Abstract
We recently found that a low number of circulating dendritic cells (DC) is predictive of increased relapse, acute GVHD, and poor survival following allogeneic SCT (
Reddy V et al, Blood 2004;103(11):4330–5
). Interleukin-12 (IL-12) is an immunostimulatory cytokine involved in the activation of naïve T cells by DC (Rissoan et al. Science 1999;283(5405):1183–6
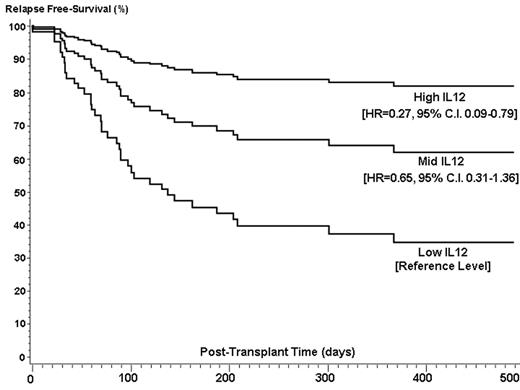
). We hypothesized that patients with high levels of circulating IL-12 in the post transplant period have improved relapse free survival. We studied 134 patients, 120 of whom were evaluable and transplanted during the period of July 1999 to April 2004. Seventy-two patients had transplants from related and 48 from unrelated donors, for predominantly high risk (88%) hematologic malignancies. Median follow up was 1158 days (range 70–1792). Blood samples were collected as baseline prior to conditioning, on day 0 prior to stem cell infusion and during the first week (day 4 and/or 7) after transplant. Plasma IL-12 levels were measured by ELISA. To determine the independent effect of post-transplant IL-12 levels and clinical outcomes, a cluster analysis was performed on the logarithmically transformed mean IL-12 concentration at days 4 and 7 post-transplant. The analysis generated a low, medium and high IL-12 group. Forty-six patients had low levels of IL-12 (median=2 pg/ml, range 0–6.5), 49 patients had medium (median=20.5 pg/ml, range 7–75.5) and 25 patients had high levels (median=181 pg/ml, range 84–623). There was a significant association between IL-12 level and onset of relapse. Using a multivariate Cox model with the low group level as reference, the high IL-12 group level had an adjusted hazard ratio (HR) of 0.27 (95% C.I. 0.09–0.79) and the medium group level a HR of 0.65 (95% C.I. 0.31–1.36). Incidence of relapse at 500 days by Kaplan-Meier analysis by IL-12 group were 23.0% (high group), 40.3% (medium group), and 48.8% (low group). Covariates in the multivariate models were gender match, disease risk, graft source, patient age, donor relation. There was a significant relationship between IL-12 levels and composite death and relapse, the high IL-12 group had a HR of 0.37 (95%C.I.=0.17–0.80) and the medium group a HR of 0.85 (95%.C.I. 0.50–1.45). There was no association between IL-12 levels and risk of AGVHD (p-value=0.51). In addition to IL-12, disease risk was a significant risk factor for the composite endpoint of relapse or death (HR=5.4, p-value=0.0052). The model generated for the outcome of relapse only did not have any additional significant risk factors. In conclusion, high post-transplant levels of IL-12 are associated with less relapse and improved relapse free survival after transplantation. This data suggests that IL-12 administration should be considered as a possible component in studies addressing treatment of relapse after transplantation.Author notes
Corresponding author
2005, The American Society of Hematology
2004