Abstract
Abstract 4688
While persistence to drug therapy is essential to achieve optimal patient benefits, poorly controlled MM results in more rapid disease progression, disease-related complications, impact on quality of life, and premature death. Additionally, the cost of delivering medical care for myeloma patients is also an important consideration for society and payers.
To evaluate the real-world persistence with lenalidomide treatment in MM patients, and assess the relationship between treatment persistence and (1) indicators of poor disease control and disease-related complications and (2) the total health care costs for patients with MM.
Commercial and Medicare Advantage enrollees initiating LEN for treatment of MM with pharmacy and medical benefits in the 6 months prior and 1 year following initiation of LEN were identified in a US health plan claims database (7/1/2007–6/30/2011). MM was identified by at least 2 medical claims at least 7 days apart with a MM diagnosis code (ICD-9: 203.0x). Treatment discontinuation was defined as the first appearance of a gap greater than 30 days between runout date (prescription fill date + days supply) and next lenalidomide prescription fill. Persistence was defined as days from the first LEN treatment to the earlier of either the date of discontinuation or end of the follow-up period (i.e., 6/30/2011). Disease-related complications included sepsis, indictors of relapse or disease progression (defined as the addition of bortezomib (BORT) to a LEN regimen, a switch to BORT from a LEN regimen, or discontinuation of LEN followed by restarting LEN), sepsis, and evidence of skeletal-related events (SREs) defined as fracture, spinal cord compression, surgery and/or radiation to the bone. Total health care costs include combined payer and patient paid amounts under the medical benefit (e.g., hospital, office, ER) and retail pharmacy benefit (inclusive of specialty pharmacy). Multivariate regression-based models were used to examine the relationship between persistence and measures of disease control and complications, as well as the relationship between persistence and first-year health care costs controlling for age, gender, comorbidity score, prior stem cell transplant, prior SREs, and insurance type (commercial or Medicare Advantage).
Among the 605 patients meeting the inclusion criteria, persistency with lenalidomide averaged 6.0 months (median = 4.9) with 57.9% of patients being persistent for the entire year. A one month increase in persistence was associated with a lower probability of SREs (OR=0.96; p=0.078), sepsis (OR=0.86; p<0.001), and relapse or disease progression (OR=0.78; p<0.001). The probability of an inpatient hospitalization (OR=0.68; p-value<0.001) and additional ER visits (OR=0.83; p=0.002) were both lower with longer duration. When examining the relationship between persistence and health care costs, a one-month increase in persistence was found to be associated with, on average, a 8% decrease in medical care costs (p=0.007) and an 8% increase in pharmacy costs (p<0.001).
Improved persistence with lenalidomide therapy was associated with improved patient outcomes as demonstrated by fewer SREs and lower likelihood of developing sepsis, consequently leading to cost saving due to fewer hospitalizations and ER visits. The reduction in medical costs offsets the expected increase in pharmacy costs as lenalidomide is covered under the pharmacy benefit. This analysis demonstrates that continuous treatment with lenalidomide can not only improve disease control in MM patients, but in addition also reduces health care utilization and related costs as indicated by the lower risk of a hospitalization and number of ER visits, and could therefore be budget neutral in terms of overall societal burden of health care costs associated with MM.
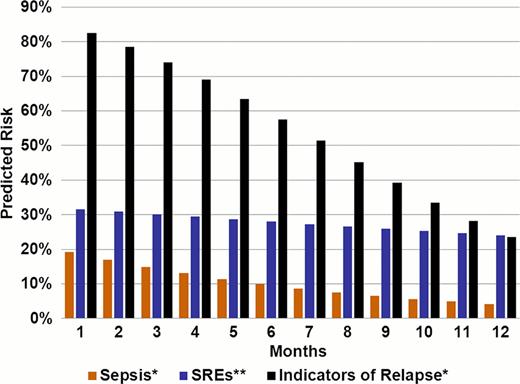
Predicted Risk of Sepsis and SREs as a function of lenalidomide persistence – 1 year follow-up.
Predicted Risk of Sepsis and SREs as a function of lenalidomide persistence – 1 year follow-up.
* p<0.001; ** p=0.078.
Henk:OptumInsight: Consultancy. Kaura:Celgene: Employment. Khan:Celgene: Employment.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal