Abstract
Successful stem cell transplantation (SCT) across HLA barriers can be performed with cord blood, megadoses of stem cells, or with nonmyeloablative conditioning strategies. Because the HLA-mismatched transplants are often T-cell depleted, leukemia relapse rates are high. Treatment of relapsed leukemia after HLA-mismatched SCT is difficult. A novel potential strategy to treat relapsed leukemia after HLA-mismatched SCT is the use of patients' mismatched HLA molecules as antigen-presenting molecules to generate hematopoietic system–specific cytotoxic T cells (CTLs) from the stem cell donor. Adoptive transfer of these hematopoietic system–specific CTLs that are restricted by nonself HLA molecules may eliminate leukemia without affecting the patient's nonhematopoietic cells or donor hematopoietic cells. We investigated the feasibility of this strategy using the hematopoietic system–specific minor histocompatibility antigen HA-1, which is known to induce HLA-A2–restricted CTLs. HLA-A2−peripheral blood mononuclear cells were stimulated with HLA-A2+ T2 cells pulsed with synthetic HA-1 peptide or with dendritic cells transduced with the HA-1 cDNA. Tetrameric HLA-A2/HA-1 peptide complexes were used to monitor and enrich HA-1–specific CTLs. In the alloreactive cultures, HA-1–specific CTLs were enriched up to 7% by 3 rounds of antigen-specific stimulations and up to 87% by fluorescence-activated cell sorting of tetramer-positive T cells. The HA-1–specific CTLs showed specific lysis of the relevant target cells, including leukemic cells. Because the polyclonal CTL cultures also contained natural killer cells and allo–HLA-A2–specific CTLs, CTL clones were generated that showed the expected HA-1 specificity only. Thus, HA-1–specific CTLs restricted by nonself HLA-A2 molecules can be generated in an HLA-A2–mismatched setting.
Introduction
Allogeneic stem cell transplantation (SCT) is the treatment of choice for various hematologic malignancies.1 The curative graft-versus-leukemia (GvL) effect of SCT is mainly mediated by donor-derived alloreactive T cells. The potent immunotherapeutic effect of donor-derived alloreactive T cells is also illustrated by the successful application of donor lymphocyte infusions to relapsed chronic myelogenous leukemia.2 However, if the donor T cells are not selected for preferential reactivity against leukemic cells, the GvL is often associated with graft-versus-host disease (GvHD). Hence, the ideal strategy for immunotherapy without GvHD is to target donor-derived T cells to antigens specifically expressed by the patient's hematopoietic system, including the leukemic cells. In HLA-matched, minor histocompatibility antigen (mHag)–mismatched SCT settings, this strategy is feasible by targeting the donor-derived cytotoxic T cells (CTLs) to the polymorphic hematopoietic system–specific mHags HA-1 and HA-2.3 Because of hematopoietic system–restricted and patient-specific target-cell damage, the ex vivo–generated HA-1/HA-2–specific CTLs can be used as immunotherapeutic agents to eliminate relapsed leukemia with a low risk of GvHD.
Because not every patient has an HLA-identical family member, a substantial proportion of leukemia patients currently undergo transplantation with stem cells of unrelated, often partially HLA-matched donors.4 Successful marrow engraftment across an HLA mismatch is possible by the use of cord blood,5 megadoses of CD34+ stem cells,6 and by nonmyeloablative conditioning7,8 combined with intensive T-cell depletion.8 Because T-cell–depleted grafts lack the GvL effect,1,9 leukemia relapse rates in HLA-mismatched SCT are high. As yet, there is no adequate therapy for leukemia relapses after HLA-mismatched SCT. However, a novel approach for the treatment of relapsed leukemia after HLA-mismatched SCT is to take advantage of the HLA mismatch of the recipient for the generation of immunotherapeutic T cells. Here, the recipients' mismatched HLA molecules are applied as antigen-presenting molecules for hematopoietic system–specific antigens to generate CTLs from the stem cell donor. These CTLs have 2 characteristics: they are hematopoietic system specific and they are “nonself” HLA restricted. Earlier studies showed the existence of T cells restricted by nonself HLA molecules. Sadovnikova et al10,11 have generated mdm-2– and cyclin-D1–specific nonself major histocompatibility complex (MHC)–restricted T cells using peptide-loaded transporter associated with antigen presentation (TAP)–deficient cells as stimulator cells for MHC-incompatible T cells. Similarly, Munz et al12 showed the generation of nonself HLA-restricted, peptide-specific T-cell responses by stimulating HLA-A2−and HLA-A3− peripheral blood mononuclear cells (PBMCs) with HLA-A2+ or HLA-A3+ TAP-deficient cells pulsed with synthetic peptide libraries fitting the HLA-A2 or HLA-A3 motifs. Previously, we generated an HLA-DRw26–restricted hematopoietic system–specific CD4+ T-cell clone by stimulating HLA-DRw26− PBMCs with HLA-DRw26+ acute myeloid leukemia (AML) cells. This T-cell clone recognizes a developmentally regulated antigen expressed exclusively by AML cells and CD34+ progenitor cells.13 Concordantly, Gao et al14 showed the in vitro generation of Wilms' tumor antigen (WT-1) peptide-specific CTLs that are restricted by nonself HLA-A2 molecules and show restricted leukemic cell lysis. Thus, the use of HLA molecules present on patients' cells but absent on donor cells as antigen-presenting molecules for hematopoietic system–specific antigens can result in the generation of hematopoietic system–specific CTLs restricted by nonself HLA molecules.
In this study, we have used the mHag HA-1 as a model antigen to verify the feasibility of generation of hematopoietic system–specific CTLs restricted by nonself HLA molecules. The mHag HA-1 is an ideal antigen to test the feasibility of this strategy because its several relevant characteristics are known. HA-1 is an immunogenic T-cell epitope that induces HLA-A2–restricted CTLs in vivo in recipients of HLA-matched, HA-1–mismatched stem cell donors. Immunogenetic analyses demonstrated mendelian segregation; the HA-1 phenotype frequency in the HLA-A2+ population is 69%. The tissue distribution of HA-1 is restricted to the hematopoietic system; HA-1–specific CTLs lyse leukemic cells and their progenitors but not nonhematopoietic cells.15-18 The HA-1 T-cell epitope is a nonameric peptide (ie, HA-1H) encoded by a diallelic locus that differs by a single amino acid (ie, HA-1R) from its allelic counterpart.19 The HLA-A2/HA-1R ligand is not immunogenic (for a review, see Goulmy20).
The mHag HA-1 is recognized in association with the HLA-A2 molecule. Therefore, throughout this study, PBMCs from HLA-A2−individuals were used as responder cells. The responder cells were stimulated with either HLA-A2+ T2 cells pulsed with HA-1 peptide or with HLA-A2+ dendritic cells (DCs) transduced with the HA-1 cDNA. In this way, HA-1–specific T cells restricted by “nonself HLA-A2” molecules were generated, which were monitored and enriched by tetrameric HLA-A2/ HA-1 peptide complexes (HA-1A2 tetramers).
Materials and methods
HA-1 peptide
HA-1 peptide was synthesized using a semiautomatic multiple peptide synthesizer according to the reported sequence.19The purity of the peptide was greater than 90% as analyzed by reversed-phase high-pressure liquid chromatography.
Tetrameric HLA-A2/HA-1 peptide complexes
Tetrameric HLA-A2/HA-1 peptide complexes (HA-1A2tetramers) were synthesized as described previously.21 For the phenotypic analysis and flow cytometric sorting, cells were surface labeled with the appropriate dilution of phycoerythrin (PE)–conjugated tetramers for 30 minutes at 37°C in phosphate-buffered saline with 1% fetal calf serum. The cells were then analyzed on a Becton Dickinson FACS-Calibur flow cytometer. Tetramer-positive cells were sorted using a FACS-Vantage flow cytometer (Becton Dickinson, San Jose, CA). Data were analyzed using Cell Quest (Becton Dickinson) and WinMDI (version 2.8, J. Trotter; Scripps Research Institute, La Jolla, CA) software.
Induction of HA-1–specific CTLs restricted by nonself HLA-A2 molecules
Responder cells.
The mHag HA-1 is recognized in the context of HLA-A2. Therefore, HA-1–specific CTLs restricted by nonself HLA molecules were generated using PBMCs from 2 HLA-A2− healthy individuals as responder cells (HLA donor no. 1: HLA-A29, -A30, -B12, -B44, -Cw6, -DR7, -DR53, -DQ2; HLA donor no. 2: HLA-A1, -A24, -B7, -B8, -Cw7, -DR15, -DR17, -DR51, -DR52, -DQ2, -DQ6). Genomic mHag typing revealed that both donors were HA-1H positive. Peripheral blood of donors 1 and 2 was collected after obtaining informed consent. PBMCs were isolated by Ficoll Hypaque density centrifugation. Responder cells were cryopreserved in liquid nitrogen until use.
Stimulator cells. T2 cells.
TAP-defective T2 cells were cultured in RPMI 1640 medium (Life Sciences, Breda, The Netherlands) with 15% human serum. T2 cells synthesize HLA-A2 and -B5 but do not express them because of the TAP defect. T2 cells were pulsed with HA-1 peptide (10 μg/mL) for 16 hours at 37°C in the presence of 1 μg/mL β2-microglobulin and irradiated (30 Gy) before coculture with responder cells at a stimulator cell–to–responder-cell ratio of 1:10.
C1R-A2 cells.
The HLA-A2 transfectant of C1R Epstein-Barr virus (EBV)–transformed B-cell line (EBV-LCL) was described elsewhere.11 Untransfected C1R cells do not express HLA-A or HLA-B, but show a low expression of Cw4. C1R-A2 cells were cultured in RPMI medium with 15% human serum. C1R2-A2 cells were pulsed with HA-1 peptide (10 μg/mL) for 16 hours at 37°C and irradiated (30 Gy) before coculture with responder cells at a stimulator cell–to–responder-cell ratio of 1:10.
DCs transduced with HA-1 cDNA.
The transduction of CD34+ progenitor cell–derived DCs with the HA-1–coding cDNA using a retroviral gene-delivery system is described elsewhere.25 The HLA typing of the HA-1–transduced DCs was as follows: HLA-A2, -A24, -B7, -B13, -Cw6, -Cw7, -DRB1*0701, -DRB1*11, -DQB1*0202, -DQB1*0301, -DPB1*0301, -DPB1*02012. The transduction efficiency of the DCs was 20%. HA-1 gene–transduced DCs were irradiated (30 Gy) before coculture with responder cells at a stimulator cell–to–responder cell ratio of 1:5.
Generation of HA-1–specific CTLs restricted by nonself HLA-A2 molecules using T2 cells as stimulator cells
The protocol described by Sadovnikova et al11 was used with slight modifications. Briefly, 20 × 106responder cells from donor no. 1 were cocultured with T2 cells as stimulator cells in the presence of RPMI 1640 with 15% human serum (culture medium). At day 7, the CD8+ cells were sorted using immunomagnetic beads (MACS; Miltenyi Biotech, Bergisch Gladbach, Germany) and restimulated in culture medium by the addition of peptide-pulsed C1R-A2 cells (2 × 105 cells/mL), 30 Gy irradiated autologous PBMCs (2 × 106 cells/mL), and HA-1 peptide (0.5 μg/mL). The T-cell line was restimulated with peptide-pulsed T2 cells at day 14 and with peptide-pulsed C1R-A2 cells at day 21. The T-cell line was subcloned at day 28 by limiting dilution at 1000, 750, 500, 250, and 100 cells per well in 96-well, round-bottom tissue-culture plates in 50 μL/well culture medium supplemented with peptide-pulsed T2 cells (1 × 105 cells/mL), 30 Gy irradiated autologous PBMCs (1 × 106 cells/mL), and interleukin-2 (IL-2; 12 IU/mL). The subclones that showed more than 30% HA-1 peptide–specific lysis were pooled and restimulated in 24-well plates in the presence of peptide-pulsed C1R-A2 cells (2 × 105 cells/mL), autologous PBMCs (2 × 106 cells/mL), and IL-2 (60 IU/mL). The pooled subclones were stained with HA-1A2 tetramers and sorted by flow cytometry. The sorted cells were either restimulated as bulk or cloned by limiting dilution at 0.3 cell per well in 50 μL/well culture medium supplemented with a feeder cell/cytokine mix containing 60 IU/mL IL-2, 1% Leuco-agglutinin (Sigma, St Louis, MO), 30 Gy irradiated PBMCs from 6 random donors (1 × 106cells/mL), and 50 Gy irradiated HA-1+ EBV-LCLs (1 × 105 cells/mL). The clones were expanded with IL-2–containing (60 IU/mL) culture medium. The HA-1–specific CTL clones restricted to nonself HLA-A2 molecules could be cultured for 4 to 6 weeks in vitro by weekly stimulations with the feeder cell/cytokine mix.
Generation of HA-1–specific CTLs restricted by nonself HLA-A2 molecules using DCs transduced with HA-1 cDNA as stimulator cells
HLA-A2− PBMCs (15 × 106) from donor no. 2 were stimulated with HLA-A2+, HA-1–transduced DCs in Iscoves modified Dulbecco medium (IMDM; Life Sciences) supplemented with 10% heat-inactivated human plasma, 6 IU/mL IL-2, and 1 U/mL IL-12. At day 7, the CD8+ cells were positively selected by immunomagnetic beads (MACS; Miltenyi Biotech). The CD8+ T cells were restimulated with the original HA-1–transduced DCs at days 7, 14, and 21. IL-2–containing (120 IU/mL) IMDM plus 10% pooled human plasma was added 24 hours after each restimulation and every other 3 days. At day 28, the CD8+ T cells that showed bright staining with HA-1A2 tetramers were sorted by flow cytometry and cloned as described above.
Cell-mediated lympholysis assays
Standard 4-hour chromium (51Cr)–release assays were performed as previously described.351Cr-labeled target cells were pulsed with 1 μg/mL peptide for 60 minutes before the addition of effector cells. For cold target inhibition assays, unlabeled target cells were added in the wells at various cold target cell–to–hot target cell ratios. The percentage specific lysis was calculated using the following formula: 100 × (cpm experimental release − cpm spontaneous release)/(cpm maximal release − cpm spontaneous release).
Results
Generation of HA-1–specific CTLs restricted by nonself HLA-A2 molecules using T2 cells pulsed with HA-1 peptide
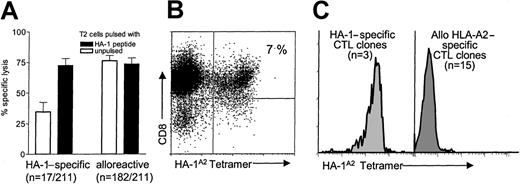
The alloreactive T-cell line induced with HA-1 peptide–pulsed T2 cells was subcloned by limiting dilution, and the proliferating subclones were analyzed for cytotoxic activity against unpulsed and HA-1 peptide–pulsed T2 cells. Whereas many (182 of 211) subclones lysed both peptide-pulsed and unpulsed T2 cells, 17 of 211 subclones showed preferential lysis against HA-1 peptide– pulsed T2 cells. The mean cytotoxic activities of these latter subclones against HA-1 peptide–pulsed and unpulsed T2 cells were 68% and 35%, respectively (Figure 1A). These “HA-1–specific” subclones were pooled and stained with HA-1A2 tetramers. A total of 7% lymphocytes showed bright staining with HA-1A2 tetramers (Figure 1B). To verify the specificity of the HA-1A2 tetramer staining, we analyzed 15 allo–HLA-A2–specific CTL clones. HA-1A2 tetramers stained solely HA-1–specific CTL clones. None of the 15 allo–HLA-A2–specific CTLs showed staining with HA-1A2 tetramers (Figure1C).
Generation of HA-1–specific CTLs restricted by nonself HLA-A2 molecules using T2 cells pulsed with HA-1 peptide.
(A) Subclones that showed more than 30% specific reactivity against HA-1 peptide–pulsed T2 cells as compared with unpulsed T2 cells are designated as “HA-1–specific” (n = 17 of 211). Subclones that did not discriminate between peptide-pulsed and unpulsed T2 cells are designated as “alloreactive” (n = 182 of 211). The results are presented as the mean cytotoxic activity. The error bars represent the SEM. (B) HA-1A2 tetramer staining of the “HA-1–specific” T-cell cultures, showing PE-conjugated HA-1A2 tetramers (x axis) and PE-Cy-5–conjugated anti-CD8 antibody (y axis). Appropriate gates were set on vital lymphocytes according to their typical forward- and side-scattering characteristics. (C) The specificity of HA-1A2 tetramer staining. Three CD8+ HA-1–specific CTL clones and 15 CD8+ allo–HLA-A2–specific CTL clones were stained with HA-1A2 tetramers. Appropriate gates were set on vital lymphocytes according to their typical forward- and side-scattering characteristics. The histograms represent the tetramer staining of CD8+ T cells. Representative examples are shown for each group of CTL clones.
Generation of HA-1–specific CTLs restricted by nonself HLA-A2 molecules using T2 cells pulsed with HA-1 peptide.
(A) Subclones that showed more than 30% specific reactivity against HA-1 peptide–pulsed T2 cells as compared with unpulsed T2 cells are designated as “HA-1–specific” (n = 17 of 211). Subclones that did not discriminate between peptide-pulsed and unpulsed T2 cells are designated as “alloreactive” (n = 182 of 211). The results are presented as the mean cytotoxic activity. The error bars represent the SEM. (B) HA-1A2 tetramer staining of the “HA-1–specific” T-cell cultures, showing PE-conjugated HA-1A2 tetramers (x axis) and PE-Cy-5–conjugated anti-CD8 antibody (y axis). Appropriate gates were set on vital lymphocytes according to their typical forward- and side-scattering characteristics. (C) The specificity of HA-1A2 tetramer staining. Three CD8+ HA-1–specific CTL clones and 15 CD8+ allo–HLA-A2–specific CTL clones were stained with HA-1A2 tetramers. Appropriate gates were set on vital lymphocytes according to their typical forward- and side-scattering characteristics. The histograms represent the tetramer staining of CD8+ T cells. Representative examples are shown for each group of CTL clones.
Generation of HA-1–specific CTLs restricted by nonself HLA-A2 molecules using DCs transduced with HA-1 cDNA
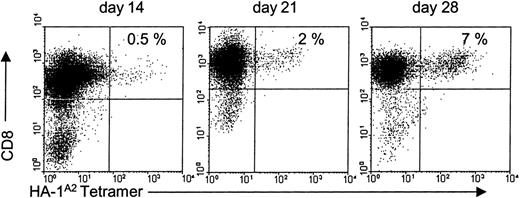
The PBMCs of another HLA-A2− individual were stimulated with HLA-A2+ DCs that were transduced with HA-1. After selection of CD8+ T cells at day 7, the cells were restimulated weekly. The development of HA-1–specific CTLs was monitored with HA-1A2 tetramers. As illustrated in Figure2, tetramer-positive T cells totaled only 0.5% at day 14. The frequency of HA-1A2 tetramer-positive cells increased significantly upon antigen-specific restimulations and totaled 2% and 7% at days 21 and 28, respectively (Figure2).
Generation of HA-1–specific CTLs restricted by nonself HLA-A2 molecules using DCs transduced with HA-1 cDNA.
The cells were stained with PE-conjugated HA-1A2 tetramers and with PE-Cy-5–conjugated anti-CD8 antibody at the indicated days. Appropriate gates were set on vital lymphocytes according to their typical forward- and side-scattering characteristics.
Generation of HA-1–specific CTLs restricted by nonself HLA-A2 molecules using DCs transduced with HA-1 cDNA.
The cells were stained with PE-conjugated HA-1A2 tetramers and with PE-Cy-5–conjugated anti-CD8 antibody at the indicated days. Appropriate gates were set on vital lymphocytes according to their typical forward- and side-scattering characteristics.
Selection of HA-1–specific CTLs restricted by nonself HLA molecules using tetrameric HLA-A2/HA-1 peptide complexes
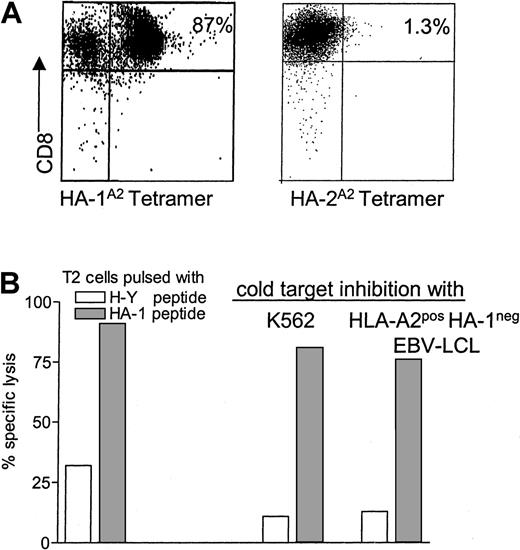
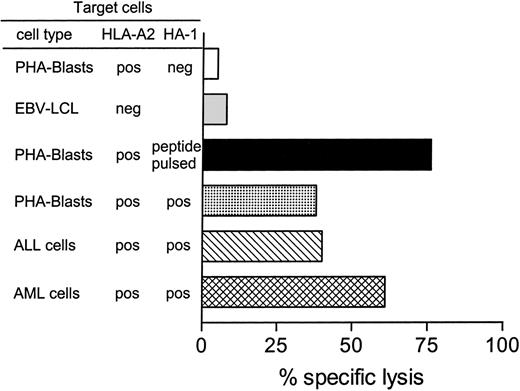
The HA-1A2 tetramer-positive CD8+ cells in the polyclonal cultures were sorted by flow cytometry. In the CTL line induced by T2 cells, the HA-1A2 tetramer-positive T cells were enriched from 7% to 87% after a single round of sorting (Figure3A). The sorted T cells did not cross-react with the control HA-2A2 tetramer (Figure 3A) and showed strong lysis of HA-1 peptide–pulsed T2 cells (Figure 3B). The H-Y peptide-pulsed T2 cells were lysed by 30%. The latter lysis on the control H-Y peptide-pulsed T2 cells could be due to allo–HLA-A2–specific T cells or natural killer (NK) cells contaminating the culture. Therefore, cold target inhibition studies were performed by the addition of cold (unlabeled) K562 cells and HLA-A2+ HA-1− EBV-LCLs during the cell-mediated lympholysis assays. The lysis of HA-1 peptide–pulsed T2 cells was not significantly affected by the addition of cold K562 cells or HLA-A2+ HA-1− EBV-LCLs. In contrast, the lysis of H-Y peptide-pulsed T2 cells was abrogated by the addition of both cold K562 cells and HLA-A2+ HA-1−EBV-LCLs. Thus, the T-cell line contained not only HA-1–specific CTLs, but also allo–HLA-A2–specific T cells and NK cells (Figure 3B). Addition of the HA-1 peptide–pulsed HLA-A2+ EBV-LCLs as cold target cells abrogated the lysis of HA-1 peptide–pulsed targets, indicating the specificity of the assay (data not shown). The CTL line was subsequently tested against target cells that express the natural HLA-A2/HA-1 ligand. Unlabeled K562 cells and HLA-A2+ HA-1− EBV-LCLs were used as cold targets to inhibit the cytotoxic activity mediated by contaminating NK cells and allo HLA-A2–specific CTLs. Effective lysis was demonstrated against HA-1 peptide–pulsed target cells, HA-1+phytohemagglutinin blasts, EBV-LCLs, and leukemic cells of AML and acute lymphocytic leukemia (ALL) origin. HA-1− or HLA-A2− target cells were not lysed (Figure4). The HA-1–specific CTLs induced by transduced DCs could be enriched to 20% purity by FACS sorting (data not shown). This CTL line was therefore directly cloned by limiting dilution.
Selection of HA-1–specific CTLs restricted by nonself HLA molecules using HA-1A2 tetramers.
(A) The percentage of HA-1A2 tetramer–positive CD8+ T cells after sorting. HA-2A2 tetramers were used as specificity control. (B) The cytotoxic activity of sorted T cells against T2 cells pulsed with HA-1 peptide and control H-Y peptide (both 1 μg/mL) without or with the addition of cold K562 or HLA-A2+/HA-1− EBV-LCLs (cold target cell–to–hot target cell ratio = 20). The results are expressed as the mean of the duplicate cultures at an effector-to–hot target cell ratio of 1:1.
Selection of HA-1–specific CTLs restricted by nonself HLA molecules using HA-1A2 tetramers.
(A) The percentage of HA-1A2 tetramer–positive CD8+ T cells after sorting. HA-2A2 tetramers were used as specificity control. (B) The cytotoxic activity of sorted T cells against T2 cells pulsed with HA-1 peptide and control H-Y peptide (both 1 μg/mL) without or with the addition of cold K562 or HLA-A2+/HA-1− EBV-LCLs (cold target cell–to–hot target cell ratio = 20). The results are expressed as the mean of the duplicate cultures at an effector-to–hot target cell ratio of 1:1.
The cytotoxic activity of HA-1–specific CTLs restricted by nonself HLA-A2 molecules against HLA-A2+ and HLA-A2− target cells that naturally express the HLA-A2/HA-1 ligand.
The indicated target cells were used as hot targets for the allo–HLA-A2–restricted HA-1–specific CTLs in the presence of cold K562 cells or HLA-A2+, HA-1− EBV-LCLs (cold target cell–to–hot target cell ratio = 20). The results are expressed as the mean value of the duplicate cultures at an effector-to–hot target cell ratio of 1:1.
The cytotoxic activity of HA-1–specific CTLs restricted by nonself HLA-A2 molecules against HLA-A2+ and HLA-A2− target cells that naturally express the HLA-A2/HA-1 ligand.
The indicated target cells were used as hot targets for the allo–HLA-A2–restricted HA-1–specific CTLs in the presence of cold K562 cells or HLA-A2+, HA-1− EBV-LCLs (cold target cell–to–hot target cell ratio = 20). The results are expressed as the mean value of the duplicate cultures at an effector-to–hot target cell ratio of 1:1.
Generation of HA-1–specific CTL clones restricted by nonself HLA-A2 molecules
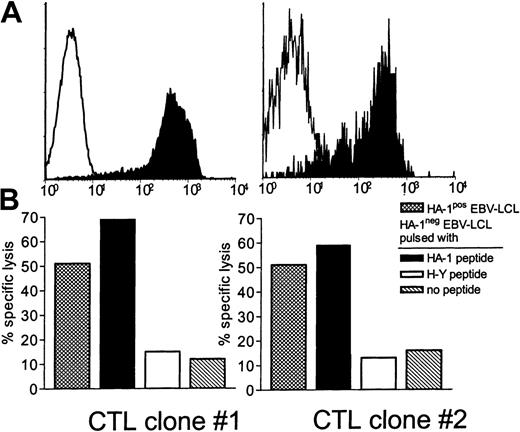
Because the HA-1–specific CTLs induced by T2 cells and HA-1–transduced DCs contained undesired allo–HLA-A2–specific cells and NK cells, CTL clones were obtained by limiting dilution at 0.3 cell per well. Two CTL clones showed bright staining with HA-1A2tetramer (Figure 5A), but no staining with the control HA-2A2 tetramer. As expected, both CTL clones showed strong and specific lysis of both HA-1 peptide–pulsed EBV-LCLs and EBV-LCLs that naturally express the HLA-A2/HA-1 ligand (Figure 5B).
Tetramer staining and HA-1–specific cytotoxic activity of HA-1–specific CTL clones restricted by nonself HLA-A2 molecules.
(A) Staining of CTL clones with HA-1A2 tetramers. Filled histograms represent the staining with HA-1A2 tetramer. Open histograms represent the staining with the control HA-2A2 tetramer. (B) Cytotoxic activity of CTL clones against HA-1 peptide–pulsed (1 μg/mL) cells and HA-1+EBV-LCLs in a 51Cr-release assay. The results are expressed as the mean value of the duplicate cultures at an effector-to–hot target cell ratio of 10:1.
Tetramer staining and HA-1–specific cytotoxic activity of HA-1–specific CTL clones restricted by nonself HLA-A2 molecules.
(A) Staining of CTL clones with HA-1A2 tetramers. Filled histograms represent the staining with HA-1A2 tetramer. Open histograms represent the staining with the control HA-2A2 tetramer. (B) Cytotoxic activity of CTL clones against HA-1 peptide–pulsed (1 μg/mL) cells and HA-1+EBV-LCLs in a 51Cr-release assay. The results are expressed as the mean value of the duplicate cultures at an effector-to–hot target cell ratio of 10:1.
Discussion
In this study, we show that the T-cell repertoire of HLA-A2− individuals contains CTLs specific for the mHag HA-1 presented by nonself HLA-A2 molecules. These HA-1–specific CTLs restricted by nonself HLA molecules can be propagated in vitro by specific stimulation with HLA-A2+ stimulator cells pulsed with synthetic HA-1 peptide or transduced with HA-1 cDNA. The HA-1–specific CTLs restricted by nonself HLA-A2 molecules show effective lysis of HA-1 peptide–pulsed and of target cells that naturally express the HLA-A2/HA-1 ligand. Importantly in view of the final goal of this study, HA-1+ AML and ALL cells also were lysed by HA-1–specific CTLs restricted by nonself HLA-A2 molecules. The apparent drawback of the methodology described herein is the generation of allo–HLA-A2–specific reactivities besides the HA-1–specific CTLs. To eliminate this undesired alloreactivity, effective depletion or selection strategies must be executed.
To generate HA-1–specific CTLs restricted by nonself HLA-A2 molecules, we used 2 approaches. In the first approach, similar to that of Sadovnikova et al,11 we used T2 cells pulsed with HA-1 peptide as stimulator cells. Because the empty HLA-A2 molecules on the surface of T2 cells can be uniformly loaded with exogenous peptides, this approach could minimize the induction of undesired allo–HLA-A2 reactivities. Moreover, similar to Sadovnikova et al,11 we restimulated the responder cells with the alternative usage of C1R-A2 cells and T2 cells. Because C1R-A2 cells and T2 cells are genetically distinct, it was expected that different sets of “irrelevant” endogenous peptides would be presented by T2 cells and C1R-A2 cells. Thus, alternative restimulation of alloreactive T-cell lines with T2 and C1R-A2 cells could prevent the restimulation of undesired allo–HLA-A2 CTLs directed to “undesired” endogenous peptides. Our second approach involved the use of DCs transduced with the HA-1 cDNA as stimulator cells, which also could present the “irrelevant” endogenous peptides. Both approaches induced HA-1–specific CTLs restricted by nonself HLA-A2 molecules, but also induced similar levels of undesired allo–HLA-A2 reactivities.
It is noteworthy that in both approaches, the responder cells were mHag HA-1H positive. Thus, endogenous expression of HA-1 by the responder does not affect the generation of HA-1–specific CTLs restricted by nonself HLA-A2 molecules. In both approaches, the responder and the stimulator cells were mismatched not only for HLA-A2, but also for other HLA class I molecules that could induce additional undesired alloresponses. The presence of these additional mismatches apparently did not hamper the generation of HA-1–specific CTLs in the responder/stimulator combinations we used. Nonetheless, because the HLA system is highly polymorphic, our data cannot rule out the possibility that mismatches for highly immunogenic HLA class I alleles could negatively influence the generation of nonself-restricted HA-1–specific CTLs. The negative effect of additional mismatches may be less relevant for the “T2” approach because T2 cells and C1R-A2 cells do not express HLA class I molecules on the cell surface. However, it may be preferable to select closely HLA-matched responder and stimulator cells for the generation of nonself-restricted CTLs, as is the case in the HLA-mismatched SCT setting.
It was reported that undesired alloreactive T cells from donor PBMCs can be efficiently removed by depletion of CD69/CD25+ T cells triggered by short-term stimulation of HLA-mismatched patient cells.22 We indeed observed that CD69/CD25-depleted T cells showed no anti–HLA-A2 reactivity in the initial weeks of the cultures. However, strong anti–HLA-A2 alloreactivity developed upon restimulation with allo–HLA-A2 target cells in the long-term cultures of more than 40 days, indicating ineffective elimination of allo–HLA-A2–specific responses using these depletion strategies (data not shown).
Earlier we reported that mHag-specific CTLs show specific staining with HLA class I/mHag peptide tetramers.21 The intensity of the tetramer staining correlates with the avidity of the mHag-specific CTLs to the natural mHag ligand.23 On the basis of these results, we used tetrameric HLA/mHag peptide complexes for the selection and enrichment of HA-1–specific CTLs restricted by nonself HLA-A2 molecules. A recent report showed that certain alloreactive T cells can stain with tetrameric HLA/peptide complexes independent of the peptide complexed with the HLA molecule.24 Thus, tetramer staining in alloreactive T-cell cultures may not always reflect the peptide specificity. In our study, we did not observe nonspecific staining of alloreactive T cells with HA-1A2tetramers. Thus, in our protocols, tetrameric HLA class I/peptide complexes served as satisfactory tools for the monitoring and enrichment of HA-1–specific CTLs restricted by nonself HLA molecules. However, depletion of all undesired alloreactivity by the sole use of HA-1A2 tetramers was not possible, and limiting dilution of the sorted T cells was necessary for the effective selection of HA-1–specific CTLs.
In conclusion, our results provide proof of the principle that specific CTLs can be generated against a nonself HLA-A2/HA-1 peptide ligand. Naturally, further optimization of the in vitro protocols will be indispensable for effective elimination of the undesired alloreactivity.
The successful induction of both WT-1– and HA-1–specific CTLs restricted by nonself HLA molecules clearly underlines the feasibility of adoptive immunotherapy of hematologic malignancies with hematopoietic system–specific CTLs restricted by nonself HLA molecules after HLA-mismatched SCT. This novel strategy also introduces the possibility of a variety of other hematopoietic system–specific antigens to be used as target antigens for the generation of CTLs restricted by nonself HLA molecules. The candidate antigens include leukemia-associated antigens with known immunogenicity, hematopoietic system–specific transcription factors with high expression on leukemic cells (GATA-1, PU-1, IKAROS), and hematopoietic system–specific differentiation antigens (CD45, CD19, and CD20). Naturally, future studies are necessary to test the immunogenicity of peptides of these candidate proteins in the context of various HLA alleles. These studies will expand the arsenal of target antigens for the generation of hematopoietic system–specific CTLs restricted by nonself HLA molecules and provide a basis for broader application of this strategy for the treatment of relapsed leukemia after HLA-mismatched SCT.
We thank Prof Dr A. Brand and Dr M. Oudshoorn for reading the manuscript.
Prepublished online as Blood First Edition Paper, April 17, 2002; DOI 10.1182/blood-2002-01-0024.
Supported in part by grants from the Leiden University Medical Center, the J.A. Cohen Institute for Radiopathology and Radiation Protection, the Dutch Cancer Society, and the Leukemia & Lymphoma Society. T.M. is a Leukemia & Lymphoma Society Translational Research Fellow.
The publication costs of this article were defrayed in part by page charge payment. Therefore, and solely to indicate this fact, this article is hereby marked “advertisement” in accordance with 18 U.S.C. section 1734.
References
Author notes
Tuna Mutis, Department of Immunohematology and Blood Transfusion, Bldg 1 E3-Q, Leiden University Medical Center, Albinusdreef 2, 2333 ZA Leiden, The Netherlands; e-mail:t.mutis@lumc.nl.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal