Abstract
Background: Recent studies demonstrate an intriguing association between CMV reactivation and reduced risk of post-transplant AML relapse, yet mechanistic explanations remain elusive. Donor killer immunoglobulin-like receptor (KIR) genotypes have been associated with both AML and CMV clinical outcomes post allogeneic HCT. In this study we evaluated the CMV reactivation association with AML relapse risk, and the possible impact of donor KIR genotypes on the CMV-AML relapse relationship.
Patients/Methods: A consecutive case-series of 288 patients with AML who underwent allogeneic HCT between 1995 and 2011 at City of Hope were identified, patients were excluded who were not in remission at HCT, or received ex-vivo/in-vivo T cell depletion. A landmark analysis on 276 patients who survived without relapse for at least 55 days (this time point was selected given that the majority of CMV reactivations had occurred by this time, with very few relapse events). The median age was 49 years (range: 18 - 70). All patients were in 1st (n=229) or 2nd remission (n=47). Transplant conditioning included fully ablative (n=151) or reduced intensity regimens (fludarabine 125mg/m2 + melphalan 140mg/m2: n=125). Patients received peripheral blood hematopoietic stem cell (n=240) or bone marrow (n=36) grafts from matched sibling donors (n=190) or unrelated donors (8/8 match: n=86). Graft-versus-host disease prophylaxis consisted of a calcineurin inhibitor plus sirolimus or a short course of methotrexate. No patients in this cohort received prophylactic anti-CMV therapy. CMV was monitored by shell vial culture or polymerase chain reaction (PCR) once or twice a week from day +21 to day +100. Preemptive therapy with ganciclovir or foscarnet began when CMV reactivation was detected by positive culture or PCR. KIR genotyping was performed on donor DNA samples as previously described (Tissue Antigens, 2004;64:462) using 28 primers in 4 multiplex PCR reactions for detection of 14 functional KIR genes.
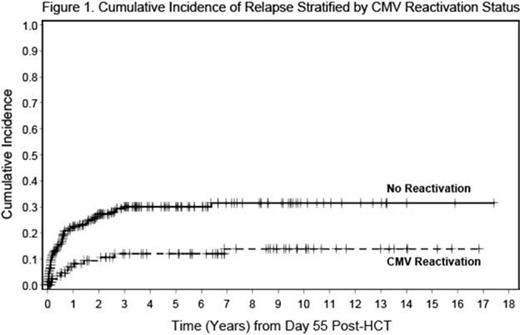
Results: CMV reactivation was observed in 85 of 276 patients (31%). The 5-year cumulative incidence of relapse was 30.2% (95% CI: 24.1 – 37.7%) in patients without CMV reactivation, significantly higher than in patients experiencing CMV reactivation (12.1%: 95% CI 6.7 – 21.6%, p=0.002) (Figure 1). Other clinical variables showing a significant association or p<0.10 by univariate analysis were: cytogenetic risk (high risk vs others: 37.6% vs. 20.0%, p= 0.01), transplant era (before or after 2005: 18.6% vs 28.0%, p=0.065), and conditioning (flu-mel vs others: 30.0% vs. 20.3%, p=0.095). In multivariate analysis, only CMV reactivation and high-risk cytogenetics were highly significant (Table 1). The association between CMV reactivation and reduced AML relapse was independent of the donor/recipient CMV serostatus.
We then examined the protective effect of CMV reactivation on relapse in subgroups of patients based on KIR genotypes (available in 251 cases). A significant protective effect on 5-yr relapse incidence (RI) was observed in the group with donor KIR B/X genotype (>1 activating KIR gene, n=164): 11.7% RI (95% CI 5.5 – 24.8) in patients with CMV reactivation vs. 29.5% (95% CI 22.0 – 39.6) in those without (p=0.016). No significant differences (p=0.3) in relapse were seen in the A/A genotype (only 1 activating KIR gene, n=87). Likewise, when we evaluated an activating KIR gene, 2DS1, which is reported to protect from AML relapse, the significant association was preserved in donors with 2DS1 (n=96): 11.5% RI (95% CI 4.0 – 33.4) in patients with CMV reactivation vs. 30.7% (95% CI 21.5 – 43.9) in those without (p=0.05). No significant relationship (p=0.12) between relapse and CMV reactivation was seen in donors without 2DS1 (n=155).
Conclusions: Our data confirm the earlier observation of a significant association between CMV reactivation and protection from AML relapse, and suggest that in patients with donor-derived activating KIRs, HLA-KIR interactions may augment the protection from AML relapse after CMV reactivation.
Landmark Analysis of Cumulative Incidence of Relapse Event = Relapse, Completing risk = non-relapse mortality
| Variables | Value | # of events | Hazard Ratio (95% CI) | p-value | |
| CMV Reactivation | No (n=191) Yes* (n=85) | n = 56 n = 11 | 2.6 (1.4 - 4.9) | 0.003 | |
| Cytogenetic Risk | Fav/Int/Unknown*(n=207) Unfavorable (n=69) | n = 42 n = 25 | 1.8 (1.1 - 2.9) | 0.018 | |
| * reference group, Fav - favorable, Int - intermediate | |||||
| Variables | Value | # of events | Hazard Ratio (95% CI) | p-value | |
| CMV Reactivation | No (n=191) Yes* (n=85) | n = 56 n = 11 | 2.6 (1.4 - 4.9) | 0.003 | |
| Cytogenetic Risk | Fav/Int/Unknown*(n=207) Unfavorable (n=69) | n = 42 n = 25 | 1.8 (1.1 - 2.9) | 0.018 | |
| * reference group, Fav - favorable, Int - intermediate | |||||
No relevant conflicts of interest to declare.
Author notes
Asterisk with author names denotes non-ASH members.