Introduction
Despite improvements in first-line treatment of childhood T-ALL, relapse remains the main cause of treatment failure. Patients with T-ALL experiencing leukemia recurrence have a dismal outcome, mostly due to a failure to achieve a second complete remission (CR) or to subsequent relapse. Assessment of minimal residual disease (MRD) may allow identifying subsets of patients with different prognosis. We analyzed the outcomes of 141 Italian children and adolescents who experienced T-ALL relapse after frontline multicenter AIEOP-BFM ALL treatment trials.
Methods:
This retrospective study aimed at describing the outcomes of Italian patients with T-ALL who were enrolled in the AIEOP-BFM ALL2000, 2006 and 2009 trials and subsequently experienced disease relapse. Among the 750 T-ALL Italian patients enrolled in the above-mentioned trials, 141 had a disease recurrence (70/251 patients in ALL2000 trial, 29/190 in ALL2006 trial, and 42/309 in ALL2009 trial). Molecular MRD monitoring after induction therapy for leukemia relapse was available for 38 patients.
Results:
The 141 patients, 113 males and 28 females, had a median age of 9 years at diagnosis (range 1-17) and 10 at relapse (range 2-19).
At diagnosis, 7 patients were allocated to the Standard (SR), 45 to the Medium (MR), and 89 to the High Risk (HR) group, respectively. Thirty-four (4 MR and 30 HR patients) of these children were given allogeneic hematopoietic stem cell transplantation (allo-HSCT) in 1st CR and 41 had received central nervous system (CNS) radiotherapy.
Relapses were classified as very early (occurring <18 months from diagnosis), early (occurring ≥18 months from diagnosis and <6 months after completion of primary therapy), and late (occurring >6 months after the end of the frontline protocol) in 92, 36, and 13 patients, respectively.
Site of relapse was isolated bone marrow (BM) in 74 patients, combined BM/extramedullary (EM) in 23 patients, and isolated EM in 44 patients (involving a single EM site in 37 cases and >1 EM site in 7 cases; CNS was involved in 29 patients).
At the time of relapse, 7 patients were treated according to AIEOP ALL REC98 Trial, 57 according to AIEOP ALL REC2003 Trial, while the remaining 77 patients received other combination of chemotherapy.
After reinduction/consolidation treatment, 58 patients were given allo-HSCT from either a matched family donor (16) or an unrelated donor (UD, 31 patients, of which 21 from a matched UD and 10 from a mismatched UD) or an HLA-partially matched relative (11).
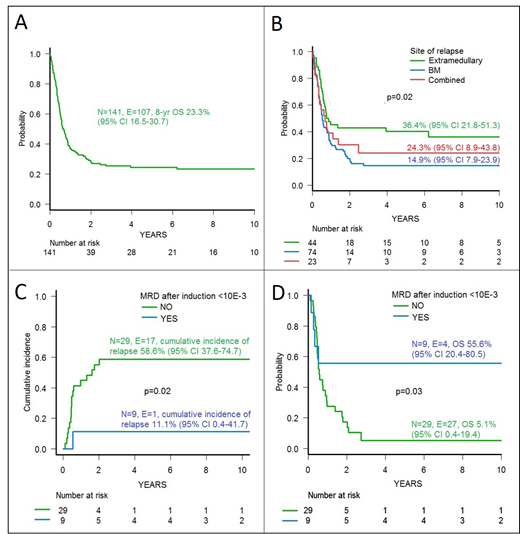
With a median follow-up of 7.5 years (range 2-14), 34 patients are currently alive; 17 of these patients had EM isolated relapse, which was very early in 13 cases, and 17 had BM involvement at relapse, with late relapse in 8 cases. The 8-year overall survival (OS) of the whole cohort was 23.3% (95% CI 16.5-30.7) (Figure 1A). Isolate EM relapse (Figure 1B) and late relapses were associated with a better OS probability. Both factors remained statistically significant in multivariable analysis. Moreover, in univariable analysis a better prognosis was observed in patients treated more recently (i.e., after year 2008) (8-year OS 31.8% vs 16.2%, p=0.01).
After allo-HSCT, 29 patients are currently alive, while the remaining 29 patients died from progressive disease (21) or transplant-related causes (8), leading to a 8-year OS for patients given allo-HSCT in 2nd RC of 48.5% (95% CI 34.7-61.0).
Of the 83 children given sole chemotherapy, 5 are currently alive, while the remaining 78 died due to progressive disease (53), organ-failure (7), infection (9), or other causes (9).
MRD monitoring was performed for 38/97 patients with BM involvement (5 with late, 13 with early, and 20 with very early relapse, respectively). Patients with a post-induction MRD <10-3 showed a reduced incidence of relapse (Figure 1C), resulting into better probability of 8-year OS (Figure 1D) in comparison to patients with higher MRD levels.
Conclusions:
Our results confirm that T-ALL relapse, especially if involving BM and occurring within 6 months from treatment discontinuation is still associated with poor prognosis, although in the last 10 years a higher proportion of children with relapsed T-ALL has been rescued by second line therapy, including transplantation. In this Italian retrospective cohort, a MRD value >10-3 at the end of induction therapy predicts a miserable outcome, this finding allowing to identify patients eligible to experimental therapies.
Merli:Novartis: Honoraria; Amgen: Honoraria; Bellicum: Consultancy; Sobi: Consultancy. Rizzari:JazzPharma, Shire, medac , Sigma-Tau, Baxalta, Shire and Servier: Consultancy, Honoraria; Together with study group from Shire, medac , Sigma-Tau, Baxalta, Shire and Servier: Research Funding. Parasole:Servier: Honoraria; Baxalta: Honoraria; Eusapharma: Honoraria. Locatelli:bluebird bio: Consultancy; Miltenyi: Honoraria; Novartis: Consultancy, Membership on an entity's Board of Directors or advisory committees; Amgen: Honoraria, Membership on an entity's Board of Directors or advisory committees; Bellicum: Consultancy, Membership on an entity's Board of Directors or advisory committees.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal