Abstract
Despite the advances in Diffuse Large B-Cell Lymphoma (DLBCL) treatment, there is a lack of uniformity regarding survival among the entire patient population. This study investigates several individual-level markers of socioeconomic and clinical status in relation to DLBCL survival.
This is a retrospective cohort study that utilizes a study population that was derived from the Moffitt Cancer Center Total Cancer Care protocol, a database that contains clinical, biological, and demographic information for over 73,000 patients as well as molecular and cytogenetic information on over 36,000 tumors.
The database included 440 persons who were diagnosed with Diffuse Large B-Cell Lymphoma between 1998 and 2012. Of these persons, 274 met the eligibility criteria. A descriptive analysis was first conducted on all variables in the study and was then stratified by insurance status. A forward step-wise Cox proportional hazard regression was performed to calculate adjusted hazard ratios (HR) and their 95% confidence intervals for the association between insurance status and relapse, progression, or death utilizing SAS 9.3 (SAS Institute, Inc., Cary, NC). The Kaplan-Meier method was used to generate survival curves for each insurance group and compared according to the log-rank test. This was done in order to examine any differences in median survival time (in months) between the two groups.
In terms of both overall survival and event-free survival, race was a significant prognostic factor in this study with non-Caucasian subjects being more likely to experience mortality (HR 2.33; 95% CI, 1.39 - 3.88). Subjects who presented with b-symptoms (fevers, unintentional weight loss >10%, and night sweats) at the time of diagnosis were significantly more likely to experience mortality (HR 2.48; 95% CI, 1.67 - 3.67) than those who were without them. Both stage and nodal status of a subject’s disease at the time of diagnosis were significantly associated with the outcome as subject’s with advanced stage disease (HR 3.89; 95% CI, 2.25 - 6.76) and extra nodal disease (HR 1.58; 95% CI, 1.04 - 2.39) had a higher risk of death.
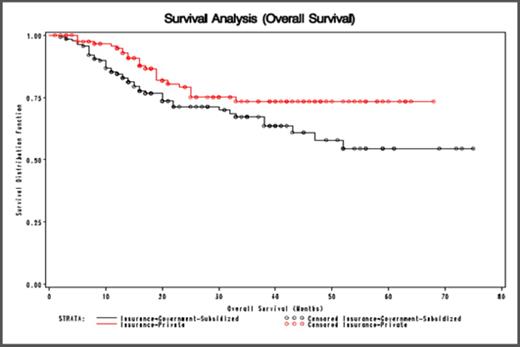
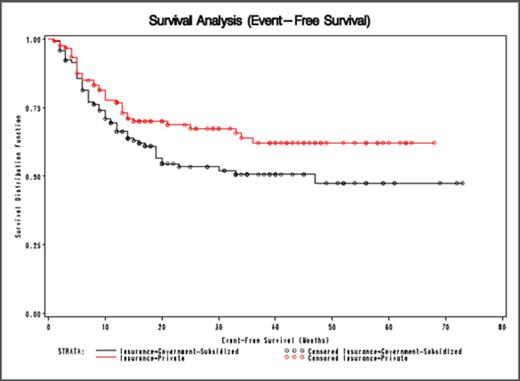
For overall survival, subjects in the privately-insured group experienced a significant difference in overall survival time (Log-Rank p=0.04) compared to those subjects with government-subsidized insurance (Figure 1). There was also a statistically significant difference in event-free survival between the two insurance groups (Log-Rank p=0.05) (Figure 2). Notably, age was not a significant covariate for OS or EFS, suggesting that the government-subsidized group was not biased by an increased proportion of elderly Medicare enrolled patients.
Overall Survival in Diffuse Large B-Cell Lymphoma by Insurance Status
Overall Survival in Diffuse Large B-Cell Lymphoma by Insurance Status
Event Free Survival in Diffuse Large B-Cell Lymphoma by Insurance Status
Event Free Survival in Diffuse Large B-Cell Lymphoma by Insurance Status
In this retrospective cohort study, we observed that event-free survival time among subjects with private insurance were significantly improved from those subjects with government-subsidized insurance and overall survival time among subjects with private insurance were significantly improved from those subjects with government-subsidized insurance. We determined that after adjustment for demographic and clinical covariates, the covariates race, presentation of b-symptoms at the time of diagnosis, stage at the time of diagnosis, and nodal status of a subject’s disease were all significant prognostic factors in both overall and event-free survival.
No relevant conflicts of interest to declare.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal