Abstract
Acute promyelocytic leukemia is the first malignant disease highly curable with targeted therapy directed at a unique molecular abnormality. The characteristic bleeding diathesis is the most notorious manifestation of the disease, which historically has accounted for a high mortality rate during induction. Acute promyelocytic leukemia is one of the few hematologic diseases that must be recognized under the microscope by the practicing hematologist because early institution of all-trans retinoic acid (ATRA) at the first suspicion of the disease before confirmation of the diagnosis and aggressive blood product support are critical to reduce early mortality. ATRA plus anthracycline-based chemotherapy for induction and consolidation followed by maintenance ATRA with low-dose chemotherapy is currently the standard of care. However, the combination of ATRA and arsenic trioxide, with minimal chemotherapy to control leukocytosis, is very effective therapy for newly diagnosed patients. This combination may replace conventional approaches for most, if not all, patients in the very near future. Acute promyelocytic leukemia should be considered in any patient with newly diagnosed acute myeloid leukemia because the treatment is urgent and different from all other subtypes.
Introduction
Acute promyelocytic leukemia (APL) is a subtype of acute myeloid leukemia (AML) with distinctive biologic and clinical features that is now highly curable. Most patients are young, present with leukopenia, and exhibit a life-threatening coagulopathy, which is the most notorious manifestation of the disease. The cells from almost all patients have a balanced reciprocal translocation between chromosomes 15 and 17,1 which generates a fusion transcript joining the PML (promyelocyte) and RAR-α (retinoic acid receptor-α) genes.2 Leukemic promyelocytes have the unique ability to undergo differentiation with exposure to retinoic acid and both differentiation and apoptosis with exposure to arsenic trioxide (ATO). The disease is relatively rare in adults, accounting for only 10% to 15% of the approximately 13 400 adults diagnosed with AML in the United States each year. Although the incidence of APL among children with AML is similar in some series, a higher overall percentage of APL in children with AML compared with adults has been reported in others.3 In children, the disease is often associated with a high white blood cell count (WBC > 10 000/μL), the microgranular variant (M3V), and more all-trans retinoic acid (ATRA)-related toxicities, particularly pseudotumor cerebri.4
Intensive studies of the biology and treatment of the disease have resulted in a remarkably thorough understanding of its pathogenesis.5 Furthermore, a cure rate of approximately 80% to 90% of patients who survive induction and achieve complete remission (CR) can be expected.6 Yet there are nuances in the approach to patients with APL that are often overlooked, and complicated issues in treatment that remain to be studied. Here, the initial approach for patients with suspected APL, strategies for induction, consolidation and maintenance, assessment of molecular response, and the management of patients with relapsed disease are addressed. APL represents the first example of a malignant disease that is highly curable with molecularly targeted therapy against its specific genetic abnormality. This achievement reflects collaborative laboratory and clinical studies, led initially by innovative investigators in China7 and then France8 and subsequently by many other cooperative oncology groups throughout the world, which have culminated in the ultimate reward for both practicing physicians and patients.
Initial approach for suspected APL
Review morphology
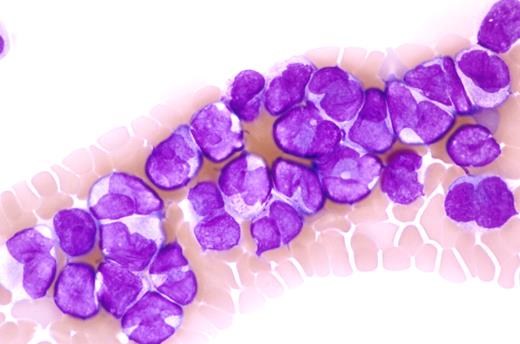
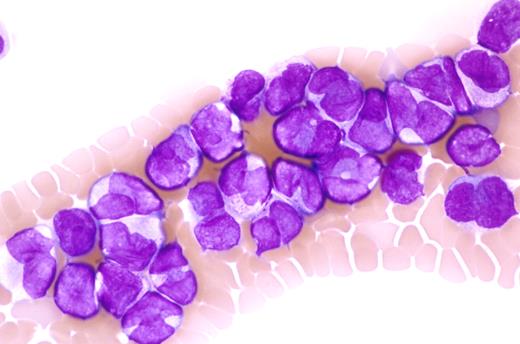
In contrast to almost every other disease for which treatment is started only after the correct diagnosis is established, treatment must begin before the diagnosis is confirmed in patients with suspected APL. Given the potentially rapidly fatal coagulopathy so characteristic of this disease, this is a practice of which we think even Sir William Osler would approve. The presumptive diagnosis of APL can usually be made by review of the peripheral blood smear alone or with the bone marrow aspirate and core biopsy by an experienced hematologist and hematopathologist in the presence of the characteristic clinical findings.9 The peripheral blood smear often shows leukopenia with circulating promyelocytes, which usually have abundant, often irregular-appearing primary azurophilic granules. Leukemic promyelocytes with multiple Auer rods may be found and are identified only in APL (Figure 1). Although often obscured by the granules, the nuclear contour is bilobed or reniform in appearance. The latter feature is important because patients with the M3V have the same predisposition toward catastrophic bleeding yet the same excellent outcome with appropriate treatment10 (Figure 2). Abundant primary azurophilic granules, although strongly suggestive of APL, do not confirm the diagnosis because leukemic cells from some patients with other subtypes of AML may have such prominent granules (Figure 3). Appreciation of these details of the morphology in APL by practicing hematologists is critical because this is the one subtype of AML for which immediate treatment must begin when the disease is first suspected and an experienced hematopathologist may not be immediately available.
The bone marrow aspirate shows numerous abnormal promyelocytes with prominent cytoplasmic granules, characteristic of hypergranular acute promyelocytic leukemia. Some of these cells exhibit reniform or bilobed nuclei, and several cells contain multiple Auer rods. The blood smear from this patient showed a pancytopenia with rare abnormal promyelocytes. Wright-Giemsa stain. Slides were viewed with an Olympus BX51 microscope using a 100×/1.4 oil-objective lens. Images were acquired with Olympus DP70 and 71 cameras and Olympus DP70 and 71 software. Images were not manipulated.
The bone marrow aspirate shows numerous abnormal promyelocytes with prominent cytoplasmic granules, characteristic of hypergranular acute promyelocytic leukemia. Some of these cells exhibit reniform or bilobed nuclei, and several cells contain multiple Auer rods. The blood smear from this patient showed a pancytopenia with rare abnormal promyelocytes. Wright-Giemsa stain. Slides were viewed with an Olympus BX51 microscope using a 100×/1.4 oil-objective lens. Images were acquired with Olympus DP70 and 71 cameras and Olympus DP70 and 71 software. Images were not manipulated.
This blood smear shows characteristic morphologic features of microgranular acute promyelocytic leukemia (M3V). A prominent leukocytosis is present with numerous cells exhibiting bilobed or monocytoid-appearing nuclei. Cytoplasmic granulation is absent to inconspicuous. Rare cells contained Auer rods (not shown in this field). Wright-Giemsa stain. Slides were viewed with an Olympus BX50 microscope using a 60×/1.4 oil-objective lens. Images were acquired using Olympus DP70 and 71 cameras and Olympus DP70 and 71 software. Images were not manipulated.
This blood smear shows characteristic morphologic features of microgranular acute promyelocytic leukemia (M3V). A prominent leukocytosis is present with numerous cells exhibiting bilobed or monocytoid-appearing nuclei. Cytoplasmic granulation is absent to inconspicuous. Rare cells contained Auer rods (not shown in this field). Wright-Giemsa stain. Slides were viewed with an Olympus BX50 microscope using a 60×/1.4 oil-objective lens. Images were acquired using Olympus DP70 and 71 cameras and Olympus DP70 and 71 software. Images were not manipulated.
This bone marrow aspirate represents a patient with non-APL AML and shows a marked shift to immaturity that could be easily mistaken for APL. Almost all of the cells are promyelocytes with prominent cytoplasmic granulation. Against the diagnosis of APL is the observation that the nuclei are round to oval in shape and Auer rods are completely absent. In this case, cytogenetic and molecular studies were negative for t(15;17) and the PML/RARα fusion transcript. Wright-Giemsa stain. Slides were viewed with an Olympus BX51 microscope using a 100×/1.4 oil-objective lens. Images were acquired with Olympus DP70 and 71 cameras and Olympus DP70 and 71 software. Images were not manipulated.
This bone marrow aspirate represents a patient with non-APL AML and shows a marked shift to immaturity that could be easily mistaken for APL. Almost all of the cells are promyelocytes with prominent cytoplasmic granulation. Against the diagnosis of APL is the observation that the nuclei are round to oval in shape and Auer rods are completely absent. In this case, cytogenetic and molecular studies were negative for t(15;17) and the PML/RARα fusion transcript. Wright-Giemsa stain. Slides were viewed with an Olympus BX51 microscope using a 100×/1.4 oil-objective lens. Images were acquired with Olympus DP70 and 71 cameras and Olympus DP70 and 71 software. Images were not manipulated.
Begin ATRA before confirmation of the diagnosis
The treatment of patients with APL represents a true emergency in the care of patients with acute leukemia primarily because of bleeding, which continues to represent a major cause of early death.11,12 Once the diagnosis is suspected on the basis of clinical findings and the peripheral blood smear (even without waiting for a bone marrow examination), and before the diagnosis is confirmed by cytogenetic or molecular studies, ATRA should be started at the standard dose of 45 mg/m2 per day in divided doses and given emergently, both to resolve the coagulopathy as well as to initiate induction therapy. It is important to determine the risk classification based on the WBC and platelet count.13 If the patient presents with low- or intermediate-risk disease (WBC < 10 000/μL) and significant coagulopathy, ATRA is continued for 1 to 3 days before initiating chemotherapy (specific chemotherapy discussed in “Initial studies of ATRA in APL”) to ameliorate the coagulopathy, provided that the WBC is not rising rapidly. Chemotherapy is started after 1 to 3 days of ATRA because, in patients with low- and intermediate-risk disease, the risk of APL differentiation syndrome is lower.14 However, if the patient presents with high-risk disease (WBC ≥ 10 000/μL), the administration of ATRA alone may induce further leukocytosis with exacerbation of the coagulopathy and may contribute to development of the APL differentiation syndrome. Therefore, for patients who present with high-risk disease, ATRA plus chemotherapy are started concurrently and, again, before the diagnosis of APL is confirmed by cytogenetics or molecular studies. As long as the diagnosis is AML, an anthracycline will be administered regardless of the specific subtype, and waiting for genetic confirmation to initiate chemotherapy in patients with high-risk APL introduces a potentially life-threatening delay. Although classifying patients into low-, intermediate-, and high-risk disease based solely on the WBC and platelet count is clinically useful, the specific levels are necessarily arbitrary and not applicable to certain patients. The 5-year cumulative incidence of relapse among low- and intermediate-risk patients in the APL2000 trial, one of the most contemporary series reported, was 19% and 10%, respectively, suggesting that the clinical risk classification was not sufficient to predict the relapse rate in all patients.15 It is probable that, as the pathogenesis of the disease is further unraveled, more refined molecular prognostic factors will be identified, which can further classify patients and guide therapy as is the case with other subtypes of AML.16
ATRA dose and duration
Because the optimal dose and duration of ATRA are not established, some practical comments may be helpful. The standard dose of ATRA is continued until achievement of CR by peripheral blood and bone marrow criteria as long as the patient is tolerating ATRA well. ATRA has underappreciated toxicities that may be misdiagnosed. Rashes are relatively common and may be attributable to other causes.17-20 Figure 4A shows an erythematous papular and pustular rash that developed on the elbow of a patient 18 days after initiation of ATRA and chemotherapy. The histologic findings show infiltration of the subcutaneous tissue with maturing myeloid cells, Sweet syndrome, reminiscent of lung findings in patients with the APL differentiation syndrome (discussed in “APL differentiation syndrome”).19-21 These 2 syndromes share several clinical and microscopic findings, and there may be a link between them.19 In practice, ATRA is often continued with progression of such toxicity when, instead, an interruption in ATRA or a course of corticosteroids may be indicated and beneficial. The recent report of a nonrandomized series suggested that patients have a less favorable outcome if they receive less than full duration of ATRA.22 However, in our experience, the majority of patients who receive at least 2 weeks of ATRA (in the event it is discontinued for prohibitive toxicity) subsequently achieve CR. ATRA toxicity has protean manifestations, which are often attributed to other causes, including bone marrow necrosis, pancreatitis, and hypercalcemia.23 Many pediatric hematologists-oncologists start ATRA at a lower dose of 25 mg/m2 per day for patients younger than age 20 because of the general perception that children and young adults tolerate ATRA less well than older adults, with a relatively high incidence of pseudotumor cerebri,4 and there are data suggesting that a half-dose of ATRA or even less may be as effective as the standard dose.24,25 Recent in vitro data suggest that low-dose retinoic acid induces differentiation, but not loss of leukemia-initiating cells (the putative stem cell) compared with higher doses.26 The in vitro studies did not include anthracyclines; therefore, the results of the in vitro studies may not pertain when ATRA is given to patients who usually receive concomitant anthracyclines. Although lower doses appear to be equally effective in small trials, clinical studies comparing doses of ATRA have not been carried out in children or adults. Therefore, ATRA is started and continued at the standard dose in adults unless prohibitive toxicities attributable to ATRA develop, which is not common.
Clinical photograph of the elbow and skin biopsy from a patient with APL treated with ATRA and chemotherapy who developed a rash on day 18 of initial therapy. (A) Coalescing cluster of erythematous papules and pustules with scattered satellite papules on the upper extremity. (B) Histopathology at low power reveals a subepidermal blister with marked dermal edema and a mixed interstitial infiltrate composed of neutrophils and mononuclear cells with scattered nuclear debris. At high power, these cells appear to be immature myelomonocytic cells with some extravasated erythrocytes and nuclear debris. Slides were viewed with an Olympus BX41 microscope using a 40× (A) and a 60× (B) dry lens. Images were acquired using Olympus DP70 and 71 cameras and Olympus DP70 and 71 software. Images were not manipulated.
Clinical photograph of the elbow and skin biopsy from a patient with APL treated with ATRA and chemotherapy who developed a rash on day 18 of initial therapy. (A) Coalescing cluster of erythematous papules and pustules with scattered satellite papules on the upper extremity. (B) Histopathology at low power reveals a subepidermal blister with marked dermal edema and a mixed interstitial infiltrate composed of neutrophils and mononuclear cells with scattered nuclear debris. At high power, these cells appear to be immature myelomonocytic cells with some extravasated erythrocytes and nuclear debris. Slides were viewed with an Olympus BX41 microscope using a 40× (A) and a 60× (B) dry lens. Images were acquired using Olympus DP70 and 71 cameras and Olympus DP70 and 71 software. Images were not manipulated.
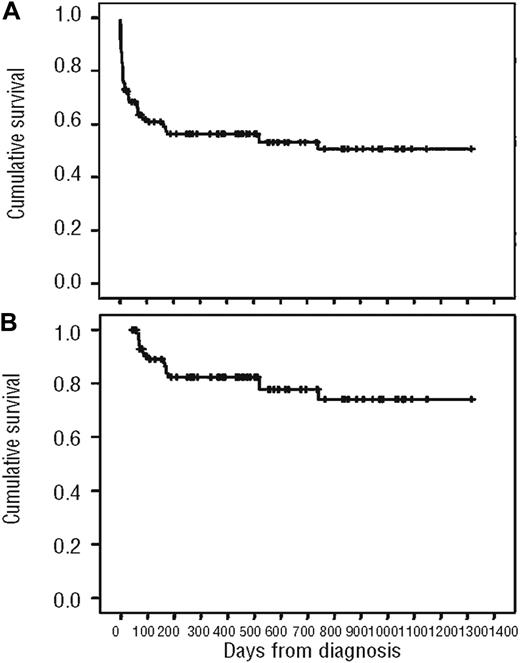
The most important message is that ATRA should be started at the earliest suspicion of APL. The adoption of new strategies of starting ATRA in emergency rooms in patients with suspected new diagnoses of APL, after urgent consultation with a hematologist and hematopathologist, may be effective in avoiding long delays so characteristic of the hospital course of many patients. Very early treatment with ATRA at the first suspicion of the diagnosis may be one of the few ways in which the early death rate resulting from bleeding, often in the central nervous system (CNS), lung, or gastrointestinal tract, and representing approximately 50% to 60% of early deaths,12 can be decreased. The early death rate is probably higher than the approximately 10% reported in large cooperative group clinical trials because a number of patients die early before registering to a clinical trial, even at institutions treating patients with contemporary ATRA and anthracycline-based strategies.27 Figure 5 shows the overall survival of all APL patients and those achieving CR treated in Brazil with conventional ATRA plus anthracycline-based chemotherapy where no patients were excluded on the basis of age or performance status.27 The induction mortality rate in this retrospective analysis was 32% when all patients were included, which suggests that the overall outcome from diagnosis in APL is not as favorable as often described in large clinical trials, which report only those patients who survive long enough to be registered for the trial. Although this may seem higher than other series, it probably represents a true appraisal of induction mortality, which is often difficult to determine in most contemporary reports.
Overall survival of APL patients treated with ATRA in combination with anthracyclines in Brazil. (A) Analysis of all patients. (B) Analysis excluding patients who died during induction.27
Overall survival of APL patients treated with ATRA in combination with anthracyclines in Brazil. (A) Analysis of all patients. (B) Analysis excluding patients who died during induction.27
Institute supportive care measures
Very aggressive supportive care measures may be more critical during the first few days of therapy in APL than those instituted with any other subtype of AML. Clinical bleeding, profound thrombocytopenia, and hypofibrinogenemia are characteristically present. A complete blood count is drawn 2 or 3 times per day initially until resolution of the coagulopathy. The fibrinogen and perhaps prothrombin time and partial thromboplastin time are drawn at least twice daily. Fibrin split products and D-dimer are less reliable indicators of ongoing coagulopathy attributable to the disease because both may be elevated after an initial decrease resulting from chemotherapy or fever.28 Platelets are transfused to maintain the platelet count more than 30 000 to 50 000/μL, and cryoprecipitate is administered to maintain the fibrinogen level more than 150 mg/dL.29 Both should be transfused multiple times a day if necessary to maintain these levels during the first week or so of therapy until the coagulopathy resolves. It is probable that very aggressive blood product support may decrease the incidence of fatal hemorrhage. In a study from Japan, the intended targeted levels for platelets (30 000/μL) and fibrinogen (1.5 g/L) were reached in only 71% and 40%, respectively, on the day of bleeding, and the risk of bleeding may be present for up to 20 days.30 A risk of thrombosis is present both at presentation as well as during the course of treatment.31,32 There is no clear benefit for routine heparin, except perhaps in the presence of a major deep vein thrombosis or antifibrinolytic therapy, although such agents have not been studied prospectively in the ATRA era.33 The routine use of heparin was abandoned with the introduction of ATRA because of the anticipation that ATRA would obviate its need. However, the early death rate has declined minimally, if at all, and bleeding remains a major cause of death during induction.34 The use of newer low-molecular-weight heparins could be explored in future clinical trials.
To avoid bleeding, which can be difficult to control, placement of a central venous catheter should be avoided. Instead, a midline peripherally inserted central venous catheter in the upper extremity can be placed for access. A routine lumbar puncture, which may be indicated in patients who present with high-risk disease (discussed in “Hyperleukocytosis”), should never be performed until all evidence of the coagulopathy has resolved.
Confirm diagnosis rapidly by genetics
Several laboratory techniques can be performed to definitively confirm the diagnosis of APL. Metaphase karyotyping has the advantage of being highly specific and can detect variant translocations and should be obtained in every patient with suspected APL. However, karyotyping is expensive, can take time, and is not successful in detecting cryptic molecular rearrangements. Reverse-transcriptase polymerase chain reaction (RT-PCR) for the PML-RAR-α fusion transcript is also routinely obtained. This can be considered the “gold standard” test because it identifies patients who are responsive to ATRA and can be detected in patients who are leukopenic.35,36 The few disadvantages include possible contamination, artifacts that might lead to a false-positive test, and a 48-hour turnaround time. Florescence in situ hybridization can be carried out but adds little to routine karyotyping and RT-PCR. PML antibody testing is rapid and can be positive in patients with atypical breakpoints.37 Although it has few disadvantages and is used in Europe, it has not been routinely adopted in the United States and we do not perform this test.
APL differentiation syndrome
The diagnosis of this cardiorespiratory distress syndrome requires vigilance and anticipation.38-42 The APL differentiation syndrome is often mistaken for fluid overload with pleural effusions or pneumonia. In contrast, diffuse alveolar hemorrhage may mimic the APL differentiation syndrome, and the 2 may be difficult to distinguish.43 At the earliest symptom of cough or shortness of breath or sign of pulmonary infiltrate, pleural or pericardial effusion, dexamethasone is instituted at a dose of 10 mg twice daily. It may be best to not necessarily wait for a chest radiograph to become abnormal. If the symptoms or signs are severe, ATRA (or ATO, discussed in “Introduction of ATO”) is discontinued and resumed at resolution of all signs and symptoms, but under the cover of steroids because the syndrome may recur. A nonrandomized study has suggested some benefit to prophylactic corticosteroids to prevent the syndrome.44 Caution should be exercised because the administration of corticosteroids to neutropenic patients may predispose them to infection. Nevertheless, for patients who present with significant leukocytosis (WBC ≥ 30 000-50 000/μL), prophylactic corticosteroids (dexamethasone) are strongly considered, provided there are no major contraindications, given clinical experience that such patients have a high incidence of potentially fatal complications.15,44 It should be acknowledged that there are few data to support this approach.
Hyperleukocytosis
Hyperleukocytosis is often associated with the M3V at diagnosis or may develop during treatment. Because of initial reports of death after leukapheresis in APL,41 this practice has been avoided. The possibility of apheresis resulting in lysis of the leukemia promyelocytes and other cells that subsequently may induce worsening coagulopathy suggests that one needs to be very cautious regarding this strategy. However, very few patients were reported initially, and this approach could be further explored.
The optimal treatment of patients who present with high-risk disease is the major obstacle in curing virtually all patients with APL in 2009. The less favorable outcome among high-risk patients is attributable both to higher induction mortality as well as a higher relapse rate. At this time, the best induction strategy appears to be simultaneous administration of ATRA plus cytotoxic chemotherapy. Concurrent ATRA and chemotherapy are commenced immediately as discussed earlier in “Begin ATRA before confirmation of the diagnosis” (Table 1). For patients with high-risk disease or for those who develop a WBC count more than 10 000/μL during therapy, CNS prophylaxis can be considered once CR has been achieved with administration of 4 weekly courses (the number is arbitrary to some extent) of intrathecal methotrexate or alternating with cytosine arabinoside (Ara-C) in an effort to prevent relapse in the CNS, although there are no data to support this approach.45,46 New strategies for future studies in high-risk patients include prophylactic corticosteroids, low-molecular weight heparins, the addition of FMS-like tyrosine kinase-3 (FLT3) inhibitors given the high incidence of FLT3 internal tandem duplication gene mutations, and autologous hematopoietic stem cell transplantation (HSCT) in first CR because this is an effective strategy for patients in second molecular CR (CR2) and transplantation-related mortality is extremely low.47-49
Initial studies of ATRA in APL
Several studies carried out by cooperative oncology groups around the world in the 1990s and 2000s established what is now the standard approach to the patient with newly diagnosed APL. The European APL group shows that the current ATRA plus chemotherapy (in this case daunorubicin + Ara-C) leads to a better outcome than sequential ATRA followed by chemotherapy.50 The Gruppo Italiano Malattie EMatologiche dell'Adulto (GIMEMA) Italian Cooperative Group demonstrates excellent outcome when ATRA was combined with single-agent idarubicin for induction.51,52 The first North American Intergroup study shows a benefit to maintenance therapy with ATRA given every other week.53 The Programa Español de Tratamientos en Hematología (PETHEMA) Spanish Cooperative Group omits Ara-C from both induction and consolidation and demonstrates excellent outcomes.54 The German AML Cooperative Group (GAMLCG) shows that high-dose Ara-C given in induction obviates the otherwise less favorable prognosis among high-risk patients55 (Table 2).
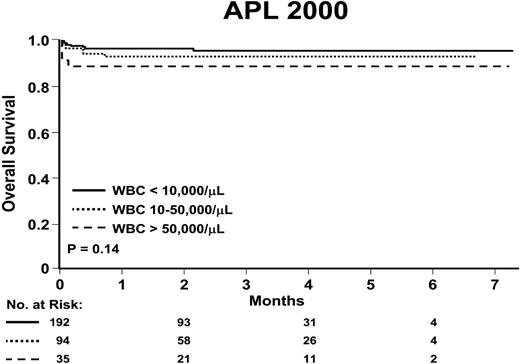
Therefore, ATRA plus anthracyclines either alone or with Ara-C for induction is the standard of care. For patients not participating on a clinical trial, ATRA and either daunorubicin (with or without Ara-C) or idarubicin can be given because there is no clear advantage of one anthracycline over the other. Idarubicin may result in a longer period of aplasia in some patients. Nevertheless, our preference for low- and intermediate-risk patients is ATRA plus idarubicin alone without Ara-C. Avoiding 7 days of continuous-infusion Ara-C is appealing. Myeloid growth factors are not routinely administered in induction during the neutropenic period unless there is a documented life-threatening infection or signs or symptoms of sepsis.56 With such contemporary strategies, overall survival is excellent15 (Figure 6). However, the standard of care has begun to change with the introduction of ATO in the treatment of newly diagnosed patients.
Introduction of ATO
Although contemporary strategies using ATRA plus anthracycline-based chemotherapy lead to cures in the overwhelming majority of patients with newly diagnosed APL, there are some potential long-term sequelae. These include the emergence of extramedullary disease at the time of relapse,57 second malignancies, including myelodysplastic syndromes,58 and delayed cardiomyopathy.59 Interestingly, reversible cardiac dysfunction related to ATRA has been reported.60 New strategies that incorporate ATO early in the treatment of the disease possibly may obviate such complications.
ATO is the single most active agent in APL. Its mechanisms include direct degradation of the PML-RAR-α fusion transcript, with resulting transcription of RAR-α target genes leading to apparent differentiation as well as growth arrest of leukemia-initiating cells by apoptosis or loss of self-renewal.26 ATO also appears to release cytochrome C from the mitochondria, leading to caspase activation, which itself leads to apoptosis and synergy with retinoic acid in leukemia-initiating cell loss.
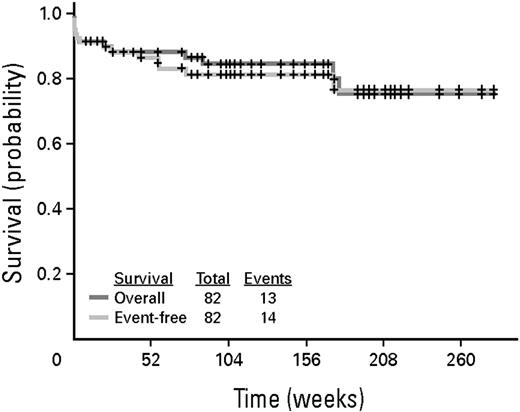
A series of studies has been carried out in newly diagnosed patients, which combine ATO with ATRA and intensive chemotherapy, ATRA, and ATO with minimal chemotherapy or ATO alone without ATRA or chemotherapy (Table 3). Investigators at the Shanghai Institute of Hematology combined ATRA, ATO, and chemotherapy in induction, administered intensive chemotherapy and consolidation, and gave maintenance and reported a CR rate of 93% and a disease-free survival of 94% with an overall survival of 98%.61 Investigators at the M. D. Anderson Cancer Center combined ATRA plus ATO administering modest amounts of chemotherapy or gemtuzumab ozogamicin (GO) only for patients who presented with high-risk disease or developed a WBC count more than 10 000 μL during the course of treatment.62 The CR rate was 90% with a disease-free survival of 90% and an overall survival of 85% (Figure 7). Investigators in India carried out a study in which they not only eliminated all chemotherapy, but they also eliminated ATRA, administering only single-agent ATO and reported a CR rate of 86% and cumulative incidence of relapse at 10% and an overall survival of 85%.63 Mathews et al63 reported that patients who presented with a WBC count less than 5000/μL and a platelet count greater that 20 000/μL treated with single-agent ATO had a survival at 5 years of 100% without a single patient relapsing. Higher-risk patients had an event-free survival of only 67%, which supports the addition of ATRA to ATO in newly diagnosed patients. In the study by Raanani et al, the APL differentiation syndrome developed in only 2 of 17 (12%) patients treated with concurrent ATRA and ATO.43 In the study by Ghavamzadeh et al, in which newly diagnosed patients were treated with only 2 cycles of single-agent ATO, the disease-free survival at 2 years was only 63.7%, strongly suggesting that 2 cycles was not enough therapy.64 Furthermore, the APL differentiation syndrome developed in 21%.
Kaplan-Meier curve of event-free survival and survival for the entire group of patients treated with ATRA and ATO for induction and consolidation.62
Kaplan-Meier curve of event-free survival and survival for the entire group of patients treated with ATRA and ATO for induction and consolidation.62
We are captivated by these recent reports showing that patients can be effectively treated and potentially cured with ATRA plus ATO. Therefore, for patients who are unable to tolerate anthracyclines because of heart disease or with a history of having received maximal cumulative doses of anthracyclines given for another disease, older adults, or those who decline chemotherapy, ATRA, and ATO are administered concurrently with the addition of limited doses (one to 4) of anthracycline. We prefer idarubicin and only for those who present with or develop a WBC count more than 10 000/μL during therapy and as few doses as are needed to control the WBC count. Similar to patients treated with conventional ATRA plus anthracycline-based approaches, neither the presence of FLT3 mutations nor secondary cytogenetic changes appear to influence outcome with ATO given for induction and consolidation.67 The combination of ATRA and ATO has emerged as the most exciting new treatment strategy in APL and will probably replace anthracycline-based chemotherapy and become standard of care for many, if not most patients soon.
Consolidation therapy
Consolidation strategies depend on the risk classification for relapse at diagnosis. Two or 3 cycles of anthracycline-based chemotherapy are administered for low- and intermediate-risk patients in first complete remission (CR1). For patients not participating on a clinical trial, 2 or 3 cycles of an anthracycline, either daunorubicin or idarubicin, plus 1 to 2 weeks of ATRA are administered until the achievement of molecular CR. ATRA for 1 to 2 weeks is given with each cycle of consolidation based on comparisons of consecutive historical series. For patients with high-risk disease (WBC > 10 000/μL), either intermediate- or high-dose Ara-C can be administered depending on age as a first consolidation as done in the GIMEMA APL 2000 study or ATO for 2 courses of 25 days each as carried out in the second North American Intergroup C9710 study.68 There is no clear best choice between these 2 approaches for a given patient because they have not been compared in a randomized trial. Given the shorter duration of consolidation, our preference is intermediate-dose Ara-C, reserving ATO for relapsed disease if a patient was not treated with ATRA plus ATO for initial induction.
Role of maintenance
Two randomized trials, the first North American Intergroup Study I0129 and the European APL Group APL93 trial, confirm the benefit of maintenance.50,53 However, a GIMEMA trial randomized patients in molecular CR1 after intensive standard consolidation chemotherapy to ATRA alone, ATRA plus low-dose chemotherapy, low-dose chemotherapy, or observation and found no benefit to any maintenance therapy.69 The Japanese Adult Leukemia Study Group APL97 trial also showed no benefit to multiple cycles of intensive maintenance chemotherapy (no ATRA administered at all) among patients who were molecularly negative after intensive consolidation.11 However, because the Japanese Adult Leukemia Study Group APL 97 trial did not study ATRA as maintenance and the GIMEMA trial has been published only in abstract form, until further studies are completed and the maintenance randomization arms of C9710 are analyzed, maintenance therapy for 1 to 2 years with intermittent ATRA and low-dose chemotherapy with 6-mercaptopurine and methotrexate is given, which may be particularly beneficial in patients with high-risk disease.15,50 There are no prospective comparative data to indicate whether 1 or 2 years of maintenance is better. Therefore, until further studies are completed, maintenance is continued for 2 years unless toxicity develops. The third in a series of North American Intergroup trials (S0521), which is currently ongoing, randomizes patients who are molecularly negative after intensive consolidation to receive or not receive maintenance therapy with ATRA and low-dose chemotherapy. The standard approach for induction, consolidation, or maintenance need not be modified based on the presence at diagnosis of other putative prognostic factors, such as additional cytogenetic abnormalities, therapy-related APL, M3V morphology, FLT3 mutations, and CD56 expression, or based on a specific PML isoform.10,70-74
Assessment of response and monitoring
Although it is tempting to repeat a bone marrow examination 10 to 14 days after beginning induction, as is routine practice for all other subtypes of AML, in patients with APL the appearance of the marrow may change minimally by that time and often is not even aplastic. Furthermore, evaluation of molecular response after initial induction is not useful because many patients remain positive because of delayed maturation of the leukemic cells, and there is no prognostic value in the result. In contrast, molecular remission after consolidation has important prognostic value.75 Therefore, a bone marrow need not be done during the nadir of induction but rather should be done once the peripheral blood counts recover from induction to determine whether a CR by morphology has been achieved. Cytogenetics and molecular testing need not be done at the end of induction because they may be positive despite morphologic CR and have no prognostic value. However, if cytogenetics and molecular studies are done at the end of induction and show a normal karyotype and no molecular evidence of disease, the patient can be followed by RT-PCR from the peripheral blood without additional bone marrow examinations. Alternatively, if cytogenetics and RT-PCR for the PML-RAR-α fusion transcript are not done at the end of induction or either are still positive, a bone marrow should be examined at the end of consolidation and evaluated for both.
After maintenance therapy is completed, the frequency of monitoring and in which risk groups are not clearly established. The outcome for patients presenting with low- and intermediate-risk disease with contemporary strategies is so favorable that frequent monitoring can be questioned. Monitoring from the peripheral blood is much more practical than repeating frequent bone marrows. Given the very low-relapse rate among low-risk patients, it seems reasonable to depart from what has become routine practice and monitor much less frequently than has been recommended in the past. Indeed, these patients may not require monitoring at all once in molecular CR1. Patients with intermediate-risk disease are monitored every 3 to 6 months and those with high-risk disease every 3 months during and after the completion of maintenance therapy, although data to indicate the optimal frequency are lacking.
Strategies for patients with relapsed APL
Inducing second remission
Relapse is becoming increasingly uncommon, particularly among low- and intermediate-risk patients.76 However, among those who present with high-risk disease, relapse remains problematic and is the major focus of clinical research. For patients who sustain a morphologic relapse, ATO is administered for at least two 25-day courses.77-79 Among patients receiving only 2 courses of ATO, the median duration of CR2 was 8 months (range, 24-22 months) at a median follow-up of 17 months.79 In the US multicenter trial, patients achieving a CR2 were then eligible to receive 4 additional courses of ATO, although some underwent either allogeneic or autologous HSCT. The disease-free survival at 18 months was 56%, and the overall survival was 66%.78 Several studies have suggested that the addition of chemotherapy to ATO may be better than ATO alone.77 Whether the addition of ATRA to ATO in patients with relapsed disease is beneficial is not clear. One small, but prospective randomized trial suggested no benefit.80 However, the median time from the last ATRA exposure was 5 months, suggesting that patients were resistant to ATRA, and it is not clear whether a patient has not been exposed to ATRA for a longer time would benefit. Therefore, in general, ATRA is not routinely administered with ATO in patients with relapsed APL. Four weekly courses of intrathecal therapy methotrexate or alternating methotrexate and Ara-C can be given. The approach for patients who have a molecular relapse is similar. Two samples are taken 2 to 4 weeks apart to document that the RT-PCR is definitely positive. If the initial sample is from the peripheral blood, then a narrow sample is taken and cytogenetics are also studied to confirm that there has been no cytogenetic relapse. Interestingly enough, anecdotal experience suggests that patients with only a molecular relapse may fare well with ATO alone and may not require postremission therapy once in a molecular CR2.81 However, until further data are available, such patients proceed to postremission therapy as patents with morphologic relapse.
Consolidating second remission
Once patients attain molecular CR2, the best outcome is achieved with high-dose chemotherapy and autologous HSCT, although the initial study reported very few patients.47 Peripheral blood stem cells can be mobilized with high-dose Ara-C, both as an effective mobilizing regimen and to provide CNS coverage, given increasing reports of extramedullary relapse, particularly in the CNS. Although GO is a very effective drug in this disease and can induce molecular CR2 in relapsed patients,82-84 there is a risk of venoocclusive disease/sinusoidal obstruction syndrome for patients who subsequently undergo HSCT. Although the risk after subsequent autologous HSCT may be relatively small compared with that present after allogeneic HSCT, ATO is preferred. The approach is similar for patients who sustain a morphologic relapse. Two 25-day courses of ATO are administered followed by 4 courses of intrathecal therapy and then patients proceed to autologous HSCT. A strategy of salvage therapy to achieve molecular CR2 followed by autologous HSCT can be expected to result in a 5-year disease-free or relapse-free survival of 70% to 80%.47-49,85 For patients who are not candidates for autologous HSCT, 4 additional cycles of ATO can be given after induction and consolidation (6 total cycles) as done in the U.S. Multicenter trial, in which approximately 50% of patients who received only ATO, but not HSCT, were alive and free of recurrence at a median follow-up of 17 months.78 Subsequent maintenance with intermittent ATRA can be considered, although there are no data to indicate that this is effective.
CNS relapse
For patients who develop an isolated CNS relapse, although the treatment for such patients is less clear, our approach is the same as those who sustain a molecular and morphologic relapse. ATO is known to cross into the CNS and achieves levels of approximately 30% to 50% of the serum levels.86,87 In general, unless a patient has a significant space-occupying chloroma in the brain parenchyma, radiation therapy is not given. Intrathecal chemotherapy is given twice weekly until clear and then weekly for 4 weeks, and then monthly for 4 to 6 months, although such a schedule is necessarily arbitrary.
Future directions
APL should be considered in every patient with newly diagnosed AML because the treatment is so urgent, effective, and different from that of all other subtypes of AML. Although the majority of patients with APL are cured of their disease with contemporary strategies, several important questions remain to be addressed in future studies to cure all patients. First, what is the best treatment for high-risk patients? Is administering intermediate- or high-dose Ara-C in consolidation or ATO preferable? Second, will the combination of ATRA and ATO with minimal or no chemotherapy replace standard therapy with ATRA plus anthracyclines? Ongoing cooperative group comparisons, such as the North American Intergroup trial S0535, evaluating concurrent ATRA, ATO, and GO for induction followed by 3 courses of consolidation with daunorubicin plus ATRA, ATO, and GO than maintenance and the GIMEMA[b]/DSIL-APL0406 protocol, which compares ATRA plus ATO with minimal chemotherapy to standard ATRA plus anthracycline, will be of great interest.
Two novel strategies bear close watching. Oral arsenic appears very effective, and the combination with oral ATRA will be an attractive strategy (a potential “dream team”).88 Second, tamibarotene (AM-80) has some potential advantages over ATRA in that it does not bind the RAR-γ.89 Therefore, it may be associated with less epithelial toxicity, such as rash and perhaps even less frequent development of the APL differentiation syndrome. It also seems to bind proteins less avidly, leading to higher sustained levels, which may or may not be important. The remarkable success in APL resulted from understanding the molecular basis of leukemogenesis, close collaboration among both laboratory scientists and clinical investigators, and rapid conduct of well-designed clinical trials. These endeavors should serve as a paradigm of how to treat other subtypes of AML.
Acknowledgments
The authors thank Drs Daniel Douer and Jacob M. Rowe for helpful comments on the manuscript and Drs LoAnn C. Peterson and Joan Guitart for assistance with preparation of the figures.
Authorship
Contribution: M.S.T. wrote the manuscript; and J.K.A. edited the manuscript.
Conflict-of-interest disclosure: The authors declare no competing financial interests.
Correspondence: Martin S. Tallman, Northwestern University Feinberg School of Medicine, Division of Hematology Oncology, Robert H. Lurie Comprehensive Cancer Center, 676 N St Clair St, Suite 850, Chicago, IL 60611; e-mail: m-tallman@northwestern.edu.