Abstract
Maintaining results of successful induction therapy is an important goal in multiple myeloma. Here, members of the International Myeloma Working Group review the relevant data. Thalidomide maintenance therapy after autologous stem cell transplantation improved the quality of response and increased progression-free survival (PFS) significantly in all 6 studies and overall survival (OS) in 3 of them. In elderly patients, 2 trials showed a significant prolongation of PFS, but no improvement in OS. A meta-analysis revealed a significant risk reduction for PFS/event-free survival and death. The role of thalidomide maintenance after melphalan, prednisone, and thalidomide is not well established. Two trials with lenalidomide maintenance treatment after autologous stem cell transplantation and one study after conventional melphalan, prednisone, and lenalidomide induction therapy showed a significant risk reduction for PFS and an increase in OS in one of the transplant trials. Maintenance therapy with single-agent bortezomib or in combination with thalidomide or prednisone has been studied. One trial revealed a significantly increased OS with a bortezomib-based induction and bortezomib maintenance therapy compared with conventional induction and thalidomide maintenance treatment. Maintenance treatment can be associated with significant side effects, and none of the drugs evaluated is approved for maintenance therapy. Treatment decisions for individual patients must balance potential benefits and risks carefully, as a widely agreed-on standard is not established.
Introduction
Maintaining the response of first-line therapy is an important objective in multiple myeloma (MM), where even the most intensive therapy followed by autologous stem cell transplantation (ASCT) is usually unable to extend progression-free survival (PFS) to beyond 36 months, with the majority of patients eventually experiencing relapse. Two different concepts regarding treatment after the initial induction therapy exist: consolidation versus maintenance therapy. Whereas consolidation therapy typically consists of the application of a short course of treatment with the aim of deepening the response achieved with the initial therapy (ie, further reducing the number of tumor cells), maintenance therapy is applied for a prolonged period of time with the goal of preventing tumor progression. To date, no clinical trial has specifically compared consolidation versus maintenance approaches to assess the benefit of one approach over the other.
The high efficacy of the 3 novel agents, thalidomide, bortezomib, and lenalidomide, observed in the front-line and relapse settings has provided the rationale to also test their capacity to maintain the benefits of first-line therapy to prolong remission, a period usually devoid of symptoms of the disease and of toxicities of therapy, and importantly, to extend overall survival (OS). However, it should be noted that the achievement of an OS benefit of a maintenance therapy may be difficult when effective salvage treatment is available at relapse. The demonstration of a prolonged time to progression seems to be a valid objective, provided the prolonged time span without progression of disease is associated with better quality of life and evidently of benefit to the patient.1
The first attempts with maintenance therapy were already undertaken with conventional chemotherapy agents shortly after their effectiveness in MM had been demonstrated.2-4 Results of these initial and of later studies5-9 were unsatisfactory, and so efforts to improve the outcome of maintenance concepts are ongoing. Here we review current results obtained with novel drugs for maintenance treatment.
Methods
Members of the International Myeloma Working Group met twice during the IMF summits on the occasion of the European Hematology Association meetings in 2010 and 2011 to review and discuss the evidence for maintenance treatment with novel agents and to formulate recommendations for clinical practice. All relevant data published in the literature or presented at meetings of the American Society of Oncology, American Society of Hematology, European Hematology Association, and the International Myeloma Workshop were considered.
For meta-analysis, randomized controlled trials of patients receiving thalidomide, thalidomide combination, or lenalidomide maintenance therapy were included. Extraction of summary statistics from the published data were performed according to standard methods for survival-type endpoints, with hazard ratios (HRs) and their CIs as preferred sources for estimation, and log-rank P values/event counts as second choice.10 Standard techniques for meta-analysis11 were used to calculate the pooled estimates, as incorporated in the software packages METASUB Version 1.1 (idv) and Review Manager Version 4.2 (Nordic Cochrane Center). Both fixed (primarily) and random effects model methodology were applied. All reported P values result from 2-sided versions of the respective tests.
Results and discussion
Chemotherapy, interferon, and glucocorticosteroids
The first trials designed to prolong the duration of the remission phase and OS simply continued chemotherapy after successful induction treatment with melphalan and prednisone (MP).2-4 This led to a significant prolongation of the duration of remission but not to superior survival, and thus was not pursued further.
Interferon was shown to exert anti-myeloma activity as a single agent in 1979,12 and subsequent trials used interferon for induction and for maintenance therapy. Individual trials revealed variable results, with significant prolongation of remission duration and also of survival in some, and negative outcomes in other studies. Two meta-analyses, one on individual patient data5 and the other using published data,6 revealed a significant but limited improvement in both remission duration and survival of approximately 6 months. Because of toxicity and the inability to select those patients likely to benefit from and tolerate interferon, this concept has, with few exceptions, generally been abandoned.
Glucocorticosteroids have significant activity in myeloma as single agents13 and induce additive or synergistic activity in combination with other drugs.14 Berenson et al showed a significant increase in remission duration and in survival with 50 mg prednisone every other day compared with 10 mg every other day,7 but in another study with single-agent dexamethasone (40 mg days 1-4, every 28 days), no benefit was observed.8 A comparison of dexamethasone with interferon maintenance treatment showed similar remission durations, but more relapsing patients could be reinduced with melphalan-dexamethasone after interferon maintenance therapy than after dexamethasone.9 Taken together, the available evidence is insufficient for recommending corticosteroid maintenance therapy.
Thalidomide
After the demonstration of the limited benefits of interferon5,6 and corticosteroids7-9 as maintenance therapy, thalidomide became the next logical candidate for clinical evaluation. The absence of severe hematotoxicity and its availability as an oral drug were favorable prerequisites for long-term use, but these advantages proved partly abrogated by its specific toxicity profile, in particular neurotoxicity. Thalidomide as maintenance treatment has mainly been studied in young patients after ASCT.
Three of the 6 trials15,16,22 with thalidomide maintenance treatment after ASCT15-22 used thalidomide only as maintenance treatment. In 2 studies, thalidomide was administered both during the induction and maintenance phases,18,21 whereas in the Medical Research Council (MRC) Myeloma IX study,17 approximately half of the patients randomized to thalidomide maintenance treatment had thalidomide during induction therapy (Table 1).
Thalidomide maintenance studies after ASCT and conventional therapy
| Study group . | Median age, y (no. of patients) . | Induction therapy . | Maintenance dose, duration of treatment . | Improvement in quality of response . | EFS or PFS* . | OS* . | Survival after relapse . | Thalidomide tolerance . |
|---|---|---|---|---|---|---|---|---|
| IFM 99-02: Attal et al15 (2006) | Mean 59 ± 8 (N = 597) | VAD: 3 or 4 cycles, Single ASCT | (A) Thalidomide 400 mg/d until PD | VGPR: (A) 67% | 3-y EFS: (A) 52% | 4-y OS: (A) 87% | 1-y OS: (A) 75% | 39% stopped thalidomide because of side effects, mostly PNP, all grades of PNP 68%, grades 3 or 4: 7% |
| Pamidronate 90 mg, every 4 wks, until PD | ||||||||
| (B) Pamidronate 90 mg, every 4 wks, until PD | (B) 55% | (B) 37% | (B) 74% | (B) 73% | ||||
| (C) None | (C) 57% | (C) 36% | (C) 77% | (C) 78% | ||||
| P = .03 | P < .009 | P < .04 | P = .7 | |||||
| ALLG MM6: Spencer et al16 (2009) | ≤ 70 (N = 243) | Mostly VAD Single ASCT | (A) Thalidomide 100-200 mg/d, for 12 mo | VGPR: (A) 65% | 3-y PFS estimate: (A) 42% | 3-y OS estimate: (A) 86% | 1-y OS estimate: (A) 79% | 30% stopped therapy because of intolerance (mostly PNP), 10% grades 3 or 4 PNP and 9% stopped because of PD |
| Prednisolone 50 mg on alternate days until PD | ||||||||
| (B) Prednisolone 50 mg on alternate days until PD | (B) 44% | (B) 23% | (B) 75% | (B) 77% | ||||
| P = .001 | P < .001 | P = .004 | P = .237 | |||||
| MRC Myeloma IX: Morgan et al17 (2012) | Intensive, 59 (N = 493) | CVAD vs CTD, single ASCT | (A) Thalidomide, 50-100 mg/day, until PD† | No difference in the percentage of patients that upgraded response status P = .19 | PFS: (A) 30 mo | 3-year OS: (A) 75% | (A) 20 mo | 52.2% discontinued maintenance before PD mainly because of adverse events, median duration of treatment: 7 mo‡ |
| (B) None† | (B) 27 mo P = .003 | (B) 80% P = .26 | (B) 36 mo P = .003 | |||||
| Nonintensive, 73 (N = 327) | CTD attenuated vs MP | (A) Thalidomide, 50-100 mg/day, until PD† | PFS: (A) 11 mo | (A) 38 mo | (A) 21 mo | |||
| (B) None† | (B) 9 mo P = .014 | (B) 39 mo P = .995 | (B) 26 mo P = .25 | |||||
| TT2: Barlogie et al18 (2006) | ≤ 75, median NA (N = 668) Median follow-up: 42 mo | (A) 4 induction cycles, double ASCT 4 consolidation cycles, thalidomide 400 mg/d during induction, 100 mg between ASCT, 200 mg with consolidation | (A) Thalidomide 100 mg during the first year, thereafter 50 mg on alternate days, until PD | CR: (A) 62% | 4-y EFS: A) 65% | OS: A) Not stated | Median OS: A) 1.1 y | 30% stopped thalidomide within 2 y |
| (B) Same induction without thalidomide | (B) None | (B) 43% P = .001 | (B) 44% P = .01 | (B) Not stated P = .9 | (B) 2.7 y P = .001 | |||
| TT2: Barlogie et al19 (2008) | Median follow-up: 70 mo | CR: (A) 64%† | EFS median: (A) 6.0 y | 8-y OS estimate: (A) 57% | 5-y OS estimate: (A) 27% | ∼ 80% stopped thalidomide because of toxicity within 2 y† | ||
| (B) 43% | (B) 4.1 y | (B) 44% | (B) 23% | |||||
| P = .001 | P = .001 | P = .09 | P = .11 | |||||
| TT2: Barlogie et al20 (2010) | Median follow-up: 87 mo (N = 668) | NA | EFS median: 4.8 y | OS median 9 y | 7.2 y OS estimate: | NA | ||
| (A) 45.2% | ||||||||
| (B) 42.2% | ||||||||
| P = .27 | ||||||||
| HOVON 50: Lokhorst et al21 (2008) | 56 (N = 556) | VAD vs TAD Single or double ASCT | (A) Thalidomide, 50 mg/d, until PD | VGPR: | EFS: | Median: | Median OS: | PNP grades 2-4: ∼ 50% Treatment discontinued or dose reduced: 58% |
| (A) 66% | (A) 34 mo | (A) 73 mo | (A) 20 mo | |||||
| (B) 22 mo, P < .001 | ||||||||
| (B) IFN-α, 3 MU, 3 times weekly, until PD | (B) 54% | PFS: | (B) 60 mo | (B) 31 mo | ||||
| P = .005 | (A) 34 mo | P = .77 | P = .009 | |||||
| (B) 25 mo P < .001 | ||||||||
| NCIC CTG MY10: Stewart et al22 (2010) | 58 (N = 332) | Induction therapy not specified Single ASCT | (A) Thalidomide 200 mg/d and alternate-day prednisone 50 mg, until PD | PFS: (A) 28 mo | 4-y OS estimate: (A) 68% | Increased toxicity, including PNP and reduced quality of life, improved appetite, and sleep VTE: 7% | ||
| (B) None | (B) 17 mo | (B) 60% | VTE: 0% | |||||
| P < .0001 | P = .21 | |||||||
| CEMSG: Ludwig et al25 (2010) | 72 (N = 124) | Thalidomide/dexamethasone vs MP | (A) Thalidomide 200 mg up to maximum tolerated dose, until PD IFN-α-2b, 3 MU, 3 times weekly | (A) PR to VGPR or CR: 8% | PFS: (A) 27.7 mo | (A) 52.6 mo | OS after PD: (A) 8.1 mo | PNP grades 3 or 4: 11% |
| (B) IFN-α-2b, 3 MU, 3 times weekly | (B) PR to VGPR or CR: 2% | (B) 13.2 mo P = .0068 | (B) 51.4 mo P = .81 | (B) 25.5 mo P = .056 |
| Study group . | Median age, y (no. of patients) . | Induction therapy . | Maintenance dose, duration of treatment . | Improvement in quality of response . | EFS or PFS* . | OS* . | Survival after relapse . | Thalidomide tolerance . |
|---|---|---|---|---|---|---|---|---|
| IFM 99-02: Attal et al15 (2006) | Mean 59 ± 8 (N = 597) | VAD: 3 or 4 cycles, Single ASCT | (A) Thalidomide 400 mg/d until PD | VGPR: (A) 67% | 3-y EFS: (A) 52% | 4-y OS: (A) 87% | 1-y OS: (A) 75% | 39% stopped thalidomide because of side effects, mostly PNP, all grades of PNP 68%, grades 3 or 4: 7% |
| Pamidronate 90 mg, every 4 wks, until PD | ||||||||
| (B) Pamidronate 90 mg, every 4 wks, until PD | (B) 55% | (B) 37% | (B) 74% | (B) 73% | ||||
| (C) None | (C) 57% | (C) 36% | (C) 77% | (C) 78% | ||||
| P = .03 | P < .009 | P < .04 | P = .7 | |||||
| ALLG MM6: Spencer et al16 (2009) | ≤ 70 (N = 243) | Mostly VAD Single ASCT | (A) Thalidomide 100-200 mg/d, for 12 mo | VGPR: (A) 65% | 3-y PFS estimate: (A) 42% | 3-y OS estimate: (A) 86% | 1-y OS estimate: (A) 79% | 30% stopped therapy because of intolerance (mostly PNP), 10% grades 3 or 4 PNP and 9% stopped because of PD |
| Prednisolone 50 mg on alternate days until PD | ||||||||
| (B) Prednisolone 50 mg on alternate days until PD | (B) 44% | (B) 23% | (B) 75% | (B) 77% | ||||
| P = .001 | P < .001 | P = .004 | P = .237 | |||||
| MRC Myeloma IX: Morgan et al17 (2012) | Intensive, 59 (N = 493) | CVAD vs CTD, single ASCT | (A) Thalidomide, 50-100 mg/day, until PD† | No difference in the percentage of patients that upgraded response status P = .19 | PFS: (A) 30 mo | 3-year OS: (A) 75% | (A) 20 mo | 52.2% discontinued maintenance before PD mainly because of adverse events, median duration of treatment: 7 mo‡ |
| (B) None† | (B) 27 mo P = .003 | (B) 80% P = .26 | (B) 36 mo P = .003 | |||||
| Nonintensive, 73 (N = 327) | CTD attenuated vs MP | (A) Thalidomide, 50-100 mg/day, until PD† | PFS: (A) 11 mo | (A) 38 mo | (A) 21 mo | |||
| (B) None† | (B) 9 mo P = .014 | (B) 39 mo P = .995 | (B) 26 mo P = .25 | |||||
| TT2: Barlogie et al18 (2006) | ≤ 75, median NA (N = 668) Median follow-up: 42 mo | (A) 4 induction cycles, double ASCT 4 consolidation cycles, thalidomide 400 mg/d during induction, 100 mg between ASCT, 200 mg with consolidation | (A) Thalidomide 100 mg during the first year, thereafter 50 mg on alternate days, until PD | CR: (A) 62% | 4-y EFS: A) 65% | OS: A) Not stated | Median OS: A) 1.1 y | 30% stopped thalidomide within 2 y |
| (B) Same induction without thalidomide | (B) None | (B) 43% P = .001 | (B) 44% P = .01 | (B) Not stated P = .9 | (B) 2.7 y P = .001 | |||
| TT2: Barlogie et al19 (2008) | Median follow-up: 70 mo | CR: (A) 64%† | EFS median: (A) 6.0 y | 8-y OS estimate: (A) 57% | 5-y OS estimate: (A) 27% | ∼ 80% stopped thalidomide because of toxicity within 2 y† | ||
| (B) 43% | (B) 4.1 y | (B) 44% | (B) 23% | |||||
| P = .001 | P = .001 | P = .09 | P = .11 | |||||
| TT2: Barlogie et al20 (2010) | Median follow-up: 87 mo (N = 668) | NA | EFS median: 4.8 y | OS median 9 y | 7.2 y OS estimate: | NA | ||
| (A) 45.2% | ||||||||
| (B) 42.2% | ||||||||
| P = .27 | ||||||||
| HOVON 50: Lokhorst et al21 (2008) | 56 (N = 556) | VAD vs TAD Single or double ASCT | (A) Thalidomide, 50 mg/d, until PD | VGPR: | EFS: | Median: | Median OS: | PNP grades 2-4: ∼ 50% Treatment discontinued or dose reduced: 58% |
| (A) 66% | (A) 34 mo | (A) 73 mo | (A) 20 mo | |||||
| (B) 22 mo, P < .001 | ||||||||
| (B) IFN-α, 3 MU, 3 times weekly, until PD | (B) 54% | PFS: | (B) 60 mo | (B) 31 mo | ||||
| P = .005 | (A) 34 mo | P = .77 | P = .009 | |||||
| (B) 25 mo P < .001 | ||||||||
| NCIC CTG MY10: Stewart et al22 (2010) | 58 (N = 332) | Induction therapy not specified Single ASCT | (A) Thalidomide 200 mg/d and alternate-day prednisone 50 mg, until PD | PFS: (A) 28 mo | 4-y OS estimate: (A) 68% | Increased toxicity, including PNP and reduced quality of life, improved appetite, and sleep VTE: 7% | ||
| (B) None | (B) 17 mo | (B) 60% | VTE: 0% | |||||
| P < .0001 | P = .21 | |||||||
| CEMSG: Ludwig et al25 (2010) | 72 (N = 124) | Thalidomide/dexamethasone vs MP | (A) Thalidomide 200 mg up to maximum tolerated dose, until PD IFN-α-2b, 3 MU, 3 times weekly | (A) PR to VGPR or CR: 8% | PFS: (A) 27.7 mo | (A) 52.6 mo | OS after PD: (A) 8.1 mo | PNP grades 3 or 4: 11% |
| (B) IFN-α-2b, 3 MU, 3 times weekly | (B) PR to VGPR or CR: 2% | (B) 13.2 mo P = .0068 | (B) 51.4 mo P = .81 | (B) 25.5 mo P = .056 |
Data are median values unless otherwise stated.
Same regimen for intensive and nonintensive patients.
Results for intensive and nonintensive group combined.
In the Intergroupe Francophone du Myélome (IFM) 99 02 study, patients were randomized after double ASCT to thalidomide plus pamidronate, to pamidronate alone, or to control.15 A significant improvement in the quality of response was observed in the thalidomide-containing arm, with more patients achieving very good partial response (VGPR) or complete response (CR) compared with the 2 other groups. Furthermore, an increased event-free survival (EFS), as well as improved OS could be shown, but the benefits of thalidomide maintenance therapy were seen only in patients with less than VGPR after double ASCT, and only in those without del13 and high β2-microglobulin. Survival after relapse did not vary between the 3 study arms. After long-term follow-up of patients with cytogenetics available (thereby excluding 90 patients),20 the initially observed survival benefit was not maintained, with an estimated 5-year OS rate of 74% in the thalidomide-pamidronate arm and 70% in both control groups (P = .53).
In the Australian trial,16 patients were randomized after single ASCT to either thalidomide maintenance treatment in combination with alternate-day prednisolone or to prednisolone alone. Treatment with thalidomide was planned for 12 months, but alternate-day prednisolone could be continued in both arms until progression. Fifty-eight percent of the patients initially randomized to thalidomide remained on maintenance therapy. The thalidomide-containing treatment resulted in a higher rate of VGPR, increased PFS, and increased OS. OS after relapse did not differ between the 2 groups.
The MRC myeloma IX study consists of 2 trials, one in younger and the other in older patients.17 In the entire patient group, no difference was noted in the percentage of patients that upgraded response status. In the transplant study, thalidomide maintenance treatment resulted in increased PFS, whereas for the survival rate at 3 years no improvement was obtained. Survival regarding FISH-defined cytogenetic risk groups was assessed in both patient cohorts combined. In patients with favorable FISH, PFS was significantly prolonged with thalidomide maintenance therapy (P = .004) with no apparent improvement yet of OS (P = .48), but survival curves indicate a likely late survival benefit after longer follow-up. Patients with adverse FISH [t(4;14), t(14;16), t(14;20), del17p, del 1p32), gain 1q21] showed similar PFS (9 vs 12 months, P = .48) but worse OS (P = .009) with thalidomide maintenance.17
Barlogie et al compared thalidomide in combination with Total Therapy II (TT2) and posttransplant chemotherapy with the same chemotherapy without thalidomide.18-20 Maintenance thalidomide was given until disease progression (PD) or intolerance. After a median follow-up of 40 months, both a significantly higher CR rate and EFS at 4 years were noted, whereas for OS no difference was observed. After relapse, survival was significantly shorter in patients pre-exposed to thalidomide.20 A reanalysis after a median follow-up of 6 years revealed a survival estimate of 57% in the experimental arm and of 44% (P = .09) in the control arm.19 EFS was superior in the thalidomide arm, with a median of 6.0 years versus 4.1 years (P = .001). Patients with metaphase-defined cytogenetic risk factors had significantly longer survival (OS at 5 years, 56% vs 43%, P = .02). The cumulative frequency of CR was significantly higher in the thalidomide group, regardless of cytogenetic status. Segregation of survival curves became evident 2 to 3 years after the start of therapy in patients with cytogenetic abnormalities, and after 7 years in those without. Survival after relapse was significantly longer in control patients without cytogenetic abnormalities (5-year OS estimate, 25% vs 6%, P = .04), but was similar between both treated and untreated patients with cytogenetic risk factors (5-year OS estimate, 29% vs 33%, P = .99). A further reanalysis after an additional 38 months of follow-up, for a total follow-up of 87 months, finally showed OS to be significantly extended in the thalidomide arm (P = .04), despite discontinuation of thalidomide for toxicity and other reasons in nearly 80% within 2 years.20
In the HOVON-50 study,20 patients were randomized to either thalidomide, adriamycin, dexamethasone (TAD) followed by single or double ASCT and maintenance therapy with low-dose thalidomide (50 mg/day) or to vincristine, adriamycin, and dexamethasone (VAD) followed by single or double ASCT and maintenance treatment with interferon-α. Maintenance treatment was given until progression. Patients randomized to thalidomide maintenance achieved a significantly higher VGPR rate, longer EFS, and a tendency for improved OS. Survival after relapse was significantly shorter in patients exposed to thalidomide induction and maintenance treatment. Fifty percent of patients developed peripheral neuropathy (PNP), and 58% had dose reductions or discontinued thalidomide.
The National Cancer Institute of Canada CTG (NCIC CTG) trial22 randomized patients to either thalidomide 200 mg daily and alternate-day prednisone (50 mg) or control. After a median follow-up of 4 years, the survival rate was 68% for the maintenance group and 60% for the control group (P = .21). PFS was significantly longer for patients randomized to maintenance therapy. Quality of life was inferior in patients on maintenance therapy in most domains, with the exception of appetite and sleep, which were better with thalidomide/prednisone therapy.
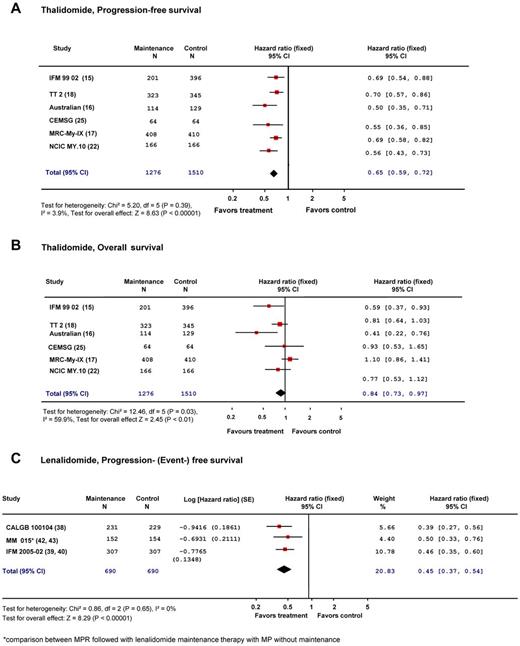
A recently presented meta-analysis of 5 of the 6 transplant studies revealed a significant improvement in PFS (HR = 0.64, 95% CI, 0.55-0.75, P < .001) and OS (HR = 0.73, 95% CI, 0.60-0.89, P = .002) with thalidomide maintenance therapy.23 Grade 3 or 4 PNP (reported in 2 trials) was worse with thalidomide (relative risk = 6.97, 95% CI, 1.44-33.78, P = .02), and grade 3 or 4 thromboembolic complications (reported in 4 studies) were more common (relative risk = 2.01, 95% CI, 0.96-4.23, P = .07) in the thalidomide arms; for other toxicities, no relevant difference was noted.
Our meta-analysis of the published trial results revealed a significant reduction of the risk for progression (HR = 0.65, 95% CI, 0.59-0.72) with thalidomide maintenance therapy. Outcome did not differ between trials that used thalidomide during the maintenance phase only and those that used thalidomide both for induction and maintenance treatment. For OS a major effect of variability between trials was noted (test for heterogeneity, P = .03). Therefore, the positive result for overall effect (HR = 0.84, 95% CI, 0.73-0.97, P = .01) must be interpreted with caution. The most likely explanation for this heterogeneity is the inclusion of elderly patients in the MRC and GEMSG trial, where no improvement in OS was noted. The variability for OS in the thalidomide trials might also be explained by the availability of novel agents at relapse, which differed among countries and for different time periods.
The improvement in quality of response with thalidomide maintenance reported in most trials15,16,18,21,22 supports a consolidation in addition to a maintenance effect of thalidomide. Patients with unfavorable cytogenetics defined by FISH did not benefit from thalidomide maintenance in the IFM and the MRC IX studies; indeed, in the latter trial, survival was significantly shorter in patients with FISH-defined adverse cytogenetics.17 These observations and evidence from other studies suggest that patients without FISH-defined cytogenetic risk factors are more likely to benefit from thalidomide maintenance treatment, whereas those with a FISH-defined high-risk profile likely should not be offered this form of maintenance therapy. In Arkansas, genetic risk is defined both by metaphase cytogenetics and more recently by gene expression profiling.24 Patients defined this way are only partly comparable with FISH-defined high-risk patients, which may explain the greater benefit of thalidomide in the Arkansas high-risk group.
An interesting phenomenon of different outcomes at different periods of trial maturity was noted in the TT2, the IFM, and the MRC IX trials. In the TT2 study, OS was not different after 42 months of follow-up, became superior in patients with metaphase-defined adverse cytogenetics after 70 months, and was significantly longer in the total group of patients after 87 months of follow-up.20 In the IFM study, an analysis of 88% of patients initially enrolled revealed an inverse pattern, with a significant advantage seen at first analysis that was lost at later follow-up.20 The pattern of increasing benefit in the TT2 trial indicates the favorable impact of thalidomide maintenance primarily in good-risk patients, because an effect in high-risk patients should have become evident much earlier because of the reduced survival generally seen in high-risk disease. This notion is also supported by the MRC IX trial, which indicates a tendency for improved survival in FISH-favorable patients after long follow-up. The conversion of survival curves after long-standing disease in the IFM trial does not support this explanation and may reflect a significant influence of salvage therapy in good-risk patients on OS.
In 2 trials exploring the role of thalidomide maintenance treatment after conventional therapy,17,25 approximately 50% of patients had already been exposed to thalidomide-containing induction regimens. In the Central European Myeloma Study Group (CEMSG) trial,25 patients were randomized to thalidomide plus interferon or to interferon maintenance therapy. The thalidomide-containing combination induced a significant increase in PFS (27.7 vs 13.2 months, P = .0068), but OS was similar between the 2 groups (52.6 vs 51.4 months, P = .81) and did not differ between patients 75 years of age or older and younger patients (P = .39). Survival after disease progression tended to be shorter in patients exposed to thalidomide-interferon maintenance therapy (P = .056). Patients receiving thalidomide-interferon had more PNP (69% vs 38%, P = .0015), constipation (44% vs 19%, P = .0004), skin toxicity (33% vs 11%, P = .0041), and elevated creatinine (13% vs 5%, P = .026). In the MRC myeloma IX study, PFS was significantly, but only moderately, increased with thalidomide maintenance (11 vs 9 months, P = .014), whereas for OS no difference (38 vs 39 months, P = .995) was noted.17 Survival after relapse was shorter in thalidomide-exposed patients, but the difference did not reach statistical significance (21 vs 26 months, P = .25). When novel drugs were selected for salvage therapy after relapse, survival was improved, a finding that was also noted in younger patients.17
Seven randomized trials have compared melphalan, prednisone, and thalidomide (MPT) with MP in elderly patients,26-33 and in 4 of them thalidomide was given after MPT as maintenance.26,30-32 There was significant heterogeneity in the design of these studies, with differences in the dose, schedule, and duration of MPT therapy (Table 2). A borderline significant improvement in OS with MPT followed by thalidomide maintenance therapy was noted in the HOVON trial28 (40 vs 31 months, P = .05), whereas in the 3 other studies with thalidomide maintenance therapy after MPT, no difference in OS (47.6 vs 45 months; P = .79,26 29 vs 32 months, P = .16,31 and 26 vs 28 months, P = .0655,32 respectively) was observed.
Trials comparing MPT plus thalidomide maintenance versus MP
| Study group . | Median age, y (no. of patients) . | Induction therapy . | Maintenance dose, duration of treatment . | Improvement in quality of response . | EFS or PFS* . | OS* . | Survival after relapse . | Thalidomide tolerance . |
|---|---|---|---|---|---|---|---|---|
| GIMEMA: Palumbo et al26 (2006) | 72 (N = 255) | (A) MPT thalidomide 100 mg/d 6 cycles | Thalidomide 100 mg/d until relapse | CR + PR: (A) 76.0% | 2-y EFS: (A) 54% | 3-y OS: (A) 80% | NA | Grades 3 or 4 AEs: (A) 48% |
| (B) 47.6% | (B) 25% P = .0002 | |||||||
| nCR/CR: | ||||||||
| (B) MP | (A) 27.9% | (B) 27% | (B) 64% | |||||
| 6 cycles | None | (B) 7.2% | P = .0006 | P = .19 | ||||
| GIMEMA: Palumbo et al27 (2008) | 72 (N = 331) | A) MPT 6 cycles | Thalidomide 100 mg/d until relapse | CR + VGPR: (A) 44.9% | PFS: (A) 21.8 mo | (A) 45 mo | (A) 11.5 mo | Grades 3 or 4: (A) 55% |
| (B) MP 6 cycles | None | (B) 14.7% | (B) 14.5 mo | (B) 47.6 mo | (B) 24.3 mo | (B) 22% | ||
| P < .001 | P = .001 | P = .79 | P = .01 | |||||
| HOVON: Wijermans et al30 (2010) | 72 (N = 333) | (A) MPT: thalidomide 50 mg/d 8 cycles | Thalidomide 50 mg/d until relapse | > PR: (A) 66% (B) 45% P < .001 | EFS: (A) 13 mo (B) 9 mo P < .001 | (A) 40 mo (B) 31 mo P = .05 | NA | Grade ≥ 2 toxicities: (A) 87% (B) 60% |
| (B) MP 8 cycles | ≥VGPR | PFS: | 2-y OS: | |||||
| None | (A) 27% (B) 10% P < .001 | (A) 33% (B) 21% P = .05 | 67 vs. 61% | |||||
| 4-y OS: 43% vs 30% | ||||||||
| 2 y-PFS: | ||||||||
| (A) 34% | ||||||||
| (B) 14% | ||||||||
| NMSG: Waage et al31 (2010) | 74.5 (N = 357) | (A) MPT: thalidomide up to 400 mg/d; cycles were given until plateau phase | Thalidomide 200 mg/d until relapse | ≥ PR: (A) 57% (B) 40% | PFS: (A) 15 mo (B) 14 mo P = .84† | (A) 29 mo (B) 32 mo P = .16 | NA | Grades 3 or 4 nonhematologic: (A) 40% (B) 19% |
| PNP: (A) 6% | ||||||||
| (B) MP: cycles were given until plateau phase | None | ≥ VGPR: (A) 23% | (B) 1% | |||||
| (B) 7% P < .0001 | TVT: (A) 8% | |||||||
| (B) 8% | ||||||||
| TMSG: Beksac et al32 (2011) | (N = 122) | (A) MPT: thalidomide 100 mg, 12 mo | Thalidomide 100 mg/d continuously | ≥ PR: (A) 57.9% (B) 37.5% P = .03 | DFS: (A) 21.0 mo (B) 14.0 mo P = .342 | (A) 26 mo (B) 28 mo P = .655 | Infections (grades 3 or 4): (A) 22.4% (B) 7% | |
| (B) MP, 12 mo | None |
| Study group . | Median age, y (no. of patients) . | Induction therapy . | Maintenance dose, duration of treatment . | Improvement in quality of response . | EFS or PFS* . | OS* . | Survival after relapse . | Thalidomide tolerance . |
|---|---|---|---|---|---|---|---|---|
| GIMEMA: Palumbo et al26 (2006) | 72 (N = 255) | (A) MPT thalidomide 100 mg/d 6 cycles | Thalidomide 100 mg/d until relapse | CR + PR: (A) 76.0% | 2-y EFS: (A) 54% | 3-y OS: (A) 80% | NA | Grades 3 or 4 AEs: (A) 48% |
| (B) 47.6% | (B) 25% P = .0002 | |||||||
| nCR/CR: | ||||||||
| (B) MP | (A) 27.9% | (B) 27% | (B) 64% | |||||
| 6 cycles | None | (B) 7.2% | P = .0006 | P = .19 | ||||
| GIMEMA: Palumbo et al27 (2008) | 72 (N = 331) | A) MPT 6 cycles | Thalidomide 100 mg/d until relapse | CR + VGPR: (A) 44.9% | PFS: (A) 21.8 mo | (A) 45 mo | (A) 11.5 mo | Grades 3 or 4: (A) 55% |
| (B) MP 6 cycles | None | (B) 14.7% | (B) 14.5 mo | (B) 47.6 mo | (B) 24.3 mo | (B) 22% | ||
| P < .001 | P = .001 | P = .79 | P = .01 | |||||
| HOVON: Wijermans et al30 (2010) | 72 (N = 333) | (A) MPT: thalidomide 50 mg/d 8 cycles | Thalidomide 50 mg/d until relapse | > PR: (A) 66% (B) 45% P < .001 | EFS: (A) 13 mo (B) 9 mo P < .001 | (A) 40 mo (B) 31 mo P = .05 | NA | Grade ≥ 2 toxicities: (A) 87% (B) 60% |
| (B) MP 8 cycles | ≥VGPR | PFS: | 2-y OS: | |||||
| None | (A) 27% (B) 10% P < .001 | (A) 33% (B) 21% P = .05 | 67 vs. 61% | |||||
| 4-y OS: 43% vs 30% | ||||||||
| 2 y-PFS: | ||||||||
| (A) 34% | ||||||||
| (B) 14% | ||||||||
| NMSG: Waage et al31 (2010) | 74.5 (N = 357) | (A) MPT: thalidomide up to 400 mg/d; cycles were given until plateau phase | Thalidomide 200 mg/d until relapse | ≥ PR: (A) 57% (B) 40% | PFS: (A) 15 mo (B) 14 mo P = .84† | (A) 29 mo (B) 32 mo P = .16 | NA | Grades 3 or 4 nonhematologic: (A) 40% (B) 19% |
| PNP: (A) 6% | ||||||||
| (B) MP: cycles were given until plateau phase | None | ≥ VGPR: (A) 23% | (B) 1% | |||||
| (B) 7% P < .0001 | TVT: (A) 8% | |||||||
| (B) 8% | ||||||||
| TMSG: Beksac et al32 (2011) | (N = 122) | (A) MPT: thalidomide 100 mg, 12 mo | Thalidomide 100 mg/d continuously | ≥ PR: (A) 57.9% (B) 37.5% P = .03 | DFS: (A) 21.0 mo (B) 14.0 mo P = .342 | (A) 26 mo (B) 28 mo P = .655 | Infections (grades 3 or 4): (A) 22.4% (B) 7% | |
| (B) MP, 12 mo | None |
NA indicates not available.
Data are median values unless otherwise stated.
P value from oral presentation; definite value not stated in final publication.
The optimal dose of thalidomide should be the minimal effective dose that is associated with superior tolerance and least toxicity. Since its introduction, the doses of thalidomide have continuously been decreased from the initial 400 mg/d18 to as little as 50 mg/d in the HOVON-50 study.30 As the results have been similar in most trials, a dose of 50 to 100 mg/d may be recommended as an appropriate dose.
The median duration of thalidomide treatment varied between 7 months in the MRC IX trial,17 13.2 months in the CEMSG study,25 15 months in the IFM trial,15 and almost 24 months in the HOVON study,30 which used the lowest dose of thalidomide and in which 47% of patients were still on therapy at that time. Recommending a specific length of thalidomide therapy is difficult, but in a multivariate analysis, no impact of treatment duration was noted.19 Limiting the duration of thalidomide exposure should reduce the risk of severe side effects, particularly PNP, the most relevant toxicity.15,16 Other side effects are constipation, fatigue, mood disturbances, and, particularly in elderly patients, arrhythmias, bradycardia, and thromboembolic complications.
Lenalidomide
Lenalidomide is an attractive drug for maintenance therapy with the advantage of oral administration. It was found to be particularly active in patients with high IRF4 expression34 and with higher cereblon expression.35 Dexamethasone enhances the antimyeloma effect of lenalidomide but antagonizes the immunostimulatory effects in a dose-dependent manner.36 Hence, single-agent lenalidomide seems to be the logical choice for maintenance treatment when tumor load has already been reduced significantly and control of the residual tumor cells by active immune surveillance is the clinically relevant priority. A pilot phase 2 study showing the feasibility and efficacy of lenalidomide consolidation and maintenance therapy laid the basis for further clinical testing.37
The Cancer and Leukemia Group B (CALGB) 100104 study randomized 460 patients after ASCT to lenalidomide maintenance therapy or to placebo.38 The induction regimen before ASCT was not specified, and patients were stratified according to previous thalidomide or lenalidomide exposure during induction therapy and to β2-microglobulin levels. After a median follow-up of 28 months from ASCT, median time to progression was 48 months in the lenalidomide maintenance and 30.9 months in the placebo group (HR = 0.39, 95% CI, 0.27-0.56, P < .0001; Table 3). Lenalidomide maintenance treatment was equally effective in patients with high or low β2-microglobulin levels and in those previously exposed to thalidomide or lenalidomide therapy. OS was significantly increased with lenalidomide maintenance therapy despite a crossover to lenalidomide by some of the placebo patients after unblinding of the study in January 2010. Twenty-three deaths were observed in the treatment and 39 in the control arm (P = .018). Patients receiving lenalidomide maintenance therapy had significantly more episodes of neutropenia (P < .0001), anemia (P = .0639), and thrombocytopenia (P = .035), significantly more grade 3 to 5 nonhematologic adverse events (AEs, P = .0048), including more infections (P < .0001), but there was no difference in the frequency of fatigue, neuropathy, rash, and thromboembolism. Twelve percent of patients on lenalidomide and 1% on placebo came off therapy because of AEs, and 20% of patients on lenalidomide and 7% on placebo came off therapy for other reasons. At the time of reporting (IMW, May 2011), 29 second malignancies (7 before randomization, 18 in the lenalidomide maintenance, and 4 in the control group) had been observed. An EFS analysis, with events defined as progression, second cancers, and deaths, demonstrated a median EFS of 42 months in the lenalidomide arm and 22 months in the placebo arm.
Maintenance studies with lenalidomide in patients after ASCT and after conventional chemotherapy
| Study group . | Median age, y (no. of patients) . | Induction consolidation therapy . | Maintenance dose, duration of treatment . | Improvement in quality of response . | TTP or PFS* . | OS* . | Survival after relapse . | Lenalidomide tolerance . |
|---|---|---|---|---|---|---|---|---|
| CALGB: McCarthy et al38 (2011) | NA (N = 460) | Any, followed by ASCT (M 200) | (A) 10 mg/d with dose adaptations (5-15 mg/d) continuously† | NA | (A) TTP, median 42 mo | No. of deaths: (A) 23 | NA; 78% of eligible patients of the control group had been crossed over to lenalidomide treatment | Discontinuation because of AEs (A) 12% (B) 2% Because of other reasons: (A) 13% (B) 6% SPM: (A) 15, (B) 6 |
| (B) Placebo | (B) 22 mo P < .0001 | (B) 39 P = .018 | ||||||
| IFM: Attal et al39,40 (2010) | 55 (N = 614) | VAD, Vel-dexamethasone and other induction therapy, single or double ASCT | (A) 10-15 mg/d continuously†‡ | (A) CR: 25% VGPR: 76% | (A) 42 mo | 5 y: (A) 79% | (A) 12 mo | Discontinuation because of AEs A) 21% SPM: 26 |
| Consolidation: lenalidomide 25 mg/d, days 1-21, every 28 d, 2 cycles | (B) Placebo | (B) CR: 23% VGPR: 71% | (B) 24 mo P < .0000001 | (B) 73% | (B) 12 mo | (B) 15% SPM: 6 | ||
| P = .49 P = .13 | ||||||||
| MM015: Palumbo et al42,43 (2010) | 71 (N = 459) | (A) MPR-R | (A) 10 mg/d, days 1-21, continuously† | (A) 77% P < .001 | (A) 31 mo | 4-y estimate (A-C) 58%-59% | NA | Discontinuation because of AEs (A) 20% SPM: 8% |
| (B) MPR | (B) Placebo | (B) 68% | (B) 14 mo | (B) 16% SPM: 6.6% | ||||
| (C) MP | (C) Placebo | (C) 50% | (C) 13 mo A vs C, P < .001 | (C) 2.9% SPM: 2.6% |
| Study group . | Median age, y (no. of patients) . | Induction consolidation therapy . | Maintenance dose, duration of treatment . | Improvement in quality of response . | TTP or PFS* . | OS* . | Survival after relapse . | Lenalidomide tolerance . |
|---|---|---|---|---|---|---|---|---|
| CALGB: McCarthy et al38 (2011) | NA (N = 460) | Any, followed by ASCT (M 200) | (A) 10 mg/d with dose adaptations (5-15 mg/d) continuously† | NA | (A) TTP, median 42 mo | No. of deaths: (A) 23 | NA; 78% of eligible patients of the control group had been crossed over to lenalidomide treatment | Discontinuation because of AEs (A) 12% (B) 2% Because of other reasons: (A) 13% (B) 6% SPM: (A) 15, (B) 6 |
| (B) Placebo | (B) 22 mo P < .0001 | (B) 39 P = .018 | ||||||
| IFM: Attal et al39,40 (2010) | 55 (N = 614) | VAD, Vel-dexamethasone and other induction therapy, single or double ASCT | (A) 10-15 mg/d continuously†‡ | (A) CR: 25% VGPR: 76% | (A) 42 mo | 5 y: (A) 79% | (A) 12 mo | Discontinuation because of AEs A) 21% SPM: 26 |
| Consolidation: lenalidomide 25 mg/d, days 1-21, every 28 d, 2 cycles | (B) Placebo | (B) CR: 23% VGPR: 71% | (B) 24 mo P < .0000001 | (B) 73% | (B) 12 mo | (B) 15% SPM: 6 | ||
| P = .49 P = .13 | ||||||||
| MM015: Palumbo et al42,43 (2010) | 71 (N = 459) | (A) MPR-R | (A) 10 mg/d, days 1-21, continuously† | (A) 77% P < .001 | (A) 31 mo | 4-y estimate (A-C) 58%-59% | NA | Discontinuation because of AEs (A) 20% SPM: 8% |
| (B) MPR | (B) Placebo | (B) 68% | (B) 14 mo | (B) 16% SPM: 6.6% | ||||
| (C) MP | (C) Placebo | (C) 50% | (C) 13 mo A vs C, P < .001 | (C) 2.9% SPM: 2.6% |
TTP indicates time to progression.
Data are median values unless otherwise stated.
Until PD or intolerance.
Patients on placebo were not allowed to cross over to lenalidomide after PD.
In the IFM-2005-02 lenalidomide maintenance trial, 614 patients who had single or double ASCT were treated with 2 cycles of lenalidomide consolidation therapy and were thereafter randomized to lenalidomide maintenance therapy or placebo.39 After a median follow-up of 24 months after randomization to maintenance, an independent data monitoring committee recommended stopping and unblinding the trial because of a dramatically improved PFS in the lenalidomide maintenance arm. Consolidation therapy with lenalidomide resulted in an upgrading of the quality of response, with CR increasing from 14% to 20% (P < .001) and more than or equal to VGPR from 58% to 67% (P < .001), respectively. Improved response correlated with longer PFS. Best response during maintenance therapy was slightly, but not significantly, higher in patients maintained with lenalidomide (CR rate, 25% vs 22%, P = .4; VGPR rate, 77% vs 70%, P = .08). With a median follow-up of 36 months after randomization (46 months from diagnosis), median PFS was significantly longer in patients randomized to lenalidomide maintenance therapy (41 vs 24 months, HR = 0.5, P < .0000001); the benefit in terms of longer PFS was noted independently of the quality of response at randomization, type of induction regimen, and β2-microglobulin. PFS and OS were shorter in patients with FISH-defined unfavorable cytogenetics compared with the standard-risk group. For patients progressing on placebo, crossover to lenalidomide maintenance treatment was not allowed: OS at 5 years after diagnosis was similar in the lenalidomide and control groups (79% vs 73%, P = .8).40 The median interval between time of progression and death was relatively short (11 vs 13 months). Patients on lenalidomide maintenance therapy had an increased incidence of secondary malignancies (26 vs 6 cases). Common toxicities were relatively low, with 21% of patients on lenalidomide and 15% on placebo discontinuing therapy because of toxicity.
The results of the lenalidomide maintenance studies require longer follow-up to confirm whether the positive finding in the CALGB study will prove robust and whether similar improvements will be seen in the IFM study, which differed with respect to the patient population and treatment. If good-risk patients benefit more from lenalidomide maintenance, survival curves should start to diverge after prolonged follow-up.
In any event, a time span without progression of disease is usually associated with better quality of life and, hence, is of substantial benefit to the patient. Lenalidomide maintenance therapy was well tolerated with almost negligible hematotoxicity, no neurotoxicity, and no increase in thromboembolic complications or infections. The observation of an increased occurrence of second primary malignancies (SPMs), however, is notable. The incidence of SPM was slightly higher in the IFM trial, where a proportion of patients had been exposed to induction therapy incorporating dexamethasone, cyclophosphamide, etoposide, and cisplatin, which contains drugs of known leukemogenic potential. Further studies are needed to evaluate the true risk of this complication, to identify risk factors for its development, and hopefully, to develop strategies for the prevention of SPMs. Before more information is available, a firm recommendation cannot be made. Physicians and patients must weigh the benefits of lenalidomide maintenance therapy against the low but relevant risk of SPM.
In elderly patients, a phase 2 trial with melphalan, prednisone, and lenalidomide (MPR) was the forerunner for the MM-015 trial.41 The MM-015 3-arm trial randomized elderly patients to 9 cycles of MPR followed by lenalidomide maintenance treatment (MPR-R) until PD or intolerance, or to 9 cycles of MPR, or MP without maintenance therapy.42 The MPR regimen resulted in significantly higher response rates (MPR-R, 77%; MPR, 68%; MP, 50%; P < .001) with approximately 3 times as many CRs in the maintenance arm compared with MP only (MPR-R, 16%; MPR, 10%; MP, 4%; P < .001; Table 3). Sixty percent of responses were achieved within 3 months after induction treatment initiation, but improvements in the quality of response occurred with continued treatment, particularly during the first year, with few patients achieving further tumor reduction thereafter. After a median follow-up of 27 months, PFS was significantly longer with lenalidomide maintenance treatment (31 vs 14 vs 13 months for MPR-R, MPR, and MP, respectively; MPR-R vs MP, HR = 0.395, P < .001).43 A landmark analysis conducted from the beginning of cycle 10 demonstrated the significant impact of maintenance therapy regarding PFS for the MPR-R compared with the MPR arm (HR = 0.34, P < .001). In addition, a subgroup landmark analysis showed that the significant benefit of MPR-R over MPR was maintained regardless of International Staging System stage (I and II vs III), response (≥ VGPR vs PR), and age (65-75 years vs > 75 years). With a median follow-up of 41 months for OS, the OS rate at 4 years was similar between the 3 groups (58%-59%). Grade 3 and 4 neutropenia and thrombocytopenia were significantly more frequent in the MPR arm, and prophylactic G-CSF was administered to 49% of patients in the MPR-R group compared with 29% of patients in the MP arm; platelet transfusions were administered to 6% and 5% of patients, respectively.42 Overall, 20% of patients in the MPR-R, 16% in the MPR, and 8% in the MP group discontinued therapy because of AEs. Notably, the rate of discontinuation was higher in patients older than 75 years than in those 65 to 75 years old (22% vs 12%, respectively), indicating that treatment tolerance is reduced in the very elderly population. A subsequent analysis revealed an increased rate of secondary malignancies in the MPR-R and MPR compared with the MP group (12 [8.0%], 10 [6.6%], and 4 [2.6%] patients, respectively).
Our meta-analysis of the published results of the 3 lenalidomide maintenance studies, which included a total of 1380 patients, revealed a 65% risk reduction for progression for patients on lenalidomide maintenance therapy (Figure 1C; HR = 0.45, 95% CI, 0.37-0.54, P < .00001). The significant increase in PFS with a reduction of the relative risk of relapse by 65% as a result of lenalidomide maintenance is unprecedented. Lenalidomide maintenance therapy is effective both in patients subjected to high-dose therapy with ASCT38,39 and in those treated with conventional therapy42 but is unable to overcome the adverse prognosis of FISH defined high-risk cytogenetics.39
Meta-analysis of maintenance studies. (A) PFS with thalidomide or thalidomide combinations in young and older patients. (B) OS with thalidomide or thalidomide combinations in young and older patients. (C) PFS with lenalidomide maintenance therapy in young and older patients.
Meta-analysis of maintenance studies. (A) PFS with thalidomide or thalidomide combinations in young and older patients. (B) OS with thalidomide or thalidomide combinations in young and older patients. (C) PFS with lenalidomide maintenance therapy in young and older patients.
Bortezomib
Two studies used bortezomib in combination with thalidomide for maintenance treatment either compared with control or with bortezomib plus prednisone maintenance therapy.44,45 The Spanish Programa Espaniol de Tratamientos en Hematologica (PETHEMA) trial randomized 260 patients 65 years of age or older to either bortezomib, melphalan, and prednisone (VMP) or bortezomib, thalidomide, and prednisone (VTP) for induction treatment44 (Table 4). The induction therapy consisted of one 6-week cycle with biweekly bortezomib followed by five 5-week cycles with weekly bortezomib to reduce toxic side effects. After induction, 178 patients were randomized to either bortezomib and thalidomide (VT) or VP maintenance therapy. Bortezomib maintenance was administered every 3 months using the conventional day 1, 4, 8, and 11 schedule. The VT group received thalidomide at a dose of 50 mg/day, and the VP cohort received prednisone at a dose of 50 mg/m2 every other day. Both treatments were given for up to 3 years. VT and VP maintenance treatment improved the quality of response with the CR (immunofixation negative) rate rising from 24% to 46% in patients on the former and to 39% in patients on the latter therapy. After a median follow-up of 46 months from first randomization, PFS was 39 months for patients receiving VT and 32 months for those treated with VP (P = .1). The nonsignificant benefit of VT maintenance therapy was independent of the type of induction therapy. OS did not differ between the 2 groups (not reached vs 60 months, P = .1, for VT vs VP, respectively). During maintenance treatment, grade 3 or 4 neutropenia was seen in 1% of patients receiving VT. No further grade 3 or higher hematologic toxicities were noted in either arm. Grade 3 or 4 PN was seen in 3% of patients in the VP and 9% in the VT group.
Maintenance and consolidation studies with bortezomib in combination with thalidomide or prednisone
| Study group . | Median age, y (no. of patients) . | Induction therapy . | Maintenance dose, duration of treatment . | Improvement in quality of response . | EFS or PFS* . | OS* . | Tolerance . |
|---|---|---|---|---|---|---|---|
| PETHEMA: Mateos et al44 (2011) | 73 (N = 260) | VMP vs VTP | (A) VT: bortezomib 1.3 mg/m2, days 1, 4, 8, and 11 every 12 wks for 3 y; thalidomide 50 mg/d for 3 y | CR IF (A) 24%-46% | PFS (A) 39 mo | (A) not reached | G3 and G4 PNP (A) 9% (B) 3% |
| (B) VP: bortezomib 1.3 mg/m2, days 1, 4, 8, and 11 every 12 wks for 3 y; prednisone 50 mg every 2 d for 3 y | (B) 24%-39% | (B) 32 mo P = .1 | (B) 60 mo P = .1 | Discontinuation because of AEs (A) 13% (B) 9% | |||
| GIMEMA: Palumbo et al45 (2010) | 71 (N = 511) | VMPT-VT | Bortezomib 1.3 mg/m2, days 1 and 15, every 4 wks; thalidomide 50 mg/d until PD or intolerance | CR (A) 38% | 3-y PFS (A) 60% | 3-y OS (A) 88.8% | G3 and G4 Neutropenia (A) 38% (B) 28.1% |
| Cardiologic | |||||||
| VMP | (B) 24% | (B) 42% | (B) 89.2% | (A) 10.4% | |||
| P = .0008 | P < .07 | P = .9 | (B) 5.5% | ||||
| HOVON/GMMG: Sonneveld et al46 (2010) | 57 (N = 613) | PAD | Bortezomib 1.3 mg/m2, biweekly, for 2 y; thalidomide 50 mg/d for 2 y | (A) CR/nCR 50% | 3-y PFS | 3-y OS | G3 and G4 PNP |
| ≥ VGPR 65% | (A) 48% | (A) 78% | (A) 16% | ||||
| VAD | (B) CR/nCR 38% | (B) 42% | (B) 71% | (B) 7% | |||
| ≥ VGPR 61% | P = .047 | P = .048 |
| Study group . | Median age, y (no. of patients) . | Induction therapy . | Maintenance dose, duration of treatment . | Improvement in quality of response . | EFS or PFS* . | OS* . | Tolerance . |
|---|---|---|---|---|---|---|---|
| PETHEMA: Mateos et al44 (2011) | 73 (N = 260) | VMP vs VTP | (A) VT: bortezomib 1.3 mg/m2, days 1, 4, 8, and 11 every 12 wks for 3 y; thalidomide 50 mg/d for 3 y | CR IF (A) 24%-46% | PFS (A) 39 mo | (A) not reached | G3 and G4 PNP (A) 9% (B) 3% |
| (B) VP: bortezomib 1.3 mg/m2, days 1, 4, 8, and 11 every 12 wks for 3 y; prednisone 50 mg every 2 d for 3 y | (B) 24%-39% | (B) 32 mo P = .1 | (B) 60 mo P = .1 | Discontinuation because of AEs (A) 13% (B) 9% | |||
| GIMEMA: Palumbo et al45 (2010) | 71 (N = 511) | VMPT-VT | Bortezomib 1.3 mg/m2, days 1 and 15, every 4 wks; thalidomide 50 mg/d until PD or intolerance | CR (A) 38% | 3-y PFS (A) 60% | 3-y OS (A) 88.8% | G3 and G4 Neutropenia (A) 38% (B) 28.1% |
| Cardiologic | |||||||
| VMP | (B) 24% | (B) 42% | (B) 89.2% | (A) 10.4% | |||
| P = .0008 | P < .07 | P = .9 | (B) 5.5% | ||||
| HOVON/GMMG: Sonneveld et al46 (2010) | 57 (N = 613) | PAD | Bortezomib 1.3 mg/m2, biweekly, for 2 y; thalidomide 50 mg/d for 2 y | (A) CR/nCR 50% | 3-y PFS | 3-y OS | G3 and G4 PNP |
| ≥ VGPR 65% | (A) 48% | (A) 78% | (A) 16% | ||||
| VAD | (B) CR/nCR 38% | (B) 42% | (B) 71% | (B) 7% | |||
| ≥ VGPR 61% | P = .047 | P = .048 |
Data are median values unless otherwise stated.
A Gruppo Italiano Malattie Ematologiche dell'Adulto (GIMEMA)45 study randomized 511 patients to either nine 6-week cycles of VMPT induction therapy followed by VT maintenance or to nine 6-week cycles of VMP induction treatment. After inclusion of 139 patients, the biweekly administration of bortezomib was reduced to a once-weekly schedule to enhance the tolerance of bortezomib, and both the VMPT and the VMP schedules were changed to nine 5-week cycles. Patients on VMPT followed by VT maintenance achieved a higher rate of CR and more than or equal to VGPR (38% vs 24%, P < .001, and 59% vs 50%, P = .03, respectively) and had both a significantly higher rate of PFS at 3 years (56% vs 41%, P = .008) and a longer time to next treatment (72% vs 60%, P = .007). The OS rate at 3 years was similar in both groups (89% vs 87%, P = .77). Patients in the VMPT arm experienced more grade 3 and 4 neutropenia (38% vs 28%, P = .02), thromboembolic events (5% vs 2%, P = .08), and cardiologic side effects (10% vs 5%, P = .04). However, the evaluation of the benefit of maintenance treatment in this trial is difficult because different induction treatments had been used in the 2 arms.
Combining 2 drugs with significant neurotoxic potential poses the risk of substantial toxicity, but contrary to such concerns, clinical experience shows an acceptable tolerance if a “low-dose intensity” concept is used. Thalidomide was administered at a daily dose of 50 mg continuously, and the dose intensity for bortezomib was 6 doses over 3 months in the Italian study and 4 doses over the same period in the Spanish study. VT maintenance treatment resulted in a low rate of grade 1 or 2 neurotoxicity and a low discontinuation rate, as well as a tendency for increased PFS compared with bortezomib plus prednisone in the PETHEMA study.44 In the GIMEMA trial,45 a tendency for an increase in PFS (P = .07) compared with control was observed. OS did not differ between VT and VP maintenance therapy in the Spanish study, and in the Italian trial, no difference in the survival rates at 3 years were noted between patients receiving VT maintenance therapy or those randomized to the control arm (88.1% vs 89.2%, P = .9).
The joint HOVON/GMMG trial randomized 613 patients to bortezomib-doxorubicin-dexamethasone (PAD) or VAD induction therapy followed by single or double ASCT.46 Patients started on PAD received bortezomib maintenance (1.3 mg/m2, biweekly for 2 years), and those randomized to VAD were treated with thalidomide maintenance therapy (50 mg, daily for 2 years). After a median follow-up of 40 months, the near CR/CR rate was 38% in the VAD/ASCT/thalidomide arm and 50% in the PAD/ASCT/bortezomib arm; the respective rates for more than or equal to VGPR were 61% and 75%. PFS and OS were significantly longer in the PAD/ASCT/bortezomib-treated patients (HR = 0.81, P = .047, and HR = 0.74, P = .048, respectively), with PFS and OS rates at 36 months of 48% and 78% in the PAD/ASCT bortezomib group and 42% and 71% in the VAD/ASCT/thalidomide group, respectively. A total of 67% of patients in the VAD/ASCT/thalidomide arm and 57% in the PAD/ASCT/bortezomib arm started maintenance therapy; 64% of those on thalidomide maintenance discontinued maintenance therapy because of PD (31%), toxicity (31%), and other reasons (2%). In the bortezomib arm, 47% discontinued maintenance because of PD (29%), toxicity (9%), or other reasons (9%) and 27% required dose reductions. In essence, the PAD/ASCT/bortezomib protocol was in all study objectives superior to the VAD/ASCT/thalidomide regimen, including patients with renal impairment47 and with adverse FISH-determined cytogenetics t(4,14) amplification of 1q21, and del 17p).48 The study showed that bortezomib maintenance therapy can be tolerated for up to 2 years, but the design of the study does not allow a clear dissection of the role of bortezomib maintenance therapy.
As several questions regarding the optimal use of bortezomib (in particular, scheduling, dosing, duration of therapy, and combination with other drugs) remain unresolved, specific recommendations cannot be made for bortezomib maintenance therapy at this time.
Considerations for clinical practice
Presently, in most countries, none of the novel drugs evaluated for maintenance therapy is approved for this indication. Nevertheless, patients will find access to the available information and will query their treating physicians about possible treatment options after induction therapy besides a wait-and-see strategy, which remains a valuable alternative. Based on present scientific evidence (Table 5), thalidomide maintenance treatment after ASCT is a possible option that increases PFS and, albeit to a lesser degree, OS. Thalidomide maintenance should not be offered to patients with FISH-defined poor-risk cytogenetics because those patients had inferior outcome with thalidomide maintenance therapy compared with controls. The lowest dose shown to be active is 50 mg daily, and the duration of therapy should potentially be limited to one year or less to limit the risk of significant toxicity. For elderly patients, the situation is less clear. In both studies conducted so far, approximately half of the patients had already been exposed to thalidomide during induction therapy. Results showed a significant increase in PFS, but not in OS. Thalidomide maintenance therapy in elderly patients with favorable cytogenetics is therefore also a valuable option, but thalidomide tolerance decreases with increasing age. Results of some studies suggest that thalidomide maintenance should preferentially be considered in patients who have not been exposed to thalidomide during induction therapy, but this observation was not confirmed in the MRC trial.17
Summary of benefits and limitations of maintenance therapy with novel drugs for clinical decision making
| Drug . | Dose/regimen . | Duration of therapy . | Impact on . | Risk groups . | Tolerance . | Level of evidence/rade of recommendation . | Comments . | ||
|---|---|---|---|---|---|---|---|---|---|
| Quality of response . | PFS . | OS . | |||||||
| Thalidomide | 50* (100) mg/d | Up to 1 y,† no correlation between duration and outcome‡ | Yes | Yes | Yes, preferentially if not part of the induction regimen; yes, in meta-analysis | No benefit In FISH defined high-risk patients§ Possible benefit in patients with abnormal metaphase cytogenetics and GEP-defined high risk | PNP, fatigue and other limiting dose and duration of therapy | I/A | Poor tolerance in some (particularly elderly) patients; not recommended for patients with FISH defined high-risk profile |
| Lenalidomide | 10‖ (5-15) mg/d continuously or days 1-21, every 28 d | Until PD or intolerance | Yes | Yes | Presently shown in one-third of studies | Does not overcome negative impact of FISH-defined unfavorable cytogenetics | Few discontinuations because of AEs | I/A | Unprecedented extension of PFS, increase in OS in 1 of 3 studies; usually well tolerated, increased risk for secondary primary malignancies |
| Bortezomib‖ | 1.3 mg biweekly | 2 y or until PD or intolerance | Yes¶ | Yes¶ | Yes¶ | Active in patients with renal failure and cytogenetic risk groups | PNP grades 3 or 4: 16% (based on intravenous administration) | Not applicable | Only comparison between PAD-ASCT bortezomib with VAD-ASCT thalidomide available |
| Bortezomib-thalidomide | GIMEMA: bortezomib-thalidomide yielded increased PFS vs control. PETHEMA: bortezomib-thalidomide resulted in a tendency for increased PFS vs VP. In both studies, an impact on OS was not observed. Results of ongoing trials need to be awaited. | ||||||||
| Drug . | Dose/regimen . | Duration of therapy . | Impact on . | Risk groups . | Tolerance . | Level of evidence/rade of recommendation . | Comments . | ||
|---|---|---|---|---|---|---|---|---|---|
| Quality of response . | PFS . | OS . | |||||||
| Thalidomide | 50* (100) mg/d | Up to 1 y,† no correlation between duration and outcome‡ | Yes | Yes | Yes, preferentially if not part of the induction regimen; yes, in meta-analysis | No benefit In FISH defined high-risk patients§ Possible benefit in patients with abnormal metaphase cytogenetics and GEP-defined high risk | PNP, fatigue and other limiting dose and duration of therapy | I/A | Poor tolerance in some (particularly elderly) patients; not recommended for patients with FISH defined high-risk profile |
| Lenalidomide | 10‖ (5-15) mg/d continuously or days 1-21, every 28 d | Until PD or intolerance | Yes | Yes | Presently shown in one-third of studies | Does not overcome negative impact of FISH-defined unfavorable cytogenetics | Few discontinuations because of AEs | I/A | Unprecedented extension of PFS, increase in OS in 1 of 3 studies; usually well tolerated, increased risk for secondary primary malignancies |
| Bortezomib‖ | 1.3 mg biweekly | 2 y or until PD or intolerance | Yes¶ | Yes¶ | Yes¶ | Active in patients with renal failure and cytogenetic risk groups | PNP grades 3 or 4: 16% (based on intravenous administration) | Not applicable | Only comparison between PAD-ASCT bortezomib with VAD-ASCT thalidomide available |
| Bortezomib-thalidomide | GIMEMA: bortezomib-thalidomide yielded increased PFS vs control. PETHEMA: bortezomib-thalidomide resulted in a tendency for increased PFS vs VP. In both studies, an impact on OS was not observed. Results of ongoing trials need to be awaited. | ||||||||
Lowest dose shown to be effective and therefore recommended; several studies used 100 mg or higher doses.
Spencer et al limited thalidomide therapy to 12 months.16
Barlogie et al.19
Morgan et al showed shortened survival in unfavorable FISH patients.17
Recommended starting dose; doses have been adapted to 5-15 mg in the CALGB study.
Different regimens during induction therapy limit comparability with the thalidomide maintenance arm.
Lenalidomide after ASCT is associated with a significantly increased PFS,38,39 and in one study38 with a significant survival benefit. It is well tolerated and active in most risk groups, with the exception of FISH-defined high-risk patients.39 The starting dose should be 10 mg daily, with dose modification of 5 to 15 mg being feasible. Both continuous treatment as well as a 3 weeks on/one week off regimen have been shown to be effective. So far, treatment has been continued until PD or untoward toxicity. It is not clear whether shorter therapy would render similar effects. In elderly patients, only one prospective randomized trial has been presented as yet. Results are essentially identical to those obtained in younger patients; thus, the same recommendations apply to elderly and younger patients. Recent updates of all 3 studies indicate that exposure to lenalidomide confers an increased risk for secondary malignancies. Whether lenalidomide maintenance therapy should be routinely offered to patients is controversial among experts. Some consider the marked gain in PFS and the survival advantage observed in one of the 2 studies in younger patients as a strong argument for therapy, whereas others weigh the increased incidence of SPMs as an important risk and so prefer to wait for more mature survival data before making specific recommendations.
Data on single-agent bortezomib maintenance treatment are available only in patients who had already been exposed to bortezomib during induction therapy.46 Bi-weekly bortezomib maintenance therapy is feasible and can be tolerated for up to 2 years, but dose reductions may be necessary in up to one-third of patients. Although a significant benefit of bortezomib maintenance therapy is likely, the design of the study allows only the conclusion that a bortezomib-based induction regimen followed by ASCT and bortezomib maintenance is superior to VAD induction followed by ASCT and thalidomide maintenance therapy. Bortezomib maintenance in combination with thalidomide has been shown to yield superior PFS compared with control45 or (although not statistically significant) compared with bortezomib plus prednisone in elderly patients.44 Further studies, particularly in patients not previously exposed to these drugs during induction phase, are warranted.
The online version of this article contains a data supplement.
Acknowledgments
The authors thank the members of the International Myeloma Foundation who reviewed the manuscript and provided comments.
The experts' meetings on maintenance therapy were supported by the International Myeloma Foundation. This study was supported in part by the Austrian Forum against Cancer.
Authorship
Contribution: H. Ludwig designed the outline and prepared the first draft of the manuscript; B.G.M.D. organized and chaired 2 experts' meetings on maintenance therapy during IFM summits; A.H. conducted the meta-analysis; and all authors participated significantly in the development of the manuscript, provided critical review and edits, and gave final approval of the manuscript.
Conflict-of-interest disclosure: K.C.A. received honoraria from ONYX, Millennium, Celgene, Novartis, BMS, and Merck and was the cofounder for Acetylon. B.B. received honoraria from Celgene, IMF, MMRF, Millennium, and Genzyme and research funding from Celgene, Novartis, NCI, Millennium, Johnson & Johnson, Centocor, Onyx, and Icon. M.B. received honoraria from Celgene and Janssen-Cilag. P.L.B. received honoraria from Celgene. M.C. received honoraria from Celgene and Janssen-Cilag. B.G.M.D. received honoraria from Celgene and Millennium. H.E. received honoraria from Celgene and Janssen-Cilag. T.F. received honoraria from Celgene, Merck, Onyx, BMS, and Janssen-Cilag. H. Lokhorst received honoraria from Celgene. H. Ludwig received honoraria from Celgene, Janssen-Cilag, and Mundipharma and research funding from Celgene, Janssen-Cilag, and Mundipharma. M.-V.M. received honoraria from Janssen-Cilag, Celgene, and Millennium. P.M. received honoraria from Celgene and Onyx. R.N. received honoraria from Celgene and Millennium and research funding from Celgene, Onyx, and Millennium. A.P. received honoraria from Celgene, Janssen-Cilag, Merck, and AMGEN. P.G.R. received honoraria from Celgene, Millennium, and Johnson & Johnson. J.S.M. received honoraria from Celgene, Millennium, and Janssen-Cilag. K.A.S. received honoraria from Celgene, Millennium, and ONYX and research funding from Millenium. A.W. received honoraria from Janssen-Cilag, Celgene, and Mundipharma. The remaining authors declare no competing financial interests.
Correspondence: Heinz Ludwig, Department of Medicine I, Center for Oncology and Hematology, Wilhelminenspital, Montleartstrasse 37, 1160 Vienna, Austria; e-mail: heinz.ludwig@wienkav.at.