Abstract
Background
Multiple Myeloma (MM) is an essentially incurable hematologic malignancy with the goals of therapy being disease control, improved quality of life, and prolonged survival.1,2 Despite improved survival with proteasome inhibitors and immunomodulatory agents, outcomes for patients with refractory disease, resistant to these classes of therapy, are poor. Daratumumab, an anti-CD38 antibody, is a commonly utilized therapy for relapsed/refractory multiple myeloma (RRMM) as a single agent based on the SIRIUS study which resulted in adequate response and acceptable safety profiles.3,4 Currently, it is approved in various combinations including with bortezomib. The approval of daratumumab in combination with bortezomib days 1, 4, 8, and 11 of a 21-day cycle was based on the CASTOR study which resulted in high response rates and acceptable safety profiles.5With the addition of bortezomib, additional toxicities in this RRMM setting may be a concern.6 Previous studies of bortezomib in RRMM patients have demonstrated that once-weekly bortezomib is equally as efficacious and better tolerated than the standard twice-weekly schedule, with a lower incidence of peripheral neuropathy and myelosuppression.8,9 However, there are currently no published reports of combining once-weekly bortezomib with daratumumab for patients with RRMM.
Methods
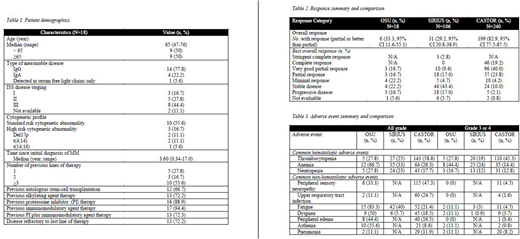
The present study sought to evaluate the progression-free survival (PFS) of daratumumab administered with once-weekly bortezomib for patients with RRMM. Secondary objectives included evaluation of overall survival (OS), overall response rate (ORR), time to response (TTR), and toxicity of once-weekly bortezomib with daratumumab. Eighteen patients were identified in an Institutional Review Board (IRB)-approved retrospective review of our institutional experience with daratumumab and once-weekly bortezomib. The median age of patients was 65 years (range 47 - 76, Table 1). Ten patients (55.6%) had three or more prior lines of therapy. Twelve patients (66.7%) had previous autologous stem cell transplantation. Sixteen patients (88.9%) had prior proteasome inhibitor (PI) therapy. Thirteen patients (72.2%) had disease refractory to their last line of therapy.
Results
The median PFS was 3.5 months. Median OS was not reached and TTR were undetermined due to the small sample size. The ORR was 33.3%, with 6 out of 18 patients experiencing an objective partial response or better (Table 2). Of those that responded, 4 patients (66.7%) remained on therapy at the time of data collection.The side effect profile was more tolerable, with less thrombocytopenia (27.8% all grade) and peripheral neuropathy (33.3% all grade) than previously reported (Table 3).
Conclusions
Daratumumab monotherapy was approved in heavily pretreated RRMM based on the SIRIUS trial showing promising efficacy and a favorable safety profile.4 The median PFS was 3.7 months compared to our PFS of 3.5 months. The combination of daratumumab with bortezomib administered twice weekly was approved based results from the CASTOR trial showing superiority of daratumumab in combination with bortezomib and dexamethasone over bortezomib and dexamethasone.5 As depicted in Table 2, our ORR of 33.3% is similar to the ORR of 29.2% in the SIRIUS trial, however differs greatly from 82.9% in the CASTOR trial.
While the present work is retrospective and hypothesis-generating, our results suggest that further prospective inquiry is necessary to determine the additional efficacy of adding once-weekly bortezomib to daratumumab.
Dempsey:Heron Therapeutics: Honoraria; TESARO: Honoraria.
Author notes
Asterisk with author names denotes non-ASH members.