Abstract
Introduction: Myeloablative allogeneic stem cell transplantation in patients (pts) with MCL has been traditionally used only in young pts without co-morbidities due to its high toxicity. During the last 10 years, many different reduced intensity conditioning (RIC) regimens have been introduced into clinical practice trying to reduce this toxicity, preserving the establishment of a meaningful graft-tumor effect (GVT). However, few homogeneus pts series have been reported focused on MCL, with encouraging results in some studies. Thus, we report herein the outcome of 18 consecutive MCL pts who received an allo-PBSC-RIC from an HLA-identical sibling donor with a long follow-up.
Patients and methods: The RIC consisted in iv fludarabine 125–150 mg/m2 from day-8 to -4 and iv melphalan 80 or 140 mg/m2 on day-3 to -2. Rituximab 375 mg/m2 was added to RIC in 8 pts on days-9, +1, +8 and +15. GVHD prophylaxis consisted in standard cyclosporine and methotrexathe. Gradual cyclosporine tappering from day +50 was initiated if mixed chimerism or persistent disease were present. We focus on engraftment kinetics, early toxicities, non-relapse mortality (NRM), chimerism kinetics, GVHD as well as estimated anti-tumoral efficacy, progression-free and overall survival (PFS and OS).
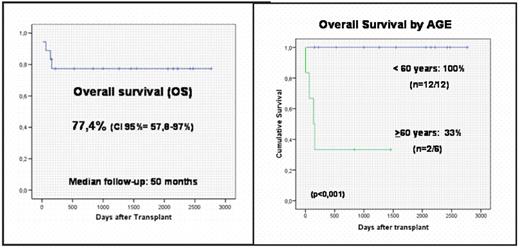
Results: 18 MCL pts were included from 2000 to 2008, with a median follow-up of 50 months. Median age was 56 years (range: 43–68), 13 were males, with a median pre-RIC treatment lines of 2 (1–4) including 2 autoHSCT. Before alloRIC, 13 pts (72%) were in 1st or later CR, while 5 pts (28%) were in chemo-sensitive PR. Median CD34+/kg infused cells were 5,8 ×106 (4,3–10,8) and 2,0 ×108 (0,7–4,1) CD3+ lymphocytes/kg. All pts engrafted, reaching ANC>500 on day +16 (13–20) and platelets>20.000 on day +12 (8–32), with no graft failures. Early toxicity (<day +100) included WHO grade 3–4 mucositis in 8 (44%), febrile neutropenia in 6 (33%) and bacterial infections in 4 (22%) with 2 deaths (1 varicella-zoster encephalitis and 1 refractory acute GVHD). There were 2 other deaths during the 1st year, both due to infections in the setting of extensive chronic GVHD, for a 1-year NRM of 22%. Complete donor T-cell chimerism (CC) was present at day +30 in 71% of evaluated pts and in 100% pts at day +90. Acute grade II–IV GVHD ocurred in 39% of pts at risk, with 17% of grade III–IV. Chronic GVHD affected 12/16 pts (75%), wich was extensive in 6 (38%). Only 1 patient (trasplanted in PR after 2 treatment lines) relapsed (6%). The 5-year estimated PFS and OS were both 77% (CI95%=58–97%) and 14 pts remain alive in CR. The only apparent prognostic factor in our study is age: 8 pts aged 60 or older have an OS of 33,3% vs 100% for the 10 pts younger than 60 years (p<0.001).
Conclusions: AlloRIC with fludarabine and melphalan in MCL pts offers a good toxicity profile, with high engraftment rate and good long term disease-free survival, especially in pts younger than 60. The very low long-term relapse rate seen in the context of a high incidence of chronic GVHD supports the continued sensitivity of MCL to a GVT effect.
Disclosures: No relevant conflicts of interest to declare.
Author notes
Corresponding author

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal