Abstract
Objectives: Low donor chimerism after hematopoietic cell transplantation (HCT) is associated with increased risk of post transplant relapse. Our group has shown that donor lymphocyte infusion (DLI) was ineffective for converting <40% donor CD3 chimerism to full donor chimerism. If successful, however, donor CD3 chimerism >90% elicited GVT effects (Blood 2004;103:790). To facilitate effectiveness of DLI for patients (pts) with low or declining donor CD3chimerism, a prospective multicenter trial assessing the safety and efficacy of addingpentostatin was developed.
Patients and Methods: Pts at risk for rejection after HCTs, defined as low (<50%) but persistent (>5%) donor CD3 chimerism and with stable/in remission disease, were included. Pts were excluded if they had evidence of relapse/progression, ongoing grades II-IV acute (a)GVHD, or extensive chronic (ec)GVHD. Between 2003 and 2014, 36 pts were treated on the study; 35 pts received a total of 41 DLIs following a dose of pentostatin, and 1 pt received pentostatin only. Diagnoses included AML (n=13), NHL (n=4), CLL (n=7), CML (n=2), MDS (n=6), MPD (n=2), MM (n=1), NHL and MDS (n=1). Pts received nonmyeloablative (n= 35) or ablative (n=1) conditioning, followed by PBSCs from HLA-matched related (n=17) or unrelated (n=17) donors, or 1-allele mismatched unrelated donor (n=2). Median age at HCT was 58 (34-72) years. DLI was given at a median of 96 (54-339) days after HCT. A dose of pentostatin was given 2 days before infusing 1x107 CD3 cells/kg (n=26), 2x107 CD3 cells/kg (n=1), or 3x107 CD3 cells/kg (n=14). Per protocol, prophylactic immunosuppression (IS) with cyclosporine and MMF was given after DLI to the last 6 pts on study.
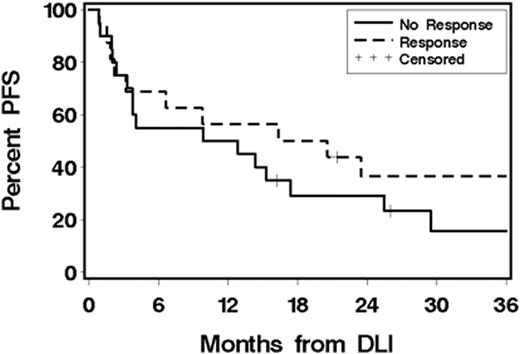
Results: Median donor CD3chimerism beforepentostatin/DLI was 28 (5-47)%. Efficacy, defined by increases in donor CD3chimerism>10% maintained to day 56 post-DLI, was seen in 16 pts (44.4%) with a median CD3 donorchimerism of 64 (48-100)%. There was a trend for better efficacy among the 21 pts who received first treatment within 100 days after transplant (57%) compared to the 15 pts who received first treatment more than 100 days after HCT (27%) (p=0.07). Six pts received 2nd treatment ofpentostatin/DLI; among them 1 responded. Fifteen pts (12 responders) developedaGVHD after DLI [grade I (n=2), II (n=9), III (n=3), IV (n=1)] at a median of 10 (0-83) days after DLI. One pt developed skinGVHD, grade II, afterpentostatin administration and DLI was aborted. Of the 16 pts who developedaGVHD afterpentostatin/DLI, 3 had a prior history of GVHD after transplant. Thirteen pts developedcGVHD, ofwhom 10 developedecGVHD at a median of 112 (13-347) days after DLI. One pt developedecGVHD with no prioraGVHD. Among the 6 pts who received prophylaxis IS after DLI 1 pt developedaGVHD grade II, and none developedcGVHD. However, only 2 of those 6 pts responded. Seventeen pts developed grade 4cytopenia after DLI; 9 pts developed both neutropenia and thrombocytopenia, 4 pts developed neutropenia, and 4 pts developed thrombocytopenia. Among the 13 patients who developed grade 4 neutropenia, 9 (69%) were non-responders. Median time between DLI and lowest ANC count was 22 (2-100) days, and neutropenia lasted for median of 7 (1-52) days. Twelve pts received platelet transfusions started at median of 33 (1-98) days after DLI. Nineteen pts relapsed at a median of 91 (26-777) days after DLI. Among the 20 non-responders 12 relapsed (60%), compared to 7 of 16 responders (44%) (HR 0.64 (0.3-1.6), p=0.35). Ten of the 17 pts (59%) who developedcytopenia relapsed, 6 ofwhom (60%) were non-responders. Median number of significant infections was 2 (0-10) per pt. Twenty-eight pts died at a median of 522 (67-2028) days after DLI. Causes of death were relapse (n=21), respiratory failure/infections (n=4), grade IV GVHD (n=2), or other causes (n=1). Five of the 16 responders (31%) are alive, all in CR. Six of the 20 non-responders (30%) are alive, only 3 in CR (Figure 1).
Summary:Pentostatin/DLI increased donor CD3chimerism in pts after HCT if was given within 100 days after transplant, and it was well tolerated. Response was associated with GVHD. Delayed treatment after HCT and prophylactic IS after DLI were associated with decreased efficacy. There was a trend for higher relapse rate among the non-responders and pts who developed cytopenia, but the differences were not statistically significant.
Pulsipher:Novartis: Consultancy, Other: Advisory Board, Steering Committee for Phase II Study; Jazz Pharmaceutical: Consultancy, Other: Advisory Board; Chimerix: Consultancy, Other: Advisory Board ; Medac: Other: Travel support for a study group.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal