Abstract
Abstract 2547
Minimal residual disease (MRD) eradication in patients with chronic lymphocytic leukemia (CLL) treated by standard chemo-immunotherapy regimens correlates with improved outcome. However, there is limited information about the interest of negative MRD after allogeneic stem cell transplantation (allo-SCT). In this study we investigated whether blood phenotypic remission could impact post-transplant outcome in patients with CLL.
We retrospectively included patients who underwent allo-SCT for CLL and with post-transplant MRD monitored by four or six-colour flow cytofluorometry in blood samples (sensitivity≥10−4). Prognostic impact was evaluated on overall survival (OS) and progression-free survival (PFS). Each of these parameters was evaluated according to the best response and to the 12 month-MRD status, using log-rank test.
Thirty-three patients from 4 hematology departments were included. Median age at transplant was 54 years (range, 41 to 66 years). The median number of prior chemotherapy regimens was 3 (range, 1 to 6) including autologous stem cell transplantation in 48% of the patients. Status at transplant was available in 27 patients and 11% of them had negative MRD, 26% haematological complete response (CR), 59.% partial response (PR) and 4% had refractory disease. Twenty-two patients (67%) received a reduced intensity conditionning regimen. Conditioning regimen included serotherapy (antithymoglobulin n = 10, alemtuzumab n = 1, rituximab n = 1) in 12 patients. Twenty-two patients (67%) were transplanted with HLA identical sibling donor. The median number of MRD evaluations after transplant was 5 (range, 1 to 23). Response to transplant: After transplant, 16 patients achieved negative MRD, 15 patients achieved haematological CR, 1 PR and 1 did not respond to transplant. Among the 16 patients with phenotypic remission, negativation of MDR was obtained before the cessation of immunosuppressive therapy for 15 of them (94%) and median time to negativation was 7 months (range, 2 to 20 months). In patients achieving phenotypic remission chronic GVHD rate was 75% versus 44% in patients with post-transplant detectable MRD. Post-transplant outcomes: With a median follow-up of 27 months, the 2-y OS and the 2-y PFS were respectively 84% and 53%. Cause of death (n = 8) was progression in 4 cases and transplant related mortality in 4 cases. Impact of phenotypic remission: The achievement of phenotypic remission (whatever the time of evaluation) correlates with better PFS: 2-y PFS was 85% in these patients versus 27% in the other patients (p = 0.012). Considering the 19 patients with MRD evaluation available at 12 months after transplant, 2-y PFS was 100% in 12-month-negative-MRD patients (n = 10) versus 17% in positive-MRD patients at that date (p = 0.003) No relapse was observed in the group of patients who achieved phenotypic remission at 12 months post-transplant (figure ).
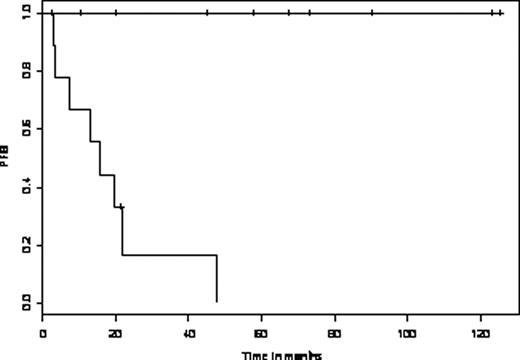
Post-transplant PFS according to the 12-month MRD status. Upper curve: 12-month MRD-negative patients (n = 10). Lower curve: 12-month MRD-positive patients (n = 9)p = 0.003.
Post-transplant PFS according to the 12-month MRD status. Upper curve: 12-month MRD-negative patients (n = 10). Lower curve: 12-month MRD-positive patients (n = 9)p = 0.003.
These data suggest that achievement of post transplant negative MRD in patients with CLL is associated with a long-term control of the disease and better PFS. In our series, no relapse occurred in patients with negative MRD at 12 months post transplant. These results could lead to decrease immunotherapy and to administrate donor lymphocytes to patients with post-transplant persistent positive MRD.
Leblond: ROCHE: Honoraria, Membership on an entity's Board of Directors or advisory committees, Speakers Bureau; MUNDIPHARMA: Honoraria, Membership on an entity's Board of Directors or advisory committees, Speakers Bureau; CELGENE: Honoraria, Membership on an entity's Board of Directors or advisory committees; Janssen: Honoraria, Membership on an entity's Board of Directors or advisory committees.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal