Abstract
Introduction
Evaluation of minimal residual disease (MRD) in multiple myeloma (MM) by multi-parameter flow cytometry (MFC) is a biomarker for risk of relapse. Applicability of MFC in routine practice has been challenging with suboptimal marrow samples and sampling needed at multiple time points. Sensitive serological assays which can detect MRD and have prognostic utility are needed to optimize the management of MM patients. The HevyliteTM assay (The Binding Site, UK) evaluates serum heavy/light chain ratios for IgG, IgA and IgM. We hypothesised the normalisation of serological markers is a good surrogate for plasma cell reconstitution in a healthy bone marrow (BM) microenvironment. The aim of this study was to prospectively compare Hevyliteand FreeliteTM assays with MFC of BM plasma cells from patients receiving autologous stem cell transplants (ASCT). We wanted to investigate if a correlation exists between MFC MRD negativity and the serological normalisation of Hevylite plus Freelite assays.
Methods
Hevylite, Freelite, SPEP, IFE on serum and MFC on bone marrow were performed on 23 patients post induction therapy and at a median of 90 days post-ASCT. Serological tests were performed again in available patients at 275 days post-ASCT. The combination of Freelite and Hevylite, which measures involved (iHLCr) and uninvolved (uHLCr) heavy light chain (HLC)-pairs, allows investigation of plasma cell reconstitution and its prognostic value in transplant patients. Six-colour MFC was performed as previously published (Rawstron et al. JCO 2013). IMWG uniform response criteria were used to categorise patients. Kaplan Meier estimates of Progression Free Survival (PFS) from time of transplantation until disease progression or death (whichever came first) were calculated and log-rank test was used for comparisons across groups. Sensitivity, specificity and ROC area analysis were used to assess performance of serologic response tests against flow MRD negativity, which is considered gold standard.
Results
Total of 23 patients were recruited to the study, 8 female (34.8%), 15 male (65.2%), with median age 61 (46-71). Isotype and ISS distribution were as follows; 11 IgG (47.8%), 4 IgA (17.4%), 1 IgM (4.35%), 7 LC only (30.4%) and 8 ISS1 (34.8%), 6 ISS2 (26.1%), 9 ISS3 (39.1%). Median marrow PC involvement at diagnosis was 45%, (20-90%) (N=18). At diagnosis, median LDH levels 192 IU/L, (153-475), median Hb 109.5 g/l, (72-152), with renal impairment noted in 6/23 (26.1%) and abnormal skeletal survey 15/23 (65.2%). High risk MM FISH was reported in 1/23 (4.35%), unknown 11/23 (47.8%) with rest determined to have standard risk. Median time from start of induction to HDM/ASCT 8 months (6.5-20) and median number of lines of treatment before HDM/ASCT was 1. Two deaths were noted on study. Median follow-up of surviving patients from diagnosis was 31 months (10-42). VGPR or better was achieved in 18/23 (88%) patients post-transplant by IMWG criteria.
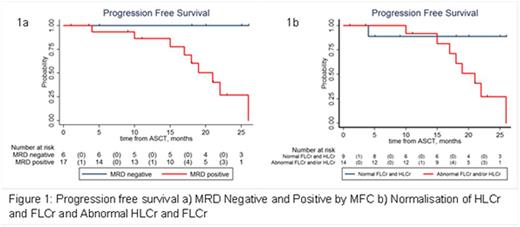
Hevylite ratio (iHLCr and uHLCr) normalised in 11/23 (48%) patients, with Freelite ratio (FLCr) normalisation in 14/23 (61%). MFC MRD negativity at 3 months post-ASCT was noted in 6/23 (26%) patients, in whom the post-ASCT Hevylite ratio and FLCr were also normalised. Comparing response assessments post-ASCT using standard IMWG criteria, MFC MRD, HLCr normalisation and FLCr normalisation, we found that MFC MRD is more sensitive to pick up residual disease over other tests. MFC MRD positivity correlates with early disease progression as MRD negativity significantly improves PFS outcomes (not reached vs 21 months) p=0.01 (Figure 1a). Patients with both HCLr and FLCr normalisation have significantly better PFS outcomes (not reached vs 21 months) p=0.04 (Figure 1b). ROC curve comparison of MFC MRD negativity and HLCr and FLCr normalisation tests, shows a 100% (95% CI 54.1% - 100%) sensitivity and 82% specificity (95% CI 56.6 - 96.2%) for serological normalisation. This demonstrates that HLCr and FLCr normalisation serves as a useful surrogate marker for MFC MRD negativity in our study.
Conclusions
We report the first prospective study demonstrating HLCr and FLCr normalisation post-transplant is a useful surrogate marker for flow MRD negativity, which is a widely accepted gold standard. This data requires further validation in a larger cohort of post-ASCT MM patients.
Ramasamy:Celgene: Honoraria, Research Funding.
Author notes
Asterisk with author names denotes non-ASH members.