Abstract
Introduction
For patients in need of a hematopoietic stem cell transplant (HSCT) but lacking an HLA matched donor, a haploidentical family donor is a particularly appealing alternative. However, to prevent graft-versus-host disease (GVHD), haploidentical HSCT necessitates intensive in vivo or ex vivo T-cell depletion that results in frequent and often lethal infectious complications and/or high relapse rates, thus decreasing overall survival. To overcome this limitation, we have developed a strategy that photodepletes host-reactive cells from the donor T cell graft, while preserving anti-infection and anti-leukemia reactivity.
Patients and Methods
In an open-label, multi-center phase 2 clinical trial (CR-AIR-007; NCT01794299), 12 of a planned 23 patients with high-risk hematologic malignancies were treated to date with this immunotherapy approach consisting of donor lymphocytes selectively allodepleted of host-reactive T-cells using photodynamic therapy (ATIR). ATIR was infused 28-32 days after haploidentical CD34-selected HSCT. No post-transplant GVHD prophylaxis was used. These patients were compared to a control group of 28 patients treated in a previous Phase 2 study with an investigational product manufactured using a process different from the Phase 1 trial and resulting mainly in dead and inactive cells instead of ATIR (CR-AIR-004).
Results
Twelve patients, mean age of 45 (range 21-64), 6 females/6 males with AML (n=9) and ALL (n=3) were treated with ATIR so far. ATIR consisted mainly of T-cells (>90%), with residual B and NK cells (≤10%). Selective depletion of recipient-reactivity in each ATIR cell graft was assessed using a CFSE-based proliferation assay. Cell division numbers upon stimulation were analyzed using Modfit LT software (Fig 1A), which generated a proliferation index representing viable/reactive T-cells in donor cells (blue) and final ATIR product (green)(Fig 1B). Selective depletion of recipient-reactive T-cells with preservation of reactivity towards 3rd party antigens and anti-CD3/CD28 was observed in all ATIR cell grafts and used as a release criteria in the 007 study.
A) CFSE-dilution pattern in Modfit LT software of ATIR stimulated with 3rd party cells. B) CFSE-based proliferation confirmed selective depletion of recipient-reactive T-cells in all grafts (representative depiction).
A) CFSE-dilution pattern in Modfit LT software of ATIR stimulated with 3rd party cells. B) CFSE-based proliferation confirmed selective depletion of recipient-reactive T-cells in all grafts (representative depiction).
Preparative regimen consisted of A) FTBI (1200 cGy; n=5) or B) melphalan (120 mg/m2; n=7), along with thiotepa (10 mg/kg), fludarabine (30 mg/m2 x5 d) and ATG (2.5 mg/kg x4 d). Neutrophil and platelet engraftment was achieved in all patients at a median of 12 days (range: 9-35). No patient experienced graft rejection.
Patients (n=28) in the 004 control group, mean age of 42 (range 18-61), 13 females/15 males had AML (n=19), ALL (n=6) or MDS (n=3). CFSE proliferation in T-cell grafts could not be assessed a posteriori due to low cell viability. These 004 patients received the same A) FTBI- (n=14), B) melphalan- (n= 10) based preparative regimen as 007 patients, except for 4 patients receiving single fraction (800 cGy) TBI. Neutrophil and platelet engraftment was achieved at a median of 16 days (range: 7-54). Three patients showed secondary graft rejection.
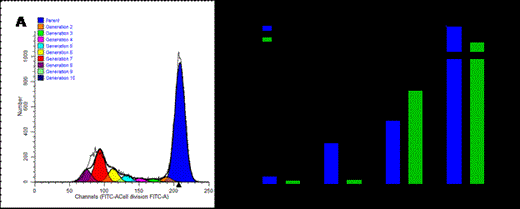
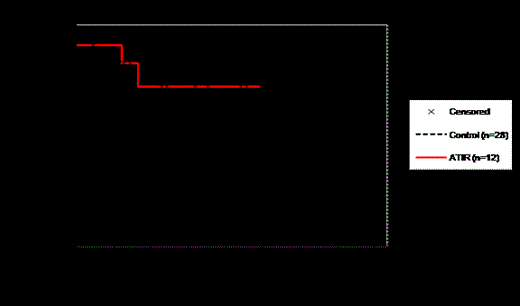
Two patients in study CR-AIR-007 developed acute GVHD grade I (skin only) approximately 130 days post HSCT, which was of short duration, (18 and 41 days). Two patients died of infection and no patient relapsed at a mean follow-up of 8 months post HSCT (range 1-14 months). In the CR-AIR-004 control group, 2 patients developed grade I, 1 patient grade II and 3 patients grade III GvHD, none of these cases were lethal. Seventeen patients died of transplant related complications and 2 patients of relapse/disease progression. TRM is 20% in 007 group vs 63% in the 004 control group and OS is 80% in 007 group vs 35% in the 004 control group at 9 months post-transplant (Figures 2A and 2B).
Conclusions
These data confirm that a novel immunotherapy strategy consisting of donor lymphocytes selectively photodepleted of alloreactive cells (ATIR) can be manufactured consistently and reproducibly. Results to date show that ATIR is safe and does not cause any grade III/IV GvHD. Moreover, haploidentical HSCT patients treated with ATIR demonstrate very promising TRM and OS rates when compared to the control group.
Roy:Kiadis Pharma: Consultancy, Research Funding. Foley:Hoffman-LaRoche: Advisory Board/Lectures Other, Honoraria; Lundbeck: Advisory Board/Lectures, Advisory Board/Lectures Other, Honoraria; Sanofi: Advisory Board/Lectures, Advisory Board/Lectures Other, Honoraria; Celgene: Advisory Board/Lectures, Advisory Board/Lectures Other, Honoraria; Pfizer: Advisory Board/Lectures Other, Honoraria; Novartis: Advisory Board/Lectures Other, Honoraria; Jansen: Advisory Board/Lectures Other, Honoraria; Alexion: Advisory Board/Lectures, Advisory Board/Lectures Other, Honoraria; Roche Canada: Honoraria, Research Funding, Unrestricted educational grant, Unrestricted educational grant Other. De Jong:Kiadis Pharma: Employment. Velthuis:Kiadis Pharma: Employment. Gerez:Kiadis Pharma: Employment. Reitsma:Kiadis Pharma: Employment. Wagena:Kiadis Pharma: Employment.
Author notes
Asterisk with author names denotes non-ASH members.
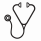
This icon denotes a clinically relevant abstract

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal