Abstract
Background
Monoclonal gammopathy of undetermined significance (MGUS) is a precursor condition to multiple myeloma and other lymphoproliferative disorders. In individuals with MGUS, the average risk of progression to a lymphoproliferative disorder has been estimated to be 1% per year, however, most previous studies have been performed on clinically established cohorts and very few have been population-based. A high monoclonal (M)-protein concentration, non-isotype IgG, and skewed free light chain (FLC) ratio are routinely taken into account when assessing risk for progression. Other risk factors have also been identified, such as low serum albumin.
Methods
The cohort under study consisted of 299 individuals, 158 men and 141 women, with MGUS, identified through screening the participants of the population-based, longitudinal AGES-Reykjavik Study using serum protein electrophoresis and FLC assessment. The median age was 78 years (range 67-93 years). The outcome was first incidence of lymphoproliferative disorder, denoting multiple myeloma, lymphoma, amyloidosis, lymphocytic leukemia, plasmacytoma, and Waldenström's macroglubulinemia. Information on outcomes was supplemented by cross-linkage to national registries, and median follow-up time was 8.8 years. A Cox proportional hazards model was used to estimate hazard ratios (HRs) and 95% confidence intervals (CIs) for the risk of lymphoproliferative disorders. Results were adjusted for serum albumin in categories (below 35 g/L, 35-40 g/L, or above 40 g/L), M-protein concentration (above or below 15 g/L), FLC ratio, levels of free light chains, use of statins, smoking status, renal function in categories, and M-protein isotype. The multivariate model was reduced in a step-wise manner to a final model with only significant covariates.
Results
During follow-up, 26 of 299 individuals with MGUS proceeded to develop a lymphoproliferative disorder, representing a cumulative risk of 8.7% and an annual risk of 1.0%. MM occurred in 17 of 218 individuals with non-IgM MGUS, representing a cumulative risk of 7.8% and an annual risk of 0.9%.
In multivariate analysis, the final model contained serum albumin, M-protein concentration, and isotype A versus all other isotypes. Low serum albumin (HR = 6.3, 95% CI 1.0-40.6 for <35 g/L, and HR = 3.9, 95% CI 1.1-14.2 for 35-40 g/L), high M-protein concentration (HR = 4.1, 95% CI 1.2-14.0), and isotype A (HR = 5.8, 95% CI 1.6-21.0) were significantly associated with risk of progression.
In a similar model for progression to multiple myeloma only, low serum albumin, high M-protein concentration, and isotype A were also significantly associated with risk of progression, although the impact of low serum albumin was greater (HR = 33.1, 95% CI 2.4-462.2 for <35 g/L, HR = 10.97, 95% CI 1.4-88.3 for 35-40).
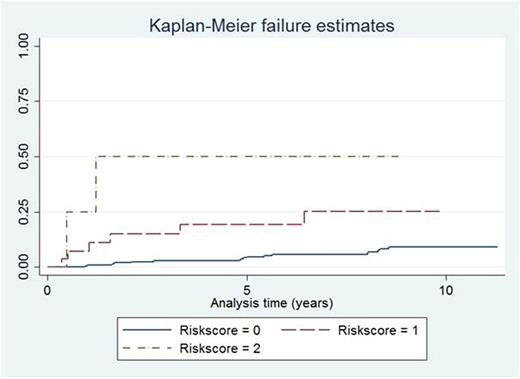
When assigning a risk score for progression where 1 point each was assigned for isotype IgA, serum albumin <35 g/L, and M-protein concentration >15 g/L, the HRs for individuals with 1 point was 3.9 (95% CI 1.6-9.9), and for 2 points 10.02 (95% CI 2.3-43.3). No individual had 3 points. For Kaplan-Meier estimates from risk scores, see Figure.
Summary and conclusions
In this large, population-based screening study, we found an annual risk of progression from MGUS to lymphoproliferative disease of 1%. Low serum albumin, high M-protein concentration, and M-protein isotype A were all independent risk factors for progression. Our results are in line with results from previous studies where a low serum albumin at MGUS diagnosis also has been associated with shorter survival and/or malignant transformation. Results from our study contradict previous studies that have pointed to skewed FLC ratio as an important risk factor for progression; in our study, a skewed FLC ratio was not significantly associated with risk of progression when adjusted for other covariates. The findings in our study suggest that serum albumin is important to take into account when assessing the risk of progression for individuals with MGUS.
Kaplan-Meier estimates for risk of progression, by risk score.
Kaplan-Meier estimates for risk of progression, by risk score.
Korde:Medscape: Honoraria. Landgren:Merck: Honoraria; Takeda: Honoraria; Amgen: Honoraria, Research Funding; Medscape Myeloma Program: Honoraria; BMS: Honoraria; Celgene: Honoraria, Research Funding.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal