Abstract

Introduction: Azacitidine (AZA) therapy has become the recommended first-line treatment for patients with high-risk myelodysplastic syndromes (MDS) and oligoblastic acute myeloid leukemia (AML; bone marrow blasts <30%). However, only around 50% of patients achieve objective responses with AZA therapy and the vast majority of responding patients have disease progression within 2 years resulting in dismal survival rates.
Vitamin D (VitD) is a central regulator of calcium and bone homeostasis and affects multiple signaling pathways controlling proliferation, apoptosis and differentiation. More than 30 years ago, VitD was demonstrated to induce in vitro differentiation of AML blast cells. Consequently, VitD alone or in combination with other differentiating agents has been used for treatment of MDS patients showing inconsistent and rather limited efficacy. We retrospectively tested the hypothesis that VitD levels prior to start of treatment are predictive of overall survival (OS) in newly diagnosed MDS and oligoblastic AML patients receiving upfront AZA therapy. In addition, the antiproliferative effects of AZA in combination with different VitD derivatives were investigated in vitro.
Patients, materials and methods: A total of 58 patients treated at our center between 2006 and 2014 had serum samples available for assessment of VitD status. Serum samples were collected at a median of 18 days prior to start of AZA treatment and cryopreserved at -80°C. VitD status was assessed by measurement of circulating 25-hydroxyvitamin D levels applying a standard chemiluminescent immunoassay (DiaSorin Deutschland GmbH, Dietzenbach, Germany). Overall survival (OS) was estimated using the method of Kaplan and Meier. Survival times were measured from the date of AZA treatment start. Comparison of OS between the VitD groups was done using the logrank test and by cox regression adjusting for known confounders.
For in vitro analyses, a tetrazolium based MTT assay was used for assessment of growth inhibition of two different AML cell lines (HL60 and MOLM13) after exposure to AZA alone or in combination with VitD (1alpha,25-dihydroxyvitamin D and 25-hydroxyvitamin D; both from Cayman Chemical, Ann Arbor, MI, USA) or the VitD antagonist TEI-9647 (kindly provided by Teijin Pharma Ltd., Tokyo, Japan). Drug interactions were analyzed using the median-effect method of Chou and Talalay and combination index (CI) values were calculated according to the classic isobologramm equation with CI<1, CI=1 or CI>1 corresponding to synergism, additivity or antagonism, respectively. In cases where no antiproliferative activity upon single-agent treatment was assessable (low-dose VitD and TEI-9647), an analysis in terms of sensitization (potentiation) or inhibition of AZA activity was performed instead.
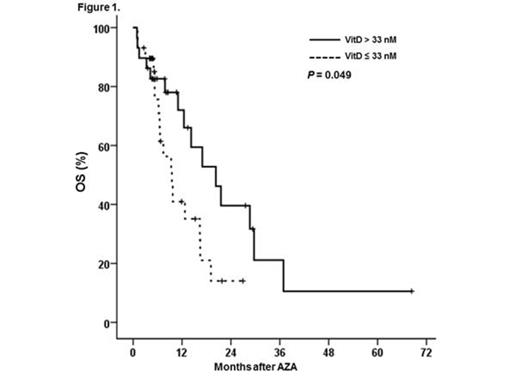
Results: Estimated median follow-up time was 14.2 months. Median serum VitD level prior to AZA treatment was 33 nM (range 11-102 nM). A total of 18 patients underwent allogeneic stem cell transplantation (alloSCT) following AZA therapy and follow-up was censored at the time of alloSCT. Patient, disease and treatment characteristics did not differ significantly between the low (≤33 nM; n=29) and high (>33 nM; n=29) VitD group. Estimated one-year survival was 72% (95% CI 54-90%) in the high VitD group, which was significantly longer as compared to the low VitD group (41%, 95% CI 20-62%, p<0.05; Figure 1). In multivariate analysis with OS as endpoint, VitD (per 10 nM decrease, HR 1.83 95% CI 1.06-3.16, p=0.03) and adverse cytogenetics (HR 2.58 95% CI 1.10-6.06, p=0.03) were independent predictors of shorter survival. In vitro treatment of HL60 and MOLM13 cells with AZA in combination with VitD produced synergistic and additive antiproliferative effects. Addition of nanomolar concentrations of VitD to AZA resulted in potentiation of AZA activity. Conversely, combination with TEI-9647 resulted in inhibition of AZA activity.
Conclusions: Our study suggests that higher VitD levels were associated with a survival advantage following upfront AZA therapy. As compared to AZA monotherapy combination treatment with VitD resulted in enhanced cytotoxic effects in vitro. VitD repletion/supplementation during AZA treatment should therefore be explored.
Luft:Immundiagnostik AG: Research Funding.
Author notes
Asterisk with author names denotes non-ASH members.

This icon denotes a clinically relevant abstract

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal