Abstract
Abstract 2849
We have previously reported on the natural history of polycythemia vera (PV), focusing primarily on overall and leukemia-free survival (ASH Annual Meeting Abstracts. 2011;118(21):277-). In the current study, we present, on behalf of the International Working Group for Myeloproliferative neoplasms Resarch and Treatment (IWG-MRT), our analysis regarding risk factors for thrombosis.
Under the auspices of IWG-MRT, seven international centers of excellence for myeloproliferative neoplasms participated in the current study. The two principle investigators (AT and TB) reviewed all the cases and selected 1,545 patients who met the 2008 WHO criteria for PV, were age 18 years or older, diagnosed after 1970, and whose submitted data included diagnostically essential information.
Median age was 61 years (range, 18–95; 51% females). Arterial and venous thrombosis history before or at diagnosis was documented in 246 (16%) patients and 114 (7.4%) patients, respectively. Major hemorrhage hemorrhage before or at diagnosis was documented in 17 (4.5%) patients. Other features at diagnosis included pruritus (36%), microvascular disturbances (28.5%), palpable splenomegaly (36%), abnormal karyotype (12%), leukoerythroblastosis (6%), increased LDH (50%), thrombocytosis (53%), extreme thrombocytosis (platelets >1 million mm3; 4%) leukocytosis (49%), JAK2 V617F (95%), other JAK2 mutations (3%), subnormal serum erythropoietin (Epo) level (81%), and endogenous erythroid colonies (EEC; 73%). History of hypertension (46%), hyperlipidemia (18.3%), diabetes (8.4%), and tobacco use (16%) was also obtained.
To date, 347 (23%) deaths, 50 (3%) leukemic progressions, and 138 (9%) fibrotic transformations have been recorded. Overall, cytoreductive treatment was not used in 416 (27%) patients and the remaining were exposed to different agents based on physician discretion. Post-diagnosis arterial or venous thrombosis occurred in 184 (12%) and 137 (9%) patients, respectively.
Arterial and venous thrombosis-free survival, from time of diagnosis, were separately analyzed using the occurrence of thrombosis as the endpoint (uncensored variable) and last follow-up or death before thrombosis as the censored variable. In univariate analysis, the following were significantly associated with post-diagnosis arterial thrombosis: advanced age, leukocyte count, presence of a leukoerythroblastic smear (LES), history of hypertension and history of arterial thrombosis before or at diagnosis; multivariable analysis using all these five parameters identified arterial thrombosis history (RR 2.5, 95% CI 1.6–4.0; p<0.0001), LES (RR 2.3, 95% CI 1.3–4.2; p=0.005) and history of hypertension (RR 1.6, 95% CI 1.1–2.4; p=0.02) as independent predictors of post-diagnosis arterial thrombosis. Only two parameters predicted post-diagnosis venous thrombosis, in univariate analysis, and both remained significant during multivariable analysis: abnormal karyotype (RR 3.1, 95% CI 1.7–5.4; p=0.0001) and history of venous thrombosis (RR 2.4, 95% CI 1.2–4.9). Of note, the type of JAK2 mutation or presence of either subnormal Epo or EEC did not influence either arterial or venous thrombosis.
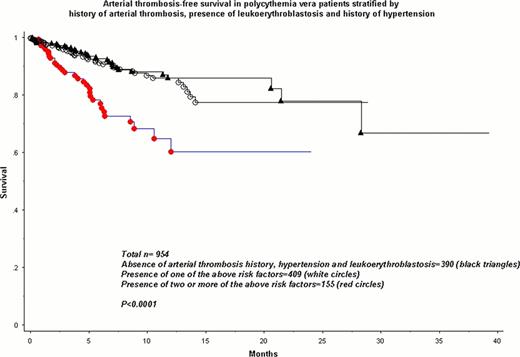
The figures below illustrated arterial or venous thrombosis-free survival of patients stratified by the absence of all risk factors or presence of one or ≥2 risk factors. For arterial thrombosis, the presence of ≥2 risk factors clearly delineated a high risk group (RR 3.1, 95% CI 1.9–5.0) whereas the presence of one (RR 2.4, 95% CI 1.4–4.2) or two risk factors (RR 10.1, 95% CI 3.6–28.2) for venous thrombosis delineated an intermediate and high risk group, respectively.
History of arterial thrombosis and venous thrombosis are key risk factors, respectively, for recurrent arterial and venous thrombosis in PV. In addition, abnormal karyotype is a strong independent risk factor for venous thrombosis and the presence of leukoerythroblastosis and hypertension, for arterial thrombosis. This information allows for a simple and practical risk stratification and raises interesting pathogenetic implications that require further clarification.
Vannucchi:Novartis: Membership on an entity's Board of Directors or advisory committees. Gisslinger:Novartis: Consultancy, Research Funding, Speakers Bureau; Celgene: Consultancy, Research Funding, Speakers Bureau. Passamonti:Novartis: Honoraria, Membership on an entity's Board of Directors or advisory committees; Celgene: Honoraria, Membership on an entity's Board of Directors or advisory committees; Sanofi-Aventis: Honoraria, Membership on an entity's Board of Directors or advisory committees.
Author notes
Asterisk with author names denotes non-ASH members.


This feature is available to Subscribers Only
Sign In or Create an Account Close Modal