Abstract
Introduction:
Little is known about the lethality of acute GVHD (aGVHD) in T -cell depleted (TCD) allogeneic hematopoietic stem cell transplantation (HSCT). We examined the incidence of aGVHD and its relative contribution to non relapse mortality (NRM) in a cohort of consecutive TCD HSCT at a single institute.
Methods:
We report 132 consecutive subjects who had undergone TCD HLA-identical sibling HSCT between 2006 and 2016 for hematologic malignancies. All subjects received conditioning with Fludarabine 125mg/m2, Cytoxan 120 mg/kg and 1200 cGy total body irradiation (TBI) (<age 55 years) or 400-600 cGy (³age 55) followed by either a CD34+ selected (n=112) or CD3/19 depleted (n=20) peripheral blood stem cell graft with a T cell addback of 5-50x10e4CD3+/kg (Miltenyi CliniMACS, resulting in 3.5 to 4-log TCD). Low dose cyclosporine was used until day 21 for GVHD prophylaxis.
Thirty-six subjects were over the age of 55 years, 66 were females and 66 were males. Transplant indications were acute leukemia (92), myelodysplastic / myeloproliferative syndromes (26), lymphoid malignancies (7) and chronic myelogenous or myelomonocytic leukemia (7). Fifty-three percent of subjects were at a high risk of relapse. The median follow-up post HSCT was 4.3 years.
Results:
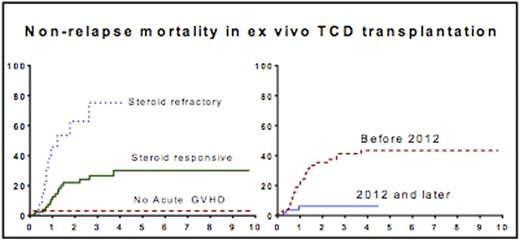
The incidence of Grade 1-2 and 3-4 aGVHD were 51.6% and 19%, respectively. Of these, 15% of aGVHD was steroid refractory and was treated with infliximab/basiliximab or with mesenchymal stromal cells. Extensive or limited chronic GvHD was observed in 30% and 24% of subjects. 74% of those at risk developed cytomegalovirus (CMV) reactivation. The Kaplan-Meier (KM) estimate for overall survival (OS), NRM and cumulative incidence of relapse (CIR) for the entire cohort was 71%, 14.6% and 24% respectively at one year, and 52%, 32.5% and 39% at 5 years. We considered the impact of CMV reactivation, slow donor lymphoid chimerism and steroid refractory aGVHD on NRM. However there was no significant impact from CMV reactivation or slow (> 31 days) achievement of complete donor lymphoid chimerism. Significantly improved outcomes were noted for those transplanted beyond 2012: OS, NRM and CIR being 82%,6.2% and 20% at one year, and 68%, 6.2% and 41% at 3 years. Cox proportionate hazard modeling identified steroid refractory aGVHD (HR 4.0, P=0.007) and transplant prior to 2012 (HR 6.7, P=0.001) as significant factors impacting NRM.
Conclusions:
T cell addback after ex vivo TCD HSCT was associated with a significant burden of aGVHD. Steroid refractory aGVHD impacted NRM, but slow lymphoid engraftment, disease risk, CMV reactivation and age did not. Significant improvements in NRM in the current era suggest greatly improved salvage of steroid refractory aGVHD.
No relevant conflicts of interest to declare.
Author notes
Asterisk with author names denotes non-ASH members.