Abstract
Background: Individuals with clinically ascertained monoclonal B-cell lymphocytosis (c-MBL) having the phenotype of the chronic lymphocytic leukemia (CLL) have a 1-4% per year risk of progression to CLL requiring therapy. The risk factors for progression and the outcomes of individuals with c-MBL are not well defined.
Methods: Using the Mayo Clinic CLL Database, we identified individuals with c-MBL (absolute B-cell count of <5x109/L, in the absence of symptoms, organomegaly, splenomegaly and cytopenias) who were seen at Mayo Clinic, Rochester, MN between 01/1995 - 5/2016. Patients in whom an absolute B-cell count was not available were included in the analysis if the absolute lymphocyte count was <5x109/L. Baseline clinical characteristics and prognostic test results (including IGHV mutation status, genetic abnormalities detected by FISH, and expression of ZAP-70, CD38 and CD49d) were recorded. Time to first therapy (TFT) was analyzed using cumulative incidence methods accounting for competing risk of death. Multivariable Cox proportional hazards regression analysis was used to identify factors that predicted TFT. Because of missing data for some prognostic parameters, multiple models were run, introducing one novel prognostic factor at a time to the base model (which consisted of age and sex). Overall survival (OS) of these individuals was compared to age- and sex-matched population of the state of Minnesota.
Results: Eight hundred and fifty-one individuals with c-MBL were identified and included in this analysis. Median age was 69 years (range, 38-95 years), and 527 (62%) were males. The median absolute B-cell count at the time of diagnosis was 2.6 x 109/L (range, 0.1-5.0 x 109/L). The median serum beta-2 microglobulin (β2M) was 2.2 mg/dL (range, 1.0 - 21.5 mg/dL). One hundred and nine (30%) individuals had unmutated IGHV genes, and 38 (7%) had high-risk FISH (defined as either del17p13 or del11q23). The CD38 (≥30%), ZAP-70 (≥20%), and CD49d (≥30%) status was positive in 19%, 23% and 34% individuals, respectively.
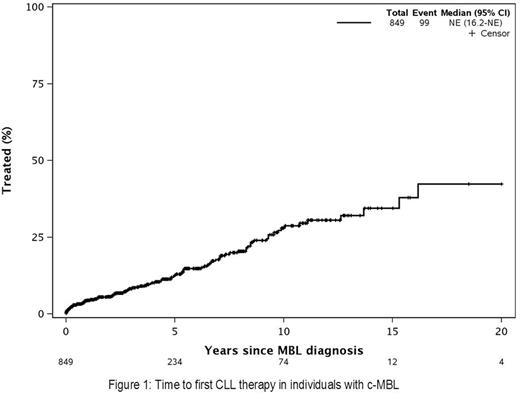
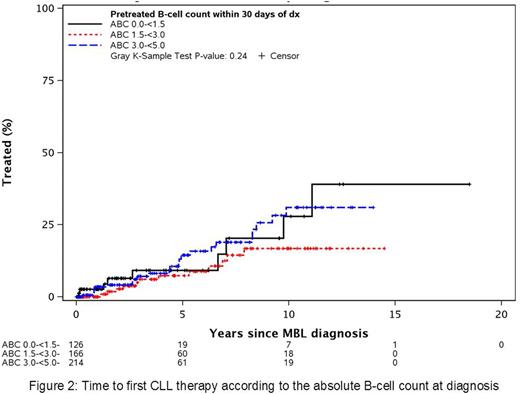
After a median follow-up of 6.8 years, 99 individuals required therapy for progressive disease (at a rate of 2.1% per year, Figure 1). On multivariable analysis, the following factors were associated with a higher risk of progression to CLL requiring therapy: a) unmutated IGHV status (hazard ratio [HR]:3.8, 95%CI 2.1 - 7.0, p<0.0001); b) positive CD49d status (HR: 3.1, 95%CI 1.6 - 5.9, p=0.0006); and c) positive CD38 status (HR: 2.8, 95% CI 1.7 - 4.8, p<0.0001). Although the HR for high-risk FISH was 2.0 (95% CI 0.9 - 4.4), it was not significantly associated with TFT (p=0.11), likely due to small sample size. Age, sex, serum β2M, and ZAP-70 expression were not predictive of TFT. Among these individuals with B-cell counts <5x109/L, further stratification of the absolute B-cell count at diagnosis showed no association with TFT (Figure 2).
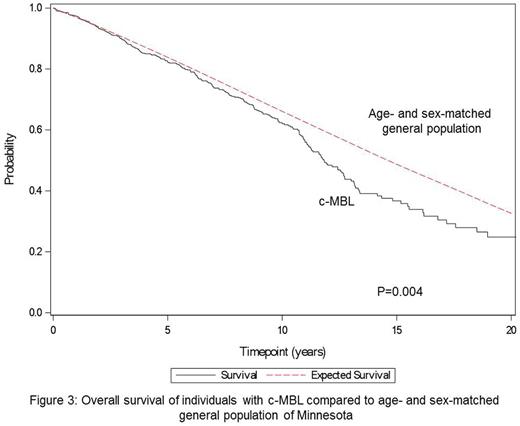
The median OS of individuals with c-MBL was 11.8 years. Although the OS among individuals with c-MBL and the age- and sex-matched general population of Minnesota appeared similar for the first 10 years of follow-up, OS was significantly shorter in the c-MBL group during the full follow-up interval (p=0.004, Figure 3).
Conclusion: In this large cohort of individuals with clinically ascertained MBL, the risk of progression to CLL requiring therapy was 2.1% per year. Biological characteristics of the B-cell clone including IGHV mutation status, and CD49d and CD38 status predicted time to first CLL therapy. On extended follow-up, the OS of individuals with c-MBL was significantly shorter relative to age- and sex-matched general population. These findings have important implications for counselling individuals with clinically ascertained MBL.
Parikh:Pharmacyclics: Honoraria, Research Funding. Ding:Merck: Research Funding. Kenderian:Novartis: Patents & Royalties, Research Funding. Shanafelt:Pharmacyclics: Research Funding; GlaxoSmithkKine: Research Funding; Janssen: Research Funding; Genentech: Research Funding; Celgene: Research Funding; Cephalon: Research Funding; Hospira: Research Funding.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal