Abstract

Introduction
Imatinib has indeed revolutionized the treatment of chronic myelogenous leukemia (CML) since more than 15 years now, especially in CP. The first patients (pts) in this setting were treated with this compound within the IRIS phase III trial from Novartis, started in January 2000. Regular updates of the results of this study have been presented during various meetings until year 7, and academic studies have recently reported the outcomes of IM first-line CP CML pts after 66 months follow-up. However, little is known about the very long-term outcomes (>8 years) of such first-line pts and these data might be of interest while generic forms of IM will be soon launched in this setting.
In this study, we aimed to look at long-term outcomes in terms of efficacy and toxicities in first-line CP CML pts treated with branded form of IM (Glivec®).
Methods
This is a comprehensive retrospective analysis of first-line CP CML pts treated with IM first-line 400 mg daily since diagnosis and followed in 2 university reference centers for CML between 2000 and 2015, inside or outside academic or industrial clinical trials. All living pts have given their agreement for participation in this retrospective analysis. Pts have been analyzed in intention-to-treat, CML was defined according to ELN criteria [CP, accelerated phase (AP) and blast crises (BC)], Sokal, Euro and EUTOS scores have been calculated as published. Molecular biology tests have been performed according to ELN guidelines and BCR-ABL1/ABL1 were expressed as % on the international scale and 3 ELN conversion factors have been applied successively along time according to material exchanges performed with the central European laboratory in Mannheim. Cytogenetic and molecular responses have been defined according to the ELN criteria. Overall survival (OS) was calculated from the date of IM initiation until death at any time and for any reason; until progression to AP or BC at any time for progression-free survival (PFS); and until death, progression to AP or BC, failure on IM or IM treatment discontinuation for any cause including treatment-free remission (TFR), for event-free survival (EFS). The cut-off date for this analysis was the 20th of July 2,015.
Results
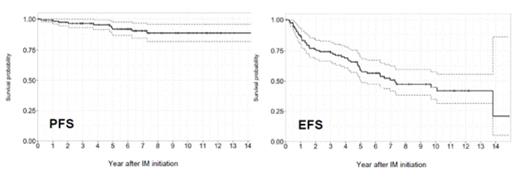
At time of analysis, 120 pts could be analyzed, with a median follow-up of 85.5 (1-194) months, 70 (58%) were males, with a median age of 55 (11-85) at IM initiation. Sokal score was high for 24(20%) pts, intermediate for 58 (49%), low for 34 (30.5%), unknown in 4 (0.5%) pts. Four (3.5%) pts had a variant Ph chromosome, 7 (6%) with additional chromosomal abnormalities, and 2 a masked Ph chromosome, 6 harbored atypical BCR-ABL1 transcripts excluded from analysis. Early molecular response (M3) was achieved in 86 (72%) pts, unreached in 20 (16%) pts, and unknown for 15 (12.5%) pts. It was predictive of Major Molecular Response (MMR) at 12 months (p=0.01, OR 5.35, 95%CI [1.3-31.94]), for MR4 rates at 24 months (p=0.03, OR 7.35 95%CI [1-328]) and for EFS (p=0.006) but not for OS and PFS in a multivariate Cox model analysis. MMR was achieved in 42% of evaluable pts at 12 months. Eutos, Euro and Sokal scores had no impact on OS, PFS and EFS. Five pts progressed to BC (1 myeloid, 4 lymphoid) within the 5 first years and died after allogeneic stem cell transplantation. The PFS rates were 97.5% at 2 years, 92% at 5 years, 88.6% at 10 and 14 years, EFS rates were 76% at 2 years, 60% at 5 years, 45% at 10 years and 21% at 14 years (figure 1), OS rates were 98% at 2 years, 95% at 5 years, 87% at 10 and 14 years.
Figure 1: PFS and EFS in pts on IM first-line. (Dashed lines represent 95%CI).
MR4.5 was achieved in 58 (48.5%) pts after a median of 46 (3-191) months and TFR strategy (or trial) was proposed in 28 pts (23.5%) and successful in 15 (12.5%) pts. At latest follow-up, after a median of 85.5 (4-180) months, 64 (53.5%) pts are still on IM, and 44 (37%) have switched to an alternative therapy for intolerance (17 pts, 14%) or resistance (16 pts, 13.5%, 7 with a BCR-ABL mutation) to IM and 11 for other causes (pregnancy, secondary tumors…). Overall, at latest follow-up, 10/120 pts died, 5 of CML progression and 5 from other causes.
Conclusions
After a very long median follow-up of more than 85 months, IM still consistently provides high rates of remission and survival, without disease progression and severe long-term toxicities. In addition, half of the pts reached the MR4.5 level, ≥2 years stable in 23.5% of the pts offering the possibility of a treatment-free strategy.
Nicolini:Bristol-Myers Squibb: Honoraria, Membership on an entity's Board of Directors or advisory committees, Speakers Bureau; Ariad Pharmaceuticals: Honoraria, Membership on an entity's Board of Directors or advisory committees, Speakers Bureau; Novartis: Honoraria, Membership on an entity's Board of Directors or advisory committees, Research Funding, Speakers Bureau. Mahon:Novartis: Consultancy, Honoraria; ARIAD: Consultancy; Pfizer: Consultancy; Bristol-Myers Squibb: Consultancy, Honoraria. Etienne:Novartis: Consultancy, Honoraria; BMS: Honoraria.
Author notes
Asterisk with author names denotes non-ASH members.

This icon denotes a clinically relevant abstract

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal