Introduction: Systemic mastocytosis with associated hematologic neoplasm (SM-AHN) is defined by the presence of a concomitant hematologic malignancy with chronic myelomonocytic leukemia (CMML) being a particularly common partner. The overall survival of patients with SM-AHN is inferior to those with SM alone, even when matched for relevant prognostic covariates. However, the prognostic impact of mastocytosis in patients with CMML is unknown.
Methods: CMML patients with concomitant mastocytosis were identified from the Moffitt Cancer Center CMML database. We assessed baseline demographic, clinical, and molecular findings and used Kaplan-Meier method to estimate overall survival (OS). The log-rank test was used to compare Kaplan-Meier curves, We then compared the SM-CMML cohort to a well-established institutional database of CMML patients. Baseline demographic and clinical variables were analyzed using GraphPad Prism and SPSS was used for Cox Regression Analysis.
Results: Between 5/2004 and 5/2019 22 of 645 CMML patients (3.4%) were identified to have concomitant mastocytosis. The median follow-up for the 22 patients with SM-CMML was 51 months. Nine (41%) patients were diagnosed with de novo CMML prior to SM. In these cases, secondary SM-CMML occurred at a median time of 7 months after CMML diagnosis. Ten patients (45%) were diagnosed with CMML and SM concurrently and 3 (14%) were diagnosed with SM prior to CMML. Among 17 patients tested for KIT mutations, 12 were found to harbor a mutation. The remaining five patients did not undergo high-sensitivity KIT testing on a bone marrow aspirate. Eleven patients had extended gene sequencing performed with the most common additional mutations involving TET2 (45%), SRSF2 (55%), ASXL1 (27%), RAS (27%), DNMT3A (27%), and RUNX1 (27%). The median overall survival (OS) was estimated to be 38.6 months.
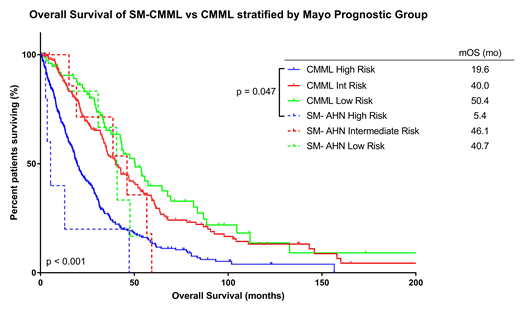
Next, we compared this cohort of SM-CMML patients to a large, established database of CMML patients (excluding those with concomitant SM). Age at diagnosis, baseline white blood cell count, hemoglobin, and platelet count were well matched between the two groups. Applying the Mayo CMML Prognostic Model to the cohort of SM-CMML patients demonstrated that 32%, 41%, and 27% were low, intermediate and high risk, respectively. In the CMML cohort, 13%, 35%, and 51% were low, intermediate and high, risk respectively, suggesting the SM-CMML was more common in the lower-risk group (p=0.025). The median OS was similar between the two cohorts (median OS 31.3 vs 38.6 months, p = 0.43). However, multivariate analysis including Mayo Prognostic Scoring System, age > 65, and SM component revealed all three variables to be independently associated with survival (HR 1.8, p < 0.001; HR 1.7, p = 0.047; and HR 1.5, p 0.003, respectively). Assessing the impact of mastocytosis in low, intermediate, and high-risk groups separately, the inferior prognostic impact of mastocytosis was most prominent in high-risk patients (OS 19.6 mo vs. 5.4 mo; p = 0.049). Survival outcomes between SM-CMML and CMML were not statistically different in intermediate and low-risk groups (p = 0.47 and p = 0.19, respectively).
Among 16 deaths in the SM-CMML cohort, cause of death was able to be assessed in 13 patients. Four (31%) patients died after transformation to acute myeloid leukemia (AML). These patients were either intermediate- or high-risk by Mayo Prognostic Model. Nine patients (69%) died due to multisystem organ failure due to progressive systemic mastocytosis without development of acute leukemia. Among these, 4 (44%) were low-risk, 3 (33%) were intermediate-risk, and 2 (22%) were high-risk.
Conclusions: SM-CMML typically presented with lower-risk disease when graded by the Mayo CMML Prognostic Model. Compared head-to-head, OS was similar between SM-CMML and CMML; however multivariate analysis revealed the SM component to be a significant adverse prognostic factor. The presence of bone marrow mastocytosis is associated with inferior survival in high-risk CMML cases. Cause of death among SM-CMML patients was attributable to both progressive mastocytosis and transformation to AML. AML transformation was limited to intermediate- and high-risk group while progressive mastocytosis was seen across the risk spectrum. Future studies are warranted to determine if SM therapy can mitigate this outcome.
Kuykendall:Abbvie: Honoraria; Celgene: Honoraria; Incyte: Honoraria, Speakers Bureau; Janssen: Consultancy. Talati:Celgene: Honoraria; Agios: Honoraria; Jazz Pharmaceuticals: Honoraria, Speakers Bureau; Daiichi-Sankyo: Honoraria; Astellas: Honoraria, Speakers Bureau; Pfizer: Honoraria. Komrokji:DSI: Consultancy; Incyte: Consultancy; Agios: Consultancy; JAZZ: Consultancy; JAZZ: Speakers Bureau; Novartis: Speakers Bureau; pfizer: Consultancy; celgene: Consultancy.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal