Abstract
Background: Venetoclax (VEN) is a selective, potent, orally bioavailable BCL-2 inhibitor FDA-approved for patients with del(17p) chronic lymphocytic leukemia (CLL) and who have received ≥1 prior therapy. Based on preclinical evidence of synergy, VEN plus rituximab is being assessed in an ongoing Phase 1b study.
Methods: Patients with relapsed/refractory (R/R) CLL received daily VEN with stepwise ramp-up over 3-4 weeks to reach daily doses of 200-600mg. After 1 week at the target dose, monthly rituximab was added for 6 doses. Responses and progression were assessed by iwCLL criteria with CT scan and bone marrow biopsy. Bone marrow assessments were done at screening, completion of combination therapy (month 7), and 2 months after clinical/radiologic criteria of iwCLL response were met. Minimal residual disease (MRD) was assessed in peripheral blood and marrow aspirates using ≥4 color flow cytometry (min sensitivity: 0.01%). Data cutoff was 04March2016, with analysis focusing on updated safety of cytopenias experienced on the course of treatment.
Results: Forty-ninepatients enrolled (48 CLL/1 SLL). Patients had received a median of 2 prior therapies (range: 1-5) and disease in 25 (51%) was considered refractory to the most recent therapy. Median time on study was 28 (<1-42) months, with 31 patients active on study. Eighteen patients discontinued: 11 due to disease progression, 3 due to toxicity (peripheral neuropathy [1], MDS [1], and death due to TLS [1]), 3 withdrew consent, and 1 was lost to follow up.
Across all doses, the most common AEs of any grade were diarrhea (57%), neutropenia (55%), upper respiratory tract infection (55%), and nausea (51%). Peripheral blood cytopenias were the most common Grade 3/4 AEs (neutropenia [53%], thrombocytopenia [16%], anemia [14%], febrile neutropenia [12%], and leukopenia [12%]).
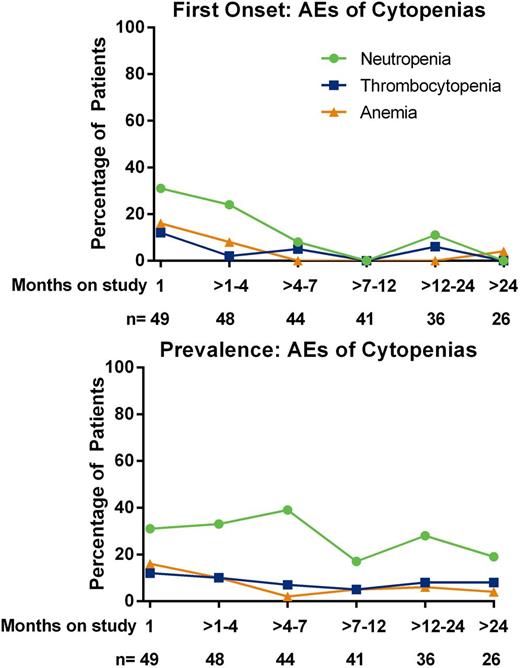
Twenty-seven (55%) patients had a history of neutropenia, of whom 6 were receiving G-CSF support prior to starting VEN. Overall, in the first month of therapy, 15 (31%) experienced an AE of neutropenia (any grade). Thereafter, the rate of new AEs of neutropenia decreased over time. While there was individual patient variability, mean ANC was stable over time. Overall, 26 (53%) patients had Grade 3/4 neutropenia. Neutropenia was generally well tolerated and managed by G-CSF support in 24 patients, in addition to ≥1 dose modification in 11 of the 24 patients. Of 8 (16%) patients who experienced grade 3 infections, 2 were while neutropenic. There were no grade 4 infections.
Among the 11 (22%) patients who developed any-grade thrombocytopenia, none occurred within 2 weeks of a reported bleeding-related AE. One patient had thrombocytopenia overlapping with disease progression on therapy.
Objective response rate for all patients was 86% (n=42), with 51% (n=25) who had complete response (CR/CRi; 12 achieved CR/CRi by month 7). At the completion of combination therapy (month 7), 39 patients had evaluable bone marrow assessments. Thirty (77%) had no histologic evidence of CLL in the bone marrow and 22 patients (56%) had attained bone marrow MRD-negativity. In longer follow up at any point during treatment for all 49 patients, 37 (75%) patients achieved complete marrow clearance and 28 (57%) achieved marrow MRD-negativity.
Conclusions: Transient manageable neutropenia was the most common AE, with first onset usually seen within the first month of treatment and the onset of new neutropenia AEs decreased over time. No patients discontinued the study due to cytopenias. Patients were able to continue on study and high rates of response to treatment were observed. VEN given with rituximab achieved rapid and profound reductions in disease burden in peripheral blood and bone marrow. 77% of evaluable patients achieved morphologic clearance by month 7, and 57% were MRD-negative at any point on study.
Brander:TG Therapeutics: Research Funding; Gilead: Honoraria. Roberts:AbbVie: Research Funding; Servier: Research Funding; Janssen: Research Funding; Genentech: Research Funding; Genentech: Patents & Royalties: Employee of Walter and Eliza Hall Institute of Medical Research which receives milestone payments related to venetoclax. Ma:Pharmacyclics, LLC, an AbbVie Company: Consultancy, Honoraria, Research Funding, Speakers Bureau; Janssen: Consultancy, Honoraria, Speakers Bureau; Gilead: Consultancy, Honoraria, Research Funding, Speakers Bureau; Genentech: Consultancy, Honoraria, Speakers Bureau; Novartis: Research Funding; Xeme: Research Funding; AbbVie: Research Funding. Lash:AbbVie: Employment. Verdugo:AbbVie: Employment, Other: may own stock. Zhu:AbbVie Inc.: Employment, Other: may own stock. Kim:AbbVie: Employment. Seymour:Roche: Consultancy, Honoraria, Membership on an entity's Board of Directors or advisory committees, Speakers Bureau; Takeda: Honoraria, Membership on an entity's Board of Directors or advisory committees; Janssen: Consultancy, Honoraria, Membership on an entity's Board of Directors or advisory committees, Research Funding, Speakers Bureau; Gilead: Consultancy, Honoraria, Membership on an entity's Board of Directors or advisory committees, Speakers Bureau; Celgene: Consultancy, Honoraria, Membership on an entity's Board of Directors or advisory committees, Speakers Bureau; Genentech: Consultancy, Honoraria, Membership on an entity's Board of Directors or advisory committees, Research Funding; AbbVie Inc.: Consultancy, Honoraria, Membership on an entity's Board of Directors or advisory committees, Research Funding, Speakers Bureau.
Author notes
Asterisk with author names denotes non-ASH members.