Abstract
Abstract 3508
Allo-HCT is a therapeutic option for patients (pts) with relapsed or refractory B-cell non-Hodgkin lymphoma (B-NHL). However, the outcome of allo-HCT with a reduced-intensity conditioning (RIC) regimen for TL remains controversial, and no previous reports have compared the outcomes after allo-HCT for FL, TL, and DLBCL in the rituximab era.
We retrospectively analyzed 73 consecutive pts with FL (n=33), TL (n=18), or DLBCL (n=22) who received allo-HCT at our institute between January 2000 and December 2008. We defined TL as DLBCL that was histologically proven in pts with pre- (n=8) or co- (n=10) existing FL. The median age of the 73 pts was 47 years (range, 26–67). The median duration from diagnosis to HCT was 38 months (range, 6–175). The median number of prior chemotherapy regimens was 4 (range, 1–10): 57 pts (78%) had received prior rituximab, and 23 (32%) had received high-dose chemotherapy with autologous HCT prior to allo-HCT. The disease status at allo-HCT was CR or PR/refractory; 23 (32%)/50 (68%) for all pts, 10/23 for FL, 7/11 for TL, and 6/16 for DLBCL. The age-adjusted international prognostic index (aaIPI) at HCT was high or high-intermediate risk in 21 pts (28%), and FLIPI at HCT was high risk in 11 pts with FL (15%). The median level of serum albumin at HCT was 4.2 g/dL (range, 2.7–5.1). A myeloablative conditioning regimen was used for 14 pts (19%), and a RIC regimen was used for 59 pts (81%). The donor and stem cell source were related peripheral blood stem cells in 44 pts (60%), related bone marrow in 2 (3%), unrelated bone marrow in 21 (29%), and cord blood in 6 (8 %).
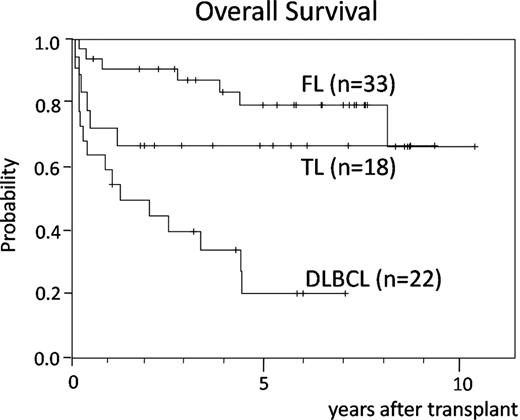
With a median follow-up of 68 months in surviving pts, the 5-year estimated overall survival (OS; Figure) and progression-free survival (PFS) were 58% and 54% for all pts, 80% and 71% for FL, 67% and 67% for TL, and 20% and 17% for DLBCL, respectively. The 5-year cumulative incidences of relapse/disease progression (PD) and non-relapse mortality were 25% and 39% for all pts, 10% and 22% for FL, 24% and 13% for TL, and 50% and 67% for DLBCL, respectively. Grade III-IV acute GVHD occurred in 25% of all pts, and OS was significantly worse in such pts [hazard ratio (HR) 2.5 (95%CI 1.2–5.3), p=0.02]. Extensive chronic GVHD (cGVHD) occurred in 53% of pts who survived 100 days or longer, and OS for patients with extensive cGVHD was significantly worse than that in pts without extensive cGVHD [HR 4.5 (1.3-15.6), p=0.02]. The cause of death included PD in 10 pts, GVHD in 5, infection in 4, non-infectious lung complication in 5, cerebral infarction or hemorrhage in 2, and unknown in 3. No pts with FL died of PD, and no pts with TL who had survived for 7 months after HCT relapsed thereafter. By a multivariate analysis, the OS for DLBCL was significantly worse than that of TL [HR 4.8 (1.7-13.2), p=0.002]. OS for FL was not significantly different from that of TL [HR 0.74 (0.2-2.4), p=0.6]. Other factors that influenced OS were aaIPI at HCT [high or high-intermediate risk, HR 3.7 (1.6-8.5), p=0.002] and the serum albumin level at HCT [<4 g/dL, HR 2.4 (1.1-5.5), p=0.03].
In the rituximab era, pts with TL showed more favorable outcomes after allo-HCT compared to those with DLBCL, and there was no significant difference in OS between FL and TL. AaIPI and the serum albumin level at HCT may be useful surrogate markers that influence OS for pts with B-NHL after allo-HCT. Allo-HCT, mainly with the use of a RIC regimen, might be a promising option for pts with relapsed or refractory FL and TL.
No relevant conflicts of interest to declare.

This icon denotes a clinically relevant abstract
Author notes
Asterisk with author names denotes non-ASH members.