Abstract
Background: Lenalidomide, one of the immunomodulatory drugs, is an important component of treatment for multiple myeloma. Lenalidomide inhibits the proliferation of tumor cells via antiangiogenesis, induces apoptosis and acts directly on the immune system and tumor microenvironment. Immunomodulatory effects of lenalidomide notably stimulate the production of cytokines and activation of T-cells and natural killer cells. Skin rash is a frequent adverse event of lenalidomide. Some studies have shown a correlation between the efficacy of anti-cancer agents such as tyrosine kinase inhibitors and the development of skin rash. However, the relationship between the development of lenalidomide-associated skin rash and its efficacy is unclear. We conducted a retrospective survey to clarify whether development of skin rash correlates with the efficacy of lenalidomide.
Materials and Methods: All patients with multiple myeloma who received lenalidomide at 9 hospitals in Japan from July 2009 to December 2015 were serially registered. The chart review was performed for all identified patients to obtain the following information; age, sex, performance status at the initiation of lenalidomide, International Staging System (ISS) classification, prior chemotherapy regimen, tumor response, development of skin rash and clinical outcomes. A log-rank test was used to assess the relationship between the presence of skin rash and survival. A two-sided p < 0.05 was considered statistically significant. This study received approval from the appropriate ethics committees.
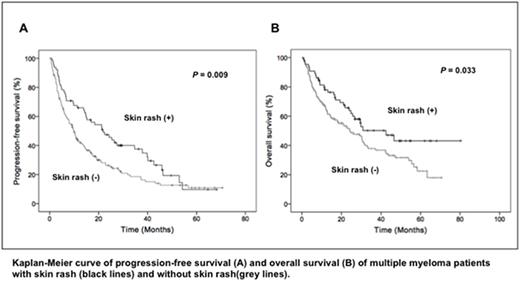
Results: We identified 215 patients (92 women and 123 men), with a median age was 69 years (range, 39-86 years). Types of myeloma were as follows: 139 patients of IgG, 43 of IgA, and 29 of Bence-Jones protein. ISS was available for 204 patients, and of these, 63, 73, and 68 patients were classified as ISS stage I, II, and III, respectively. The median number of prior therapies was 2 (range, 0-6); 161 (74.9%) and 46 patients (21.4%) had previously received bortezomib and thalidomide, respectively. Fifty patients (23.3%) had undergone previous autologous stem cell transplantation. Sixty-five patients (30.2%) developed a skin rash after lenalidomide initiation, and the median time to onset of skin rash was 12 days. The patients with and without skin rash were similar with respect to age, type of myeloma, and ISS. The median follow-up of survivors was 28.9 months (range, 1.7-80.3 months). The progression-free survival and overall survival were better in patients who had skin rash than in those who did not (p = 0.009 and p = 0.033, respectively) (Figures A and B).
Conclusions: In this study, the progression-free survival and overall survival among patients with skin rash during lenalidomide therapy was significantly superior to the patients without skin rash. Lenalidomide-associeated skin rash in patients with multiple myeloma may be a predictive factor of their clinical outcome.
Nagai:Takeda: Honoraria, Research Funding; Janssen: Research Funding; Mundipharma KK: Research Funding.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal