The POEMS syndrome (coined to refer to polyneuropathy, organomegaly, endocrinopathy, M protein, and skin changes) remains poorly understood. Ambiguity exists over the features necessary to establish the diagnosis, treatment efficacy, and prognosis. We identified 99 patients with POEMS syndrome. Minimal criteria were a sensorimotor peripheral neuropathy and evidence of a monoclonal plasmaproliferative disorder. To distinguish POEMS from neuropathy associated with monoclonal gammopathy of undetermined significance, additional criteria were included: a bone lesion, Castleman disease, organomegaly (or lymphadenopathy), endocrinopathy, edema (peripheral edema, ascites, or effusions), and skin changes. The median age at presentation was 51 years; 63% were men. Median survival was 165 months. With the exception of fingernail clubbing (P = .03) and extravascular volume overload (P = .04), no presenting feature, including the number of presenting features, was predictive of survival. Response to therapy (P < .001) was predictive of survival. Pulmonary hypertension, renal failure, thrombotic events, and congestive heart failure were observed and appear to be part of the syndrome. In 18 patients (18%), new disease manifestations developed over time. More than 50% of patients had a response to radiation, and 22% to 50% had responses to prednisone and a combination of melphalan and prednisone, respectively. We conclude that the median survival of patients with POEMS syndrome is 165 months, independent of the number of syndrome features, bone lesions, or plasma cells at diagnosis. Additional features of the syndrome often develop, but the complications of classic multiple myeloma rarely develop.
Introduction
Associations between plasma cell dyscrasia and peripheral neuropathy are well recognized.1 One third to one half of patients with osteosclerotic myeloma have neuropathy,2-4 and one half of patients with myeloma and peripheral neuropathy have osteosclerotic lesions.5 These figures contrast distinctly with the 1% to 8% incidence of neuropathy in patients with classic multiple myeloma.6 7
In 1956, the interaction of plasma cell dyscrasia and peripheral neuropathy was shown to be more complex with Crow's1description of 2 patients with osteosclerotic plasmacytomas with neuritis and other “striking features,” which included clubbing, skin pigmentation, dusky discoloration of the skin, white fingernails, mild lymphadenopathy, and ankle edema. Scheinker's autopsy case in 1938 was the first report of what we now call POEMS syndrome, Crow-Fukase syndrome, PEP syndrome (plasma cell dyscrasia, endocrinopathy, and polyneuropathy), or Takatsuki syndrome.8,9 The patient was a 39-year-old man with a solitary plasmacytoma, sensorimotor polyneuropathy, and localized patches of thickened and deeply pigmented skin on the chest.3,10 Subsequently, others reported patients with osteosclerotic myeloma and peripheral neuropathy with organomegaly, skin changes, endocrinopathy, edema, hypertrichosis, gynecomastia, and ascites.2-4,9,11-18 In a 1977 review by Iwashita et al,3 30 patients with osteosclerotic myeloma and peripheral neuropathy, as compared with 29 patients without peripheral neuropathy, had a higher incidence of hyperpigmentation, edema, skin thickening, hepatomegaly, hypertrichosis, and clubbing. In 1980, Bardwick et al19 coined the acronym POEMS to represent a syndrome characterized by polyneuropathy, organomegaly, endocrinopathy, M protein, and skin changes. Not represented in the acronym are several important features, including sclerotic bone lesions, Castleman disease, papilledema, pleural effusion, edema, ascites, and thrombocytosis.8 20-22
No single test establishes the diagnosis of POEMS syndrome. Seemingly disparate signs and symptoms must be linked to establish the diagnosis. Although several series have been reported,8,19,22ambiguity exists about the number of features necessary for diagnosis, effective therapies, and prognosis. The interconnections between POEMS syndrome, osteosclerotic myeloma, and Castleman disease are still under investigation. Cytokines have been implicated in the pathogenesis of the disease.23-25 POEMS appears to be mediated by an imbalance of proinflammatory cytokines. Interleukin-1β (IL-1β), IL-6, and tumor necrosis factor-α inconsistently have been reported to be increased in association with the syndrome.26-28Preliminary data suggest that vascular endothelial growth factor is an excellent candidate as a pathogenic factor in POEMS29,30; it induces a rapid and reversible increase in vascular permeability, is a growth factor for endothelial cells, and is considered important in angiogenesis.27
In a retrospective review of a single institution's experience, we defined the minimal criteria required for the diagnosis of POEMS syndrome, described the natural history of the disease, and studied whether pulmonary hypertension, restrictive lung disease, thrombosis, cardiomyopathy, and glomerulonephritis are true associations.
Patients and methods
The Mayo Clinic dysproteinemia database was queried for all patients with POEMS syndrome or osteosclerotic myeloma. One reviewer (A.D.) abstracted data. Through December 1998, 99 patients were identified who met the minimal criteria for study inclusion. The diagnosis had been made at our institution in 80 patients and elsewhere in 19 patients. All 99 patients had both major criteria and one minor criterion for the diagnosis of POEMS syndrome (Table1).
Criteria for the diagnosis of POEMS syndrome*
| Major criteria | Polyneuropathy |
| Monoclonal plasmaproliferative disorder | |
| Minor criteria | Sclerotic bone lesions† |
| Castleman disease† | |
| Organomegaly (splenomegaly, hepatomegaly, or lymphadenopathy) | |
| Edema (edema, pleural effusion, or ascites) | |
| Endocrinopathy (adrenal, thyroid,‡ pituitary, gonadal, parathyroid, pancreatic‡) | |
| Skin changes (hyperpigmentation, hypertrichosis, plethora, hemangiomata, white nails) | |
| Papilledema | |
| Known associations | Clubbing |
| Weight loss | |
| Thrombocytosis | |
| Polycythemia | |
| Hyperhidrosis | |
| Possible associations | Pulmonary hypertension |
| Restrictive lung disease | |
| Thrombotic diatheses | |
| Arthralgias | |
| Cardiomyopathy (systolic dysfunction) | |
| Fever | |
| Low vitamin B12values | |
| Diarrhea |
| Major criteria | Polyneuropathy |
| Monoclonal plasmaproliferative disorder | |
| Minor criteria | Sclerotic bone lesions† |
| Castleman disease† | |
| Organomegaly (splenomegaly, hepatomegaly, or lymphadenopathy) | |
| Edema (edema, pleural effusion, or ascites) | |
| Endocrinopathy (adrenal, thyroid,‡ pituitary, gonadal, parathyroid, pancreatic‡) | |
| Skin changes (hyperpigmentation, hypertrichosis, plethora, hemangiomata, white nails) | |
| Papilledema | |
| Known associations | Clubbing |
| Weight loss | |
| Thrombocytosis | |
| Polycythemia | |
| Hyperhidrosis | |
| Possible associations | Pulmonary hypertension |
| Restrictive lung disease | |
| Thrombotic diatheses | |
| Arthralgias | |
| Cardiomyopathy (systolic dysfunction) | |
| Fever | |
| Low vitamin B12values | |
| Diarrhea |
POEMS indicates polyneuropathy, organomegaly, endocrinopathy, M protein, skin changes.
Two major criteria and at least 1 minor criterion are required for diagnosis.
Osteosclerotic lesion or Castleman disease is usually present.
Because of the high prevalence of diabetes mellitus and thyroid abnormalities, this diagnosis alone is not sufficient to meet this minor criterion.
All patients (or their physicians) for whom no follow-up data were available in the preceding year were contacted. Death certificates were sought for deceased patients for whom there was inadequate information. Follow-up data were available for 93 patients (94%). Median follow-up was 70.6 months (range, 0.2 to 304 months). Twenty-four patients (24%) were evaluated from 1960 to 1985, 33 (33%) from 1986 to 1990, and 42 (42%) from 1991 to 1998. The Mayo Foundation Institutional Review Board approved the study in accordance with Minnesota state law.
The definitions of response to treatment were based on both patient and physician reports of improvement rather than on strictly defined objective criteria. Patients who had little or no residual neuropathy and otherwise regained a normal sense of well-being and function were classified as having had a very good response. Those who had improvement in their neuropathy but still perceived themselves to have a significant handicap were classified as having had a good response. Patients whose deterioration stabilized during or after treatment but did not derive any subjective or objective improvement were classified as having stable disease. Patients who continued to deteriorate despite therapy were deemed refractory.
Curves for overall survival and time to the development of new syndrome features were plotted according to the method of Kaplan and Meier31 and were compared by the log-rank test.32 Survival was calculated from the time of diagnosis. Prognostic factors for overall survival and risk of developing additional features were determined by the Cox proportional hazards model in the analysis of covariates.33 Variables analyzed in these models include the following: age, sex, organomegaly, papilledema, skin abnormalities, endocrine abnormalities, edema, weight loss, lymphadenopathy, Castleman disease, number of POEMS features, thrombocytosis, hemoglobin level, type of immunoglobulin heavy chain, bone marrow plasmacytosis, serum M-protein level, urine M-protein level, number of bone lesions, and type of treatment.
Results
Presenting features
Patient characteristics are shown in Tables2 and 3. Thirty-one patients (31%) were 45 years or younger; 62 (63%) were men. Table 3 compares the findings in this study with those of the 2 other largest patient series.8 22 The most notable differences among the studies are the high frequency of accompanying bone lesions in the present study (97% compared with 54% to 68%) and the lower frequency in the present study of edema and effusions (29% compared with 66% to 89%) and organomegaly (50% compared with 68% to 78%). In contrast to the other studies in Table3, the present series cites only the features present at diagnosis rather than features observed during disease evolution and progression.
Presenting clinical characteristics of 99 patients with POEMS syndrome
| Characteristic . | % . |
|---|---|
| Median age, y (range) | 51 (30-83) |
| Race | |
| African American | 8 |
| Asian | 0 |
| Hispanic | 3 |
| Non-Hispanic white | 89 |
| Male sex | 63 |
| Patients with given no. of classic POEMS features* | |
| 2 features | 7 |
| 3 features | 32 |
| 4 features | 31 |
| 5 features | 29 |
| Patients with given no. of revised POEMS features† | |
| 3 features | 6 |
| 4 features | 19 |
| 5 features | 32 |
| 6 features | 17 |
| 7 features | 16 |
| 8 features | 7 |
| 9 features | 2 |
| Laboratory value | |
| Albumin less than 3.0 g/dL (range) | 24 (2.3-4.5) |
| Bone marrow plasma cells more than 10% (range) | 14 (0-40) |
| Calcium more than 10.5 mg/dL (range) | 0 (7.8-10.2) |
| Creatinine more than 1.5 mg/dL (range) | 2 (0.5-1.9) |
| Erythrocyte sedimentation rate more than 29 mm/h (range) | 16 (1-58) |
| Hemoglobin less than 11 g/dL (range) | 4 (10.4-18.4) |
| Hemoglobin more than 16 g/dL (range) | 16 (10.4-18.4) |
| Leukocytes more than 10 500/μL (range) | 21 (3700-17 600) |
| Platelets more than 450 × 103/μL (range) | 54 (111-1163) |
| Serum M-spike more than 2.0 g/dL (range) | 7 (0.00-4.1) |
| Urine M-spike more than 0.5 g/24 h (range) | 0 (0.00-0.45) |
| Urine protein more than 1.0 g/24 h (range) | 5 (0.02-3.2) |
| Characteristic . | % . |
|---|---|
| Median age, y (range) | 51 (30-83) |
| Race | |
| African American | 8 |
| Asian | 0 |
| Hispanic | 3 |
| Non-Hispanic white | 89 |
| Male sex | 63 |
| Patients with given no. of classic POEMS features* | |
| 2 features | 7 |
| 3 features | 32 |
| 4 features | 31 |
| 5 features | 29 |
| Patients with given no. of revised POEMS features† | |
| 3 features | 6 |
| 4 features | 19 |
| 5 features | 32 |
| 6 features | 17 |
| 7 features | 16 |
| 8 features | 7 |
| 9 features | 2 |
| Laboratory value | |
| Albumin less than 3.0 g/dL (range) | 24 (2.3-4.5) |
| Bone marrow plasma cells more than 10% (range) | 14 (0-40) |
| Calcium more than 10.5 mg/dL (range) | 0 (7.8-10.2) |
| Creatinine more than 1.5 mg/dL (range) | 2 (0.5-1.9) |
| Erythrocyte sedimentation rate more than 29 mm/h (range) | 16 (1-58) |
| Hemoglobin less than 11 g/dL (range) | 4 (10.4-18.4) |
| Hemoglobin more than 16 g/dL (range) | 16 (10.4-18.4) |
| Leukocytes more than 10 500/μL (range) | 21 (3700-17 600) |
| Platelets more than 450 × 103/μL (range) | 54 (111-1163) |
| Serum M-spike more than 2.0 g/dL (range) | 7 (0.00-4.1) |
| Urine M-spike more than 0.5 g/24 h (range) | 0 (0.00-0.45) |
| Urine protein more than 1.0 g/24 h (range) | 5 (0.02-3.2) |
Comparison of clinical characteristics of patients in the present series and 2 previous series3-150
| Characteristic . | Present study, % N = 99 . | Soubrier et al,22 % N = 25 . | Nakanishi et al,8% N = 102 . |
|---|---|---|---|
| Polyneuropathy | |||
| Peripheral neuropathy | 100 | 100 | 100 |
| Cerebrospinal fluid protein more than 50 mg/dL | 1003-152 | 1003-152 | 973-152 |
| Organomegaly | 50 | NR | NR |
| Hepatomegaly | 24 | 68 | 78 |
| Splenomegaly | 22 | 52 | 35 |
| Lymphadenopathy | 26 | 52 | 61 |
| Castleman disease | 11 | 24 | 19 |
| Endocrinopathy | 67 | NR | NR |
| Gonadal axis abnormality | 55 | NR | NR |
| Adrenal axis abnormality | 16 | NR | NR |
| Increased prolactin value | 5 | NR | NR |
| Gynecomastia or galactorrhea | 18 | NR | NR |
| Diabetes mellitus | 3 | 36 | 25 |
| Hypothyroidism | 14 | 36 | NR |
| Hyperparathyroidism | 3 | NR | NR |
| Monoclonal plasma cell dyscrasia | 100 | 100 | 75 |
| M component on serum protein electrophoresis | 54 | 100 | 70 |
| Skin changes | 68 | NR | NR |
| Hyperpigmentation | 46 | 48 | 93 |
| Acrocyanosis and plethora | 19 | NR | NR |
| Hemangioma/telangiectasia | 9 | 32 | NR |
| Hypertrichosis | 26 | 24 | 74 |
| Thickening | 5 | 28 | 61 |
| Papilledema | 29 | 40 | 55 |
| Extravascular volume overload | 29 | NR | NR |
| Peripheral edema | 24 | 80 | 89 |
| Ascites | 7 | 32 | 52 |
| Pleural effusion | 3 | 24 | 35 |
| Bone lesions | 97 | 68 | 54 |
| Osteosclerotic only3-151 | 47 | 41 | 56 |
| Mixed sclerotic and lytic3-151 | 51 | 59 | 31 |
| Lytic only3-151 | 2 | 0 | 13 |
| Solitary lesion3-151 | 45 | 41 | 45 |
| 2 or 3 lesions3-151 | 23 | NR | NR |
| More than 1 lesion3-151 | 54 | 59 | 45 |
| More than 3 lesions3-151 | 32 | NR | NR |
| Other features | |||
| Weight loss more than 10 pounds | 37 | NR | NR |
| Fatigue | 31 | NR | NR |
| Thrombocytosis: platelet count more than 450 × 103/μL | 54 | 88 | NR |
| Polycythemia: hemoglobin more than 15 g/dL in women and more than 17 g/dL in men | 18 | 12 | 19 |
| Clubbing | 5 | 32 | 49 |
| Characteristic . | Present study, % N = 99 . | Soubrier et al,22 % N = 25 . | Nakanishi et al,8% N = 102 . |
|---|---|---|---|
| Polyneuropathy | |||
| Peripheral neuropathy | 100 | 100 | 100 |
| Cerebrospinal fluid protein more than 50 mg/dL | 1003-152 | 1003-152 | 973-152 |
| Organomegaly | 50 | NR | NR |
| Hepatomegaly | 24 | 68 | 78 |
| Splenomegaly | 22 | 52 | 35 |
| Lymphadenopathy | 26 | 52 | 61 |
| Castleman disease | 11 | 24 | 19 |
| Endocrinopathy | 67 | NR | NR |
| Gonadal axis abnormality | 55 | NR | NR |
| Adrenal axis abnormality | 16 | NR | NR |
| Increased prolactin value | 5 | NR | NR |
| Gynecomastia or galactorrhea | 18 | NR | NR |
| Diabetes mellitus | 3 | 36 | 25 |
| Hypothyroidism | 14 | 36 | NR |
| Hyperparathyroidism | 3 | NR | NR |
| Monoclonal plasma cell dyscrasia | 100 | 100 | 75 |
| M component on serum protein electrophoresis | 54 | 100 | 70 |
| Skin changes | 68 | NR | NR |
| Hyperpigmentation | 46 | 48 | 93 |
| Acrocyanosis and plethora | 19 | NR | NR |
| Hemangioma/telangiectasia | 9 | 32 | NR |
| Hypertrichosis | 26 | 24 | 74 |
| Thickening | 5 | 28 | 61 |
| Papilledema | 29 | 40 | 55 |
| Extravascular volume overload | 29 | NR | NR |
| Peripheral edema | 24 | 80 | 89 |
| Ascites | 7 | 32 | 52 |
| Pleural effusion | 3 | 24 | 35 |
| Bone lesions | 97 | 68 | 54 |
| Osteosclerotic only3-151 | 47 | 41 | 56 |
| Mixed sclerotic and lytic3-151 | 51 | 59 | 31 |
| Lytic only3-151 | 2 | 0 | 13 |
| Solitary lesion3-151 | 45 | 41 | 45 |
| 2 or 3 lesions3-151 | 23 | NR | NR |
| More than 1 lesion3-151 | 54 | 59 | 45 |
| More than 3 lesions3-151 | 32 | NR | NR |
| Other features | |||
| Weight loss more than 10 pounds | 37 | NR | NR |
| Fatigue | 31 | NR | NR |
| Thrombocytosis: platelet count more than 450 × 103/μL | 54 | 88 | NR |
| Polycythemia: hemoglobin more than 15 g/dL in women and more than 17 g/dL in men | 18 | 12 | 19 |
| Clubbing | 5 | 32 | 49 |
NR indicates not reported.
The percentage of patients with the given characteristic is shown. Percentages are based on the total number of patients in the series, with the exception of cerebrospinal fluid protein, which includes the actual number tested.
Percentage of patients with bone lesions.
Only 28, 23, and 73 patients, respectively, were tested; percentage represents percent positive of those tested.
Polyneuropathy
Peripheral neuropathy is the dominant clinical feature of this disorder (Table 3). By definition, all patients in this series had a peripheral neuropathy. Although neuropathy is typically the presenting symptom, in the present series 5 patients (5%) had a known plasma cell dyscrasia before the onset of the neuropathy.8,22 All patients in this series had increased cerebrospinal fluid protein, increased cerebrospinal fluid opening pressures, and a normal cell count.8 22 Thirty-one patients (31%) had sural nerve biopsy; in most cases, the findings were those of a demyelinating process with axonal loss.
Organomegaly
Fifty patients (50%) had organomegaly. Twenty-six patients (26%) had lymphadenopathy. Of these 26, 15 underwent biopsy: 11 had Castleman disease, and 4 had reactive changes. Twenty-four patients (24%) had hepatomegaly, and 22 (22%) had splenomegaly. No patient had massive lymphadenopathy or organomegaly. The percentage of patients with organomegaly in our series seems lower than that in other series (Table 3).
Endocrinopathy
Endocrine abnormality is a defining feature of POEMS.19 In the present study, 66 patients (67%) had at least one endocrine abnormality at presentation. Later in the course of disease, endocrine abnormalities developed in 7 other patients (7%). Most patients did not have a thorough endocrine evaluation, lowering the reported incidence. Because both diabetes mellitus and hypothyroidism are common endocrine abnormalities, care was taken to assign them as part of the syndrome only if there appeared to be a clear temporal relationship. The overall prevalence of endocrinopathy was similar to that previously reported by others (Table3).22 34
Hypogonadism was most common, though laboratory data were too sparse to determine whether there was primary or secondary failure. Forty-four men (71%) had erectile dysfunction. Twenty-eight of these men had serum testosterone levels measured; all but 4 had low levels. Of those not reporting sexual dysfunction, 5 had low serum testosterone levels. Of the 19 men who had serum prolactin levels measured, none had high levels. Seventeen men had gynecomastia; none of the 4 men tested had high serum estradiol levels. The sexual history of women was less reliably ascertained. Two women had irregular menses, one of whom also had galactorrhea. Serum estradiol levels were normal in all 4 women tested. Among the 25 patients with measured serum prolactin levels, levels were high (range, 26 to 58 μg/mL [26 to 58 ng/L]; normal, less than 23 μg/mL [23 ng/L]) in 3 men and 2 women.
Fourteen patients (14%) had hypothyroidism requiring treatment. Another 12 patients (12%) had mild increases in thyroid-stimulating hormone (5.8 to 13.4 mU/L [5.8 to 13.4 μU/mL]; normal, 0.3 to 5.0 mU/L [0.3 to 5.0 μU/mL]) and normal thyroxine levels; these patients were not treated and therefore not considered to have an endocrine abnormality in this series. The hypothyroidism was primary in 9 patients and secondary in 3. In 3 patients, hypothyroidism was the only endocrine abnormality. The remainder had gonadal or adrenal dysfunction or both. In 6 other patients, hypothyroidism developed during the course of disease; they were not included among those considered to have an endocrine abnormality at presentation (Table 3).
Three patients (3%) had diabetes mellitus, having high fasting glucose and glycosylated hemoglobin levels. Of the 35 patients who had adrenal-pituitary testing, 16 (16%) had abnormalities of the adrenal-pituitary axis at presentation. In another 5 patients, adrenal insufficiency developed later in the course of disease. In total, 9 patients had primary adrenal dysfunction, 3 had secondary adrenal dysfunction, and 10 had insufficient data to make the distinction.
Serum levels of parathyroid hormone were measured in 4 patients and were found to be increased in 3. In one patient hypoparathyroidism was diagnosed 84 months after POEMS syndrome was diagnosed.
Monoclonal plasmaproliferative disorder
By definition, all patients had evidence of a monoclonal plasmaproliferative disorder. Eighty-four patients (85%) had a detectable monoclonal protein in their serum on analysis by immunofixation. These findings are similar to those of Nakanishi et al,8 who found an M component to be present in 75% of patients. The serum protein electrophoresis patterns of 24 of our patients were normal; patterns of 7 patients appeared polyclonal. Had immunofixation not been done, the monoclonal protein would have been missed in these 31 patients. Although 40 patients had a detectable monoclonal protein in their urine, in only 3 patients did urine screening identify a monoclonal plasmaproliferative disorder that had not been detected in the serum. The quantity of monoclonal protein was small in both serum and urine, with a median serum M-spike of 11 g/L (1.1 g/dL) (range, 0.0 to 41 g/L [4.1 g/dL]; only 7 patients had an M-spike more than 20 g/L [2 g/dL]) (Table 2). The median total urine protein was 100 mg per 24 hours.
All patients had a monoclonal λ light chain. Forty-four patients had an immunoglobulin A (IgA) λ, 40 had an IgG λ, and 1 had an IgM λ. For the 12 patients who did not have a monoclonal protein in their serum or urine, a clonal λ plasmaproliferative disorder was demonstrated by immunohistochemical staining of biopsy specimens from sclerotic bone lesions or bone marrow.
Of 90 patients who had a bone marrow biopsy performed, the most common interpretation was “nondiagnostic,” with the predominant feature being a hypercellular or “reactive-appearing” marrow. Twenty-one patients had a normal-appearing marrow. Only 4 patients had more than 20% plasma cells; none of these 4 patients had lytic bone disease or anemia. In 25 patients, there was only a slight increase in plasma cells (Tables 2 and 3). Our finding that 14% of patients had a bone marrow plasmacytosis more than 10% is similar to the 5% to 20% previously reported.8 22
Skin changes
Skin changes were documented in 67 patients (68%) (Table3). The most common abnormality was hyperpigmentation (46 patients), followed by acrocyanosis and plethora (19 patients). The latter 2 features were not well-captured in the other large series, but they are described elsewhere.1,8,22 35 Five patients had skin thickening. Multiple hemangiomas were documented in 9 patients; vascular changes similar to those in Kaposi sarcoma were seen in one of these patients. A necrotizing vasculitis along with hyperpigmentation was present in another patient. Of the 26 patients with hypertrichosis, only 5 had no endocrine abnormality, and only 4 had no other skin abnormalities. The hypertrichosis was either generalized or limited to body parts, such as the extremities or face. Twenty-nine patients had 2 or 3 coexistent skin abnormalities. Although white nails can occur in patients with POEMS syndrome, no mention of this finding was made regarding the patients we studied.
Edema and effusions
On presentation, 29 patients (29%) had some form of extravascular volume overload. Peripheral edema, ascites, and pleural effusions were present in 24, 7, and 3 patients, respectively (Table 3). One patient had a pericardial effusion. The incidence of edema and effusions was lower in our series than in other series; however, if one includes patients in whom edema or effusions developed during the course of disease, the numbers increase to 29, 15, and 9, respectively.
Sclerotic bone lesions
On presentation, 95 patients had at least one abnormality detected on radiographic bone survey (Table 3). Of the 4 patients not presenting with a bone lesion, all had 4 or 5 features of POEMS syndrome, including a clonal plasmaproliferative disorder. In one patient, a sclerotic bone lesion developed 18 months later, yielding a total of 96 patients (97%) with abnormal findings on bone radiography. Of the patients with abnormal findings, all but 2 had sclerotic bone lesions. The radiographs for these 2 patients could not be located to establish whether there was any element of sclerosis associated with the lytic lesions. These 2 patients had solitary lytic lesions. In our experience, lytic lesions in patients with POEMS syndrome tend to have a sclerotic rim. Forty-nine patients had lesions with mixed sclerotic and lytic components. Forty-three patients had a solitary lesion, 22 had 2 or 3 lesions, and 31 had more than 3 lesions (Table 3). These findings are consistent with those of previous publications.8 22 Twenty-two patients underwent biopsy of a sclerotic lesion; results were diagnostic in 20.
Papilledema
Other established features
Thirty-seven patients (37%) had lost more than 10 pounds of body weight at presentation. Thirty-one patients (31%) complained of significant fatigue. Five patients (5%) had recognized clubbing at diagnosis, one of whom had coincident restrictive lung disease. Patients with clubbing seemed to have more extensive disease: all had organomegaly, endocrinopathy, skin changes, peripheral neuropathy, and plasmaproliferative disorder; in all but one of these patients, additional POEMS features developed over time. Thirteen patients (13%) complained of generalized bone pain or arthralgia; only 3 of these patients had diffuse sclerotic lesions. Fifty-three patients (54%) had thrombocytosis, and 18 (18%) had polycythemia (hemoglobin more than 150 g/L [15 g/dL] in women and more than 170 g/L [17 g/dL] in men).
Unusual features
Data from case reports and small series suggest that pulmonary hypertension, congestive heart failure, thrombosis, and renal failure may be part of the POEMS syndrome (Table 1).7,29 36-76 In the present series, 47 patients had one or more of these features.
Fourteen patients had lung disease other than effusion during the course of their illness; 3 had effusion, one of whom also had other pulmonary manifestations. Five patients had pulmonary hypertension. Five patients had restrictive lung disease. In 4 patients, respiratory failure or insufficiency developed within several months before death; 17% of deaths were due to respiratory failure.
Four patients died of complications of renal failure between 34 and 120 months after diagnosis. The renal failure occurred within 6 months before death in 3 patients and 3 years before death in 1. There was associated ascites in 3 of the 4 patients. No renal biopsies were performed. All patients who died of renal failure had coexistent ascites and a capillary leaklike syndrome.
Congestive heart failure and cardiomyopathy were among the presenting features in 3 patients. After treatment of the plasma cell dyscrasia with either radiation or combination chemotherapy, cardiac symptoms resolved in all 3 patients. In 4 other patients, congestive heart failure developed at 12, 30, 56, and 192 months. Each of the cardiac events occurred during a POEMS exacerbation. Two patients had pericarditis within a few months of presentation.
Twenty-one thrombotic events (10 venous, 11 arterial) occurred in 18 patients. Seven patients had 8 thrombotic events predating their diagnosis with POEMS. Eleven patients had 13 events after diagnosis.
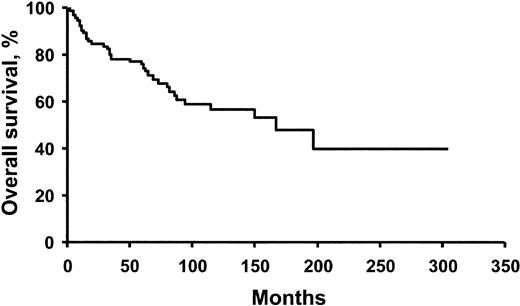
Survival and prognostic features
Overall median survival was 165 months (Figure1). Only fingernail clubbing and extravascular volume overload (edema, effusion, or ascites) were prognostic for survival. Patients with clubbing or extravascular volume overload had a median survival of 31 and 79 months, respectively. These variables were independent of each other, and their corresponding proportional hazard ratios for death were 4.0 (P = .03) and 2.1 (P = .04). Patients who received radiation therapy and those who had a very good or good response to treatment also had superior survival (Figure 2).
Overall survival for 99 patients with POEMS syndrome evaluated at a single institution.
Overall survival for 99 patients with POEMS syndrome evaluated at a single institution.
Survival on the basis of treatment with radiation.
P < .04 for comparison of the 2 groups.
Survival on the basis of treatment with radiation.
P < .04 for comparison of the 2 groups.
When we used the criteria of Bardwick et al,19 median survival for patients with 2, 3, 4, and 5 features at presentation was more than 174, 85, more than 302, and 96 months, respectively; 29%, 50%, 23%, and 34% of the patients in the respective groups have died. When we used the 9 major and minor criteria in Table 1, median survival for patients with 3, 4, 5, 6, 7, 8, and 9 features was more than 174, 85, more than 302, 49, more than 197, 103, and 50 months, respectively (P = not significant) (Figure3); 17%, 47%, 25%, 53%, 25%, 29%, and 100% of the patients in the respective groups have died. In toto, 35 patients have died (Table 4). The most commonly identified causes of death were cardiorespiratory failure and infection. No patient died of classic myeloma—that is, progressive bone marrow failure or hypercalcemia. All patients who died of renal failure had coexistent ascites and a capillary leaklike syndrome.
Survival on the basis of number of features at presentation.
P = not significant. MS indicates median survival; Pts, patients.
Survival on the basis of number of features at presentation.
P = not significant. MS indicates median survival; Pts, patients.
Causes of death among 35 patients
| Cause of death . | No. of patients4-150 . |
|---|---|
| Cardiac event | 74-151,‡ |
| Respiratory failure | 6‡ |
| Infection | 4 |
| POEMS | 3 |
| Cancer | 34-153 |
| Renal failure | 44-155 |
| Unknown | 5 |
| Other | 5# |
| Cause of death . | No. of patients4-150 . |
|---|---|
| Cardiac event | 74-151,‡ |
| Respiratory failure | 6‡ |
| Infection | 4 |
| POEMS | 3 |
| Cancer | 34-153 |
| Renal failure | 44-155 |
| Unknown | 5 |
| Other | 5# |
The deaths of 2 patients were attributed to more than 1 cause.
Includes 3 patients with congestive heart failure.
Includes 1 patient who died of cardiorespiratory arrest.
Includes acute myelogenous leukemia, cholangiocarcinoma, and cancer not otherwise specified.
Includes 1 patient who died of shock and renal failure.
#Includes suicide, cachexia, inanition, shock, and stroke.
Long-term follow-up of patients with POEMS syndrome
Not only are the number of features present at diagnosis not prognostic of survival (Figure 3), but patients often accumulate additional features of POEMS syndrome over time (Table5). In our cohort, the median time between onset of symptoms and diagnosis was 15 months (range, 3-120 months). The respective median times in months from the initial occurrence of symptoms to diagnosis for patients with 2, 3, 4, and 5 features at presentation were 11 (range, 5-60); 13 (range, 3-60); 15 (range, 3-48); and 21 (range, 3-120). Moreover, during follow-up additional classic POEMS characteristics developed in 18 patients; possible POEMS features (congestive heart failure and thrombosis) developed in 7 other patients.
Acquisition of POEMS syndrome features over time
| Patient characteristics . | Initial POEMS features . | Subsequently acquired POEMS features . | TTP, y . | FU, y . | Response to therapy . | Current status . | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| No. . | Sex . | Age, y . | P . | O . | E . | M . | S . | A . | B, no. . | C . | Pap . | |||||
| 1 | F | 66 | P | M | Diff | Hypothyroid, hypoadrenal at 126 mo; ascites, pulmonary hypertension at 156 mo | 10.5 | 14.5 | V gd | Alive | ||||||
| 2 | F | 34 | P | M | 2 or 3 | Ascites, Budd-Chiari at 149 mo; pleural effusion at 156 mo | 12.4 | 13.4 | V gd | Alive | ||||||
| 3 | F | 34 | P | M | S | Diff | Detectable monoclonal protein in serum at 39 mo; hypothyroid at 60 mo; ascites and hepatomegaly at 87 mo | 5.0 | 7.8 | Stable | Dead | |||||
| 4 | M | 46 | P | O | M | A | Diff | Pulmonary hypertension and effusion at 36 mo; hypothyroid at 52 mo; acrocyanosis at 54 mo | 3.0 | 5.8 | Good | Alive | ||||
| 5 | F | 58 | P | M | S | A | Diff | Pap | Hypothyroid at 9 mo; ascites and renal failure at 12 mo | 0.8 | 3.3 | Good | Dead | |||
| 6 | M | 43 | P | M | S | 2 or 3 | Hypoadrenal at 4 mo | 0.3 | 1.0 | Refr | Alive | |||||
| 7 | F | 50 | P | M | S | 1 | Pericardial effusion at 1 mo | 0.1 | 0.2 | Refr | Dead | |||||
| 8 | M | 38 | P | E | M | S | 1 | CHF, hypogonad, hypothyroid, hypoadrenal, peripheral edema, acrocyanosis, hypertrichosis, hyperpigmentation at 192 mo | 16.0 | 16.4 | V gd | Alive | ||||
| 9 | F | 33 | P | E | M | S | 1 | Pap | Peripheral edema at 90 mo | 7.5 | 9.5 | V gd | Alive | |||
| 10 | M | 56 | P | E | M | S | 2 or 3 | Diabetes mellitus at 94 mo | 7.8 | 9.1 | V gd | Alive | ||||
| 11 | F | 44 | P | E | M | S | 1 | Pap | Ascites and CHF at 56 mo | 4.7 | 5.0 | Good | Dead | |||
| 12 | M | 51 | P | O | M | S | Diff | C | Clubbing, ascites, and renal failure at 52 mo | 4.3 | 4.9 | ND | Dead | |||
| 13 | F | 61 | P | E | M | S | 2 or 3 | Ascites at 1 mo | 0.1 | 0.7 | ND | Alive | ||||
| 14 | F | 57 | P | O | E | M | S | A | Diff | Ascites at 22 mo; renal failure and oxygen dependence at 117 mo | 1.8 | 10.0 | V gd | Dead | ||
| 15 | F | 50 | P | O | E | M | S | 2 or 3 | Pap | Ascites at 12 mo; respiratory failure at 66 mo | 1.0 | 5.7 | Good | Dead | ||
| 16 | M | 51 | P | O | E | M | S | 2 or 3 | Hepatomegaly and hepatic dysfunction at 30 mo | 2.5 | 2.8 | Good | Dead | |||
| 17 | M | 39 | P | O | E | M | S | 1 | Lymphadenopathy at 17 mo; restrictive lung disease at 36 mo | 1.4 | 1.4 | Good | Alive | |||
| 18 | M | 64 | P | O | E | M | S | A | Diff | Pap | Hypoparathyroid at 84 mo | 7.0 | 14.6 | Good | Alive | |
| Patient characteristics . | Initial POEMS features . | Subsequently acquired POEMS features . | TTP, y . | FU, y . | Response to therapy . | Current status . | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| No. . | Sex . | Age, y . | P . | O . | E . | M . | S . | A . | B, no. . | C . | Pap . | |||||
| 1 | F | 66 | P | M | Diff | Hypothyroid, hypoadrenal at 126 mo; ascites, pulmonary hypertension at 156 mo | 10.5 | 14.5 | V gd | Alive | ||||||
| 2 | F | 34 | P | M | 2 or 3 | Ascites, Budd-Chiari at 149 mo; pleural effusion at 156 mo | 12.4 | 13.4 | V gd | Alive | ||||||
| 3 | F | 34 | P | M | S | Diff | Detectable monoclonal protein in serum at 39 mo; hypothyroid at 60 mo; ascites and hepatomegaly at 87 mo | 5.0 | 7.8 | Stable | Dead | |||||
| 4 | M | 46 | P | O | M | A | Diff | Pulmonary hypertension and effusion at 36 mo; hypothyroid at 52 mo; acrocyanosis at 54 mo | 3.0 | 5.8 | Good | Alive | ||||
| 5 | F | 58 | P | M | S | A | Diff | Pap | Hypothyroid at 9 mo; ascites and renal failure at 12 mo | 0.8 | 3.3 | Good | Dead | |||
| 6 | M | 43 | P | M | S | 2 or 3 | Hypoadrenal at 4 mo | 0.3 | 1.0 | Refr | Alive | |||||
| 7 | F | 50 | P | M | S | 1 | Pericardial effusion at 1 mo | 0.1 | 0.2 | Refr | Dead | |||||
| 8 | M | 38 | P | E | M | S | 1 | CHF, hypogonad, hypothyroid, hypoadrenal, peripheral edema, acrocyanosis, hypertrichosis, hyperpigmentation at 192 mo | 16.0 | 16.4 | V gd | Alive | ||||
| 9 | F | 33 | P | E | M | S | 1 | Pap | Peripheral edema at 90 mo | 7.5 | 9.5 | V gd | Alive | |||
| 10 | M | 56 | P | E | M | S | 2 or 3 | Diabetes mellitus at 94 mo | 7.8 | 9.1 | V gd | Alive | ||||
| 11 | F | 44 | P | E | M | S | 1 | Pap | Ascites and CHF at 56 mo | 4.7 | 5.0 | Good | Dead | |||
| 12 | M | 51 | P | O | M | S | Diff | C | Clubbing, ascites, and renal failure at 52 mo | 4.3 | 4.9 | ND | Dead | |||
| 13 | F | 61 | P | E | M | S | 2 or 3 | Ascites at 1 mo | 0.1 | 0.7 | ND | Alive | ||||
| 14 | F | 57 | P | O | E | M | S | A | Diff | Ascites at 22 mo; renal failure and oxygen dependence at 117 mo | 1.8 | 10.0 | V gd | Dead | ||
| 15 | F | 50 | P | O | E | M | S | 2 or 3 | Pap | Ascites at 12 mo; respiratory failure at 66 mo | 1.0 | 5.7 | Good | Dead | ||
| 16 | M | 51 | P | O | E | M | S | 2 or 3 | Hepatomegaly and hepatic dysfunction at 30 mo | 2.5 | 2.8 | Good | Dead | |||
| 17 | M | 39 | P | O | E | M | S | 1 | Lymphadenopathy at 17 mo; restrictive lung disease at 36 mo | 1.4 | 1.4 | Good | Alive | |||
| 18 | M | 64 | P | O | E | M | S | A | Diff | Pap | Hypoparathyroid at 84 mo | 7.0 | 14.6 | Good | Alive | |
A indicates anasarca, edema, ascites, or pleural effusion; B, bone lesions; C, Castleman disease; CHF, congestive heart failure; Diff, diffuse; E, endocrinopathy; FU, follow-up; M, monoclonal plasma cell dyscrasia; ND, no data; O, organomegaly (including hepatomegaly, splenomegaly, and lymphadenopathy); P, peripheral neuropathy; Pap, papilledema; Refr, refractory disease; S, skin changes; TTP, time to progression; and V gd, very good.
Seven patients had only 2 of the 5 POEMS features as described by Bardwick et al,19 namely, the monoclonal plasmaproliferative disorder and peripheral neuropathy. All 7 patients had at least 1 osteosclerotic bone lesion; in fact, 6 had more than 1 lesion. Additional POEMS features subsequently developed in 2 (Table5).
Among the 32 patients with 3 features of POEMS, additional features developed in 5 patients 9 to 60 months after the original diagnosis. Among the 31 patients with 4 features of POEMS, other features subsequently developed in 6. Finally, among the 29 patients with all 5 features, other POEMS features developed in 4.
Presenting features were evaluated for their value in predicting the development of other POEMS features. On univariate analysis, the only factors predictive of the development of additional POEMS features were a serum M-spike of more than 1 g/dL (P = .04), the presence of a monoclonal protein in the urine (P = .05), and the absence of radiation therapy (P = .02). On multivariate analysis, only the presence of a urinary monoclonal protein was predictive of the development of additional features (proportional hazards, 4.82; confidence interval, 1.71-13.8;P = .003). Among the 18 patients in whom additional POEMS-associated features developed over time, those patients with the fewest POEMS features as described by Bardwick et al19 had the highest risk of additional features developing (29% vs 14%).
Therapy
Patients were either treated by Mayo Clinic physicians or referred for treatment to their local physicians. Because this was a retrospective analysis, it was difficult to draw firm conclusions regarding therapy. However, we found that 73 patients (74%) had at least some response to therapy (Table 6). Fourteen patients were refractory to the treatments chosen. Sixty-four patients were treated with 70 courses of radiation, 48 with melphalan and prednisone, 15 with alkylator-based combination chemotherapy, 41 with prednisone or dexamethasone alone, 30 with plasmapheresis, and 9 with intravenous immunoglobulin.
Response to therapy in patients with POEMS syndrome
| Treatment . | No. of patients . | Response to treatment, % . | |||
|---|---|---|---|---|---|
| Improved . | Stable . | Progression . | Unknown . | ||
| Radiation | 706-151 | 54 | 4 | 16 | 26 |
| Melphalan and prednisone | 48 | 44 | 12 | 12 | 31 |
| Combination chemotherapy6-150 | 15 | 27 | 7 | 33 | 33 |
| Cyclosporine or azathioprine | 4 | 0 | 0 | 100 | 0 |
| Cyclosporine or azathioprine, plus prednisone | 6 | 50 | 0 | 17 | 33 |
| Prednisone or dexamethasone | 41 | 15 | 7 | 20 | 59 |
| Plasmapheresis | 16 | 0 | 12 | 87 | 0 |
| Plasmapheresis plus prednisone | 14 | 21 | 0 | 14 | 64 |
| Intravenous immunoglobulin | 9 | 0 | 0 | 89 | 11 |
| Treatment . | No. of patients . | Response to treatment, % . | |||
|---|---|---|---|---|---|
| Improved . | Stable . | Progression . | Unknown . | ||
| Radiation | 706-151 | 54 | 4 | 16 | 26 |
| Melphalan and prednisone | 48 | 44 | 12 | 12 | 31 |
| Combination chemotherapy6-150 | 15 | 27 | 7 | 33 | 33 |
| Cyclosporine or azathioprine | 4 | 0 | 0 | 100 | 0 |
| Cyclosporine or azathioprine, plus prednisone | 6 | 50 | 0 | 17 | 33 |
| Prednisone or dexamethasone | 41 | 15 | 7 | 20 | 59 |
| Plasmapheresis | 16 | 0 | 12 | 87 | 0 |
| Plasmapheresis plus prednisone | 14 | 21 | 0 | 14 | 64 |
| Intravenous immunoglobulin | 9 | 0 | 0 | 89 | 11 |
Includes vincristine, carmustine, melphalan, cyclophosphamide, and prednisone; vincristine, doxorubicin, and dexamethasone; cyclophosphamide, doxorubicin, vincristine, and prednisone; and cyclophospharnide-based chemotherapy.
Sixty-four patients were treated with 70 courses of radiation.
A response was defined as stabilization or improvement of symptoms as reported by the patient or the treating physician. Radiation therapy was effective; at least half of patients so treated responded. Only those patients with a solitary lesion or a dominant lesion were treated with radiation. Of the 13 patients who did not respond to radiation, 9 had received less than 4000 cGy. Responses were often inapparent until 3 to 6 months after treatment. Some patients showed continued improvement 1 to 2 years after radiation treatment. Responses of organomegaly and skin changes generally antedated a response of neuropathy.
Clinical responses to prednisone and a combination of melphalan and prednisone occurred in approximately 22% to 56% of patients. Patients receiving plasmapheresis, cyclosporine, or azathioprine responded only if they were also receiving prednisone, suggesting that these agents themselves are ineffective. No response was observed with intravenous immunoglobulin.
Discussion
Clinical features
All patients with POEMS syndrome have peripheral neuropathy and a monoclonal plasma cell dyscrasia or Castleman disease. Hepatomegaly, splenomegaly, lymphadenopathy, endocrinopathy, skin changes, papilledema, peripheral edema, ascites, sclerotic bone lesions, clubbing, polycythemia, thrombocytosis, and fatigue are all features of the syndrome.8 22
The neuropathy is symmetrical and ascending, with either an insidious or rapidly progressing onset. Patients often describe numbness and dysesthesias followed by a progressive ascending weakness that overshadows the sensory impairment. In most patients, it is the presenting symptom; however, in one series edema preceded neuropathy in 12% of patients and coincided with it in 14%.8 In our series, 5 patients had a known antecedent plasmaproliferative disorder. The neuropathy is seldom painful, and autonomic involvement is rare.5 It is typically a chronic, large-fiber sensorimotor neuropathy. Most authors have not found monoclonal immunoglobulin associated with nerve specimens,8,36,37,77 except for Adams and Said78 and Broussolle et al.79
The estimate that 11% to 30% of POEMS patients have Castleman disease is conservative because many patients do not undergo lymph node biopsy.8,22 The association between the 2 disorders is well recognized but poorly understood.8,22,38,47,65 80-114
Endocrine abnormalities are defining features of the syndrome.19 Primary and secondary hypothyroidism, hypogonadism, adrenocortical insufficiency, and diabetes mellitus have been described.19,22,86,97,115,116 Parathyroid hormone abnormalities were found in 4 of our patients and have been reported previously.2,100,117 118
Papilledema, which occurs in 29% to 55% of patients, may be asymptomatic or may cause headache, transient obscurations of vision, scotomata, enlarged blind spots, or progressive constriction of the visual field.8,22,38 119
Sclerotic bone lesions occur in most patients. They may be solitary or multiple. In the series of Soubrier et al,22 prognosis was significantly better for patients with solitary bone lesions. In our series, survival was independent of the number of bone lesions. However, response to therapy was better in patients with radiated dominant bone lesions.
Minimal criteria for the diagnosis and evolution of disease
A table and comparisons of the largest series of patients with the syndrome are provided in “Results.” In Table 1 we list the features associated with POEMS and set forth a proposed model of the minimal criteria needed to establish the diagnosis. Relapse and additional new features can occur even in patients who have responded.7,17,35,48,118,122-125 In our series, this occurred in 18% to 25% of patients, depending on whether one considers congestive heart failure and thrombotic abnormalities to be part of the syndrome. New features can develop more than 10 years after the initial presentation.35 We therefore propose the concept that 2 major criteria and at least 1 minor criterion should be met to establish the diagnosis of POEMS syndrome.
Survival
The prognosis for patients with POEMS has been reported to be poor, with median survivals estimated to be 12 to 33 months.2,8,9 However, this has not been our experience. In the present series, median survival was 165 months. Reports of patients who have had the disease for more than 5 years are not unusual.7,17,35,118,123,125 In one study, 7 of 15 patients were alive for more than 5 years, with 1 patient living for 25 years.126
Our data and those of others demonstrate that survival is not affected by the number of POEMS features,22 although clubbing and extravascular volume overload are associated with shorter survival. In the present series, 35 patients have died. Even patients with multiple bone lesions or those with more than 10% plasma cells do not progress to overt multiple myeloma. Bone fractures rarely develop. The neuropathy may be unrelenting and contribute to progressive inanition and eventual cardiorespiratory failure and pneumonia. Stroke and myocardial infarction, which may or may not be related to the POEMS syndrome, also are observed causes of death.
Less-recognized features
Less-recognized phenomena may be pulmonary hypertension, restrictive lung disease, cardiomyopathy, and an increased incidence of arterial and venous thrombosis.
At least 13 cases of pulmonary hypertension in patients with POEMS syndrome have been reported in previous series.36-45 In the present series, we report an additional 5. Moreover, restrictive lung disease was recognized in another 5% of our patients, and 20% of deaths were related to respiratory failure. In a series of 20 patients with POEMS followed up during a 10-year period, 25% had pulmonary hypertension.43
Cardiomyopathy and congestive heart disease were observed in 7 of our patients. These conditions have been reported in 3 other cases.7,42 46
Both arterial and venous thromboses have been described in patients with POEMS syndrome. In our series, there were 18 patients with stroke, myocardial infarction, and Budd-Chiari syndrome. Lesprit et al26 observed 4 of 20 patients to have arterial occlusion. An additional 15 patients with gangrene, ischemia, myocardial infarction, splenic infarcts, and strokes have been reported.47-60 Vasospastic angina,61,62pulmonary embolism, and Budd-Chiari syndrome also have been described.63 64
In 4 of our patients, renal failure developed as a preterminal event. The renal histologic characteristics of patients with POEMS have been described.29,36,48,65-76 Almost one half of these patients had coexistent Castleman disease. Light-chain deposition is not observed. Instead, membranoproliferative features and evidence of endothelial injury are characteristic.36,48,66 71-73
Treatment strategies
Because the pathogenesis of this multisystem disease is unclear, treatment is not standardized. The λ light chain has been implicated because less than 5% of patients with POEMS syndrome have monoclonal κ.5,8,9,34,78,104,124,127,128 The hypothesis implicating vascular endothelial growth factor25,28,30,37,65,99,126,129-131 eventually may be validated, providing a uniform target for therapy. To avoid the risk of systemic alkylator exposure, most would agree that for an isolated plasmacytoma, radiation is the preferred treatment.3,11,79,120,132 Systemic and skin symptoms tend to respond sooner than do symptoms of neuropathy, with the former beginning to respond within 1 month and the latter within 3 to 6 months. Besides radiation, many strategies have been used, including plasmapheresis, intravenous immunoglobulin, interferon alfa, corticosteroids, alkylators, azathioprine, autologous stem cell transplantation, tamoxifen, and transretinoic acid.3,7,8,11,20,21,48,63,71,79,96,97,100,105-107,118,120,122,125,127,130,132-144On the basis of our experience and reports in the literature,105,125,134 neither plasmapheresis nor intravenous immunoglobulin is effective treatment. Alkylators with or without corticosteroids are effective in some patients.7,100,105 High-dose chemotherapy with autologous stem cell support may be considered.143-146
Screening for the syndrome
Screening for POEMS syndrome with serum protein electrophoresis alone is inadequate. Immunofixation of serum and urine and metastatic bone survey are essential for all patients with unexplained peripheral neuropathy. If the index of suspicion is high enough, bone marrow aspirate and biopsy with immunostaining may be required. The predominance of monoclonal λ cannot be overemphasized. Skin, viscera, lymph nodes, and optic fundi should be examined carefully. If the diagnosis is strongly suspected, a thorough endocrine evaluation should be performed. If the patient has respiratory symptoms, pulmonary function testing and echocardiography should be performed.
Final comments
We propose that the diagnosis of POEMS syndrome be predicated on the presence of major and minor criteria. Two major criteria and at least one minor criterion should be satisfied to differentiate this syndrome from neuropathy associated with monoclonal gammopathy of undetermined significance, myeloma, and Waldenström disease. Primary systemic amyloidosis also should be excluded. The major criteria include a polyneuropathy and a clonal plasmaproliferative disorder (almost always λ). The minor criteria include osteosclerotic bone lesions; Castleman disease; papilledema; organomegaly, including lymphadenopathy; edema, pleural effusion, or ascites; endocrinopathy; and skin changes.
Survival for patients with POEMS syndrome is better than previously reported, with median survival of 165 months, regardless of how many syndrome features, bone lesions, or plasma cells are present at diagnosis. Patients do not have the usual complications of classic multiple myeloma. Radiation and chemotherapy are the most useful therapies. Ultimately, manipulation of the cytokine milieu may be the treatment of choice.
Prepublished online as Blood First Edition Paper, November 27, 2002; DOI 10.1182/blood- 2002-07-2299.
Supported in part by grants CA62242 and CA91561 from the National Institutes of Health.
The publication costs of this article were defrayed in part by page charge payment. Therefore, and solely to indicate this fact, this article is hereby marked “advertisement” in accordance with 18 U.S.C. section 1734.
References
Author notes
Angela Dispenzieri, Division of Hematology and Internal Medicine, Mayo Clinic, 200 First St SW, Rochester, MN 55905; e-mail:dispenzieri.angela@mayo.edu.



This feature is available to Subscribers Only
Sign In or Create an Account Close Modal