrane. We observed that phagocytosis of dead Jurkat cells by monocyte-derived macrophages was blocked when the heparin-binding capacity of the dead cells was saturated by the addition of pentosan polysulfate. From this we concluded that the ability of dead cells to bind to heparan sulfate proteoglycans on the surfaces of macrophages may assist in phagocytic clearance.
Introduction
The first critical step in the clearance of apoptotic cells is the recognition by phagocytes of changes occurring on the surface of the dying cell. These “eat me” signals trigger binding and engulfment.1 A repertoire of receptors on the phagocytic surface are used to bind to these eat me signals, a prime example of which is a specific receptor for phosphatidylserine (PS) that is exposed on the outer membranes of cells early in apoptosis.
One group of cell surface receptors for which a role has yet to be established in the phagocytosis of apoptotic cells is the heparan sulfate proteoglycans (HSPGs), whose synthesis is up-regulated during macrophage differentiation.2-7 HSPGs have an established function in cell adhesion, and recent reports demonstrate involvement in the binding step during phagocytosis of latex beads by a number of cell lines.8,9 This opsonic property coincides with the well-documented ability of HPSGs to act as receptors for pathogenic bacteria, viruses, and protozoan parasites, and binding is often associated with the eventual internalization of the infective agent (reviewed in Dehio et al9).
The structural feature responsible for the action of HPSGs as receptors is the heparan sulfate chains. These provide a linearly arranged, high-negative charge capable of binding tightly to a wide variety of extracellular protein ligands.10 In the current study, we investigated whether HPSGs could be involved in the clearance of dying leukocytes by determining whether ligands for HPSGs occur on the cell surface during apoptosis. Fluorescein isothiocyanate (FITC)-labeled heparin was used as a probe because of the close structural similarity between heparin and heparan sulfate. We have observed that heparin does not bind with high affinity to live cells (defined as the dissociation constant (Kd) < 1 μM) but only to apoptotic and necrotic cells. Dying cells exhibit an enhanced affinity because of binding to discrete domains that arise within the nucleus during apoptosis, and they are released onto the plasma membrane during cell death. Finally, we have established that the phagocytosis of dead cells by monocyte-derived macrophages is blocked by pentosan polysulfate, a high-affinity ligand for the heparin-binding sites.
Materials and methods
Materials
Camptothecin and 7β-hydroxycholesterol were obtained from Sigma (Poole, United Kingdom); CD95 (Fas antibody, R and O Systems, United Kingdom); phycoerythrin (PE)-annexin V and viability dye 7-AAD (7-amino-actinomycin D, Via-Probe, CA) and other reagents for fluorescence-activated cell sorter (FACS) analysis were obtained from Becton Dickinson, CA; TAMRA 5-6-carboxytetramethyl-rhodamine-succinimidyl-ester was obtained from Molecular Probes (Eugene, OR); Vectashield mounting medium for fluorescence with DAPI was obtained from Vector Laboratories (Burlingame, CA), and Mowiol from Calbiochem (United Kingdom). Recombinant unlabeled annexin V was obtained from Dr T. R. Hawthorne (Novartis, Basel, Switzerland); FITC-labeled anti-human CD14 and CD45 and the respective isotype controls were obtained from Sigma.
Unfractionated porcine heparin (Mr, 15 kd) was obtained from Pharmacia Upjohn (Sweden), and pharmaceutical preparations of low-molecular–weight heparin (LMWH) were obtained as follows: Certoparin (7 kd), Novartis; Fragmin (6 kd), Pharmacia Upjohn; Fraxiparin (4.5 kd) and CY222 (3.5 kd), Sanofi (France); and Bemiparin (3 kd), Laboratorios Farmaceuticos ROVI S.A. (Spain). Heparan sulfate (30 kd; Laboratorio Derivati Organici, Italy) and pentosan polysulfate (3.5 kd, SP 54, Benechemie, Germany) were kindly supplied by Dr B. Mulloy (NIBSC, Herts, United Kingdom). Chondroitin sulfate A and C were purchased from Sigma, and dermatan sulfate was obtained from Mediolanum Farmaceuti (Italy). FITC-labeled unfractionated heparin and FITC-LMWH (labeled Bemiparin) were prepared by Dr F. Wusteman (School of Molecular Medicine and Biosciences, University of Wales, Cardiff). In brief, free amino groups on the heparin were acetylated, and free reducing ends were coupled to diaminoethane using pyridine:borohydride as a reducing agent. This material was labeled with FITC and was purified by repeated purification and ion exchange chromatography on Dowex 1. No loss in anticoagulant activity was observed after the labeling. All other chemicals used were of analytical grade and were obtained from Sigma.
Cell culture
Human leukemia cells Jurkat, HL-60, THP-1, and U937 were obtained from the American Type Culture Collection (ATCC; Rockville, MD). Cells were cultured in suspension in RPMI 1640 medium (Sigma) supplemented with 10% heat-inactivated fetal calf serum (Harlan Sera Laboratories, United Kingdom), 100 U/mL penicillin G, 100 U/mL streptomycin, and 2 mM l-glutamine. β-mercaptoethanol was added to the culture medium of THP-1 cells according to ATCC recommendations. The culture was kept in a humidified incubator with 95% air and 5% CO2 at 37°C and was split every 3 to 4 days to ensure logarithmic growth to a maximum density of 106 cells/mL. After transfer to fresh medium containing 5% fetal calf serum, the cells were treated with either Camptothecin (stock prepared in dimethyl sulfoxide), 7β-hydroxycholesterol (stock prepared in ethanol), or Fas antibody. Control cells were prepared by the addition of appropriate vehicle, alone.
For flow cytometric experiments involving freshly prepared leukocytes, blood was obtained from human unmedicated volunteers after informed consent. Approximately 50 mL blood was taken by venipuncture into 0.38% sodium citrate and was mixed with 6% dextran (1:4 vol/vol). After 60 minutes at room temperature, the supernatant was removed and an equal volume of HEPES buffer was added. Cells were removed by centrifugation at 400g for 8 minutes. Lysis was performed by adding 1 mL 0.25% NaCl to the pellet and was followed immediately by 1 mL 1.6% NaCl. Cells were washed with HEPES buffer and resuspended in RPMI 1640 medium before treatment with apoptotic agents as described above. The separated cells were mostly granulocytes during FACS analysis.
Cell morphology
Cytospin preparations of cells were fixed in absolute methanol and stained with Giemsa-May-Grünwald. Cell morphology was evaluated by light microscopy using Olympus AH-2 equipment (objective ×20, ×40, ×60, ×100).
Flow cytometry
Cells were washed twice with complete RPMI 1640 medium and were resuspended at an approximate density of 1 × 106cells/mL. Aliquots (100 μL) of the cell suspension were diluted 10-fold with HEPES buffer (20 mM HEPES, 137 mM NaCl, 2.0 mM KCl, 5.6 mM glucose, 1.0 mM MgCl2, 1 g/L bovine serum albumin, pH 7.2). Various concentrations of FITC-heparin were prepared with the cells, and samples were incubated in the dark at 4°C for 10 minutes before washing once in annexin V binding buffer (10 mM HEPES, 140 mM NaCl, 2.5 mM CaCl2, pH 7.4). PE–annexin V and 7-AAD were added according to the manufacturer's instructions, and samples were immediately analyzed using a Becton Dickinson FACSCalibur flow cytometer calibrated using fluorescent beads. Acquisition processing of data from 10 000 cells was carried out during each experiment. TheKd for binding to dead cells was determined from triplicate values of relative fluorescence intensity (RFI) obtained at dilutions of FITC-heparin from 0.04 to 1.3 μM that were fit to a single-site ligand-binding equation using Enzfitter (Sigma).
Cell sorting
Cells were labeled with annexin V and 7-AAD, as described above, and were sorted into live, apoptotic, and necrotic fractions by a FACSVantage SE cell sorter (Becton Dickinson). The minimum number of cells collected into RPMI 1640 medium was 40 000 in each confocal microscopy sample.
Sorted cells were resuspended in HEPES buffer before the addition of FITC-heparin (1 μM). After 10 minutes on ice, cells were washed once in annexin V binding buffer and were relabeled with PE–annexin V and 7-AAD. The cell suspension was then mixed with Mowiol in a 1:5 (vol/vol) proportion before they were mounted onto glass slides. Confocal laser scanning microscopy was performed using a Bio-Rad MRC 1024 equipped with a krypton-argon laser in conjunction with a Nikon Eclipse 600 microscope (objective ×60). Eight thin horizontal planes of sections were made, each 1 μm apart (zoom factor, 3.23). A standard FITC filter set combined with the 488-nm laser line was used to visualize FITC-labeled heparin-binding sites, whereas a Texas Red filter set combined with the 588-nm laser line enabled localization of areas that bound PE–annexin V (cell membrane) and 7-AAD (intracellular distribution).
Fluorescence microscopy
Cells were sorted as described above and were labeled with FITC-heparin at a final concentration of 1 μM for 10 minutes. After one wash with HEPES buffer, the cells were stained with DAPI, and glass slides were prepared. Fluorescence microscopy was performed using a Zeiss Axioshop, and images were captured using Quips-FISH application (Vysis, United Kingdom).
Heparin binding to isolated nuclei
Jurkat cells were treated with Camptothecin and were isolated according to the procedure of Martelli et al.11 In brief, cells were resuspended to 1.5 × 107/mL in TM-2 buffer (10 mM Tris, pH 7.4, 2 mM MgCl2, 0.5 mM phenylmethylsulfonyl fluoride, 1 μg/mL aprotinin, 1 μg/mL leupeptin) and were incubated for 5 minutes on ice. Triton X-100 was added at 0.5% (wt/vol), and the cell suspension was sheared by one passage through a 21-gauge needle. Nuclei were sedimented at 400g for 6 minutes, washed once in TM-2 buffer, and resuspended in 1 mL HEPES buffer before FITC-heparin (final concentration, 1μM) was added. After 10 minutes, the nuclei were washed once in buffer containing 10 mM Tris-HCl, pH 7.4, 0.25 M sucrose, 5 mM MgCl2, and 1 μg/mL aprotinin and leupeptin. A sample of nuclei in suspension was transferred to a glass slide, stained with DAPI, and examined by fluorescence microscopy as described above.
Influence of the enhanced heparin affinity of dead cells on phagocytosis
Monocyte-derived macrophages (MDMs) were separated from human fresh blood using Lymphoprep density gradient medium (Nycomed, Oslo, Norway) and were cultured on Permanox chamber slides (Lab-Tek, United Kingdom) in the presence of 10% autologous serum.7Live Jurkat cells were incubated with TAMRA as described previously.12 Half the Jurkat cells labeled with TAMRA (JurkatT) were treated with Camptothecin for 30 hours. Live and dead cell preparations were added (4 × 105cells/mL) to the chambers culturing MDMs. After 60-minute incubation at 37°C, the supernatant was removed and MDM monolayers were washed with PBS containing 0.3% immunoglobulin G–free bovine serum albumin and 0.15% NaN3 at 4°C. MDMs were then labeled with FITC-labeled anti-human CD14 at 4°C in the dark for 45 minutes. The supernatant was removed, and cells were washed in PBS and were subjected to laser scanning cytometry using a laser scanning cytometer (CompuCyte, MA) connected to a BX50 fluorescence microscope (Olympus, NJ).13 Slides containing MDM monolayers were moved through a 488-nm laser line on a computer-controlled motorized stage. Differentially treated areas on the microscope slide were scanned individually by using the ×20 objective and 5-mW laser output. Fluorescence from FITC-labeled CD14 and TAMRA were collected using photomultiplier tubes protected by, respectively, a 530/30 bandpass filter and a 580/30 bandpass filter. Cells were defined on the basis of their FITC-staining and threshold level (fluorescence above background), which were optimized so that as many single cells as possible could be contoured without losing fluorescence information. For each event, fluorescence integral, area, and maximum pixel were calculated. Cell clumps were excluded based on a plot of cell area versus maximum pixel, and a plot of green versus orange integral fluorescence was used to quantify the percentages of phagocytosed TAMRA-labeled Jurkat cells. At least 1000 contoured events were recorded for each treatment area.
Data analysis
Data obtained during flow cytometry were analyzed using WinMDI version 2.8 computer software (Scripps Research Institute, La Jolla, CA), where RFI was calculated as a Gmean. Microsoft Excel was used to calculate mean values and standard error of the mean (SEM). Each experiment was repeated at least 3 times. Data for laser scanning cytometry were analyzed on a Hewlett Packard (Palo Alto, CA) computer using WinCyte 3.4 software (CompuCyte).
Results
Binding of heparin to live, apoptotic, and necrotic cells
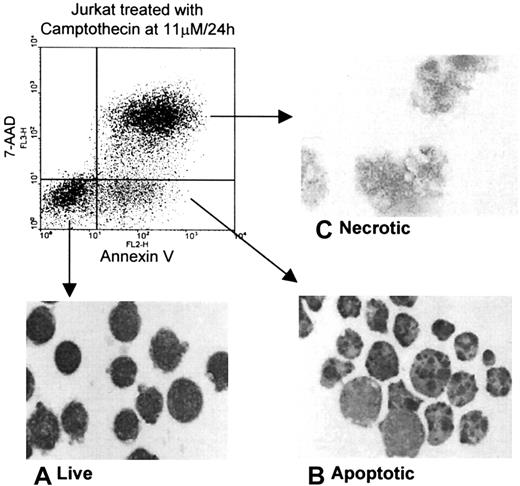
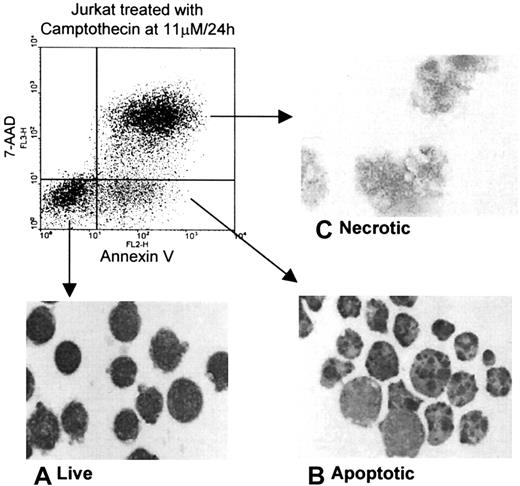
Heparin binding by leukocytic cells undergoing cell death induced by a number of agents was determined with each of 4 cell lines, namely, Jurkat, THP-1, U937, and HL-60. Live, apoptotic, and secondary necrotic cells were discriminated according to the binding of PE–annexin V and the uptake of 7-AAD, as described in “Materials and methods.” When these parameters were used to sort the cells, the typical morphology of live, apoptotic, and necrotic cells was observed by light microscopy as shown in the inserted micrographs in Figure1.
Morphology of each population of live, apoptotic, and necrotic Jurkat cells after separation by cell sorting.
Jurkat cells (1 × 107) were treated with Camptothecin for 24 hours and were separated according to the binding of PE–annexin V and the uptake of 7-AAD into live, apoptotic, and necrotic populations by cell sorting using a FACSVantage machine and were stained with Giemsa-May-Grünwald. Typical morphology of each population was determined by light microscopy, as shown in the insets: (A) live cells with intact membrane and a rim of cytoplasm; (B) apoptotic cells with characteristic apoptotic bodies; (C) necrotic cells with swollen organelles and loss of a discrete cell membrane.
Morphology of each population of live, apoptotic, and necrotic Jurkat cells after separation by cell sorting.
Jurkat cells (1 × 107) were treated with Camptothecin for 24 hours and were separated according to the binding of PE–annexin V and the uptake of 7-AAD into live, apoptotic, and necrotic populations by cell sorting using a FACSVantage machine and were stained with Giemsa-May-Grünwald. Typical morphology of each population was determined by light microscopy, as shown in the insets: (A) live cells with intact membrane and a rim of cytoplasm; (B) apoptotic cells with characteristic apoptotic bodies; (C) necrotic cells with swollen organelles and loss of a discrete cell membrane.
The binding of FITC-heparin to live, apoptotic, and necrotic Jurkat cells is shown in Figure 2. No binding was observed to live cells except for a slight increase in RFI at 5 μM FITC-heparin. In contrast, enhanced binding was observed to apoptotic and necrotic cells at all concentrations of FITC-heparin tested. The RFI reached a maximum at 5 μM FITC-heparin (tested up to 20 μM FITC-heparin, data not shown), and in comparison with live cells, it was an order of magnitude higher for apoptotic cells and more than 2 orders of magnitude higher for necrotic cells. TheKd for binding of FITC-heparin to dead cells was determined as 259 nM (data not shown). Binding was rapid (complete within 1 minute), reversed by the inclusion of 0.8 M NaCl in the heparin binding buffer, and independent of calcium (data not shown).
Flow cytometric analysis of the binding of FITC-heparin to live, apoptotic, and necrotic cells derived from cultured Jurkat T cells.
Jurkat cells were treated with Camptothecin for 24 hours before labeling with FITC-heparin at a range of concentrations (0.5 nM-5000 nM). Cells were washed and labeled with PE–annexin V and 7-AAD, as described in “Materials and methods.” Live, apoptotic, and necrotic cells were discriminated by FACS analysis, and binding at each concentration of FITC-heparin is shown as relative fluorescence intensity on the x-axis (log scale).
Flow cytometric analysis of the binding of FITC-heparin to live, apoptotic, and necrotic cells derived from cultured Jurkat T cells.
Jurkat cells were treated with Camptothecin for 24 hours before labeling with FITC-heparin at a range of concentrations (0.5 nM-5000 nM). Cells were washed and labeled with PE–annexin V and 7-AAD, as described in “Materials and methods.” Live, apoptotic, and necrotic cells were discriminated by FACS analysis, and binding at each concentration of FITC-heparin is shown as relative fluorescence intensity on the x-axis (log scale).
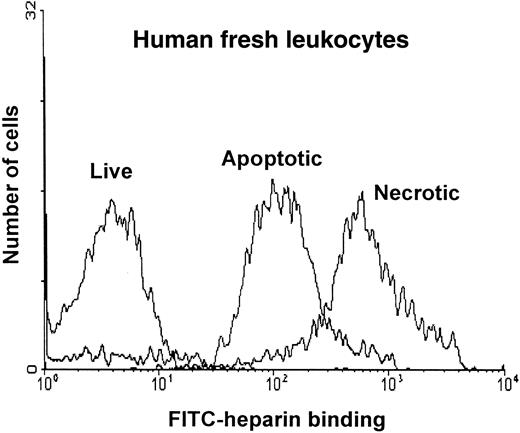
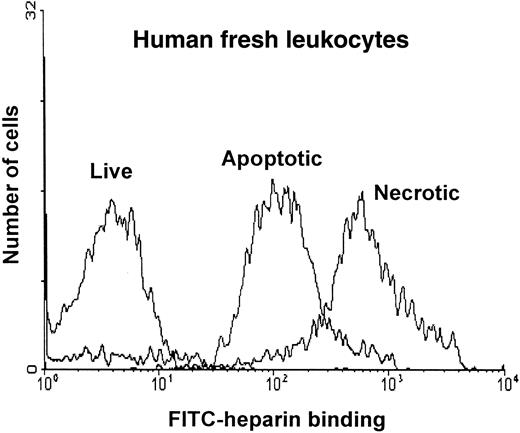
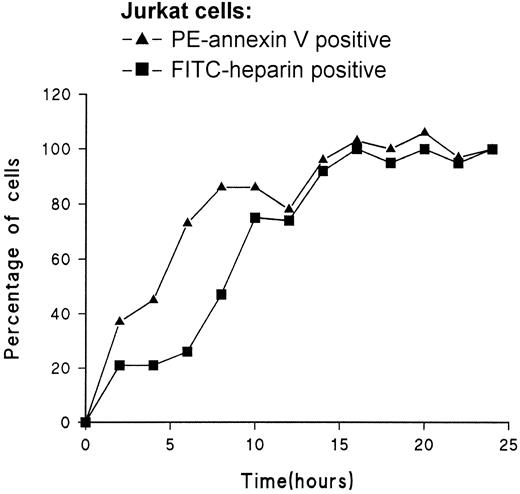
A summary of the results obtained with each of the cell lines is shown in Table 1. RFI values were determined for each of the populations at a single concentration of FITC-heparin (500 nM). The mean increase in RFI for apoptotic cells over live cells was 10-fold; for necrotic cells, it was more than 100-fold. A similar increase in RFI was observed during apoptosis of leukocytes prepared from fresh blood, as shown in Figure 3. The appearance of FITC–heparin-positive cells and PE–annexin V–positive cells was compared in timed samples taken during apoptosis of Jurkat cells (Figure 4). At later time points, good agreement was observed between the percentage of cells found to be PE–annexin V positive and the percentage of FITC-heparin positive cells. Correlation was not as good in the early phase of the study, possibly because of a degree of overlap between the binding of FITC-heparin by apoptotic and live cells (Figure 2).
Flow cytometric analysis of the binding of FITC-heparin to live, apoptotic, and necrotic cells derived from freshly prepared leukocytes.
Leukocytes were prepared from fresh blood and were treated with Camptothecin for 16 hours, as described in “Materials and methods.” Cells were labeled with FITC-heparin at a range of concentrations (0.5 nM-5000 nM) and then with PE–annexin V and 7-AAD. Live, apoptotic, and necrotic cells were discriminated by FACS analysis. Histogram plots of the binding to each population at 5 μM FITC-heparin are shown as relative fluorescence intensity on the x-axis.
Flow cytometric analysis of the binding of FITC-heparin to live, apoptotic, and necrotic cells derived from freshly prepared leukocytes.
Leukocytes were prepared from fresh blood and were treated with Camptothecin for 16 hours, as described in “Materials and methods.” Cells were labeled with FITC-heparin at a range of concentrations (0.5 nM-5000 nM) and then with PE–annexin V and 7-AAD. Live, apoptotic, and necrotic cells were discriminated by FACS analysis. Histogram plots of the binding to each population at 5 μM FITC-heparin are shown as relative fluorescence intensity on the x-axis.
Time course correlating the exposure of phosphatidylserine by cells during cell death with enhanced binding of FITC-heparin.
Jurkat cells were treated with Camptothecin, and samples were taken at timed intervals for labeling with PE–annexin V and FITC-heparin (500 nM). The results show the correlation between the fraction of cells with exposed PS (enhanced PE–annexin V binding ▴-▴) to the fraction of cells binding FITC-heparin with an RFI that was 10-fold higher than untreated cells (▪-▪). Counted cells are expressed as a percentage of PE–annexin V–positive or FITC-heparin–positive cells in the 24-hour sample.
Time course correlating the exposure of phosphatidylserine by cells during cell death with enhanced binding of FITC-heparin.
Jurkat cells were treated with Camptothecin, and samples were taken at timed intervals for labeling with PE–annexin V and FITC-heparin (500 nM). The results show the correlation between the fraction of cells with exposed PS (enhanced PE–annexin V binding ▴-▴) to the fraction of cells binding FITC-heparin with an RFI that was 10-fold higher than untreated cells (▪-▪). Counted cells are expressed as a percentage of PE–annexin V–positive or FITC-heparin–positive cells in the 24-hour sample.
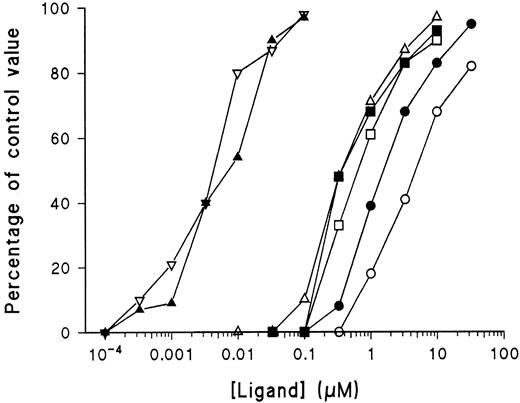
Figure 5 depicts the observations made on the ability of unlabeled heparan sulfate, pentosan polysulfate, and various molecular weights of heparin to block the binding of FITC-heparin to necrotic cells. FITC-LMWH was used for these experiments because it was observed in preliminary experiments that this has a weaker affinity for cells than FITC-heparin. As a block for the binding of FITC-LMWH, IC50 decreased with increased molecular weight (Table 2). Affinity for dead cells was reduced as the molecular weight of heparin was decreased, consistent with findings of previous reports regarding the binding of heparin to proteins, such as platelet factor 4.14 The IC50 of pentosan polysulfate (3.5 kd) was similar to that of unfractionated heparin. The ability of pentosan polysulfate to bind with high affinity despite its low molecular weight is attributed to the high-charge density of pentosan polysulfate (3.5 sulfate groups per disaccharide as opposed to 2.4-2.8 sulfate groups per disaccharide for heparin). Heparan sulfate, which has a lower degree of sulfation than heparin (0.8-1.8 sulfate groups per disaccharide) gave an IC50 value of 0.3 μM.15 Chondroitin sulfates A and C and dermatan sulfate had no effect on the binding of FITC-LMWH when tested up to 15 μM. These experiments demonstrate the specificity of heparin binding and rule out a contribution to the binding of the single FITC reporter moiety.
Inhibition of FITC-LMWH binding to dead cells by heparan sulfate, pentosan polysulfate, and heparin of various molecular weight forms.
Necrotic Jurkat cells (induced by Camptothecin and discriminated by FACS analysis, as described in Figure 1) were preincubated with increasing concentrations of these heparin-like ligands—heparan sulfate, pentosan polysulfate, unfractionated heparin (average Mr, 15 kd), and pharmaceutical preparations of depolymerized heparin of various average molecular weights (as listed in “Materials and methods”). After 60 minutes, FITC-LMWH was added at 1 μM, and incubation continued for another 10 minutes. Cells were then labeled with PE–annexin V and 7-AAD, and the RFI of the necrotic population was determined by FACS analysis as in Figure 2. The RFI at each concentration of competitive ligand was expressed as a percentage of the RFI of cells in its absence. (▪-▪), heparan sulfate; (▿-▿), unfractionated heparin; (▵-▵), 7 kd LMWH; (□-□), 6 kd LMWH; (●-●), 4.5 kd LMWH; (○-○), 3.5 kd LMWH; and (▴-▴), pentosan polysulfate.
Inhibition of FITC-LMWH binding to dead cells by heparan sulfate, pentosan polysulfate, and heparin of various molecular weight forms.
Necrotic Jurkat cells (induced by Camptothecin and discriminated by FACS analysis, as described in Figure 1) were preincubated with increasing concentrations of these heparin-like ligands—heparan sulfate, pentosan polysulfate, unfractionated heparin (average Mr, 15 kd), and pharmaceutical preparations of depolymerized heparin of various average molecular weights (as listed in “Materials and methods”). After 60 minutes, FITC-LMWH was added at 1 μM, and incubation continued for another 10 minutes. Cells were then labeled with PE–annexin V and 7-AAD, and the RFI of the necrotic population was determined by FACS analysis as in Figure 2. The RFI at each concentration of competitive ligand was expressed as a percentage of the RFI of cells in its absence. (▪-▪), heparan sulfate; (▿-▿), unfractionated heparin; (▵-▵), 7 kd LMWH; (□-□), 6 kd LMWH; (●-●), 4.5 kd LMWH; (○-○), 3.5 kd LMWH; and (▴-▴), pentosan polysulfate.
Localization of binding sites for FITC-heparin by confocal and fluorescence microscopy
Confocal microscopy of the FITC–heparin-labeled live, apoptotic, and necrotic Jurkat cells prepared by sorting confirmed that live cells do not bind heparin (Figure 6 [1A]). On apoptotic cells, 1 or 2 discrete domains of heparin binding were observed at the cell surface (Figure 6 [1B]). In cells that had membranes that were damaged but unruptured, a broader region of heparin binding was seen, though this was still discrete (Figure 6 [1C]). Heparin binding to ruptured necrotic cells was to discrete domains that exhibited high fluorescence intensity that did not coincide with the redness of chromatin present as lobules (Figure 6 [1D]) or as a residue (Figure 6 [1E]). Further histologic investigation by fluorescence microscopy confirmed that the sites responsible for heparin binding arose as discrete domains that were not present in live cells (Figure 6 [2A]) but that developed within the nucleus (stained with DAPI) during apoptosis. (Figure 6 [2B-C]). During the course of cell death, these domains became separated from the chromatin (Figure 6 [2C]) and eventually were attached to the cell membrane (Figure 6 [2B-D]) or appeared alongside the residual chromatin on the membrane of necrotic cells (Figure 6 [2E]). These domains were also observed in nuclei from cells harvested at earlier time points. Staining of the nuclei with FITC-heparin and DAPI medium showed no binding to nuclei from live cells (Figure 6 [3A]). In the first sample taken at 30 minutes, 1 or 2 larger areas of relatively less intense binding of heparin were observed (Figure 6 [3B]). In later samples at 1 and 2 hours, several discrete smaller domains of higher intensity were more common (Figure 6 [3C-D]). Nuclear material isolated at 4 and 6 hours showed lobulated nuclei that exhibited high-intensity binding to large domains that were separated from the DAPI-positive material (Figure 6 [3E-F]). During this series of experiments, the addition of excess unlabeled heparin blocked the fluorescence signal.
FITC-labeled heparin binding to live, apoptotic, and necrotic Jurkat cells and to nuclei prepared from Jurkat cells as determined by fluorescence microscopy.
Cell death was induced by Camptothecin, and cells were separated into live, apoptotic, and necrotic populations by cell sorting. The upper line of micrographs [1] shows typical examples of the binding of FITC-LMWH to each population, as observed by confocal microscopy. [1A] Live cells, [1B] apoptotic cells, [1C] unlysed necrotic cells, and [1D-E] lysed necrotic cells. FITC-LMWH is seen as green fluorescence, and the red fluorescence resulted from binding of PE–annexin V and 7-AAD. The middle line of micrographs [2] shows the binding of FITC-LMWH as determined by fluorescence microscopy. DAPI, (blue fluorescence); FITC-heparin (green). [2A] Live cells, [2B] apoptotic cells, [2C] unlysed necrotic cells, and [2D-E] lysed necrotic cells. The lower line of micrographs [3] shows FITC-heparin binding to purified nuclei prepared at timed intervals after the addition of Camptothecin. Nuclei were stained with FITC-heparin (green) and DAPI (blue). [3A] Zero time, [3B] 30 minutes, [3C] 1 hour, [3D] 2 hours, [3E] 4 hours, and [3F] 6 hours.
FITC-labeled heparin binding to live, apoptotic, and necrotic Jurkat cells and to nuclei prepared from Jurkat cells as determined by fluorescence microscopy.
Cell death was induced by Camptothecin, and cells were separated into live, apoptotic, and necrotic populations by cell sorting. The upper line of micrographs [1] shows typical examples of the binding of FITC-LMWH to each population, as observed by confocal microscopy. [1A] Live cells, [1B] apoptotic cells, [1C] unlysed necrotic cells, and [1D-E] lysed necrotic cells. FITC-LMWH is seen as green fluorescence, and the red fluorescence resulted from binding of PE–annexin V and 7-AAD. The middle line of micrographs [2] shows the binding of FITC-LMWH as determined by fluorescence microscopy. DAPI, (blue fluorescence); FITC-heparin (green). [2A] Live cells, [2B] apoptotic cells, [2C] unlysed necrotic cells, and [2D-E] lysed necrotic cells. The lower line of micrographs [3] shows FITC-heparin binding to purified nuclei prepared at timed intervals after the addition of Camptothecin. Nuclei were stained with FITC-heparin (green) and DAPI (blue). [3A] Zero time, [3B] 30 minutes, [3C] 1 hour, [3D] 2 hours, [3E] 4 hours, and [3F] 6 hours.
Influence of the heparin affinity of dead cells on phagocytosis
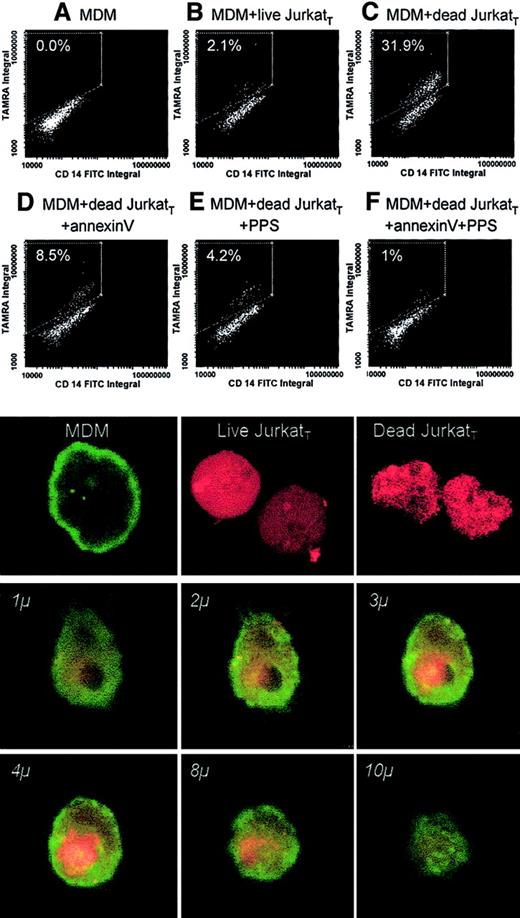
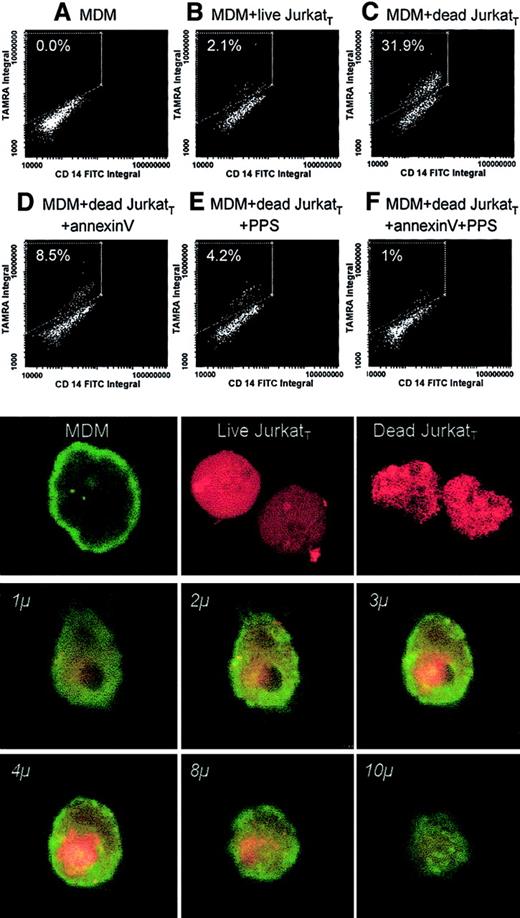
Phagocytosis was determined by the incorporation of TAMRA-labeled Jurkat cells into monolayers of MDM using laser scanning cytometry. When incubated with dead Jurkat cells, 31.9% of MDM were positive for TAMRA (Figure 7C) compared with only 2.1% in the presence of live cells (Figure 7B). When the dead cells were preincubated with annexin V (400 μg/mL for 15 minutes), the incorporation was reduced to 8.5% in agreement with the known importance of PS exposure as a ligand for the phagocytosis of dead cells (Figure 7D). The incorporation was reduced to 4.2% when cells were preincubated with pentosan polysulfate at a concentration that would block available heparin binding sites (2 μM) (Figure 7E). The observed reduction shows that the heparin-binding sites play a significant role in the uptake of dead cells, presumably through the interaction with macrophage HPSGs. The level of incorporation was reduced to 1% when pentosan polysulfate and annexin V were combined (Figure 7F).
Influence of the heparin affinity of dead cells on phagocytosis.
Live or dead Jurkat cells labeled with TAMRA (JurkatT) were incubated with human monocyte–derived macrophages (MDMs) cultured on Permanox slides. Analysis of the monolayers for the population of cells that were positive for FITC–anti-CD14 and for TAMRA was carried out by laser scanning cytometry and confocal microscopy. (upper panels) Results obtained by laser scanning cytometry in experiments carried out in the absence of JurkatT cells (A), in the presence of live JurkatT cells (B), and in the presence of dead JurkatT cells incubated without additions (C) or together with unlabeled annexin V (D), pentosan polysulfate (E), or a combination of annexin V and pentosan polysulfate (F). (lower panels) Phagocytosis of JurkatT under these experimental conditions by confocal microscopy. (top line, left to right) MDMs stained with FITC–anti-CD14 (green), live and dead JurkatT cells, respectively, labeled with TAMRA (red). (lower 6 panels) Series of sections taken through MDM after engulfment of a dead JurkatT cell. The depth of each section is marked in italics (objective, ×60; zoom factor, 5.0).
Influence of the heparin affinity of dead cells on phagocytosis.
Live or dead Jurkat cells labeled with TAMRA (JurkatT) were incubated with human monocyte–derived macrophages (MDMs) cultured on Permanox slides. Analysis of the monolayers for the population of cells that were positive for FITC–anti-CD14 and for TAMRA was carried out by laser scanning cytometry and confocal microscopy. (upper panels) Results obtained by laser scanning cytometry in experiments carried out in the absence of JurkatT cells (A), in the presence of live JurkatT cells (B), and in the presence of dead JurkatT cells incubated without additions (C) or together with unlabeled annexin V (D), pentosan polysulfate (E), or a combination of annexin V and pentosan polysulfate (F). (lower panels) Phagocytosis of JurkatT under these experimental conditions by confocal microscopy. (top line, left to right) MDMs stained with FITC–anti-CD14 (green), live and dead JurkatT cells, respectively, labeled with TAMRA (red). (lower 6 panels) Series of sections taken through MDM after engulfment of a dead JurkatT cell. The depth of each section is marked in italics (objective, ×60; zoom factor, 5.0).
Discussion
We have observed that in comparison with healthy leukocytes, apoptotic and necrotic leukocytes have a high affinity for heparin—defined as acting according to aKd of less than 1 μM. AKd of 259 nM was determined, similar to that previously reported for the binding of heparin to U937 cells.16 In that study and the other studies that have used radiolabeled heparin, it was not possible to determine whether binding was to live or dead cells.17-19 It may well be the case that the observed high-affinity binding of radiolabel was to a small fraction of apoptotic or necrotic cells that occur during culture and that may also be generated during experimental manipulation. We have confirmed our conclusion that live cells do not bind with high affinity to heparin with other cell types, including endothelial cells (M.A.G. et al, unpublished observations, 2000) and the pancreatic carcinoma cell line, MIA PaCa2.20 Our conclusion that live cells are relatively weak in binding heparin is in accord with the report of Harenberg et al,21 who investigated heparin binding to leukocytes in fresh blood. The highKd of live cells would also agree with the affinity of heparin for L-selectin, which is in the micromolar range.22,23 The lack of dependency on Ca++ for high-affinity binding to dead cells rules out any contribution of L-selectin.24
When we investigated the binding of heparin by confocal microscopy, we observed that binding occurred to discrete areas on the membrane of apoptotic cells (Figure 6 [1B]) or were separated from chromatin in necrotic cells. The development of focused, highly intense regions of heparin binding was confirmed by conventional fluorescence microscopy. The source of the heparin binding material appears to be the nucleus because the nuclei in live cells do not bind heparin. Early in the apoptotic process, however, a large binding domain was formed within the nucleus (Figure 6 [3B]). The intensity of heparin binding was considerably enhanced when it occurred outside the nucleus, indicating a lack of accessibility to binding proteins when located within the nucleus, perhaps because of the presence of other ligands.
This finding of discrete domains of nuclear material segregating during apoptosis corresponds closely to structures recently described as clusters of ribonucleoproteins,25,26 for which the term HERDS (heterogeneous ectopic ribonucleoprotein-derived structures) has been coined.27 These proteins are normally distributed throughout the nucleus in the nuclear matrix, but during apoptosis they form into small fibrillogranular structures that pass into the cytoplasm and are eventually extruded at the cell surface in membrane-bound blebs.28-32 The ribonucleoproteins are obvious candidates as heparin-binding proteins because many are highly basic proteins and contain sequences that confer high affinity for heparin.33
Our findings demonstrate that the heparan sulfate–binding property of apoptotic cells may be of physiological significance in assisting phagocytic clearance. The exposure of PS is well established as a signal for the phagocytosis of apoptotic cells, a mechanism that can be blocked by the presence of annexin V.34 Macrophages are known to express HSPGs that have been observed to play a role in the phagocytosis of latex beads.8 9 We have now shown that the phagocytosis of dead cells can be effectively blocked by saturation of the heparin-binding sites with pentosan polysulfate, a highly potent inhibitor of heparin binding to nonviable cells. Moreover, because the exposure of areas with high affinity for heparin occurs early in apoptosis, coincidentally with the exposure of PS (Figure 4), HPSG binding may make a significant contribution to the clearance mechanism. If this is the case, then heparin treatment may reduce the rate of removal of dying cells.
We thank Dr M. Ormerod (Institute of Cancer Research, Sutton, United Kingdom) for helpful discussions and for critical reading of the manuscript, Dr F. S. Wusteman (School of Molecular Medicine and Biosciences, University of Wales, Cardiff) for synthesis of fluorescein-labeled heparin, Dr Barbara Mulloy (Laboratory for Molecular Structure, National Institute for Biological Standards and Control, Potters Bar, United Kingdom) for gifts of heparan sulfate and pentosan polysulfate, and Dr T. R. Hawthorne (Novartis) for the gift of recombinant annexin V.
Supported by a grant from the British Heart Foundation (PG/98/82). No commercial support has been received for this study.
The publication costs of this article were defrayed in part by page charge payment. Therefore, and solely to indicate this fact, this article is hereby marked “advertisement” in accordance with 18 U.S.C. section 1734.
References
Author notes
Michael F. Scully, Thrombosis Research Institute, Emmanuel Kaye Building, Coagulation and Fibrinolysis Laboratory, 1B Manresa Rd, Chelsea, London SW3 6LR, United Kingdom; e-mail:mscully@tri-london.ac.uk.



![Fig. 6. FITC-labeled heparin binding to live, apoptotic, and necrotic Jurkat cells and to nuclei prepared from Jurkat cells as determined by fluorescence microscopy. / Cell death was induced by Camptothecin, and cells were separated into live, apoptotic, and necrotic populations by cell sorting. The upper line of micrographs [1] shows typical examples of the binding of FITC-LMWH to each population, as observed by confocal microscopy. [1A] Live cells, [1B] apoptotic cells, [1C] unlysed necrotic cells, and [1D-E] lysed necrotic cells. FITC-LMWH is seen as green fluorescence, and the red fluorescence resulted from binding of PE–annexin V and 7-AAD. The middle line of micrographs [2] shows the binding of FITC-LMWH as determined by fluorescence microscopy. DAPI, (blue fluorescence); FITC-heparin (green). [2A] Live cells, [2B] apoptotic cells, [2C] unlysed necrotic cells, and [2D-E] lysed necrotic cells. The lower line of micrographs [3] shows FITC-heparin binding to purified nuclei prepared at timed intervals after the addition of Camptothecin. Nuclei were stained with FITC-heparin (green) and DAPI (blue). [3A] Zero time, [3B] 30 minutes, [3C] 1 hour, [3D] 2 hours, [3E] 4 hours, and [3F] 6 hours.](https://ash.silverchair-cdn.com/ash/content_public/journal/blood/99/6/10.1182_blood.v99.6.2221/6/m_h80622273006.jpeg?Expires=1766054049&Signature=JkYEnVpofdPqLz5ugSmOTCy8E0oHsR2iDdRlZL2FgsLC9pVM0sJfgK-hWRe0tBN6JmKZHhV-dornoacgoPtAu4BSRSgFlbe7-Lt4V3dbTh-4nx4aJPN4kBgm5V0gYjlHxwFldUZijt2PzzRZ1DGsCRMHY1E2mI0A5egLEMhXWnTuiAeCQ26K0h0G2mJIwBvP6VLq357loh34PmI3ZZ65d02Snm5nxzovEVG~IMMqn9EDYjnO8p1osBnN9p-twHyhpy31tT0Dz12RSwSXZQTQySpDwQFgKRrC2zGdvuzzMTP1fNqMJc9Bn6QOFhKWb5qBrTYrSlQHxEhAem8hWuE0QQ__&Key-Pair-Id=APKAIE5G5CRDK6RD3PGA)



![Fig. 6. FITC-labeled heparin binding to live, apoptotic, and necrotic Jurkat cells and to nuclei prepared from Jurkat cells as determined by fluorescence microscopy. / Cell death was induced by Camptothecin, and cells were separated into live, apoptotic, and necrotic populations by cell sorting. The upper line of micrographs [1] shows typical examples of the binding of FITC-LMWH to each population, as observed by confocal microscopy. [1A] Live cells, [1B] apoptotic cells, [1C] unlysed necrotic cells, and [1D-E] lysed necrotic cells. FITC-LMWH is seen as green fluorescence, and the red fluorescence resulted from binding of PE–annexin V and 7-AAD. The middle line of micrographs [2] shows the binding of FITC-LMWH as determined by fluorescence microscopy. DAPI, (blue fluorescence); FITC-heparin (green). [2A] Live cells, [2B] apoptotic cells, [2C] unlysed necrotic cells, and [2D-E] lysed necrotic cells. The lower line of micrographs [3] shows FITC-heparin binding to purified nuclei prepared at timed intervals after the addition of Camptothecin. Nuclei were stained with FITC-heparin (green) and DAPI (blue). [3A] Zero time, [3B] 30 minutes, [3C] 1 hour, [3D] 2 hours, [3E] 4 hours, and [3F] 6 hours.](https://ash.silverchair-cdn.com/ash/content_public/journal/blood/99/6/10.1182_blood.v99.6.2221/6/m_h80622273006.jpeg?Expires=1766325043&Signature=1tw1pDDZ413UTOQXjMVQzTgNUCu0Qgl36dszh2z4gTEWzjGOp7~OXPVGPlNqp3muB4RvZ8WzU~mT-85g8BmXtMYbVLtvwt305fc2~G63z0ROkNMBFu~m7iN24y7sxvpMkAzN3GHsUIoKYSsRuJxpRGhUfnejMhM35W8YtkrZtjm7jlFKQ4YhxfAFUa25LbG1gRYdu6V07Wvny6PA8av4slUrAs5W5jZ0TbBHSRPM8xpNVNg-uEIWQ7StXg56iWWmOoEuwm6jfCBRkHPIEBveXnu8psQNLLdDNmA8ew6CdIGOYemuY3nUznLn9ilkWzYgtDK2pn-WE3b30zsf0KC8iw__&Key-Pair-Id=APKAIE5G5CRDK6RD3PGA)