Background Myelodysplastic Syndrome (MDS) is characterized by ineffective clonal hematopoiesis with peripheral blood cytopenias, leading to death from infection or bleeding. Azacitidine (AZA), a hypomethylating agent (HMA) is the standard of care for treatment of MDS patients (pts) with higher-risk MDS [Silverman LR, The Myelodysplastic Syndrome in Cancer Medicine, Editors: R.J. Bast, et al. 2017]. Responses to AZA occur in 50% of pts with significant effects on hematopoiesis ranging from improvement in a single lineage to complete restoration of blood counts and transfusion independence [Silverman LR, et al. Leukemia, 1993]. AZA treatment is associated with global DNA hypomethylation, including human endogenous retroviruses (HEV) which further activates innate immune signaling [Chiappinelli KB,et al. Cell, 2015]. The exact mechanism by which AZA improves hematopoiesis is unknown. AZA improves overall survival of pts, yet despite this, 100% of pts ultimately fail treatment with worsening cytopenias or transformation to leukemia [Silverman LR, et al. B. J Clin Oncol, 2002; Cancer, 2011]. Thus, understanding the mechanism of resistance and identification of targets which can reverse HMA failure and improve hematopoiesis in MDS pts is critical. Our clinical data demonstrate that AZA combined with Rigosertib (RIGO), a novel Ras mimetic that inhibits Ras/Raf signaling [Athuluri-Divakar SK, et al. Cell, 2016], yields a response rate of 54% of pts who were HMA failures [Navada SC, et al. EHA 2019]. The response was associated with significant improvement in hematopoiesis and represents a critical observation in overcoming the epigenetic clinical resistance phenotype. The precise mechanism that leads to reversal of the resistance phenotype is poorly understood.
Methods: We investigated the differential protein expression in response to different treatment (AZA, RIGO alone and sequential combinations RIGO/AZA; AZA/RIGO) in vitro in MDS-L cell line by Reverse phase protein array (RPPA). Further, we also studied the functional role of these treatments on differentiation in the cell line by growing cells on semi-solid media as well as by flow cytometry using various stem cell and differentiation markers (CD34, CD38, CD45, CD123).
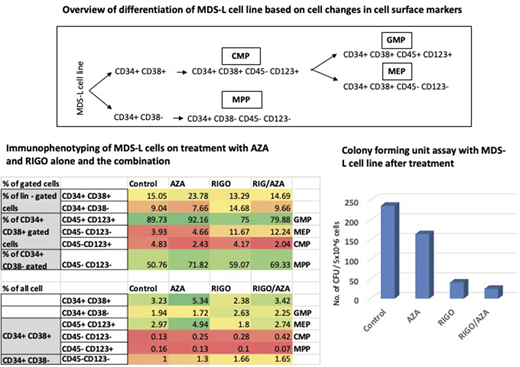
Results: RPPA analysis indicated a discrete responses to treatment in the MDS-L cell line. The response was prominent with differential expression of 43 proteins specifically in MDS-L cells treated with RIGO/AZA that include PIK3R1, AKT1, mTOR, p38 MAPK, PTEN, RPS6KA1 (Fold change (FC) < -2). All of these proteins are downregulated which suggests inhibition of PI3K and mTOR signaling. Proteins belonging to metabolic pathways, including ACC1 and ACLY, were found to be downregulated, whereas proteins related to mitochondrial function and oxidative phosphorylation (OXPHOS) were upregulated (FC > 1.5/< -1.5) in cells treated with RIGO/AZA. In addition, we found that MDS-L cells represented both CD34+CD38+ and CD34+CD38- populations by FACS analysis (Fig 1). AZA increases the percentage of CD34+CD38+, indicative of differentiation, whereas RIGO alone increased the percentage of CD34+CD38- cells, representing a primitive stem cell population (Table in Fig 1). Based on the combination of differentiation markers (illustrated in fig 1), we observed that RIGO alone, and sequenced as combination RIGO/AZA, impacts different progenitors such as granulocyte-macrophage progenitor (GMP), megakaryocyte erythroid progenitor (MEP), and multipotent progenitor (MPP). RIGO/AZA treatment showed a decrease in GMP, while the % of MEP was increased, as compared to other treatments. Moreover, we found a remarkable reduction in the number of colony forming units on differentiation media in response to RIGO (83%) and RIGO/AZA (90%).
Conclusions: These data demonstrate that in addition to inhibition of the PI3/AKT/mTOR pathway, the RIGO/AZA combination also impacts metabolic and differentiation pathways of MDS-L cells. RIGO alone appears to promote maintenance of a primitive stem cell population, while the RIGO/AZA sequenced combination appears to push the cells toward a cycling stage with increased expression of genes associated with OXPHOS. In comparison, when treated with RIGO, cells remain in a less differentiated stage. Further studies are underway to determine the effect of metabolic changes on differentiation and maintenance of hematopoietic stem cells.
Navada:Onconova Therapeutics Inc: Research Funding. Reddy:Onconova Therapeutics Inc: Research Funding. Silverman:Celgene: Research Funding; Medimmune: Research Funding; Onconova Therapeutics Inc: Patents & Royalties, Research Funding.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal