Abstract
Abstract 991
The outcome of patients with DLBCL has significantly improved with the addition of rituximab to CHOP chemotherapy. While standard clinical prognostic factors such as those included in the International Prognostic Index (IPI) still predict outcome in DLBCL in R-CHOP treated patients, predicting the outcome of patients might be further refined using biological factors. We therefore tested whether pretreatment serum cytokines, that measure the biological activity of the tumor as well as the host response, could provide additional prognostic information in DLBCL patients.
Newly diagnosed DLBCL patients were prospectively enrolled in the University of Iowa/Mayo Clinic SPORE Molecular Epidemiology Resource (MER). Serum cytokines were measured from pre-treatment blood draws using a multiplex ELISA (Upstate Cell Signaling Solutions, Lake Placid, NY). Thirty cytokines, including pro-inflammatory, Th1 and Th2 associated cytokines, were analyzed using the Luminex-100 system Version 1.7 (Luminex, Austin, TX). Data analysis was performed using the MasterPlex QT 1.0 system (MiraiBio, Alameda, CA). The assay was also performed on research serum draws from 400 non-lymphoma epidemiology controls enrolled on a corresponding lymphoma etiology case-control study. The upper limit of normal for each cytokine was defined as the 95th percentile from the control distribution. Clinical data was abstracted using a standard protocol for the MER and patients were followed systematically for event-free (progression, retreatment, or death due to any cause) and overall survival (EFS and OS, respectively). Cox proportional hazards models were used to evaluate the association between cytokines and outcome. Principal components analysis (PCA) was performed on the combined DLBCL and control cytokine dataset, agnostic to clinical characteristics and outcome, to identify cytokine profiles.
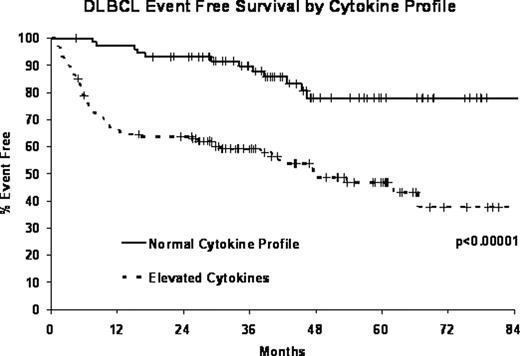
206 DLBCL patients diagnosed between September 2002 and February 2008 with available serum were included. The median age was 64 years (range 20–92) and 52% were male. At a medium follow-up of 47 months (range 5–94), 75 patients (36%) had relapsed and 63 patients had died (31%). A cytokine profile was determined based on the first two principal components (PC) of the PCA analyses with PC1 corresponding to a general (host) cytokine elevation (also seen in normal controls) and PC2 corresponding to an increase predominantly in cytokines that were commonly elevated in DLBCL patients. 75 DLBCL patients (36%) had a normal cytokine profile similar to the general population of controls; 114 DLBCL patients (55%) had elevation in tumor specific cytokines (CXCL10, CXCL9, IL-2R, IL-12, IL-8, and IL-10) and 17 (8%) had a general cytokine elevation. Patients with any elevation of cytokines (tumor specific or general elevation) had a significantly worse event-free (HR=3.96, 95% CI: 2.13–7.37, p<0.00001) and overall survival (HR=3.75, 95% CI: 1.99–7.09, p<0.0001) than those with a normal cytokine profile (see figure). While the cytokine elevations were associated with advanced stage, poor performance score and elevated LDH, they were not associated with advanced age or extranodal disease and the results remained significant after adjustment for the IPI and treatment in the Cox model (EFS HR=3.11, 95% CI: 1.66–5.85, p<0.0001; OS HR=2.93, 95% CI: 1.53–5.63, p=0.001). Elevated serum cytokines also identified patients who were unlikely to complete initial therapy or who relapsed early. In low-risk patients (IPI 0–2), only 3% of patients with normal serum cytokines relapsed in the first 12 months compared to 23% of patients with elevated cytokines. Similarly in the high-risk group (IPI 3–5), none of the patients with normal cytokines relapsed in the first year compared to 43% with elevated cytokines.
Elevated pretreatment serum cytokines, predominantly related to the malignancy, are associated with an increased likelihood of disease relapse and an inferior survival in patients with DLBCL. Furthermore, the pretreatment cytokine profile may also identify DLBCL patients at high risk for early disease relapse.
No relevant conflicts of interest to declare.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal