Abstract
To define a role for hematopoietic stem cell transplantation (HSCT) in infants with acute lymphoblastic leukemia and rearrangements of the mixed-lineage-leukemia gene (MLL+), we compared the outcome of MLL+ patients from trial Interfant-99 who either received chemotherapy only or HSCT. Of 376 patients with a known MLL status in the trial, 297 (79%) were MLL+. Among the 277 of 297 MLL+ patients (93%) in first remission (CR), there appeared to be a significant difference in disease-free survival (adjusted by waiting time to HSCT) between the 37 (13%) who received HSCT and the 240 (87%) who received chemotherapy only (P = .03). However, the advantage was restricted to a subgroup with 2 additional unfavorable prognostic features: age less than 6 months and either poor response to steroids at day 8 or leukocytes more than or equal to 300 g/L. Ninety-seven of 297 MLL+ patients (33%) had such high-risk criteria, with 87 achieving CR. In this group, HSCT was associated with a 64% reduction in the risk of failure resulting from relapse or death in CR (hazard ratio = 0.36, 95% confidence interval, 0.15-0.86). In the remaining patients, there was no advantage for HSCT over chemotherapy only. In summary, HSCT seems to be a valuable option for a subgroup of infant MLL+ acute lymphoblastic leukemia carrying further poor prognostic factors. The trial was registered at www.clinicaltrials.gov as #NCT00015873 and at www.controlled-trials.com as #ISRCTN24251487.
Introduction
Acute lymphoblastic leukemia (ALL) diagnosed within the first 12 months of life accounts for 2.5% to 5% of pediatric ALL cases and displays unique biologic, clinical, and prognostic features that vary from those of older children with ALL.1-5 Approximately 80% of infant cases harbor rearrangements of the mixed-lineage-leukemia (MLL) gene at chromosome band 11q23 (MLL+).1,6,7 The prognosis is relatively poor with only approximately half of cases achieving a cure with current therapies.1,6 Whether the proportion of patients cured can be increased by the more frequent use of concepts, such as hematopoietic stem cell transplantation (HSCT) in first remission or intensification of contemporarily applied hybrid protocols, including both lymphoid- and myeloid-directed treatment elements, is a matter of debate.8 Moreover, possible long-term adverse effects of the preparative regimen before and of graft-versus-host disease (GVHD) after HSCT, disturbing the physical development in such a young and vulnerable patient population, demand for a very strict indication only left for infants with a predictably very poor chance to maintain first remission with chemotherapy alone.9,10
In the first large international multicenter trial for the treatment of infant ALL, Interfant-99, allogeneic HSCT was a possible option (but not mandated) for patients with initially poorly responding leukemia, defined by a poor response to steroids at day 8 of chemotherapy.6 However, no significant benefit of HSCT was observed in this cohort of high-risk patients when disease-free survival (DFS) was adjusted for the waiting time to HSCT. This was in accordance with the largest retrospective study reported until then, which suggested that there was no clinical benefit associated with HSCT in infants with MLL+ ALL.11,12 Nevertheless, because of the unique opportunity to analyze a large cohort of homogeneously treated infant ALL cases (483 patients), we aimed to more precisely define a possible role of HSCT in newly defined prognostic subgroups of infants with MLL+ ALL.
Methods
Patients
Between May 1999 and January 2006, a total of 483 infants (up to 365 days of age) with previously untreated ALL were entered into the international study Interfant-99 by 17 collaborative study groups in 22 countries.6 ALL was diagnosed according to standard morphologic, cytochemical, and immunologic criteria.13 The detection of MLL rearrangements was preferentially based on reverse transcription polymerase chain reaction or MLL split-signal fluorescence in situ hybridization analysis.2,14 However, classic 11q23 translocations without reverse transcription polymerase chain reaction/fluorescence in situ hybridization confirmation also counted for MLL+ cases. Patients were treated with informed consent from the patient's parents or legal guardians. Studies were conducted in accordance with the Declaration of Helsinki, and approval was delivered by the ethic committees of all participating institutions.
Patient characteristics, including clinical and laboratory features at diagnosis, the MLL status, and early response to therapy as well as outcome of randomized chemotherapeutic treatment arms, overall outcome, and multivariate analysis of risk factors for treatment failure, have been previously published.6 Of the 483 patients, 376 (78%) were evaluable for the MLL status and other relevant prognostic factors, such as age and white blood cell (WBC) counts at diagnosis, immunophenotype, response to a 7-day pro-phase with predniso(lo)ne and 1 intrathecal dose of methotrexate at day 1, and remission status after completion of induction therapy.
Risk factors for a relapse gained from the multivariate analysis of the total study population are as follows (based on their hierarchy of statistical significance)6 : MLL rearrangement (MLL+ vs MLL−), age at diagnosis (< 6 months vs ≥ 6 months), predniso(lo)ne response (good predniso(lo)ne response [GPR]: < 1.0 g/L blasts vs poor predniso(lo)ne response [PPR]: ≥ 1.0 g/L blasts at day 8), and WBC counts in peripheral blood at diagnosis (≥ 300 g/L vs < 300 g/L).6,15 Based on these findings, 3 new subgroups with a distinct relapse risk were defined to design a subsequent new study, Interfant-06. Therein, patients are assigned to 1 of 3 treatment branches: a low-risk group defined by the absence of MLL rearrangements (MLL−), a high-risk group with MLL positivity (MLL+), age less than 6 months, and either WBC counts more than or equal to 300 g/L or PPR, and a medium-risk group, including all others. This risk stratification will be used throughout the paper to illustrate the results.
Treatment
Treatment stratification and protocols of the Interfant-99 study have been published previously, and response criteria as well as definition of relapse have been described in detail elsewhere.6 Briefly, patients were assigned to 1 of 2 treatment branches: a standard-risk group for the GPR and a high-risk group for the PPR patients. All patients received a 5-week induction therapy (prednisone for 7 and afterward dexamethasone for 21 days, vincristine [VCR], daunorubicin, L-asparaginase, low-dose cytarabine, and intrathecals) followed by a 4-week consolidation (high-dose methotrexate [MTX], 6-mercaptopurine [6-MP], high-dose cytarabine, L-asparaginase, and intrathecals) and a 7-week reinduction therapy (dexamethasone, 6-thioguanine, VCR, daunorubicin, low-dose cytarabine, cyclophosphamide, and intrathecals). GPR patients in complete remission (CR) randomly continued with a late 4-week reintensification element (similar to consolidation but with additional VCR) and maintenance therapy (6-MP, MTX, steroid/VCR pulses) or maintenance therapy only up to a total therapy duration of 24 months. PPR patients in CR who were not allocated to allogeneic HSCT randomly continued with a late 4-week reintensification (same protocol as for the GPR patients) and intensified maintenance therapy (6-MP, MTX, steroid/VCR, and etoposide/cytarabine pulses) or intensified maintenance therapy only up to a total treatment duration of 24 months. Doses of the antileukemic drugs used were adjusted according to patients' age at the start of each treatment phase: children younger than 6 months were given two-thirds of the full dose, those 6 to 12 months of age were given three-fourths of the dose, and those 12 months of age or older were given the full dose. Intrathecal drugs (methotrexate, cytarabine, and prednisolone) were given in age-dependent fixed dosages.
Indications for HSCT in study Interfant-99 were defined by the protocol and reserved for patients with PPR, being performed after completion of reinduction therapy. Of note, Interfant-99 was not designed to study a benefit or lack of benefit of HSCT in infant (MLL+) ALL. Donor selection and type of the conditioning regimen as well as of GVHD prophylaxis and treatment were at the discretion of the participating study groups and transplantation centers. The European Bone Marrow Transplantation and the international Berlin-Frankfurt-Münster study committees advised a preparative regimen with etoposide, busulfan, and cyclophosphamide. Total body irradiation (TBI) was strongly discouraged because of concerns about long-term side effects. Cyclosporin A was recommended for GVHD prophylaxis.
Statistical considerations
Event-free survival (EFS), DFS, and overall survival (OS) curves were estimated with the Kaplan-Meier method and their SE with the Greenwood formula. The starting point for the observation time was the date of diagnosis for EFS and OS, whereas the date of first complete remission (CR1) was used for DFS. Death in induction, resistance, relapse, secondary malignancy, and death in continuous CR (CCR) were considered events in the calculation of EFS rates. Relapse, secondary malignancy, and death in CCR were events in the DFS estimation, whereas death from any cause was the sole event in determining OS. The observation time was censored at the last follow-up date if no event was recorded. Follow-up was updated on December 31, 2007. The median follow-up was 5 years (range, 0-9 years). The log-rank test was used for univariate comparisons. The outcome of patients who did or did not undergo HSCT in CR1 was compared adjusting for waiting time to transplantation, both in the Cox model (using a time-dependent treatment indicator) and in the estimation of the survival curves (with a landmark at 5 months and delayed entry for patients transplanted after the landmark). A term for the interaction between time from CR1 and treatment was introduced to account for a nonproportional hazard in the overall analysis. The interaction between treatment and risk group was tested before performing a separate subgroup analysis based on the Cox model. The likelihood ratio test was used, and all tests were 2-sided (P ≤ .05 referred to as statistically significant).
Results
Of the 376 evaluable patients, 297 (79%) had an MLL-rearranged leukemia and are described in Table 1 according to risk group stratification. Events and final outcome are shown in Table 2. A total of 37 of 297 (12%) MLL+ patients had HSCT in CR1 at a median time of 5 months from CR1 (range, 2-9 months). Twenty-one of 37 (57%) patients remained in CCR, compared with 91 of 240 (38%) patients treated with chemotherapy only. Notably, 10 of 37 (27%) underwent HSCT from a matched sibling donor, 19 of 37 (51%) from a matched unrelated donor, 5 of 37 (14%) from a mismatched unrelated donor, and in 3 of 37 (8%) cases type of stem cell donor was unknown. Stem cell sources were bone marrow (n = 22), peripheral blood stem cells (n = 3), cord blood (n = 9), and not available (n = 3). In 6 of 37 MLL+ patients, HSCT was performed despite a GPR, which was not an indication for this treatment procedure in the trial (WBC counts ≥ 300 g/L, n = 4; < 6 months of age, n = 3).
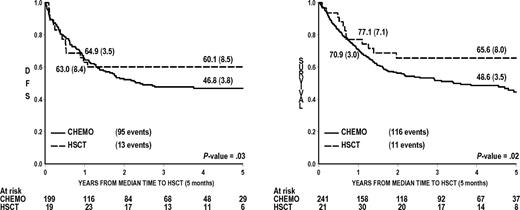
DFS and OS curves for the MLL+ patients having received chemotherapy only or HSCT in CR1 adjusted for waiting time to transplantation are shown in Figure 1. Results of the Cox regression model (Table 3) reveal that HSCT was associated with a significantly superior DFS (P = .03). The advantage of HSCT over chemotherapy becomes more evident with every successive year of follow-up, suggesting that HSCT provides greater protection against late relapses in children who do not fail initially (from relapse or toxic deaths; Table 3). These estimates, which account for waiting time to transplantation, are similar whether they are adjusted by known prognostic factors in Model I or by the risk stratification adopted in study Interfant-06 (Model II; Table 3). There was a significant interaction between risk group and treatment (P = .03), indicating that HSCT had a different effect in patients classified to the medium-risk or high-risk groups, as described in Figures 2 and 3, respectively. When analyzing DFS for both subgroups separately, the advantage of HSCT over chemotherapy was especially evident in the high-risk group (P = .01) but not in the medium-risk group (P = .09). In the high-risk group, HSCT was associated with a 64% reduction in the risk of failure resulting from relapse or death in CR (hazard ratio = 0.36, 95% confidence interval, 0.15-0.86). In the medium-risk group, there was an initial disadvantage of transplantation, which was overcome after 1 year from CR. Comparable results were found when OS instead of DFS was analyzed in the medium-risk (Figure 2) and high-risk (Figure 3) groups.
DFS and OS of 274 MLL+ infant ALL patients by treatment performed, adjusted by waiting time to HSCT. P value is from Cox Model. CHEMO indicates chemotherapy only; and HSCT, hematopoietic stem cell transplantation.
DFS and OS of 274 MLL+ infant ALL patients by treatment performed, adjusted by waiting time to HSCT. P value is from Cox Model. CHEMO indicates chemotherapy only; and HSCT, hematopoietic stem cell transplantation.
DFS and OS of 188 medium-risk patients with MLL+ infant ALL by treatment performed, adjusted by waiting time to HSCT. P value is from Cox Model. CHEMO indicates chemotherapy only; and HSCT, hematopoietic stem cell transplantation.
DFS and OS of 188 medium-risk patients with MLL+ infant ALL by treatment performed, adjusted by waiting time to HSCT. P value is from Cox Model. CHEMO indicates chemotherapy only; and HSCT, hematopoietic stem cell transplantation.
DFS and OS of 97 high-risk patients with MLL+ infant ALL by treatment performed, adjusted by waiting time to HSCT. P value is from Cox Model. CHEMO indicates chemotherapy only; and HSCT, hematopoietic stem cell transplantation.
DFS and OS of 97 high-risk patients with MLL+ infant ALL by treatment performed, adjusted by waiting time to HSCT. P value is from Cox Model. CHEMO indicates chemotherapy only; and HSCT, hematopoietic stem cell transplantation.
Discussion
One of the principal aims of the multinational trial Interfant-99 was to establish robust and independent prognostic markers in infant ALL to implement a new risk stratification system for the subsequent study, Interfant-06.6 MLL status, age, and WBC counts at initial diagnosis and response to steroids at day 8 appeared to have independent prognostic value.6 Of note, there was no difference in outcome with respect to the various translocation partners of the MLL gene. The overall 5-year EFS rate was 46.1% (SE 2.3%), and survival was 55.2% (SE 2.4%) for the whole study cohort of 483 patients. Of the 376 of 483 patients (78%) with evaluable risk factors, 297 (79%) were MLL+. Five-year EFS was 36.3% (SE 2.9%) for the 297 MLL+ patients and only 18.6% (SE 5.1%) for the subgroup of 97 patients with additional poor prognostic factors (ie, age < 6 months and either WBC counts ≥ 300 g/L or poor response to steroids at day 8).6 Consequently, this patient subset was defined as the high-risk group of the new trial Interfant-06 and, more importantly, as the target group for allogeneic HSCT in CR1.
Our present results on a large cohort of infants with MLL+ ALL actually demonstrated that only such high-risk patients (one-third of all MLL+ cases) appeared to benefit from allogeneic HSCT in CR1. Thus, the analysis may have helped to define a possible role for HSCT in the setting of infant ALL. Of note, there was a high early failure rate, with one-third of the high-risk patients having an event before the median time to transplantation, suggesting that early disease control in trial Interfant-99 was insufficient. Therefore, we are also attempting to improve remission quality in the Interfant-06 trial by an early randomized treatment intensification being delivered immediately after completion of induction therapy.
The main limitation of the present study is that the HSCT versus chemotherapy comparison was not supported by a donor-no donor design (the so-called “genetic randomization”).16,17 Thus, patients for whom a transplantation was planned but who relapsed before can only be counted in the chemotherapy group. The statistical analyses attempted to limit the related biases by adjusting for waiting time to transplantation and also by accounting for prognostic characteristics in a regression model.
Conflicting findings in several, mostly retrospective, studies dealing with the role of HSCT in infant (MLL+) ALL have suggested either no clinical advantage at all or a benefit at relatively low EFS rates.12,18-20 These (mostly single-center) studies had low patient numbers, and it was often unclear whether their results were truly representative of the whole population of patients with infant (MLL+) ALL or not.18-20 In addition, even some large retrospective multi-institutional series in infant MLL+ ALL saw no clear advantage for HSCT in CR1 compared with chemotherapy only.11,12
In a recent report from the Japan Infant Leukemia Group (MLL96 and MLL98 trials), the efficacy of an MLL-based stratifying treatment strategy involving HSCT for all infants with MLL+ ALL was evaluated.10,21 The 5-year EFS rate was only 38.6% for MLL+ ALL, which, however, was an improvement compared with historical controls. Notably, of 80 MLL+ infant cases, 27 of 49 events occurred before HSCT (mostly early bone marrow relapses); and of 22 of 49 events that occurred after HSCT, 8 were the result of toxic deaths. This report suggests that half of the events could not have been prevented by HSCT because they occurred too early for this final treatment procedure to be performed at all. In addition, the toxic death rate after HSCT was considerably high, so both findings suggest that further stratification within the MLL+ group is needed before the full potential of HSCT can be realized.
However, the results of another study using TBI during the conditioning regimen showed that, of 14 infants with MLL+ ALL transplanted in CR1, 11 (78.5%) are surviving in CCR.19 Moreover, the authors19 reported that outcome was associated with only moderate late-term effects, including growth and other neuroendocrine deficiencies, which were not different from that in older children given TBI and HSCT. Nevertheless, as the report did not specify the number of infant ALL patients with initial treatment failure and early relapses who accordingly failed before the time point of potential HSCT, studies of this type are not actually representative but encouraging to pursue HSCT for this group of poor prognostic infant ALL patients. This trial's caveat is also evident in another report using TBI within the conditioning regimen and not reporting either on the nontransplanted subgroup or on long-term side effects.18 Not surprisingly, most published studies available also indicated that disease status (CR1 vs CR2 or relapse) at HSCT and a short interval (without previous complications) between CR1 and HSCT were associated with a better prognosis.19-22
Recently, Dreyer et al23 reported on data from infant ALL trials of the Children's Cancer Group (CCG 1953) and Pediatric Oncology Group (POG 9407) that used a similar chemotherapy backbone and advised allogeneic HSCT to be performed in MLL+ cases. The 5-year EFS rates were 50.9% in the transplantation group and 48.7% in the chemotherapy only group, suggesting no clinical benefit for HSCT in CR1 for infants with MLL+ ALL. In addition, the United Kingdom infant ALL trial 92 found no difference in EFS comparing 11q23-positive patients who received HSCT (n = 12) and chemotherapy only.24 Moreover, a large retrospective collaborative study (1983-1995) that showed a marked clinical heterogeneity among MLL+ ALL requiring distinct treatment approaches for different age groups and different 11q23/MLL translocations also reported no significant benefit of HSCT in infant MLL+ ALL.12 A more recent update of this report still suggested that HSCT did not improve prognosis for t(4;11)-positive infant ALL.11 However, as the former large analysis might have been biased by patients' selection, the heterogeneous composition and intensity of the treatment approaches applied about more than 10 years earlier, the possible heterogeneous subtype distributions, and differing follow-up times, it cannot serve as the cornerstone on which the role of HSCT in infant MLL+ ALL can be founded.
A major concern in transplantation of infants is the risk of late effects because of the conditioning regimen before and occurrence and treatment of chronic GVHD after HSCT.8-10,25 There are no data available yet for the patients analyzed in the present study because of the relatively short observation time. However, late sequelae are reported to be common in transplanted long-term survivors of infant leukemia.8-10,25 Growth hormone deficiency, hypothyroidism, abnormal pubertal development, cardiac and hearing abnormalities, learning and academic difficulties, neuropsychologic deficiencies, osteopenia and osteoporosis, cataracts, hypertension, hyperinsulinemia, and dyslipidemias have all been reported to occur in young survivors after HSCT and have mostly been attributed to irradiation.8-10,25 In comparison, data on long-term side effects of transplantations not using TBI for infant ALL are scarce so that no definite conclusions can be drawn to date, although the European Bone Marrow Transplantation and international Berlin-Frankfurt-Münster study groups recommended a non–TBI-containing preparative regimen in the Interfant-99 trial.
Recently, we have shown that, in the Interfant-99 study, cases with high minimal residual disease (MRD) levels, as assessed at the end of consolidation therapy by immunoglobulin/T-cell receptor and/or MLL gene rearrangements, had an inferior DFS rate.26,27 The most striking finding was that all patients (n = 18) with MRD levels more than or equal to 10−4 after consolidation therapy relapsed, including 8 patients who would have been classified as medium risk in the Interfant-06 study and thus would have had no indication for allogeneic HSCT. Currently, the role of HSCT in improving the outcome for this patient subset awaits future studies. In addition, it is also unknown whether intensification of chemotherapy or innovative therapies (ie, FLT3 inhibitors, demethylating agents), either in conjunction with or instead of HSCT, will be able to permanently eradicate the disease.28-31 Nevertheless, given the extremely poor prognosis with standard chemotherapy only, HSCT in CR1 appears to be a possible treatment strategy for this intermediate risk group of infant MLL+ ALL with high end-consolidation MRD levels.
In conclusion, our present analysis of a large cohort of unselected infants with MLL+ ALL included in the international Interfant-99 study demonstrated that the presence of an MLL rearrangement itself is not sufficient to warrant HSCT in CR1. However, because of the superior outcome of HSCT in CR1 compared with chemotherapy only in infant MLL+ ALL carrying further poor prognostic factors (ie, age < 6 months and either WBC counts ≥ 300 g/L at diagnosis or poor response to steroids at day 8), HSCT seems to be a valuable and recommendable option for this high-risk group of infants with ALL.
The publication costs of this article were defrayed in part by page charge payment. Therefore, and solely to indicate this fact, this article is hereby marked “advertisement” in accordance with 18 USC section 1734.
Acknowledgments
The authors thank all participating institutions, physicians, and nurses for their support of the study.
The Associazione Italiana Ematologia Oncologia Pediatrica was supported by the Associazione Italiana Ricerca sul Cancro (Regional Grant Code 1105; A.B., M.G.V.) and the international trial center by the Fondazione Tettamanti and Comitato ML Verga (M.G.V., P.D.L.). The Berlin-Frankfurt-Münster Study Group-Austria was supported by the St Anna Kinderkrebsforschung, Berlin-Frankfurt-Münster Study Group-Germany by the Deutsche Krebshilfe, the Czech Pediatric Haematology by the Czech Ministry of Education (grant MSM0021620813), and the Polish Pediatric Leukemia and Lymphoma Study Group (grant 2 P054 095 30) by the Polish Ministry of Science and Higher Education (T.S.).
Authorship
Contribution: R.P., M.S., G.M., and M.G.V. designed and planned the study; G.M., A.A., M.G.V., P.D.L., and R.P. wrote the manuscript; P.D.L. was in charge of data pooling and checking and statistical analysis; M.G.V. revised the data and also performed statistical analyses; C.P., I.H., G.D.R., M.F., B.L., T.L., T.S., A.F., G.J.-S., J.R., L.B.S., J.S., M.C., C.K.L., R.S., A.B., A.V., R.P., M.S., G.M., and A.A. were principal or coinvestigators in their study groups and institutions, coordinated the study in their countries, and recruited patients; and all authors read and approved the final version of the manuscript.
Conflict-of-interest disclosure: The authors declare no competing financial interests.
Correspondence: Georg Mann, St Anna Children's Hospital, Department of Pediatric Oncology and Hematology, Kinderspitalgasse 6, 1090 Vienna, Austria; e-mail: georg.mann@stanna.at; and Rob Pieters, Erasmus MC-Sophia Children's Hospital, Department of Pediatric Oncology and Hematology, Dr Molewaterplein 60, 3015GJ Rotterdam, The Netherlands; e-mail: rob.pieters@erasmusmc.nl.
References
Author notes
G.M. and A.A. contributed equally to this study.