Abstract
Background
The Revised International Prognostic Scoring System (IPSS-R) was developed to risk stratify untreated patients (pts) with myelodysplastic syndromes (MDS). It has since been validated in pts treated with a single line of therapy; however, these approaches do not reflect typical MDS pts who receive different types of treatment in different sequences. Recently, genome sequencing technologies have identified recurrent somatic mutations that impact survival in MDS. We propose and validate a modification to the IPSS-R to include mutational data that can improve its predictive power at diagnosis regardless of the initial or subsequent therapies and at any time during the disease course.
Methods
Clinical and mutational data from MDS pts diagnosed between 1/2000-1/2012 were analyzed. A panel of 62 gene mutations obtained by next generation targeted deep sequencing which has been described as recurrent mutations in myeloid malignancies was included. Pts who underwent hematopoietic cell transplant (HCT) were censored at the time of transplant. A Cox proportional multivariate analysis including age, IPSS-R score and mutations that are present in > 10 pts was used to select independent prognostic factors. The fit of the proposed model to the data was assessed by using the concordance (c-) index.
Results
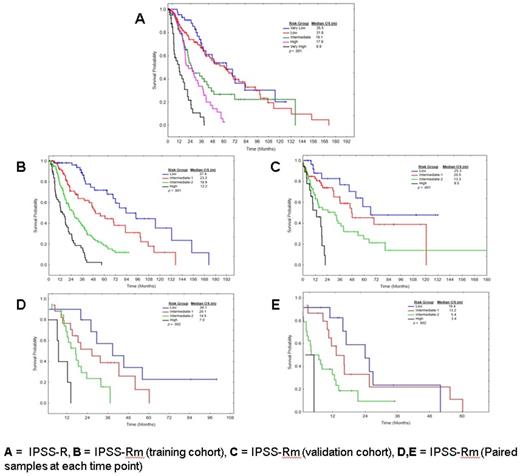
A total of 508 pts were included and divided into two cohorts, training (333 pts, used to build the new model), and validation (175 pts, used to validate it). Median age of the training cohort was 68 years (range, 20-87); 214 pts (64%) had de novo MDS, 39 (12%) had prior antecedental hematologic disorders, 37 (11%) secondary MDS, and 43 (13%) had chronic myelomonocytic leukemia. Pts received 0-7 lines of therapy: 15% did not receive any treatment, 85% received at least one treatment, 40% received > 2 treatments, 20% received > 3 treatments and 14% underwent HCT. First line therapies included: growth factors (30%), azacitidine+/- combinations (32%), decitabine+/- combinations (7%), lenalidomide (5%), investigational agents (5%), chemotherapy (2%), and immunosuppressive therapy (4%). Per IPSS-R, median OS for very low, low, intermediate, high, and very high was 35.5, 31.8, 19.1, 17.9, and 6.9 months (m), respectively, Figure1A. To minimize bias in pt selection, the validation cohort samples were randomly selected and sequenced after the development of the new model.
Among the 62 gene mutations, 24 were present in > 10 pts in the training cohort: TET2 (17%), ASXL1 (15%), SF3B1 (14%), STAG2 (11%), DNMT3A (11%), RUNX1 (10%), U2AF1 (9%), GPR98 (8%), ZRSR2 (7%), BCOR (6%), TP53 (5%), NF1 (5%), EZH2 (5%), APC (5%), SUZ12 (5%), CBL (4%), PRPF8 (4%), NRAS (3%), CUX1 (3%), DDX54 (3%), IDH1 (3%), KDM6A (3%), PHF6 (3%), and SETBP1 (3%). A cox proportional hazard analysis including age, IPSS-R score, and the 24 genes mutations listed above identified the following as independent prognostic factors: age, IPSS-R, EZH2, SF3B1, and TP53. The linear predictive Cox model score obtained using the fitted coefficients of each prognostic factor wasage x.04 + IPSS-R score x.3 + EZH2 x.7 + SF3B1 x.5 + TP53 x 1 which translated to 4 prognostic groups: low, intermediate-1, intermediate-2, and high with median OS of 37.4, 23.2, 19.9, and 12.2 m, respectively, p< .001, Figure1B with significant improvement in the C-index of the new model (.74) observed compared to the IPSS-R (.57). The model was then applied to the validation cohort with significant ability to distinguish prognostic groups for OS (p<.0001) (Figure1C) despite differences between training and validation cohorts in IPSS-R risk categories (p =.04) and treatment history. To validate whether the new model can be applied at any time during disease course, we sequenced paired samples from 53 MDS pts at different time points (diagnosis, after treatment failure, and at the time of AML progression). The median time from diagnosis to sample 1 was 5.6 m (range, 0-56) and to sample 2 was 18.2 m (range, 5-94.6). The new model was able to predict the OS at each time point (Figure 1D shows IPSS-Rm at sample1 and 1E at sample2).
Conclusion
We propose a modification of the IPSS-R scoring system that incorporates mutational data and enhances its predictive ability in pts with MDS regardless of initial or subsequent treatments. This model is dynamic and valid at varying time points of a pt's disease course.
OS by IPSS-R and IPSS-Rm in training, validation, and paired samples cohorts
Sekeres:TetraLogic: Membership on an entity's Board of Directors or advisory committees; Celgene Corporation: Membership on an entity's Board of Directors or advisory committees; Amgen: Membership on an entity's Board of Directors or advisory committees.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal