Abstract
Background: The role of allogeneic hematopoietic stem cell transplantation (allo-HSCT) in the setting of refractory multiple myeloma (MM) is still controversial. Although potentially curative in a subset of pts, concerns regarding treatment related mortality (TRM) and graft vs. host disease (GVHD) preclude its universal use. In this study, we evaluated the role of allo-HSCT for pts with relapsed MM.
Methods: 110 consecutive pts with relapsed MM underwent allo-HSCT at our institution between 2000 and 2014. The primary objective was to assess progression-free (PFS) and overall survival (OS).
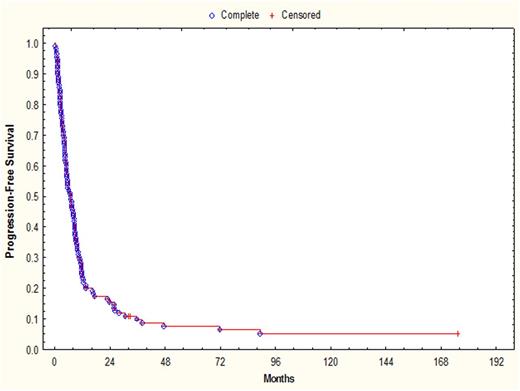
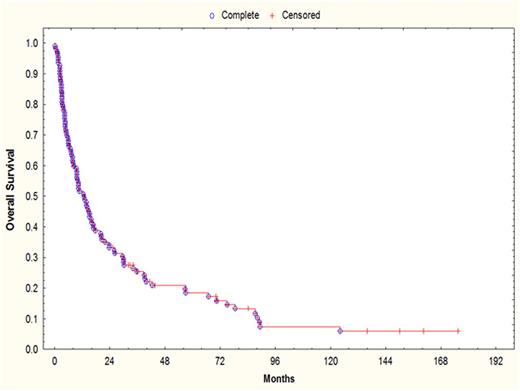
Results: Median age at allo-HSCT was 54 (range, 32-71) years and median time from diagnosis to allo-HSCT was 35.7 (range, 8.6 to 228.8) months. Fifty-two (47%) and 49 (45%) pts had standard-risk (SR) and high-risk (HR) cytogenetics at the time of allo-HSCT, respectively. Pts received a median of 5 (range, 1-9) prior chemotherapy regimens and 99 (90%) pts had at least 1 (range, 0-3) prior auto-HSCTs. One hundred one (92%) pts received either a proteasome inhibitor (PI) or an immunomodulatory drug (IMiD) prior to allo-HSCT, with 65 (59%) receiving both. Sixty eight (62%) received allo-HSCT from matched related, 34 (31%) from matched unrelated, 5 (4%) from cord blood, and 3 (3%) from mismatched donors. Preparative regimen was fludarabine/melphalan-based in 88 (80%) and fludarabine/busulfan-based in 16 (15%) pts. Median time to neutrophil and platelet engraftment was 12 (range, 8-30) and 13 (range, 0-81) days, respectively. Ten pts died of non-relapse causes within 100 days (100-day TRM: 9%) and 21 (19%) within 1 year. Grade 1-4 acute GVHD was seen in 50 (45%) and cGVHD in 35 (32%) pts, respectively. Eighteen (16%) achieved a CR, 26 (23%) a VGPR and 38 (34%) achieved a PR, with an overall response rate of 73%. With a median follow up of 41.9 months (range, 6.4 to 172.9) in surviving pts, 1- and 2-year PFS were 23% and 15%, respectively (Fig 1). One and 2-year OS were 50% and 32%, respectively (Fig 2). HR cytogenetics at allo-HSCT were associated with a significantly shorter 2-year PFS (6% for HR vs. 23% for SR; p=0.007) and OS (p=0.01). A response <PR after allo-HSCT was also associated with significantly shorter 2-year PFS (p<0.001) and OS (p<0.001).
Conclusions: Allo-HSCT is associated with durable remission and survival in approximately 15% of heavily pretreated pts with relapsed/refractory MM. Novel, more effective approaches are needed for patients with HR cytogenetic abnormalities.
No relevant conflicts of interest to declare.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal