Introduction: Daratumumab, a human IgGκ monoclonal antibody targeting CD38 with a direct on-tumor and immunomodulatory mechanism of action, is approved in combination with standard-of-care regimens for the treatment of newly diagnosed multiple myeloma (NDMM) and RRMM. When combined with standard of care regimens across four phase 3 studies, daratumumab demonstrated ≥44% reductions in the risk of progression or death, nearly doubled complete response (CR) or better rates, and tripled minimal residual disease (MRD)-negative rates at the 10-5 sensitivity threshold in pts with RRMM or NDMM (Palumbo A, et al. N Engl J Med 2016. 375[8]:754-766; Dimopoulos MA, et al. N Engl J Med 2016. 375[14]:1319-1331; Mateos MV, et al. N Engl J Med 2018. 378[6]:518-528; Facon T, et al. N Engl J Med 2019. 380[22]2104-2015). In the phase 3 POLLUX study (median follow-up 44.3 months), D-Rd reduced the risk of disease progression or death by 56% and significantly increased the overall response rate (ORR) versus Rd alone (93% vs 76%; P <0.0001) in patients (pts) with RRMM. Here, we present updated efficacy and safety analyses of POLLUX after >4 years of median follow-up.
Methods: Pts who received ≥1 prior line of therapy were randomized (1:1) to Rd (lenalidomide 25 mg PO on Days 1-21 of each 28-day cycle; dexamethasone 40 mg per week) ± daratumumab (16 mg/kg IV QW for Cycles 1-2, Q2W for Cycles 3-6, then Q4W until disease progression). Cytogenetic risk was determined by local fluorescence in situ hybridization or karyotyping; pts with high cytogenetic risk had t(4;14), t(14;16), and del17p abnormalities. PFS on subsequent line of therapy (PFS2), an exploratory endpoint, was defined as time from randomization to progression after next line of subsequent therapy or death.
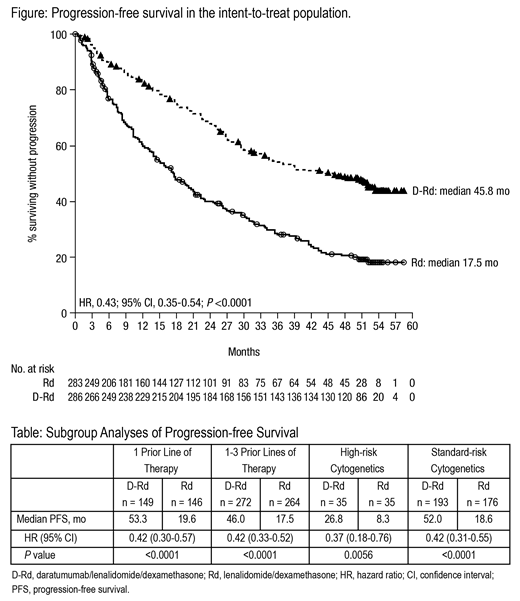
Results: A total of 569 pts were randomized (D-Rd, n = 286; Rd, n = 283). At a median follow-up of 51.3 months, D-Rd significantly prolonged progression-free survival (PFS) versus Rd (median 45.8 vs 17.5 months; hazard ratio [HR], 0.43; 95% confidence interval [CI], 0.35-0.54; P <0.0001; Figure). D-Rd also prolonged PFS versus Rd among pts with 1 prior line of therapy, among pts with 1-3 prior lines of therapy, and regardless of cytogenetic risk status (Table). A PFS benefit with D-Rd was also observed among pts who received prior lenalidomide (median 38.8 vs 18.6 months; HR, 0.34; 95% CI, 0.19-0.59; P <0.0001) and among pts refractory to bortezomib (median 34.3 vs 11.3 months; HR, 0.41; 95% CI, 0.25-0.68; P = 0.0004). D-Rd was associated with a significantly higher ORR versus Rd (93% vs 76%), including higher rates of ≥very good partial response (81% vs 49%) and ≥CR (57% vs 24%; all P <0.0001). Median time to next therapy for D-Rd versus Rd was not reached in the D-Rd group versus 22.8 months in the Rd group (HR, 0.39; 95% CI, 0.30-0.49; P <0.0001). D-Rd significantly prolonged PFS2 versus Rd (median 53.3 vs 31.6 months; HR, 0.54; 95% CI, 0.43-0.68; P <0.0001). In the D-Rd group, 121 deaths were observed versus 133 deaths in the Rd group; follow-up for overall survival is ongoing.
The median duration of treatment was 34.3 months in the D-Rd arm versus 16.0 months in the Rd arm. The most common (≥10%) grade 3/4 treatment-emergent adverse events (TEAEs) observed with D-Rd versus Rd included neutropenia (56% vs 42%), anemia (18% vs 22%), thrombocytopenia (15% vs 16%), pneumonia (16% vs 10%), and diarrhea (10% vs 4%). Similar rates of discontinuations due to TEAEs were observed for D-Rd versus Rd (16% vs 15%). The incidence of invasive second primary malignancies was 4.9% and 5.7% for the D-Rd and Rd groups, respectively.
Additional efficacy data, including minimal residual disease, and safety analyses will be presented at the meeting.
Conclusion: After >4 years of median follow-up, D-Rd continues to demonstrate a significant PFS benefit and higher rates of deeper responses versus Rd alone in pts with RRMM. Although significant PFS benefit was observed with D-Rd in RRMM pts regardless of prior lines of therapy or cytogenetic risk status, the greatest benefit was observed when used in patients treated earlier with D-Rd. The significant improvement in PFS2 suggests a potential survival benefit, but OS data is still immature. No new safety concerns were identified with this additional follow-up.
Kaufman:Celgene: Consultancy; Winship Cancer Institute of Emory University: Employment; Takeda: Consultancy; Pharmacyclics: Membership on an entity's Board of Directors or advisory committees; Janssen: Honoraria; AbbVie: Consultancy; Bristol-Myers Squibb: Consultancy; Incyte: Consultancy; Karyopharm: Membership on an entity's Board of Directors or advisory committees; TG Therapeutics: Consultancy; Amgen: Consultancy. Usmani:Amgen, Bristol-Myers Squibb, Celgene, Janssen, Merck, SkylineDX, Takeda: Other: Consultant/Advisor; Amgen, Celgene, Janssen, Sanofi, Takeda: Speakers Bureau; Amgen Array Biopharma, Bristol-Myers Squibb, Celgene, Janssen, Merck, Pharmacyclics, Sanofi, Takeda: Other: Research Grant. San-Miguel:Amgen, Bristol-Myers Squibb, Celgene, Janssen, MSD, Novartis, Roche, Sanofi, and Takeda: Consultancy, Honoraria. Bahlis:Celgene: Consultancy, Honoraria; Amgen: Consultancy, Honoraria; Takeda: Consultancy, Honoraria; AbbVie: Consultancy, Honoraria; Janssen: Consultancy, Honoraria. White:Janssen: Consultancy, Honoraria; Amgen: Consultancy, Honoraria; Celgene: Consultancy, Honoraria; Takeda: Consultancy, Honoraria; Sanofi: Consultancy, Honoraria. Cook:Amgen, Bristol-Myers Squib, GlycoMimetics, Seattle Genetics, Sanofi: Honoraria; Janssen, Takeda, Sanofi, Karyopharm, Celgene: Consultancy, Honoraria, Speakers Bureau; Celgene, Janssen-Cilag, Takeda: Honoraria, Research Funding. Ho:Novartis: Other: Trial Investigator meeting travel costs; La Jolla: Other: Trial Investigator meeting travel costs; Janssen: Other: Trial Investigator meeting travel costs; Celgene: Other: Trial Investigator meeting travel costs. Moreau:Takeda: Consultancy, Honoraria; AbbVie: Consultancy, Honoraria; Celgene: Consultancy, Honoraria; Janssen: Consultancy, Honoraria; Amgen: Consultancy, Honoraria. Krevvata:Janssen: Employment. Pei:Janssen: Employment, Equity Ownership. Ukropec:Janssen: Employment, Equity Ownership. Renaud:Janssen: Employment, Equity Ownership. Trivedi:Janssen: Employment, Equity Ownership. Kobos:Janssen: Employment. Dimopoulos:Sanofi Oncology: Research Funding.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal