Abstract
In B-cell chronic lymphocytic leukemia (B-CLL), defective apoptosis causes the accumulation of mature CD5+ B cells in lymphoid organs, bone marrow (BM), and peripheral blood (PB). These cells are the progeny of a proliferating pool that feeds the accumulating compartment. The authors sought to determine which molecular mechanisms govern the proliferating pool, how they relate to apoptosis, and what the role is of the microenvironment. To begin to resolve these problems, the expression and modulation of the family of inhibitor of apoptosis proteins (IAPs) were investigated, with consideration given to the possibility that physiological stimuli, such as CD40 ligand (CD40L), available to B cells in the microenvironment, might modulate IAP expression. The in vitro data on mononuclear cells from PB or BM of 30 patients demonstrate that B-CLL cells on CD40 stimulation express Survivin and that Survivin is the only IAP whose expression is induced by CD40L. Through immunohistochemistry, in vivo Survivin expression in lymph node (LN) and BM biopsies was evaluated. In reactive LN, Survivin was detected only in highly proliferating germinal center cells. In LN from patients with B-CLL, Survivin was detected only in pseudofollicles. Pseudofollicle Survivin+ cells were actively proliferating and, in contrast to Survivin+ B cells found in normal GC, were Bcl-2+. In B-CLL BM biopsies, CD5+, Survivin+ cells were observed in clusters interspersed with T cells. These findings establish that Survivin controls the B-CLL proliferative pool interfacing apoptosis and that its expression may be modulated by microenvironmental stimuli.
Introduction
B-cell chronic lymphocytic leukemia (B-CLL), the most common leukemia in the Western world, is characterized by the relentless accumulation of monoclonal mature CD5+ B cells in lymphoid organs, bone marrow (BM), and peripheral blood (PB).1 Virtually all circulating B-CLL lymphocytes are long-lived elements arrested in the G0/early G1 phase of the cell cycle,2 but focal aggregates of proliferating cells form the so-called pseudofollicles in lymph nodes (LN)3 and are scattered in the BM, which is a preferred site of relapse.4
The progressive rise of lymphocytes, despite the very low proportion proliferating cells, has led to the notion that B-CLL is primarily related to defective apoptosis.1 Genetic defects of the neoplastic cell and external stimuli may both influence the cell's abnormal behavior.5 Investigations on the intrinsic ability of B-CLL cells to avoid apoptosis have been mainly centered on the Bcl-2 gene family.6 Even if the t(14;18) translocation is exceedingly rare, the Bcl-2 gene product, which is the prototype antidote to apoptosis, is consistently overexpressed in B-CLL cells7,8 together with high levels of Mcl-1.9,10 The microenvironment likely plays a prominent role because the malignant cells progressively accumulate in vivo, whereas they rapidly undergo apoptosis when cultured in vitro. BM stromal cells11,12 and follicular dendritic cells13 may be involved in the natural history of the disease, but the most attractive candidates are T lymphocytes. Their numbers are increased in B-CLL patients, and activated CD4+ T cells strikingly predominate in BM and LN.14-16
All these considerations lead to the central issue of the disease. CLL cells accumulate because of defective apoptosis that causes extended survival. These cells are the progeny of a pool (albeit small) of proliferating elements that feed the downstream accumulating compartment. The questions are (1) which molecular mechanisms govern the proliferating pool, (2) how are patients interfaced with apoptosis, and (3) what, if any, is the role of the microenvironment. We have approached these problems by investigating the expression and modulation of the family of inhibitor of apoptosis proteins (IAPs)17 and by considering the possibility that physiological stimuli available to B cells in the microenvironment might modulate IAP expression.
IAPs were originally identified in baculoviruses18 and are highly conserved across species. Similar to their viral counterparts, expression of human IAP genes can inhibit apoptosis induced by a variety of stimuli. Six human IAPs have been described so far: NAIP,19 cIAP1, cIAP2,20 XIAP,21Survivin,22 and Apollon.23 They all appear to suppress apoptosis by caspase and procaspase inhibition,24therefore representing the last chance for a cell to escape its apoptotic fate. Recent evidence suggests that in vivo caspases are inactive in B-CLL cells, though they are functional when the cells are cultured in vitro.25 Therefore, it is conceivable to postulate a role for IAPs in maintaining the disease. Among IAPs, Survivin not only controls apoptosis but also participates in cell-cycle progression, thereby integrating apoptosis and cell division.26
As for microenvironmental stimuli, the presence of CD4+ T cells in involved BM and LN15 led us to focus on the interactions between the B-cell–associated molecule CD40 and its natural ligand (CD40L, CD154). CD40 belongs to the tumor necrosis factor (TNF) receptor superfamily,27 and its stimulation appears to rescue B-CLL cells from apoptosis and to induce proliferation.28,29 CD40L is a member of the TNF family that is expressed on activated T cells.30
Our experiments indicated that Survivin plays a role in the pathophysiology of B-CLL for the following reasons: (1) B-CLL cells, on CD40 stimulation, express Survivin; (2) Survivin is the only IAP whose expression is induced in B-CLL cells by CD40L; (3) in vivo Survivin+ cells are proliferating elements that coexpress Bcl-2 and are confined within the LN pseudofollicles and in clusters that gather in the BM, interspersed with T cells. These data provide a link between microenvironmental factors, here represented by CD4+ T cells, and the proliferation/apoptosis dilemma of B-CLL cells.
Patients, materials, and methods
Patients
We analyzed PB or BM from 28 patients with B-CLL and from 2 patients with B-prolymphocytic leukemia (B-PLL). Diagnosis was based on standard clinical and laboratory criteria, including cell morphology.31,32 All patients were studied either before or at least 3 months after chemotherapy. Patients were staged according to Rai.33 Table 1 summarizes the main clinical data of the patients.
We used tonsils, obtained as discarded tissues, from children undergoing tonsillectomy. Retrieval of all tissue samples followed the institutional guidelines at Ospedale Mauriziano Umberto I, Torino, Italy.
Cells
Mononuclear cells from PB, BM, and manually disaggregated tonsils were isolated by centrifugation through a Ficoll-Hypaque density gradient. Cells were washed with phosphate-buffered saline solution (PBS) and resuspended in RPMI 1640 medium supplemented with 10% heat-inactivated fetal calf serum (FCS; Life Technologies, San Giuliano Milanese, Milan, Italy), 2 mM L-glutamine, and 15 μg/mL gentamicin (complete RPMI, cRPMI). Cells were cultured in 6-well plates at a concentration of 1 × 106 cells/mL with or without 0.5 μg/mL trimeric human CD40L protein (Immunex, Seattle, WA). A fusion protein of CD40L and CD8α chain, was also used, kindly provided by Dr P. Lane (Oxford, United Kingdom).34 Mec1 and Mec2 cell lines35 were maintained in culture in cRPMI.
Flow cytometric analysis and cell sorting
Surface staining of cells was performed using the following monoclonal antibodies (mAbs): fluorescein isothiocyanate (FITC)–labeled anti-CD19 (Beckman Coulter Instrumentation Laboratory, Milan, Italy); phycoerythrin (PE)-labeled anti-CD5, anti-CD23, and anti-CD38 (Becton Dickinson Bioscience, Milan, Italy); and tricolor-labeled anti-CD19 (Caltag Laboratories, San Francisco, CA). Polyclonal FITC-conjugated rabbit antihuman IgM, IgG, IgA, and IgD, antihuman κ light chain, and polyclonal PE-conjugated rabbit antihuman λ light chain were purchased from Southern Biotechnology Associates, Birmingham, AL.
Intracellular staining was performed after fixation and permeabilization using the Fix & Perm kit (Caltag Laboratories) following the manufacturer's instructions. A mouse monoclonal antihuman Survivin (8E2 clone) was used (D. Altieri, unpublished data, January 2000). FITC-labeled goat antimouse immunoglobulin (SBA) was used as a secondary reagent.
Flow cytometric analysis and cell sorting were performed on a Facscalibur equipped with the sorter module using Cellquest research software (Becton Dickinson). Germinal center B cells were sorted from tonsils as CD19+ CD38+ IgD−elements, whereas CLL B cells were identified and sorted as CD19+ CD5+ cells.
RNA preparation and RT-PCR
Total RNA was extracted from 1 to 3 × 106 FACS sorted and unsorted cells and during the 7 days of culture using guanidinium thiocyanate method (RNAzol; Biotecx Laboratories, Houston, TX). The obtained RNA was reverse-transcribed into cDNA using 200 U Superscript II, Rnase H reverse transcription (Life Technologies Italia S.r.l., San Giuliano Milanese, Milan, Italy) and amplified by polymerase chain reaction (PCR). The PCR reaction was performed in 20 μL with 0.2 mM dNTPs, 1× GeneAmp buffer (PerkinElmer Italia, Monza, Italy), 0.5 U AmpliTaq DNA polymerase (PerkinElmer), and 10 pmol each specific primer for: cIAP1, forward 5′ GAA GAC ATC TCT TCA TCG AGG 3′; reverse 5′ CCA CAG GTG TAT TCA TCA TGA C 3′; cIAP2, forward 5′ TCC TAG CTG CAG ATT CGT TC 3′; reverse 5′ GGT AAC TGG CTT GAA CTT GAC 3′; NAIP, forward 5′ AGG GAA TTC ATG GCC ACC CAG CAG AAA 3′; reverse 5′CTC CTC GAG CAG TAA TTG AGA AAG TTC ACC 3′; XIAP, forward 5′ GGG AAT TCA TGA CTT TTA ACA GTT TTG AAG GAT 3′; reverse 5′ CTC TCG AGC ATG CCT ACT ATA GAG TTA GA 3′; Survivin, forward 5′CTCTACATTCAAGAACTGGCC3′; reverse 5′TTGGCTCTTTCTCTGTCCAG3′.
Cycling conditions were as follows: 1 cycle at 94°C for 2 minutes, 35 cycles at 94°C for 45 seconds, annealing temperature for 45 seconds (54°C for cIAP1, cIAP2, and Survivin and 52°C for NAIP and XIAP), 72°C for 45 seconds, and a final extension at 72°C for 10 minutes. Amplified products were resolved by electrophoresis on a 1.5% agarose gel.
Quantitative assessment of apoptosis
Binding of Annexin V-FITC was used to follow phosphatidylserine exposition on early apoptotic cells. Staining was performed according to the manufacturer's instructions using the Annexin V-based apoptosis detection kit (R&D Systems, Flanders, NJ). Briefly, 10 × 105 cells were incubated with saturating concentrations of Annexin V-FITC for 15 to 30 minutes at room temperature and were immediately analyzed on a Facscalibur (Becton Dickinson).
Cell-cycle analysis
Determination of the percentage of B-CLL cells at each stage of the cell cycle was made by an assessment of DNA content after staining with propidium iodide using DNA con3 kit (Consul T.S., Rivalta, Italy) according to the manufacturer's instructions. Propidium iodide incorporation was analyzed using a Facscalibur instrument (Becton Dickinson) equipped with the doublet discriminator module.
Western blotting
Whole cell protein extracts were prepared from 3 × 106 cells cultured with or without soluble CD40L using a lysis buffer containing 10 mM Tris-HCl (pH 7.6), 5 mM EDTA, 50 mM NaCl, aprotinin (5 μg/mL), pepstatin (1 μg/mL), soybean trypsin inihibitor (2 μg/mL), 1 mM phenylmethylsulfonyl fluoride, and 1% NP40 (Sigma).
Cell lysates were separated by 12% gels in sodium dodecyl sulfate–polyacrylamide gel electrophoresis (SDS-PAGE), transferred onto polyvinylidene difluoride (Bio-Rad, Hercules, CA), and blocked in TTBS and milk 3% or in PBS and BSA 5% overnight. Immunoblottings were performed using mAb against Survivin (mouse mAb 1μg/mL; R&D Systems, Minneapolis, MN), Bcl-X (1:1000 rabbit polyclonal antiserum; Transduction Laboratories, Lexington, KY), Bcl-2 (mouse mAb 1:1500; DAKO, Glastrup Denmark), and Mcl-1 (mouse mAb 1:1000; Transduction Laboratories).
Horseradish peroxidase–antimouse IgG (1:3000; Promega, Madison WI) and horseradish peroxidase–antirabbit IgG (1:5000, Promega) were used as secondary reagents. All immunoblots were revealed by enhanced chemiluminescence (Amersham, Buckinghamshire, United Kingdom).
Immunohistochemistry
Five-micrometer tissue sections of 4 reactive lymph nodes, 4 lymph nodes with diffuse infiltration of B-CLL, and 2 bone marrow trephine biopsies with heavy infiltration of B-CLL were cut on slides covered with adhesive. Sections were deparaffinized, and endogenous peroxidase was quenched with 1.5% hydrogen peroxidase in methanol (10 minutes). A series of antibodies was applied to characterize B-CLL cells (CD20, CD79a, CD5, CD23) and reactive T cells (CD3, CD8). All reagents were purchased from DAKO. Serial sections of the same cases were also immunostained with antibody recognizing molecules involved in cell proliferation, cell-cycle regulation, or apoptosis. These mAbs included anti–Bcl-2 (Ab124; DAKO), anti-p27kip1 (Transduction Laboratories), and anti–Ki-67 (MIB-1; DAKO). All sections were subjected, before immunostaining, to antigen retrieval (citrate buffer, pH 6.0) and developed using a sensitive avidin-streptavidin-peroxidase technique with semi-automated cell staining systems (Optimax; Biogenex, San Ramon, CA) and standardized procedures.
For immunohistochemical analysis of Survivin, antigen retrieval was performed in a pressure cooker containing 1.5 L of 9 mM citrate buffer, pH 6.0, that had been brought to boil. The lid was secured, and heating was continued for approximately 6 minutes, until the pressure valve released. After gentle washing with water, slides were washed with PBS, pH 7.0. Staining was performed with mouse monoclonal antihuman Survivin (8E2 clone; D. Altieri, unpublished data, January 2000). Antibody was applied at a concentration of 0.5 mg/mL in PBS, pH 7.0, containing 0.5% BSA and 5% normal goat serum (Vector Laboratories) and incubated overnight at 4°C in a moist chamber. After washing with PBS, the slides were treated with an immunoperoxidase detection system (ABC kit; Immunotech, Marseille, France), according to the manufacturer's instructions, using 3,3′-diaminobenzidine as the chromogen. After immunostaining, the slides were lightly counterstained with hematoxylin and then cover-slipped.
Results
IAP expression in freshly isolated B-CLL cells
We analyzed mononuclear cells from PB or BM of 30 patients, 28 with B-CLL and 2 with B-PLL (Table 1). B-CLL cells coexpressed CD19, CD5, and CD23 and had weak surface immunoglobulin expression. B-PLL cells had a CD19+, CD5−, CD23− phenotype and expressed bright surface immunoglobulin. In agreement with published studies,9 10 Western blot analysis revealed that all the patients had high levels of Bcl-2 and Mcl-1 and low levels of Bcl-xL (data not shown).
The percentage of leukemic B cells ranged between 90% and 95% of mononuclear cells. In 5 patients with CLL, CD19+, CD5+ cells were also FACS-separated to a purity level greater than 97%. The expression of cIAP1, cIAP2, NAIP, XIAP, and Survivin was assessed by RT-PCR on both sorted and unsorted samples, and the results were identical.
cIAP1, cIAP2, NAIP, and XIAP were consistently positive in all samples. On the contrary, Survivin expression was undetectable in most patients (25 of 30, 83%). In the remaining 5 patients (patients 5, 8, 9, 18, 25; Table 1) and in 2 CLL cell lines (MEC1 and MEC233), Survivin mRNA was readily amplifiable. This evidence was confirmed at the protein level by cytofluorometric and Western blot studies (Figures1A, 2). Cell-cycle analysis of some patients (Figure3A) revealed that the proportion of cycling cells was more pronounced than in Survivin+patients. Although the number of patients is too small to allow clinical correlation, it is worth mentioning that all 5 Survivin+ patients had active disease, according to National Cancer Institute criteria,36 and required treatment. One of them (patient 9; Table 1) had B-PLL. In all the other patients a proportion of larger, atypical cells, ranging between 20% and 40%, was observed in PB smears. On the contrary, only 4 of the remaining 25 patients who did not constitutively express Survivin had active disease requiring treatment.
Cytofluorometric analysis of Survivin expression.
Staining with mAb anti-Survivin at day 0 (A) and after 3 days of culture (B) of cells from 3 B-CLL patients, representative of the following groups: CD40L nonresponders (patient 16, Table 1); CD40L responders (patient 3, Table 1); patients whose cells were already Survivin+ at day 0 (patient 5, Table 1).
Cytofluorometric analysis of Survivin expression.
Staining with mAb anti-Survivin at day 0 (A) and after 3 days of culture (B) of cells from 3 B-CLL patients, representative of the following groups: CD40L nonresponders (patient 16, Table 1); CD40L responders (patient 3, Table 1); patients whose cells were already Survivin+ at day 0 (patient 5, Table 1).
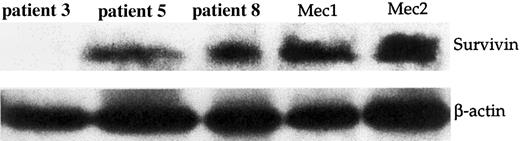
Western blot analysis of cells and cell lines of B-CLL patients.
B-CLL cells were lysed and analyzed by SDS-PAGE and Western blotting using anti-Survivin mAb (top). Anti–β actin polyclonal antiserum (bottom) was used as control. Samples at diagnosis from 1 Survivin− (patient 3) and 2 Survivin+(patients 5 and 8) B-CLL patients are shown. Mec1 and Mec2 cell lines, grown in log phase, were used as controls. 3 × 106 cell equivalents per test were used.
Western blot analysis of cells and cell lines of B-CLL patients.
B-CLL cells were lysed and analyzed by SDS-PAGE and Western blotting using anti-Survivin mAb (top). Anti–β actin polyclonal antiserum (bottom) was used as control. Samples at diagnosis from 1 Survivin− (patient 3) and 2 Survivin+(patients 5 and 8) B-CLL patients are shown. Mec1 and Mec2 cell lines, grown in log phase, were used as controls. 3 × 106 cell equivalents per test were used.
Survivin expression correlates with the proliferative status of the cells.
Cell-cycle analysis of patient cells at day 0 (A) and after 3 days of culture with CD40L (B) in a CD40L nonresponder (patient 16, Figure 1), in a CD40L responder (patient 3, Figure 1), and in a patient already Survivin+ at day 0 (patient 5, Figure 1). PI, propidium iodide.
Survivin expression correlates with the proliferative status of the cells.
Cell-cycle analysis of patient cells at day 0 (A) and after 3 days of culture with CD40L (B) in a CD40L nonresponder (patient 16, Figure 1), in a CD40L responder (patient 3, Figure 1), and in a patient already Survivin+ at day 0 (patient 5, Figure 1). PI, propidium iodide.
Survivin expression in CLL cells is modulated by CD40 engagement
We next investigated the in vitro behavior of CLL cells. As expected, these cells started undergoing spontaneous apoptosis after 24 hours of culture in conventional medium. To assess the effect of CD40 stimulation, we set up time-course experiments with cells cultured in the presence or absence of human soluble CD40L. Viability and proliferation were tested every 24 hours up to 7 days.
Two different populations of patients were observed: CD40L responders and CD40L nonresponders. In 15 of 22 (68%) studied patients (Table 1; patients 1-22), CD40L stimulation reduced the entity of spontaneous apoptosis and improved cell viability by 20% to 38% after 48 to 96 hours of culture. These patients were considered CD40L responders. The entity of response was identical irrespective of whether the cells were exposed to monomeric or trimeric soluble CD40L. The increased viability (Figure 4) resulted in a higher number of cells in stimulated versus control cultures. The increase in the proportion of proliferating cells, evaluated on the basis of DNA content assay after 3 days of CD40 stimulation, ranged between 0.5% and 5.3% (Figure 3B) compared to unstimulated controls, indicating that a number, albeit small, of B-CLL cells entered the cell cycle in response to CD40 ligation. The remaining patients (7 of 22, 31%) were considered CD40L nonresponders because both viability and proliferative activity of cultured cells were unmodified after stimulation.
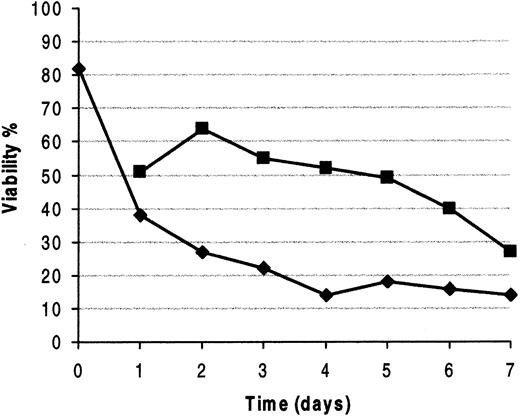
Viability of B-CLL cells is improved by CD40 engagement.
Time-course experiment of a representative CD40L responder patient whose cells were cultured in the presence (▪) or the absence (♦) of CD40L. Viability was assessed by cytofluorometric analysis of Annexin-V staining at the indicated time points (days).
Viability of B-CLL cells is improved by CD40 engagement.
Time-course experiment of a representative CD40L responder patient whose cells were cultured in the presence (▪) or the absence (♦) of CD40L. Viability was assessed by cytofluorometric analysis of Annexin-V staining at the indicated time points (days).
Even if the number of patients studied is too small to draw any statistically significant clinical correlation, we evaluated the possibility that the response to CD40L might be related to a number of known clinical parameters. The response to CD40L did not correlate with stage or duration of disease, nor did it correlate with previous treatments. Also unrelated were disease activity, evaluated according to NCI guidelines,36 the number of atypical cells in PB smears, and the immunoglobulin isotype of the malignant clone (Table1). Given that it has been shown that B-CLL patients can be divided into 2 groups with different prognoses on the basis of CD38 expression,37 we also evaluated the possibility of a correlation between the expression of CD38 on the cell surface and the response to CD40L. As shown in Table 1, no correlation was observed. No modification in the expression of Bcl-2, Mcl-1, and Bcl-xLproteins were observed in either CD40L responders or nonresponders (data not shown).
We then evaluated the possibility that IAP expression in B-CLL might be modulated by CD40L stimulation. The expression of cIAP1, cIAP2, NAIP, and XIAP remained unmodified in both CD40L responders and CD40L nonresponders. On the contrary, Survivin expression was up-regulated after 48 to 96 hours of CD40 engagement in all CD40L responders. Up-regulation was first observed by RT-PCR (Figure5) and then confirmed at protein level by cytofluorometric analysis (Figure 1B) and Western blot (data not shown). Cells of patients who were already Survivin+ at day 0 maintained Survivin positivity throughout the culture period if they were exposed to CD40L (Figure 1B). In the tested patients, Survivin expression was irreversibly lost shortly after the beginning of in vitro culture if the cells were cultured in medium alone. No modulation of Survivin expression was observed in the cells of the 7 CD40L nonresponders cultured for up to 7 days in the presence or absence of CD40L.
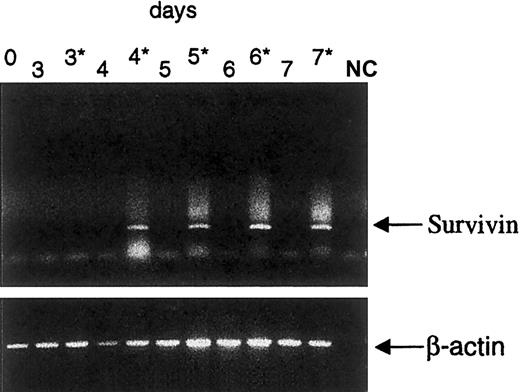
Survivin expression is induced by CD40 stimulation.
RT-PCR analysis of Survivin expression in cells from a representative CD40L responder patient cultured in the presence (3*-7*) or the absence (0-7) of CD40L at the indicated time points (days). NC, negative control.
Survivin expression is induced by CD40 stimulation.
RT-PCR analysis of Survivin expression in cells from a representative CD40L responder patient cultured in the presence (3*-7*) or the absence (0-7) of CD40L at the indicated time points (days). NC, negative control.
Survivin expression in CLL lymph nodes and bone marrow
As in vitro data were ascribing a role to Survivin, we evaluated its in vivo expression in LN and BM biopsies by immunohistochemical analysis. In reactive LN, Survivin was detected only in highly proliferating germinal center (GC) cells (Figure6A-B). Immunohistochemical data were confirmed by RT-PCR analysis on FACS-purified GC cells (data not shown).
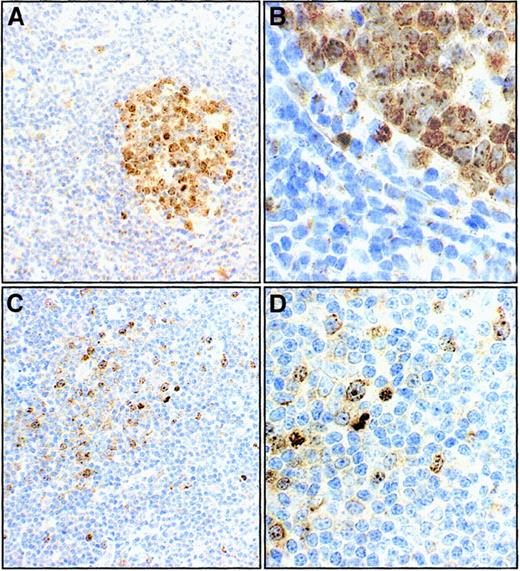
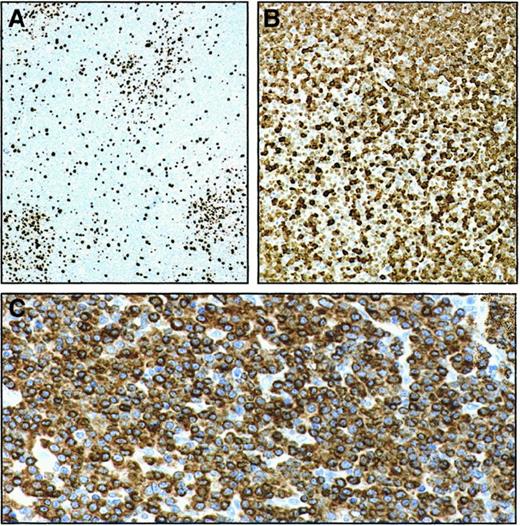
Survivin expression in reactive and B-CLL lymph nodes (immunoperoxidase staining).
In reactive lymph node follicles, only germinal center cells are Survivin+ (A and B at 100 × and 400 × magnifications in a case representative of the 4 studied). In a B-CLL lymph node completely effaced by malignant cells, a minority of cells, which are located in pseudofollicles, stain with anti-Survivin antibody (C and D, at 100 × and 400 × magnifications in a case representative of the 4 studied).
Survivin expression in reactive and B-CLL lymph nodes (immunoperoxidase staining).
In reactive lymph node follicles, only germinal center cells are Survivin+ (A and B at 100 × and 400 × magnifications in a case representative of the 4 studied). In a B-CLL lymph node completely effaced by malignant cells, a minority of cells, which are located in pseudofollicles, stain with anti-Survivin antibody (C and D, at 100 × and 400 × magnifications in a case representative of the 4 studied).
Lymph nodes from 4 patients with B-CLL were examined, and the findings were consistent and reproducible. In B-CLL LN, Survivin was detected only in pseudofollicles (Figure 6C-D). Pseudofollicle Survivin+ cells were actively proliferating, as documented by the Ki67-positivity (Figure 7A). At the same time they were uniformly and intensely Bcl-2+(Figure 7B), indicating a remarkable resistance to undergo apoptosis. Only few elements in pseudofollicles expressed the cyclin kinase inhibitor p27kip1 (Figure 7C). The overwhelming majority of malignant cells invading LN outside pseudofollicles were p27kip1+, Bcl2+ but Survivin−, Ki67−(Figures 6, 7).
Serial section analysis of pseudofollicles in B-CLL lymph node (avidin-streptavidin-peroxidase staining with different combinations of mAbs).
In the same lymph node examined in Figure 6C-D, pseudofollicles contain numerous Ki-67 (ie, proliferating) cells (100 × magnification) (A). Few p27kip1+ cells are observed in a corresponding area on serial sections (100 × magnification) (B), whereas virtually all cells are intensely Bcl-2+ (200 × magnification) (C).
Serial section analysis of pseudofollicles in B-CLL lymph node (avidin-streptavidin-peroxidase staining with different combinations of mAbs).
In the same lymph node examined in Figure 6C-D, pseudofollicles contain numerous Ki-67 (ie, proliferating) cells (100 × magnification) (A). Few p27kip1+ cells are observed in a corresponding area on serial sections (100 × magnification) (B), whereas virtually all cells are intensely Bcl-2+ (200 × magnification) (C).
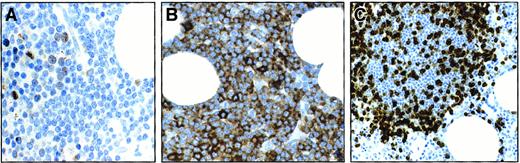
In the 2 B-CLL BM biopsies analyzed, CD5+, Survivin+ large cells were observed in sparse clusters amid a preponderance of CD5+, Survivin− smaller elements (Figure 8A-B). The presence of high numbers of T cells was evident in all LN and BM samples studied (Figure 8C).
Serial sections from a B-CLL BM biopsy infiltrated with CD5+ B-CLL cells (immunoperoxidase staining with different combinations of mAbs).
Clusters of Survivin+ cells are observed (A), scattered within a nodule of CD5+ malignant B lymphocytes (B). A large proportion of CD3+ T lymphocytes is interspersed in the same nodule (magnification A, B, C 200 ×) (C).
Serial sections from a B-CLL BM biopsy infiltrated with CD5+ B-CLL cells (immunoperoxidase staining with different combinations of mAbs).
Clusters of Survivin+ cells are observed (A), scattered within a nodule of CD5+ malignant B lymphocytes (B). A large proportion of CD3+ T lymphocytes is interspersed in the same nodule (magnification A, B, C 200 ×) (C).
Discussion
The salient feature of B-CLL natural history is the in vivo accumulation of monoclonal resting B cells. Several defects in the induction of apoptosis, including the overexpression of Bcl-2 and Mcl-1,8 9 concur to create an accumulation compartment that progressively enlarges. More generally, the overall pattern of the expression of the Bcl-2 gene family favors the extended survival of B-CLL cells. On these grounds, B-CLL is considered a malignancy whose destiny is decisively influenced by absent or defective apoptosis.
This interpretation has to be consistent with the obvious need for a proliferative compartment that supplies the accumulation compartment and with the contention that the B-CLL cell genetic abnormalities do not entirely account for all aspects of cell accumulation. The microenvironment presumably exerts a strong influence in vivo as malignant cells very rapidly undergo apoptosis once cultured in vitro. In this work, we demonstrate that Survivin expression in resting B-CLL cells is induced in vitro by CD40 stimulation, that Survivin is the only IAP whose expression is modulated by CD40L, and that in vivo Survivin+ cells are localized in LN pseudofollicles and in rare BM clusters interspersed with T cells. Survivin+ cells proliferate and, at the same time, express Bcl-2. These findings establish 2 major points. First, they indicate that Survivin has an important role in controlling the B-CLL proliferative pool and its ability to nourish the accumulation compartment. Second, they demonstrate that Survivin expression may be modulated by microenvironmental stimuli. A further ancillary point is that the constitutive expression of the antiapoptotic proteins NAIP, cIAP1, cIAP2, and XIAP by B-CLL cells circulating in the PB may contribute to their accumulation.
Survivin is a protein that prevents apoptosis by blocking caspase activity.38 Furthermore, it is expressed in the G2/M phase of the cell cycle, where it associates with the mitotic spindle microtubules.26 It has been suggested that caspase activity occurs during each cell cycle and that Survivin functions to block this activity.39 In fact, Survivin forms a supramolecular assembly together with caspase-3 and the cyclin-dependent kinase inhibitor p21waf1 within centrosomes,40 thereby preventing apoptosis and preserving p21waf1 integrity during normal mitotic progression.40 In this way, Survivin interfaces cell survival and cell proliferation. By immunostaining reactive LN, we demonstrate that in normal lymphoid tissues, the expression of Survivin is concentrated in GC that represent the B-cell proliferation compartment of lymphoid follicles41 (Figure 6). This observation fits very well with the intense Survivin positivity observed in highly aggressive lymphomas of GC origin.22 In B-CLL the proliferating pool is located in LN pseudofollicles, where proliferating B-CLL cells coexpress both Survivin and Bcl-2 (Figures 6, 7). This is in striking contrast with normal GC cells that are Bcl-2−.42 Thus, pseudofollicle-proliferating B-CLL cells differ from normal GC cells because they have lost the possibility to undergo apoptosis and are bound to accumulate. The overwhelming majority of LN B-CLL cells are Bcl-2+, p27kip1+ but Survivin−, Ki-67−. Although it remains to be established which mechanisms control the switch-off of Survivin expression in the accumulating compartment, we have acquired information about the mechanisms that control the re-expression of Survivin in cells hidden within the Survivin− accumulation compartment. In vitro we mimicked the stimulus provided in vivo by activated T cells by using soluble CD40L. Our data demonstrate that the stimulation of CD40 is able to induce Survivin expression in B-CLL cells obtained from PB or BM (Figure 5). Therefore, the observation that clusters of Survivin+ cells are detected in the BM (Figure 8), which is a privileged site of disease localization and relapse, and are interspersed with T cells stands as an interesting link between in vitro and in vivo data. This finding is clearly consistent with the notion that many activated CD4+ T cells are present in tissues involved by B-CLL.15
It may be asked why not all patients with B-CLL respond to CD40L stimulation. There are several possible answers. First, our in vitro stimulus may not be strong enough to detect all responsive cells. The number of circulating malignant cells inducible by CD40L may be variable, so that some occurrences are easily disclosed while others remain unnoticed. Second, CD40L might be one of a number of favoring microenvironmental stimuli. Other stimuli, perhaps provided by BM stromal cells12 or follicular dendritic cells,13 may be involved. Third, the term B-CLL probably does not indicate a single homogeneous disease but may cover a wider spectrum of disorders with different stimuli requirements. It has been shown that the presence of somatic mutations of IgV genes and of high percentages of CD38+ cells defines 2 groups of patients with B-CLL with significantly different prognoses.37,43 In this small series, the ability to respond to CD40L does not correlate with the expression of CD38 (Table1) nor (P. Ghia et al, unpublished results, March 2000) with the presence or absence of immunoglobulin somatic mutations, and it remains to be established whether the responsiveness or unresponsiveness to CD40L may define more subclasses of CLL. Forthcoming clinical studies on a larger series of patients will address this issue and the issue of whether the constitutive expression of Survivin has a clinical correlate, and they may identify a subset of patients with a more aggressive form of the disease as recently shown in diffuse large B-cell lymphomas.44
Taken together, the data obtained lead to a model of B-CLL growth and expansion in which a small proliferating pool within LN pseudofollicles is governed by the expression of Survivin. These cells are bound to accumulate because they also express Bcl-2. They leave the pseudofollicle mircroenvironment, down-regulate Survivin expression, and stop proliferating. During their long lifespans, they circulate and may easily reach the BM, a privileged site of disease relapse and a sanctuary for CD4+ T cells. In the BM, microenvironmental stimuli such as the CD40 stimulation provided by activated CD4+ T cells may recruit Survivin− B cells hidden in the accumulating compartment, persuade them to re-express Survivin, and perpetuate a vicious circle. According to this model, microenvironmental stimuli, namely those provided by T cells, help to propagate the disease and give ample justification to treatment approaches with purine nucleoside analogues45 or monoclonal antibodies such as Campath 1H,46 which, because they are able to damage both B and T cells, interrupt the interactions between malignant B cells and microenvironmental bystander nontumoral cells. Understanding the mechanisms that allow the progeny of LN pseudofollicles to switch off Survivin expression will give therapeutically useful information; the presence of circulating cells that retain Survivin positivity is associated with a higher proliferative activity (Figure 3) and might lead to a more aggressive clinical behavior. Identifying molecules that disrupt Survivin-caspase interactions47 can provide a new way of eradicating B-CLL by promoting the elimination of the proliferating pool.
We thank Prof P. C. Marchisio (DIBIT, Milan, Italy) for helpful discussions and Prof D. Altieri (Yale University, New Haven, CT) for providing the antihuman Survivin antibodies.
This study was supported in part by research funding from AIRC to F.C.C. and M.C. and by MURST 40% to F.C.C.
L.G. and P.G. contributed equally to this work.
The publication costs of this article were defrayed in part by page charge payment. Therefore, and solely to indicate this fact, this article is hereby marked “advertisement” in accordance with 18 U.S.C. section 1734.
References
Author notes
Federico Caligaris-Cappio, University Division of Clinical Immunology and Hematology, Ospedale Mauriziano Umberto I, Largo Turati 62, 10128 Torino, Italy; e-mail:fcaligaris@mauriziano.it.