Abstract
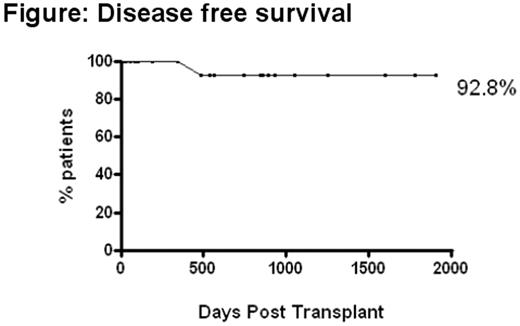
We evaluated the toxicity-profile, engraftment potential, and efficacy of fludarabine-based nonmyeloablative allogeneic HCT in patients with a variety of nonmalignant hematological disorders. Twenty three patients (median age 29 years; range 11–52) with nonmalignant hematological disorders including ATG refractory SAA (n=13), severe paroxysmal nocturnal hemoglobinuria (PNH: n=9), and pure red cell aplasia (PRCA; n=1) were transplanted from 5/99 – 8/2004 at the NHLBI. The majority of patients had an extensive transfusion history including 11/23 who had HLA allo-antibodies and 4/23 with allo-antibodies to RBCs. Conditioning with fludarabine (25 mg/m2 x 5 days), ATG (40mg/kg x 4 days) and cyclophosphamide (60mg/kg x 2 days) was followed by infusion of an un-manipulated G-CSF mobilized allograft from an HLA matched sibling (n=18), parent (n=2), or single antigen mismatched sibling (n=3). GVHD prophylaxis consisted of cyclosporine (CSA) either alone (n=2) or combined with mycophenolate mofetil (n=10) or mini-dose methotrexate (n=11). Despite a high prevalence of pre-transplant allo-immunization, all patients achieved sustained donor engraftment in both myeloid and T-cell lineages. Myeloid recovery (neutrophils >500cells/uL) occurred at a median 14 days post transplant (range 8–18 days). Conversion from mixed to full donor myeloid and T-cell chimerism occurred in all patients by 110 days post-transplant. CMV reactivation occurred in 11/21 patients at risk (KM probability 52%) without any cases of CMV disease. Grade II–IV and III–IV acute GVHD was the major transplant complication occurring in 13/23 (KM probability 60%) and 8/23 (KM probability 38%) patients respectively. Fourteen of 21 evaluable patients developed chronic GVHD (limited in 11 cases), which resolved completely with low-dose alternate day steroids and/or CSA in all but 1 case. One patient who received an allograft from his HLA matched father died 16 months post-transplant from complications related to chronic GVHD. With a median follow up of 25 months (range 1–64 months), 20/21 patients evaluable more than 100 days post-transplant survive in complete remission with full donor chimerism in all lymphohematopoietic lineages (KM probability of long-term survival 92.8 %-see figure ).
Conclusion: Fludarabine-based nonmyeloablative transplantation achieves excellent donor engraftment and long-term disease free survival in heavily transfused and allo-immunized patients with ATG refractory SAA and other nonmalignant hematological disorders associated with bone marrow failure.
Author notes
Corresponding author