Abstract
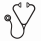
Background
Supportive care (BSC) including hematopoietic cytokines still remains an important component of treatment for lower-risk myelodysplastic syndrome (LR-MDS) including low or intermediate-1 risk by International Prognostic Scoring System (IPSS) even in the era of hypomethylating agents (HMA). The role of front-line HMA for LR-MDS has not been clearly defined yet. In the current study, we evaluated the long-term outcomes of patients with LR-MDS treated with front-line HMA compared to those treated with supportive care.
Methods
The data of 353 patients diagnosed with LR-MDS from Oct 1992 to Jul 2013 were retrospectively evaluated. The prognostic factors affecting overall survival were evaluated within all population. Then, we performed a case-constrol study using 122 patients with propensity score matched (PSM) population.
Results
Initial patient population (n=353) included 110 patients treated with BSC and 243 treated with HMA. Patients characteristics (age, gender, IPSS risk groups, IPSS blast score, IPSS cytopenia score) were similar between two groups, however, ECOG performance status (PS) and IPSS cytogenetic score were biased between two groups. ECOG-PS 2-3 were 32 patients (29.1%) in BSC and 20 (9.3%) in HMA group (p<0.001) and IPSS cytogenetic score °Ã0.5 were 27 patients (25.2%) and 33 (14.6%) in HMA group (p=0.032). In the multivariate analysis, ECOG-PS 2-3 (HR 4.586, p<0.001), IPSS blast °Ã0.5% (HR 2.549, p<0.001) and front-line HMA therapy (HR 2.019, p=0.006) were unfavorable factors affecting OS. Using PSM population, we performed a case-control study comparing the outcomes of 61 patients in each group who treated with BSC and front-line HMA. Patient characteristics were well balanced between two group. In the multivariate analysis, ECOG-PS 2-3 (HR5.036, p<0.001), IPSS blast °Ã0.5% (HR 2.157, p=0.035), and first-line HMA therapy (HR 2.213, p=0.026) were still unfavorable factors for OS. The 5-year OS rate was 62.5±10.8% in BSC group and 41.0±7.4 in HMA group, respectively (p=0.049).
Conclusion
Front-line HMA for patient with LR-MDS showed inferior long-term outcomes compared to BSC in PSM population. The role of front-line HMA should be elucidated in prospective studies on LR-MDS patients.
Overall survival between BSC and HMA groups in propensity score matched population
Overall survival between BSC and HMA groups in propensity score matched population
Off Label Use: Rituximab has been used as an off-label drug for adult ALL, and has been provided by Roche Inc. for scientific purpose. .
Author notes
Asterisk with author names denotes non-ASH members.
This icon denotes a clinically relevant abstract

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal